Introduction
Despite attaining control of hypercortisolism in most patients diagnosed with Cushing disease (CD) with precise neurosurgical techniques, medications (either steroidogenesis synthesis inhibitors, pituitary directed drugs to inhibit ACTH secretion, or cortisol receptor blockers), and in some cases, irradiation, outcome of patients is not optimal, since they still experiment more health problems and worse health perception than matched controls [ , ]. The same applies to other causes of endogenous Cushing syndrome (CS) (adrenal or ectopic). Chronic exposure to hypercortisolism determines long-term morbidity and greater health costs, which is evident even before correct diagnosis—often delayed for several years—and extends for up to 10 years after surgery [ ].
More cardiovascular, metabolic, osteomuscular, and neuropsychological problems are observed after having been diagnosed with CS; although they do improve after control of hypercortisolism, they often persist long-term and impact the future of the affected individuals [ , ]. This may involve personal, professional and social aims, which requires adaptations to new challenges, such as lower expectations regarding daily activities, working capacity, early retirement, or even income. Even in patients with the most favorable prognostic factors (those with high education, full-time employment before diagnosis, no comorbidities, and no history of depression), their chances of being in full-time work and a high income 2 years after surgery are lower than for sex- and age-matched healthy controls, despite having adapted to living with lesser capacities than before [ , ]. When adaptation to these limitations does not occur over time, patients often end up with depression, more anxiety, psychological and emotional problems, and feel helpless and bewildered [ ].
Long-term physical effects on health in treated Cushing syndrome
Multisystem morbidity and mortality are increased in patients with CS, especially around diagnosis but also after attaining remission of hypercortisolism. These chronic comorbidities include hypertension, diabetes, increased weight and central obesity, osteoporosis, fractures, and myopathy, as well as neuropsychological distress [ ]. Furthermore, acute complications and their potential consequences, such as more infections and venous thromboembolism related to hypercoagulability, are also more prevalent [ , ]. Awareness of these clinical problems is relatively recent, and given that CS is a rare disease, optimized protocols and prospective studies to demonstrate improvement after treatment are still lacking. However, as in other common chronic entities such as diabetes, hypertension, or osteoporosis, it would seem intuitive to recommend prospectively searching for and treating most of these comorbidities.
Understandably, greater health resource consumption occurs in these patients. At diagnosis, the use of antidepressants, anxiolytics, sleeping pills, opioids, renin angiotensin system-blockers, Ca-inhibitors, and antidiabetic medication is higher in CD patients compared with population controls [ ]. Five years after diagnosis the use of antidepressants, sleeping pills, opioids, renin angiotensin system-blockers and antidiabetic medication is still higher in the total CD cohort and in those CD patients in remission compared with population controls, while prescription of anxiolytics and Ca-inhibitors did not differ any more. Ten years after surgery, when numbers are smaller, the only difference in drug prescription observed between the total cohort of CD ( n = 56), those in remission ( n = 52) and controls ( n = 214) was greater use of antidiabetics in the CD groups [ ]. Although these results are compatible with improvement of diabetes, hypertension, perceived pain, and mental health after control of hypercortisolism, normalization of these health problems does not occur, since prescription of antidepressants, anxiolytics, sleeping pills, opioids, renin-angiotensin system blockers, and antidiabetic medication did not differ when comparing CD patients in remission for a median of 9.3 years and those with persistent hypercortisolism [ ].
Mortality is highest during active hypercortisolism and the first months after diagnosis, related to infections (especially with coexistent diabetes), cardiovascular events, and rarely even suicide. It is highly recommendable that these patients are managed by knowledgeable multidisciplinary teams who are aware of all these physical and psychological problems, to reduce this long-term morbidity and mortality [ , ].
Cardiovascular morbidity
As mentioned, despite normalization of hypercortisolism after successful treatment, health risks are increased during long-term follow-up. Prevalence of hypertension, central obesity, ischemic heart disease, venous thromboembolic and stroke risks persist compared with the normal population [ , , , , ]. Although the risk of heart failure has been reported not to differ from the reference population 1 year after diagnosis [ ], duration of hypertension is associated with more white matter lesions on brain MRI and 10-year cardiovascular risk, associated to worse cognitive function and reduced brain volume in CS patients in remission [ ].
Gut microbial dysbiosis, recently described in CS patients in remission, may be one of the mechanisms whereby cardiometabolic dysfunctions persist after “cure” [ ]. Furthermore, this gut microbial dysbiosis activates an inflammatory cascade in the liver, adipose tissue, and muscle, leading to insulin-resistance and sustained metabolic derangement [ ], leading to a vicious circle perpetuating a chronic, systemic, low-grade inflammation state with an unhealthy adipokine secretion profile, as described in treated CD [ ].
Metabolic complications
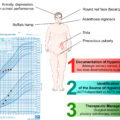
Diabetes mellitus and dyslipidemia are common during hypercortisolism; but even in remission from CD, patients have greater trunk fat mass, higher glycosylated hemoglobin (HbA1c), triglycerides, fibrinogen, and lower HDL-cholesterol concentrations as compared with controls, conveying a greater cardiovascular risk [ ]. Furthermore, both hypertension and diabetes determine increased mortality even 10 years after remission of hypercortisolism in patients previously diagnosed with CD [ ]. In fact, the degree of cortisol secretion has been found to be associated with diabetes mellitus and hypertension, nonalcoholic fatty liver disease, and a worse cardiometabolic profile even in patients with so-called nonfunctioning adrenal tumors. Namely, in so called mild adrenal cortisol secretion (MACS), i.e., in the absence of clinical signs and symptoms of CS but a lack of adequate cortisol suppression after a 1 mg overnight dexamethasone suppression test (which should suppress to < 50 nmol/L −1.8 mcg/L), diabetes is more prevalent [ ]. In these patients, a suppression below 50 nmol/L—but above 25 nmol/L, is associated to greater morbidity and a greater Frailty index, that includes 47 health variables such as diabetes, hypertension, muscle pain/stiffness with weakness in arms/legs, osteoporosis, fractures, and dyslipidemia [ ]. Thus, all these findings appear to point to hypercortisolism as a risk factor for many long-term and persistent health problems, which may be present even in very mild degrees of cortisol excess, previously considered “subclinical” CS.
Antidiabetic drugs, calcium blockers, and RAS-blockade drugs are prescribed more in patients diagnosed with CD compared with the control population in the 5 years before diagnosis, reflecting the diagnostic delay in the exposure to hypercortisolism [ ]. Five years after diagnosis, prescriptions of medications for hypertension and diabetes in patients with CD decrease compared with the time of diagnosis, reflecting improvement of these cortisol-induced comorbidities after control of hypercortisolism. However, at 10 years, antidiabetic medications including insulin are still prescribed more in CD patients compared with controls; this was especially so in patients with persistent hypercortisolism in whom the use of antidiabetic drugs and Ca-inhibitors was higher, compared with those who did attain remission, suggesting that cortisol excess was indeed related [ ].
Musculoskeletal health
Hypercortisolism is known to cause osteoporosis and greater fracture risk [ , ]. This fracture risk is increased in patients with CS even with an apparently normal standard dual X-ray absorptiometry, due to abnormal bone quality (as evidenced by microscanner or trabecular bone score) and vertebral morphometry [ ]. Prevalence of spine osteoporosis has been found to be higher in men than women diagnosed with CS, and males had more vertebral and rib fractures than females [ ]. Conventional osteoporosis treatment with bisphosphonates has been proposed for patients with persistent CS, even in the presence of normal bone mineral density [ ]. Although improvement of bone parameters and the increased fracture risk after correction of hypercortisolism can be expected, especially in the first year after surgery [ ], normalization still has to be proven. Furthermore, impaired bone geometrical and mechanical properties and reduced trabecular volumetric bone mineral density have been described in women a mean of 10 years after attaining remission of CS, which presumably contributes to a persistently elevated fracture risk [ ].
Subjective fatigability and tiredness and objective proximal myopathy with increased muscle fat infiltration and poorer muscle performance have been confirmed in women with CS, even years after cortisol normalization [ ]. Sarcopenia is also more prevalent after exposure to chronic hypercortisolemia, years after endocrine control of CS [ ]; these women with sarcopenia also complain of more pain, easy bruising and worries on physical appearance in the CushingQoL quality of life questionnaire and have worse muscle weakness-related quality of life than those without sarcopenia, as evidenced with a sarcopenia-specific questionnaire (the SarQoL questionnaire). They also performed worse on physical functioning of the generic SF-36 questionnaire [ ].
Even in adrenal adenomas with mild autonomous cortisol secretion (MACS) or so-called nonfunctioning adrenal adenomas (if their overnight post 1 mg-dexamethasone suppression cortisol is normal, i.e., below 50 nmol/L −1.8 mcg/L—but above 25 nmol/L), health variables such as muscle pain/stiffness, weakness in arms/legs, osteoporosis, and fractures, all of which determine greater frailty, are more prevalent in both types of adrenal adenomas [ , , ]. These findings evidence how even mild situations of hypercortisolism, i.e., one end of the continuum, extending from what used to be known as “subclinical” to overt hypercortisolism, may cause long-term consequences, which affect health and well-being.
Infections
During long-term remission of CD, a 5.8 increase in the standardized incidence ratio of sepsis was reported in a nation-wide study from Sweden [ ] and contributes to the elevated mortality due to infections even years after diagnosis [ ]. This increase is higher in those patients who do not attain remission and has originated the recommendation to vaccinate patients with a history of CS against influenza, herpes zoster, pneumococcal disease, and COVID-19, avoiding live vaccines in highly immunosuppressed patients. Furthermore, Pneumocystis jirovecii pneumonia prophylaxis has been suggested in cases of severe hypercortisolism [ ].
Data from the European Registry on Cushing syndrome (ERCUSYN) database have also evidenced that infectious diseases were the commonest cause of death (37%) in the 49 patients with CS who died, especially in older patients presenting with concomitant diabetes mellitus and active hypercortisolism [ ].
Neuropsychological and cognitive consequences of exposure to hypercortisolism
Most patients diagnosed with CS experience psychological distress at some time-point (anxiety, depression, and at diagnosis or during severe hypercortisolism, mania or psychosis). Additionally, other psychopathological complaints such as emotional irritability, apathy, and impaired body image are common and may persist many years after endocrine cure [ ] . Maladaptive personality traits (more negative affect and lack of positive affect and somatic arousal on most subscales of the Dimensional Assessment of Personality Pathology short-form) are also identified in patients with CD compared with others with nonfunctioning pituitary tumors [ ] . This is not surprising given the widespread presence of glucocorticoid receptors in the central nervous system and point toward a potential not totally reversible effect of previous glucocorticoid excess on the central nervous system; it also raises the question of whether treatment with high doses of exogenous glucocorticoids may have a similar effect [ ].
Subjective impression of body image while actively cushingoid ( left ) and 2 years after successful surgery ( right ), as drawn by a 20-year-old graphic designer. The author provided written consent to publish her drawings.
Reproduced with permission Webb SM, Santos A, Aulinas A, Resmini E, Martel L, Martínez-Momblán MA, et al. Patient-centered outcomes with pituitary and parasellar disease. Neuroendocrinology 2020. 10.1159/000506809.
At diagnosis depressive symptoms, anxiety, lack of confidence and great difficulty in managing stressful situations are often observed, and rarely even a history of suicidal ideas is reported [ ]. In addition, brain neuroimaging studies confirm the existence of widespread reduced white matter integrity, especially in structures important for cognitive function and emotional processing, as well as reduced gray matter volumes and cortical thickness [ , , ]. Functional brain imaging with MRI have evidenced abnormal responses both in the resting-state and during cognitive tasks, even long-term after control of hypercortisolism in several brain regions such as the posterior cingulate cortex, occipital lobe and/or cerebellum, thalamus, right postcentral gyrus, and left prefrontal cortex [ ]. In fact, patients with CS are more likely to suffer from poorer memory and concentration, attention deficits and apathy. How much improvement can be attained by cognitive training of these neurocognitive deficits is still uncertain, especially if hypercortisolism is not controlled [ ].
Furthermore, 10-year cardiovascular risk and vascular age, calculated according to an algorithm based on the Framingham heart study, correlated negatively with cognitive function and brain volume in both CS patients in remission and controls, but not in active hypercortisolism. Additionally, patients in remission of CS (but not active patients) had more severe white matter lesions than controls, which were positively correlated with diastolic pressure and duration of hypertension [ ]. Taken together, these findings can probably be explained by the longer follow-up and progressive aging in remitted patients after treatment, compared with a greater proportion of newly diagnosed patients in the active hypercortisolism group, especially in hypertensive patients. How long it takes for these lesions to occur after exposure to hypercortisolism is currently unknown; however, since they persist after normalizing cortisol, contributing to the subjective perception of impaired cognitive capacities after treatment for CS, an earlier diagnosis and treatment of both hypercortisolism and the accompanying cardiovascular risk factors is highly recommended [ ].
The significant impact of CS on neuropsychiatric health, both at diagnosis and at long-term follow-up, is evidenced in the nationwide study on psychotropic drug consumptions in Sweden over 28 years [ ]. Even in the 5 years before diagnosis the prescription of antidepressants, anxiolytics and sleeping pills was twice above that of the Swedish matched control population. Five years after diagnosis, CD patients still used more antidepressants and sleeping pills, and this was also the case for those in sustained remission for a median of 9.3 years. These results evidence that regardless of remission status, there is some degree of persistent negative effect of prior hypercortisolism on mental health, despite improvement compared with diagnosis. For example, the degree of anxiety does appear to improve 5 years after diagnosis and treatment, as evidenced by the decreased use of anxiolytics. Together, this possibly reflects adaptation to the new status on the one hand, and improvement of other comorbidities on the other. Nevertheless, the prescription of opioids in 32% of patients at diagnosis (compared with 6.8% in controls), presumably for bodily pain or fractures, which are more prevalent in CD patients [ , , , , ], is still higher 5 years after diagnosis, but not at 10 years anymore. These evidences again point toward the persistence of health problems, that do not disappear after control of hypercortisolism, and affect everyday life [ ].
Patients experience reduced tolerance to stress and less emotional stability, associated with difficulties in maintaining concentration. This may lead to difficulties in performing at work, since they may need periodic breaks to rest, especially during stressful situations, not understood nor acceptable for employers, leading to quitting jobs or early retirement, with consequent lesser income [ ]. Their difficulty in coping with stress, together with changes in their prior memory and executive capacity, may lead them to believe that they are facing dementia. Thus, education on all these issues and an empathetic and patient attitude of their health professionals can be very reassuring and helpful for these individuals. Asking patients how they feel (including emotions) and actively listen to their experiences is very much appreciated. Encouraging and highlighting improvements they may experience helps to create a close and supportive environment and is experienced as highly beneficial by the affected individuals [ ].
Agoraphobia sometimes associated with panic attacks, posttraumatic stress, and nightmares have been reported after treatment for CS. In serious cases, psychological evaluation with screening tools to better categorize the degree of anxiety and/or depression, followed by psychological treatment, may be necessary to attain improvement. On line apps that favor cognitive training, concentration and memory can also be of help in some patients to progressively improve their performance in these areas, i.e., Lumosity (
www.lumosity.com/en
). Other ways of helping can be to facilitate contact with other patients (if this is their desire) through patient associations or forums, Facebook and WhatsApp groups, or direct contact with other patients. Information on their disease and what to expect longer-term by providing written information is much appreciated, as well as the possibility and benefits of complementary treatments such as physiotherapy or adapted exercising programs. Alternatively, information is available through internet (for example on CS in general at
https://www.pituitarysociety.org/sitemap
or at
Cushing’s Patient Pamphlets
).
Since the burden and cost for the health system of this persistent morbidity in CS despite endocrine “cure” is high, strategies to facilitate overcoming these difficulties are desirable [ , ]. Apart from education and information on what to expect, psychological interventions, such as progressive exposure to stressful situations to gain self-confidence may be helpful for chronic stress disorders or agoraphobia. There are no guidelines or trials to indicate the best antidepressant treatment; in practice selective serotonin-reuptake inhibiting drugs such as citalopram or fluoxetine have been found to be helpful to overcome depression and to improve emotional discomfort as well as QoL [ ]. In severe cases, however, a psychiatric referral may be necessary to support these patients in their struggle for improvement.
Psychological recommendations to overcome these cognitive difficulties include favoring a proactive personal effort to overcome these situations and improve self-confidence and a positive attitude to face limitations. This facilitates a positive follow-up and recovery, which tends to be easier in younger patients with greater neuroplasticity. Support and monitoring by the managing team, to understand and face stressful situations can prevent collapse and favors successful professional and educational activities. In specific moments of stress, however, patients may experience the same discomforts typical of hypercortisolism, followed by physical and psychological exhaustion that requires resting for a couple of days. This is not surprising, since similarly to what occurs in active CS, during stress cortisol will exert its effects on its widely distributed receptors.
Memory, attention, information processing speed, motor function, concentration and executive functions such as verbal, visual, and working memory, verbal fluency, and decision-making, are all affected during chronic exposure to hypercortisolism and are not universally restored, despite successful treatment for CS [ , , ]. Furthermore, performance worsens when anxiety and depression are present, and especially among older adults, emotional stress impairs cognitive performance further. On the other hand, a higher baseline education linked to a better cognitive reserve can help to mitigate the effect of stress and chronic hypercortisolism on cognition [ ].
Impairment of the faculty of decision-making, including strategy and learning, has been investigated in patients with CS [ ]. Interestingly, no differences were observed between medically treated and cured CS patients, suggesting that prior exposure to hypercortisolism determined changes, which did not revert completely after treatment. Compared with controls, however, CS patients presented learning problems as far as decision-making strategies, failing to learn advantageous strategies, not using previous experience as a feedback factor to regulate their choices during testing. In parallel, high-resolution MRI of the brain showed decreased cortical thickness in the left superior frontal cortex, left precentral cortex, left insular cortex, left and right rostral anterior cingulate cortex, and right caudal middle frontal cortex in patients with CS compared with controls. Together these findings again evidence how chronic hypercortisolism promotes structural and functional brain changes, which are not completely reversible after endocrine remission.
Finally, the physical consequences of chronic exposure to hypercortisolism such as extreme fatigability, feeling chronically tired, or experimenting pain also affect the psychological and cognitive status negatively, so that a vicious circle is established. Recommending some easy and adapted physical exercise to improve muscle function and adequate analgesia can help to initiate overcoming this situation, improving the degree of anxiety and depression.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree