Fig. 6.1
Cross-sectional anatomy of the eye
6.2 Eyelids, Periorbital Skin, and Tear Film
6.2.1 Anatomy and Physiology
The thinnest skin in the body is located on the outer surface of the eyelids. It is devoid of subcutaneous fat allowing for the accumulation of fluid to manifest rapidly as swelling. The upper and lower eyelids contain fibrous connective tissue, known as the tarsal plates, which function as structural support. The eyelashes are located on the anterior portion of the eyelids and aid in the protection of the eye.
The tear film covers the anterior surface of the conjunctiva and cornea. It serves the vital role of supplying the cornea with moisture, nutrients, enzymes, immunoglobulins, and protein signals, as well as allowing the maintenance of a clear, nonkeratinized epithelium in the visual axis. Furthermore, the tear film comprises the smooth outer refractive coating essential to vision by filling in corneal irregularities. The tear film consists of three layers. The aqueous layer is produced by the accessory lacrimal glands found in the conjunctiva. Meibomian glands located within the tarsal plates produce an oily layer that sits on top of and acts to stabilize the aqueous layer. The goblet cells of the conjunctiva produce the third, or mucous, layer. The overall function of the tear film is vitally dependent on each of these individual layers, and a deficiency in any layer will adversely affect the entire ocular surface.
The tears drain from the ocular surface via two puncta located on the medial aspect of the upper and lower lid margin. The puncta lead to the canaliculi that empty into the lacrimal sac and, ultimately, into the nose via the nasolacrimal duct.
6.2.2 Acute Radiation Effects
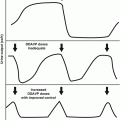
Madarosis, or loss of eyelashes, and erythema are the first side effects of radiation therapy (RT) involving the eye. Usually, eyelashes will grow back; however, permanent loss does occur. Erythema can occur within days of treatment (generally after doses of at least 20–30 Gy) and usually persists for a few days. Dermatitis is the most common acute side effect of RT. Dry dermatitis of irradiated skin can occur with doses greater than 20 Gy and often leads to desquamation. Moist dermatitis, with exposure of the dermis and associated serum leakage, can occur after the fourth week of RT following doses of 40 Gy or more, fractionated over a 4-week period. Blisters and edema may precede moist dermatitis. Symptoms include redness, peeling, burning, itching, and pain [3] (Fig. 6.2).
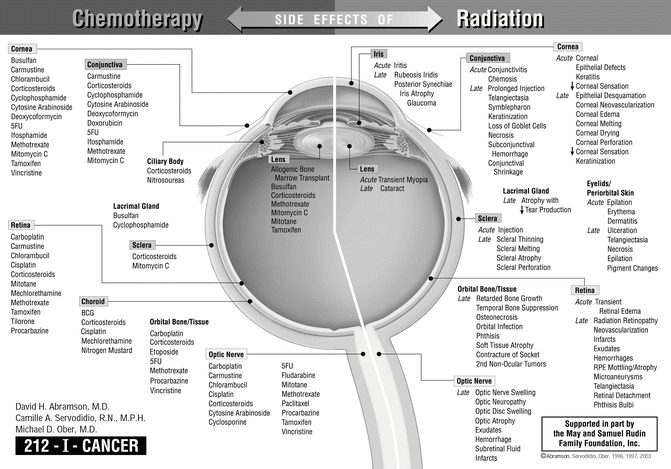

Fig. 6.2
Side effects of chemotherapy and radiation of the eye
6.2.3 Chronic Radiation Effects
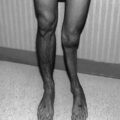
The late effects of RT to the eyelids following doses from 30 to 60 Gy include madarosis, telangiectasia (dilated, tortuous blood vessels; Fig. 6.3), hyperpigmentation, depigmentation, ectropion, hyperkeratosis, atrophy, necrosis, ulceration, and punctal occlusion. Although rarely seen today, lid deformities, such as ectropion (out-turning of eyelid margin), entropion (in-turning of eyelid margin), and atrophy or contracture, are seen when the tarsus has been included in the radiation field. The time of onset ranges from 2 months to greater than 5 years after treatment. Destruction or occlusion of the puncta may occur when the medial portions of the eyelid are irradiated, which leads to impaired tear drainage. Lid necrosis, exacerbated by excess sun exposure in areas previously irradiated, may develop months to years after treatment [4, 5].
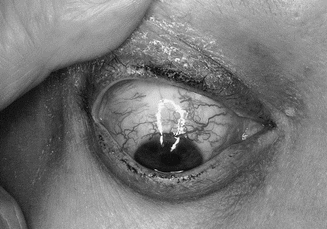

Fig. 6.3
Telangiectasia of the conjunctival blood vessels
6.2.4 Chemotherapy and Immunosuppressive Agents
Many chemotherapeutic agents, such as cyclophosphamide, ifosfamide, and methotrexate, alter the normal tear film physiology either by causing inflammation of the lacrimal glands or by being excreted directly into tears. This leads to dry eye symptoms including irritation, foreign body sensation, and photophobia, as well as inflammation around the eyelids and anterior segment of the eye [6]. Patients treated with alkyl sulfonates, including busulfan and nitrosourea, have also reported developing dry eye [7]. Both 5-fluorouracil [8] (5-FU) and docetaxel [9] can cause stenosis of the puncta and tear drainage system leading to excessive tearing called epiphora. 5-FU does so through squamous metaplasia and narrowing of the canalicular lumen [10], while docetaxel induces stromal fibrosis [11]. Some patients receiving 5-FU also develop cicatricial eyelid malpositioning [12]. Intravenous doxorubicin is associated with excessive lacrimation as well.
Paleness of the periorbital skin can occur following mithramycin infusion, while drooping of the upper eyelid, known as ptosis, has been reported following long-term corticosteroid use [13]. Vincristine can also cause unilateral or bilateral ptosis alone or as part of a cranial polyneuropathy [14–16].
6.2.5 Graft-Versus-Host Disease
The eye is primarily affected in the chronic phase of graft-versus-host disease (cGVHD), generally defined as greater than 100 days after transplant while the patient is being tapered off immunosuppressive therapy. Keratoconjunctivitis sicca, inflammation of the ocular surface secondary to insufficient tear film, is the most common manifestation of cGVHD. It is caused, in part, by lacrimal gland dysfunction from T-cell infiltration leading to scarring and decreased tear production [2, 17]. These patients are also more prone to developing dry eye because of conditioning regimens with total body irradiation and high-dose chemotherapy used to prepare the patient’s body to receive donor stem cells.
Dermatitis of the lid skin in cGVHD can lead to erythema, scaling, and ultimately lichenification or stiffening of the lids causing entropion or ectropion, lagophthalmos (incomplete lid closure), and trichiasis, all of which can worsen the symptoms of dry eye. The inflammatory response within the lids can also manifest as edema, hyperkeratosis, telangiectasias, or periorbital hyperpigmentation [2, 18]. Cicatricial occlusion of the lacrimal puncta may occur leading to epiphora [19].
6.2.6 Medical and Nursing Management
The management for eyelid complications due to cancer treatment consists mainly of skin care, including the use of ultraviolet protection, meticulous hygiene with mild soaps, use of skin lubricants, avoiding skin-sensitizing drugs (i.e., tetracycline), and occasionally corticosteroid and/or antibiotic creams. Ptosis, nasolacrimal duct obstruction, or eyelid malposition may require minor surgical manipulation by an ophthalmologist and should be referred in clinically significant cases [20]. At the first sign of epiphora secondary to punctal occlusion, prompt diagnosis and management by an ophthalmologist can prevent complete fibrosis of the canaliculi, which would require more invasive surgical intervention such as dacryocystorhinostomy. If identified early on, less invasive procedures such as punctoplasty or canalicular intubation with silicone tubes can be performed, which may prevent future occlusion [9]. In advanced cases of canalicular obstruction where surgery is contraindicated or not desired by the patient, botulinum toxin injection into the lacrimal gland can serve as a palliative option to alleviate epiphora [21]. Many cases of chemotherapy-induced ptosis eventually resolve after discontinuing the offending agent. Vincristine-induced ptosis, however, has been treated successfully with combined pyridoxine and pyridostigmine therapy [14–16].
The mainstay of dry eye therapy consists of tear replacement with artificial tears drops and ointment. Patients with symptoms or at risk should be encouraged to use liberal amounts of artificial tears. Unpreserved artificial tears are preferred, especially when they are used more than four times per day, due to the fact that the preservatives themselves can be irritating to the cornea, conjunctiva, and eyelids. Further aids include punctal occlusion, warm compresses to the eyelids, and, in advanced cases, cyclosporine drops [22]. Topical cyclosporine A, which inhibits T-cell activation and downregulates inflammatory cytokines in the conjunctiva, may even be effective in preventing or lessening the severity of dry eye when used prophylactically for cGVHD [23]. Patients with continued symptomatic or refractory dry eyes should be referred to an eye care professional without delay, as the consequences of hesitating could be permanent vision loss.
6.3 Conjunctiva
6.3.1 Anatomy and Physiology
The conjunctiva is a thin, transparent mucous membrane that lines both the posterior aspect of the eyelids (palpebral conjunctiva) and the anterior surface of the eye (bulbar conjunctiva). The folds between the palpebral and bulbar conjunctiva are known as the superior and inferior fornices, respectively. Tissue is redundant in the fornices to allow for adequate movement of the globe. The main lacrimal gland, which functions during reflex tearing, empties into the superior fornix, while the accessory lacrimal glands, supplying basal tear secretion, are found throughout the conjunctiva, concentrating in the fornices.
The conjunctiva contains a stratified nonkeratinized epithelium overlying a stroma, known as the substantia propria. Goblet cells supplying the mucin layer of the tear film are found intermixed with the epithelial cells. Besides acting as a physical barrier, the conjunctiva aids in host defenses by hosting immune cells as well as colonizing bacteria.
6.3.2 Acute Radiation Effects
Conjunctival inflammation (conjunctivitis), which manifests as vascular injection with clear or mucoid discharge, tends to occur 1–3 weeks after the start of radiation treatment. Edema of the conjunctiva, known as chemosis, may occur simultaneously or in isolation and usually lasts for a few days. The affected conjunctiva may also ulcerate leading to an increased risk of infection. The duration of these signs may be prolonged when RT doses over 30 Gy are used [3, 4, 24].
6.3.3 Chronic Radiation Effects
Late effects of RT to the conjunctiva include prolonged injection, telangiectasis, symblepharon (adhesions between the bulbar and palpebral conjunctiva), subconjunctival hemorrhage, shortening of the fornices, loss of goblet cells, keratinization, and necrosis. Exposure to 30–50 Gy results in prolonged conjunctival injection, which develops in 1–2 years, followed by telangiectatic vessels 3–6 years later. These fragile vessels tend to rupture with minor trauma, resulting in subconjunctival hemorrhage [5].
Chronic ulceration of the conjunctiva can be seen following treatment with 60 Gy. This leads to symblepharon formation. The definition of symblepharon is clarified in the paragraph above, resulting in shortening of the fornices, eyelid malpositioning, and trichiasis (turning of lashes onto the ocular surface). Goblet cell loss occurs at relatively low doses, resulting in tear film instability and dry eye symptoms, while doses over 50 Gy may result in keratinization of the conjunctiva. These keratin plaques constantly irritate the adjacent cornea, occasionally causing scarring and visual loss. Necrosis may occur after radioactive plaque therapy for retinoblastoma patients, where doses to the conjunctiva can reach between 90 and 300 Gy [3, 4, 24].
6.3.4 Chemotherapy and Immunosuppressive Agents
Conjunctivitis is a commonly reported symptom following induction therapy with many chemotherapeutic agents, including cyclophosphamide, ifosfamide, nitrosoureas, cytosine arabinoside, doxorubicin, methotrexate, deoxycoformycin, and mitomycin. 5-Fluorouracil is also associated with conjunctivitis and eye irritation. This usually occurs concurrently with the initiation of therapy, and it resolves within 2 weeks of treatment cessation. The immunosuppressive effects of corticosteroids are believed to facilitate opportunistic infections throughout the eye, including bacterial, viral, and fungal conjunctivitis, and can also lead to delayed wound healing [25]. Periocular carboplatin injections, a treatment sometimes used for intraocular tumors, can lead to fibrosis of the conjunctiva and underlying tissues [26].
6.3.5 Graft-Versus-Host Disease
In cGVHD, histological studies have demonstrated that there is a severe decline in Meibomian gland function as well as reduction in the total number of goblet cells in the conjunctiva [18, 27]. These two factors contribute to tear film deficiency and dry eye symptoms as described in the previous section. Keratinization of the conjunctival epithelium, conjunctival hyperemia with chemosis and serosanguineous exudate, subtarsal fibrosis, and conjunctival necrosis can also be seen in cGVHD [18]. Pseudomembranous conjunctivitis is a sign of severe systemic involvement in acute graft-versus-host disease, which occurs prior to tapering of immunosuppressive therapy [28]. Although not life-threatening, dry eye as a result of cGVHD has a significant effect on quality of life.
6.3.6 Medical and Nursing Management
Antibiotic eyedrops, sometimes in combination with corticosteroids, are used for prolonged conjunctivitis and for conjunctival ulceration. Artificial tears often aid chronic conjunctival irritation by providing the lubrication necessary to replace lost tear volume and dilute toxic chemotherapeutic metabolites excreted into the tear film. Vitamin A ophthalmic ointment (tretinoin 0.01 % or 0.1 %) may reverse squamous metaplasia and loss of vascularization from scar formation [29]. Patients with infectious conjunctivitis should be instructed to wash their hands frequently and take great care in interactions with others to prevent the spread of communicable diseases. In addition, sunglasses for protection from the sun and wind may be helpful in reducing symptoms. Severe conjunctival reactions, such as symblepharon and forniceal shortening, may require ophthalmologic manipulations such as symblepharon lysis on a repeated basis, or mucous membrane grafting with forniceal reconstruction. Ophthalmologic referral is therefore indicated.
6.4 Cornea
6.4.1 Anatomy and Physiology
The cornea is the transparent, avascular, anterior structure of the eye that refracts and transmits light to the inner structures of the eye. Along with the overlying tear film, it provides approximately two thirds of the refracting power of the eye. The conjunctiva borders the cornea in an area known as the limbus. This region contains corneal stem cells. Therefore, compromising this zone leads directly to the loss of corneal transparency and often its integrity. The cornea is an avascular tissue and thus depends on the limbal vessels along with the tear film and aqueous fluid from the anterior chamber for nutrients and waste removal.
The cornea consists of five specialized layers, including, from anterior to posterior: epithelium, Bowman’s membrane, stroma, Descemet’s membrane, and endothelium. The epithelium is stratified and nonkeratinized and replaces itself every 5–7 days. The stroma contains approximately 90 % of the overall corneal thickness, including a specialized superficial region known as the Bowman’s membrane. Descemet’s membrane is a tough, thickened basement membrane secreted by the endothelium. The endothelial cells form a monolayer, which controls corneal hydration via ionic pumps. Small changes in corneal hydration (thickness) drastically change the optical properties of the cornea; thus, the endothelial pumps are essential to maintaining clear vision. Endothelial cells can migrate to fill an area with damage, but they do not regenerate. Therefore, all loss of endothelial cells is permanent. Inflammation of the cornea, known as keratitis, also increases the corneal thickness and blurs vision.
6.4.2 Acute Radiation Effects
The corneal epithelium is adversely affected after RT doses of 10–20 Gy. Early effects include epithelial defects, keratitis, and decreased corneal sensation. When the tear film production or integrity is reduced, the epithelial cells become fragile and loosely adherent to themselves and the underlying stromal bed, resulting in epithelial defects. Patients with this problem will complain of ocular discomfort, foreign body sensation, excess reflex tearing, and blurry vision. Acute keratitis is often self-limited following exposure to 30 Gy, but following treatment with up to 50 Gy, it may persist for months along with conjunctivitis. Decreased corneal sensation may result from nerve damage and be exacerbated by impaired reflex tearing which, in turn, diminishes the blink rate and delays complaints from the patient [3, 24].
6.4.3 Chronic Radiation Effects
Late RT effects on the cornea include chronic epithelial defects, neovascularization, keratinization, edema, ulceration, and perforation. Epithelial defects may persist for months when radiation causes damage to corneal epithelial stem cells, accessory tear glands, goblet cells, and/or corneal nerves. The cornea responds to these nonhealing areas with neovascularization and keratinization, both of which temporarily or permanently decrease visual acuity. Abnormal blood vessels and chronic inflammation may lead to lipid deposition within the corneal stroma, further worsening vision. Damage to lacrimal glands, goblet cells, and corneal sensation impairs host defenses by limiting the cornea’s contact with tears and their accompanying nourishment, lubrication, immunoglobulins, and enzymes. Colonization and invasion of the corneal surface by bacteria may accelerate ulceration and perforation [3, 5, 24, 30].
6.4.4 Chemotherapy and Immunosuppressive Agents
Patients develop keratitis following treatment with many intravenous chemotherapeutic agents, including chlorambucil, cyclophosphamide, methotrexate, nitrosoureas, 5-fluorouracil, and deoxycoformycin [6]. Punctate corneal opacities and keratitis will occur acutely with cytosine arabinoside therapy, usually resolving approximately 4 weeks after completion. Intravitreal methotrexate, a treatment for intraocular lymphoma, can also cause a corneal epitheliopathy of varying severity, generally developing after three doses [31]. Both vincristine and vinblastine have been associated with corneal hypoesthesia, which may lead to neurotrophic corneal ulceration [32]. Patients undergoing long-term tamoxifen treatment may acquire whorl-like corneal epithelium deposits known as verticillata [33]. The immunosuppressive effects of corticosteroids facilitate opportunistic infections throughout the eye, resulting in bacterial, viral, and fungal keratitis as well as in corneal ulcers.
6.4.5 Graft-Versus-Host Disease
Chronic graft-versus-host disease can affect the cornea both directly via infiltration by macrophages and release of proinflammatory molecules and indirectly as a result of keratoconjunctivitis sicca and lagophthalmos [34]. The combination of tear film insufficiency and corneal exposure with a background inflammatory response can lead to a wide spectrum of corneal disorders. Punctate keratopathy, corneal epithelial sloughing, filamentary keratitis, or superior limbic keratoconjunctivitis may be seen as effects on the superficial structures of the cornea. Once the protective epithelial layer is compromised, the deeper structures of the cornea may become involved leading to corneal erosion, thinning, and ulceration. If untreated, perforation of the cornea can occur rapidly. Often in these cases, stromal infiltration by neutrophils is seen, but no microorganism is isolated [18]. Chronic inflammation of the cornea in GVHD can cause permanent stromal scarring, corneal vascularization [35], and calcification [2].
6.4.6 Medical and Nursing Management
Artificial tears and ointment are important in maintaining a healthy cornea following insults from cancer treatment. Patients using these solutions more than four times daily should consider unpreserved formulations. Autologous or allogeneic serum eyedrops made from the patient or a relative’s blood may be used for refractory cases. These contain epidermal growth factor, vitamin A, transforming growth factor-β, and fibronectin, which are all important for corneal and conjunctival health and are not present in artificial tears [36, 37]. Antibiotic drops are recommended for epithelial defects. Corticosteroid (dexamethasone) eyedrops are often given prophylactically with antimetabolite treatment, especially cytosine arabinoside, to reduce corneal and conjunctival irritation. Steroid drops may also be used with specific types of sterile infiltrates for keratitis, but should initially be avoided if active infectious causes are suspected. Corneal infections and ulcerations are treated with administration of antibiotic eyedrops as frequently as every 15 min. Bandage contact lenses, particularly gas-permeable silicone hydrogel lenses [38] or gas-permeable scleral lenses [39], along with antibiotic drops, may be used for nonhealing epithelial defects. Systemic immunosuppressive therapy with FK506 (tacrolimus) and corticosteroids have been used successfully to treat highly refractive dry eye cases, but this modality is limited by the potential for opportunistic infection or relapse of leukemia with long-term use [40]. It must also be noted that tacrolimus can cause a reversible toxic posterior leukoencephalopathy with cortical blindness [41]. Emergency surgical intervention with partial to complete tarsorrhaphy (sewing the eyelids shut to protect the cornea) or corneal transplantation may be required when corneal perforation is pending or apparent or with the formation of a central corneal scar [18]. Patients should be instructed to avoid factors that may contribute to eye irritation or dryness, such as fans, wind, smoke, or low-humidity situations. Moisture goggles at night and protective eyewear that reduces airflow over the eyes for outdoor activities can be beneficial [42].
6.5 Lens
6.5.1 Anatomy and Physiology
The lens is the second clear, avascular refracting surface of the eye. It lies posterior to the iris and is suspended circumferentially by a ring of fibrous bands known as the zonule. This encapsulated structure is devoid of nerves and vasculature and thus depends on the aqueous and vitreous humor for nutrients. Throughout life, the mitotically active cells located within the anterior periphery of the lens migrate inward toward the denser nucleus in the center. The cells of the lens are never shed; rather, they are incorporated into the nucleus. Thus, injured cells leave permanent, visible defects. For this reason, the crystalline lens is particularly susceptible to the formation of a cataract after cancer treatment. A cataract simply refers to the loss of optical clarity within the lens, a condition that can vary widely in severity.
6.5.2 Acute Radiation Effects
On rare occasions, transient myopia may occur in the weeks following RT as a result of increased water content within the lens.
6.5.3 Chronic Radiation Effects
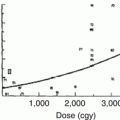
The posterior subcapsular cataract is the characteristic late complication of RT (Fig. 6.4). The lens is the most radiosensitive structure within the eye because of its perpetual mitotic activity and inability to remove injured cells or disperse heat efficiently. The report on cataracts following radiation therapy in 1957 by Merriam and Focht yielded results that remain clinically relevant today. They found the threshold for cataract development to be a single exposure to 200 rads, fractionated doses of 400 rads over 3 weeks to 3 months, or a total dose of 550 rads divided over more than 3 months. Furthermore, they reported that patients receiving a single treatment of 200 rads, fractionated doses of >1,000 rads over 3 weeks to 3 months, or 1,100 rads over greater than 3 months developed cataracts 100 % of the time [43]. The lens in children less than 1 year of age is more sensitive to radiation, as compared to the adult lens, presumably due to higher mitotic activity [24].
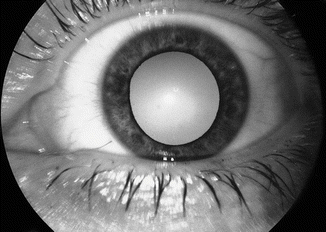

Fig. 6.4
Radiation-induced cataract
6.5.4 Chemotherapy and Immunosuppressive Agents
Cataract is the most frequently reported side effect associated with corticosteroid use. The incidence of steroid-induced cataracts ranges from 15 to 52 %, depending on dose and duration of treatment [44]. Although variable, the approximate threshold for cataract formation is 10 mg prednisone daily for 1 year [45]. It should be noted that steroid-induced cataracts have been reported following treatment with systemic, inhaled, topical, and skin formulations. Some patients treated with busulfan [46] also acquire cataracts, as do those receiving topical mitomycin C. Patients taking tamoxifen have been found to have a higher proportion of a specific class of cataract (posterior subcapsular) following years of treatment, which also may be indicative of lenticular toxicity [6, 47].
6.5.5 Medical and Nursing Management
At the present time, there are no known medical treatments for the reversal of cataracts. Prevention of cataracts is best accomplished by fractionation of the RT dose, lens shielding during treatment, and limiting exposure to toxic medications. Once a clinically significant cataract develops, surgical extractions and observation become the only options. Cataract extraction is elective in the vast majority of situations and depends upon the patient’s and family’s desires.
Cataract formation in young children is particularly significant, as visual pathways in the brain develop only during a finite period of time. When the central nervous system is presented with altered visual stimuli during this critical period, such as through an opaque lens, the potential visual acuity is reduced. When this phenomenon occurs, it is termed amblyopia. The vital time begins before or at birth and is believed to end between age 7 and 13. Once development is complete, alterations in the visual system no longer change the potential vision. When identified early in its course, amblyopia is potentially reversible. Visually impairing complications in children such as cataracts must therefore be recognized and treated early.
6.6 Uvea: Iris, Ciliary Body, and Choroid
6.6.1 Anatomy and Physiology
The uvea consists of three structures with a common embryologic origin: the iris, ciliary body, and choroid. The iris acts as the light aperture of the eye. It is a muscular membrane with a central circular opening (the pupil). Despite the wide variation in iris color on the anterior surface, the posterior surface of the normal iris characteristically contains a thick layer of heavily pigmented cells that act to absorb and thus limit the influx of light. The size of the pupil is controlled by the autonomic nervous system with input from both sympathetic and parasympathetic systems.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree