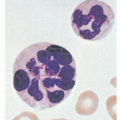
may have significant neutropenia (less than 1,000 neutrophils per dl). The disorder uniquely occurs in previously healthy young children from 6 months to 4 years of age and is seen with equal frequency in boys and girls. Occasionally cases of the disorder occur in clusters, suggesting it may be a consequence of some seasonal environmental toxin or virus. To date, however, serologic studies have failed to reveal exposure to a common virus. The natural history of TEC is that all patients recover spontaneously in a few weeks and there are no long-term hematologic sequelae. In many children with the disorder, particularly if there is evidence of recovery at the time of diagnosis, no specific therapy other than careful observation is necessary. Erythrocyte transfusions are indicated only if a child is symptomatic from the anemia, and rarely is more than one transfusion needed. Neither iron nor steroid therapy have any role in the management of this disorder. The diagnosis often is confused with that of iron deficiency anemia, although the erythrocytes in patients with TEC are normocytic (mean corpuscular volume [MCV] 70 to 85 fl, which is normal for children), whereas iron deficiency anemia is characterized by microcytosis (MCV, 50 to 70 fl). TEC also may be confused with DBA, although the latter generally presents before 6 months of age, often is associated with congenital abnormalities, and usually is characterized by macrocytic erythrocytes with many fetal-like features. (See section “Diamond-Blackfan Anemia.”)
TABLE 39.1 CLASSIFICATION OF PURE RED CELL APLASIA | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
It has been suggested that the low level immunogenicity of rhEpo might be enhanced in specific patients by the presence of Epospecific CD4+ T cells, or by HLA-DRB1*09.92, 171, 172, 173, 174
TABLE 39.2 DRUGS AND CHEMICALS ASSOCIATED WITH PURE RED CELL APLASIA | |||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree