Introduction
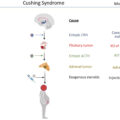
The history of Cushing’s syndrome (CS) dates back to the late 1800s when the first cases were reported, even though they were not recognized as such at the time. Identification of these complex diseases and their pathophysiology have been very challenging until the 20th century, as the hypothalamic–pituitary–adrenal axis (HPA, CRH, ACTH, and cortisol) was still unknown and their interactions poorly understood. Over time, several insightful scientists and physicians added new pieces to the puzzle and contributed to the gradual understanding of these complex conditions. Diagnostic methods and therapeutic avenues for CS were few and lacking, but improved drastically in precision and efficacy over time. As CS underlying pathophysiology and genetics are better understood nowadays, modern and more personalized therapies can be offered to affected patients. This chapter will review milestones in the discovery, pathophysiology, and management of the various etiologies of CS ( Fig. 1.1 ).
Timeline of landmark advances in CS history.
TSS , transsphenoidal surgery; DST , dexamethasone suppression test; BIPSS , bilateral inferior petrosal sinus sampling; RIA , radioimmunoassay; GC-MS , glass chromatography–mass spectrometry; CS , Cushing’s syndrome; PBMAH , primary bilateral macronodular adrenal hyperplasia; GCR , glucocorticoid receptor; MR , mineralocorticoid receptor; GPCR , G protein–coupled receptor; PPNAD , primary pigmented nodular adrenocortical disease.
Initial cases of CS and Harvey Cushing’s theory
The first suspected case of CS was reported by Osler in 1898, but was labeled as “an acute myxedematous condition, with tachycardia, glycosuria, melena, mania, and death” [ ]. It described a male patient suffering from a rapid 17 kg weight gain over 3 months with numerous symptoms including a very large abdomen, remarkable reddish-purple striae on the flanks, a bloated face, insomnia, irritability, increasing weakness, paranoid delusions, bloody diarrhea, and tachycardia. The patient was treated with oral thyroid extracts but worsened his psychosis and died in less than a week. Current knowledge would recognize this patient as having CS, but no confirmation at postmortem examination was documented.
Fourteen years later, Harvey William Cushing, a renowned American neurosurgeon, published a monograph describing 50 patients with pituitary disorders [ ]. Among them, a 23-year-old Jewish Russian woman, Minnie G, presented a 7-year history of temporal headaches, reduced visual acuity, weight gain, muscle weakness, adiposis dolorosa, and amenorrhea; her examination revealed short stature (145 cm), round face, hypertrichosis, thin skin, increased adipose tissue, and deep purple-brownish stria over the abdomen. Cushing described this intriguing syndrome as a “somewhat bizarre polyglandular syndrome” and speculated that it could be a consequence of hyperadrenalism related to an adrenal tumor. Interestingly, Carney eventually suggested that Minnie G might have a form of primary pigmented nodular adrenal disease because of her unusual clinical evolution over time [ ]. In the following years, other cases with features of CS were published, with various hypotheses for diagnosis [ ]. In 1913, Turney described a 25-year-old woman with secondary amenorrhea, bruises on the lower limbs, back pain with kyphosis, tachycardia, “extremely fat” face with “highly florid” coloring, hyperemic and dry skin, and truncal obesity with abnormally thin thighs. An X-ray examination revealed an expansion of the sella turcica, but believed that the disorder was of adrenal origin [ ]. In 1915, Anderson studied a patient with similar CS features in which tumors were found in both the pituitary and the left adrenal gland at autopsy [ ]; interestingly, findings of adrenal hyperplasia around the tumor and in the other adrenal suggested hyperactivity of both glands. In 1919, Reichman described CS patient in which adrenalectomy resulted in fatal outcome; a pituitary tumor and adrenal hyperplasia were discovered at autopsy, suggesting a relation between both anomalies [ ]. In 1926, Parkes Weber described in a CS patient a pituitary nodule, but was dismissed as the cause of the disorder because it was minute [ ]. In 1924, a probable CS case was published by Itsenko in a Russian journal originating the term Itsenko-Cushing’s syndrome still used in Eastern Europe and Russia [ ]. In the following years, an increasing number of CS cases were documented, but their precise etiology remained unknown.
The first major hypothesis for this mysterious syndrome was suggested by Cushing in 1932, 20 years after his first description of Minnie G. This founding father of modern neurosurgery was born in a family with three generations of physicians [ ]. He graduated from Yale in 1891 and completed his medical training at Harvard in 1895. He developed a close relation with the surgeon William Stewart Halsted and Sir William Osler during his career at Johns Hopkins, as they mentored him as a physician and author. In 1912, Cushing became Chief of Surgery at Peter Bent Brigham Hospital at Harvard University. During his career, he developed the use of modern anesthetic record during surgery and published over 300 articles and 13 books, including his Pulitzer Prize winning biography of Sir William Osler. One of his major interests were cerebral tumors, and he often discussed subjects of anatomy, physiology, pathology, and chemistry and detailed his laboratory experiments or clinical innovations in his publications. His creative mind resulted in many novelties, such as the use of silver clips or electrosurgery for control of bleeding and further development of various surgical methods.
In 1932, his famous work on pituitary basophilism was based on 12 cases with pathology confirmations, in which he proposed that basophil adenomas of the pituitary could be the cause of this curious clinical syndrome (CS) rather than an adrenal gland disorder. In the same year, a subsequent case was published by Bishop and Close using the term “Cushing’s syndrome” for the first time, after which its use became common to describe additional cases [ ]. The debate between adrenal and pituitary etiology of CS persisted for many years, with the frequent finding of basophil adenomas in many autopsies of patients without CS or, alternatively, cases with normal sella turcica [ ]. In 1935, Jores found that the melanophore hormone alongside another corticotroph substance was elevated in the blood in the presence of hypercorticism [ ]. During the same year, Crooke described recurrent pituitary changes in cases with CS, which reinforced the suspicion of a pituitary origin for the disease [ ]. In 1943, Albright proposed the idea of a clear distinction between CS and a genito-adrenal syndrome, laying the ground for the possibility of different etiologies [ ]. In 1947–48, Kepler detailed a categorization of CS possible causes, explaining that Cushing’s theory was one of many possibilities to explain the disorder, but reaffirmed that this relation could not be confirmed with pathology reports nor imprecise ACTH measurements available at the time [ , ]. In 1950, Bauer challenged this view by introducing his definition for the two types of “interrenalism.” Although most CS cases presented identical clinical features, he hypothesized a clear distinction between primary adrenal functional tumors, while a secondary etiology resulted from an excessive adrenal stimulation by an abnormal pituitary [ ]. Based on this distinction, the eponym “Cushing’s disease” became attributed to the disorders specifically involving a pituitary disease.
Initial biochemical basis of hypercortisolism
When Cushing’s views on pituitary basophilism were made public, biochemical science was still in its early stages without understanding of CS physiopathology [ ]. A direct link between a pituitary substance and occurrence of gigantism in animals was described by Evans in 1922, following intraperitoneal administration of pituitary extracts in animal models [ ]. In the early 1930s, Collip at Mcgill University in Montreal confirmed the suspected pituitary origin of the prolan substance found in blood, placenta, and urine during pregnancy [ ]. In 1933, his group identified multiple substances in the anterior pituitary including prolan (FSH), substance Q (GH), TSH, and a compound, which stimulated simultaneously the adrenal and thyroid glands. Collip concluded that this product was different from TSH and was later found to be ACTH. The first successful isolation of ACTH was achieved simultaneously by the teams of Li and Sayers in 1943 [ , ]. Other major scientific breakthroughs happened between 1935 and 1950, as Kendall and Reichstein first isolated compound E, cortisone, followed by several adrenal steroids and precursors [ ]. In 1948, Hench demonstrated the therapeutic effect of cortisone administration in a patient with rheumatoid arthritis and opened the way for the use of glucocorticosteroids (GC) in the treatment of many disorders [ ]. Together, these three scientists were awarded the 1950 Nobel Prize in Physiology or Medicine “for their discoveries relating to the hormones of the adrenal cortex, their structure, and biological effects” [ ].
Another breakthrough happened in 1951 when Nelson found increased serum concentration of 17-hydroxycorticorticosteroid following ACTH administration. Two years later, cortisol and corticosterone were isolated in adrenal veins, which became the first step in the development of a detection method for those hormones in the blood or urine [ ]. The development of radioimmunoassay (RIA) in the late 1950s greatly contributed to the understanding of CS, especially with the ACTH RIA in the 1960s [ , ]. With these new technologies, increased levels of cortisol were confirmed in blood and urine of all patients with CS, and the disorder could now be classified based on hormonal levels of ACTH and cortisol, confirming, in the early 1970s, Bauer’s hypothesis regarding distinct adrenal and pituitary etiologies of CS.
Progress in biochemical basis of CS
Understanding the hormonal pathways involved in the hypothalamic–pituitary–adrenal (HPA) axis represents an important milestone in the history of CS. In 1948, Harris described the neural control of the posterior pituitary (neurohypophysis) and theorized that the anterior pituitary gland activity was also directly influenced by the neurones of the hypothalamus [ ]. Three decades later, CRH, a 41-amino-acid neuropeptide involved in the stress response of the hypothalamus was identified by Vale [ ]. Further experimentation confirmed the link between CRH expression and stress, showing that CRH concentration was increased by stress-inducing experiences [ ]. The role of CRH on pituitary corticotroph function was eventually linked to direct release of pro-opiomelanocortin (POMC) peptides, while also activating POMC gene transcription, thus proving Harris’s initial suspicion of neural involvement in the function of the anterior pituitary [ ].
In 1968, Segal and Christy investigated whether another factor distinct from ACTH could be inducing adrenal growth. Inactivation of ACTH by antiserum in rats did not cause adrenal atrophy, although corticosteroid levels were effectively reduced [ , ]. In 1977, Mains, Eipper, and Ling found that a pituitary precursor POMC molecule extracted from rodent pituitary was the common source of both ACTH and beta-endorphins, alongside another unknown glycopeptide (y-MSH) [ ]. Two years later, the cloning of POMC gene was achieved, identifying that ACTH is located in the center of the molecule, flanked by beta-LPH at the C-terminal and y-MSH at the N-terminal [ ]. It was later discovered that subsequent specific intratissular cleavage with specific convertases would allow the conversion of POMC prohormone into active substances like ACTH [ ].
In the mid-1980s, mechanisms of repression of POMC gene transcription in the pituitary by glucocorticoid receptors (GR) and various transcription factors were detailed by Drouin et al. [ ]. In the early 1990s, evidence of GC-induced inhibition of hypothalamic CRH expression and release was reported [ ]. During the same period, vasopressin (VP) was shown to be another important regulator of ACTH in corticotroph cells via its AVPR3 (or AVPR1b), acting as a weak stimulant of ACTH secretion, while also potentiating CRH effects, especially during chronic stress [ ]. Aguilera et al. also described an attenuation effect of vasopressin on glucocorticoids’ negative feedback on the pituitary cells, which was theorized to be a possible mechanism to keep a functional stress response in a situation of chronic stress or GC exposure [ ].
In parallel to the hypothalamic and pituitary roles in the HPA axis in the 1980–1990s, advances in adrenal steroid metabolomics were fueled by advances in biochemical analytic techniques such as chromatography–mass spectrometry (GC-MS) [ ]. Mechanisms of adrenal hormonal synthesis were studied extensively, and the role of cholesterol as a steroid substrate was confirmed in the late 1970s [ ]. Major breakthroughs were made while studying patients with steroidogenic enzyme deficits resulting in congenital adrenal hyperplasia (CAH), including the demonstration of the 21-hydroxylase deficit in those patients [ ]. Using a combination of urinary steroid analysis and chromatography techniques, many steroidogenic enzymes were characterized between 1955 and the early 2000s alongside the consequences of their respective activity deficit [ ]. During the past 15 years, the usefulness of gas chromatography/mass spectrometry (GC/MS) or tandem mass spectrometry coupled with liquid chromatography (LC/MS–MS) for adrenal steroid profiling and adrenal tumor signatures was confirmed using computational machine learning–based analysis [ , ].
The gradual understanding of adrenal enzymatic functions led to the discovery of key pathways leading to cortisol metabolism. A breakthrough in this field was the characterization of the enzyme 11-beta-hydroxysteroid dehydrogenase (11-βHSD) by Carl Monder’s team in 1985 who demonstrated its role in bidirectional conversion of cortisol into cortisone [ ]. The interest in 11-βHSD sparked in the mid-late 1980s with the discovery of “apparent mineralocorticoid excess” (AME) in which children presented with severe hypertension, sodium retention, potassium loss, metabolic alkalosis, and suppressed renin, but undetectable levels of all known mineralocorticoids [ , ]. In parallel, the mineralocorticoid receptor (MR) was cloned by Evans and was equally activated in vitro by cortisol, corticosterone, and aldosterone, which presented a paradox because in vivo MR did not seem to be affected by cortisol [ ]. The solution to this problem was eventually explained by the inactivation of cortisol in the kidney via the effect of the 11-βHSD2, which could in turn explain the physiopathology behind AME in patients with abnormal 11-βHSD2 function [ ].
In the 1990s, apparent resistance to glucocorticoid effects was reported [ ] and was sometimes found to be present in multiple members of the same family, thus leading to a genetic disorder hypothesis. The successful cloning of the glucocorticoid receptor (GR) cDNA from the NR3C1 gene by Hollenberg in 1985 greatly contributed to elucidate this clinical problem [ ]. GR had at least two isoforms, GRα (active) and GRβ (inactive), and further studies by Chrousos et al. described multiple instances of mutations and polymorphisms in the NR3C1 gene, presenting phenotypes with different degrees of glucocorticoid resistance and autosomal transmission in some cases [ ].
Investigation of CS
In the early 1950s, it was generally accepted that clinical evaluation was insufficient to properly diagnose CS because some patients were lacking the classic signs of the syndrome. Direct methods of measurement of cortisol in patients were limited, and physicians had to rely on other means to estimate adrenal function. The main technique available was the estimation of urinary 17-ketosteroids, metabolites of adrenal androgens, which were thought to correlate to the degree of hypercorticism in patients, even if lacking accuracy [ ]. In parallel, correlation between urinary steroids and daily adrenal cortisol production was considered poor while unable to diagnose adrenal hypofunction. In the late 1950s, Rosner et al. demonstrated that, despite its limitations, his method using glass chromatography for measuring unconjugated urinary cortisol was efficient in diagnosing CS [ ]. Following development of RIA, measurement of urinary cortisol became more readily accessible in the early 1980s, but necessitated separation by chromatography of unconjugated cortisol from conjugated cortisol metabolites to avoid cross-reactivity [ ].
Several methods for determining plasma steroids were also developed, the most frequently used at the time being the multiple step techniques for measuring plasma 17-hydroxycorticosteroids by Nelson and Samuels or Siler-Porter [ , ]. In 1962, Mattingly developed a simplified method using natural fluorescence, the first to be accessible in clinical settings, despite having a poor specificity for cortisol [ ]. In 1973, this method was replaced by RIA techniques and, after continuous development, remains widely available to perform cortisol measurement [ ]. Despite their usefulness, RIA presents important limitations such as cross-reactivity with other endogenous or exogenous steroids and does not differentiate free cortisol from cortisol bound to proteins, which can hinder diagnostic evaluation in some settings [ ]. Newer techniques using GC-MS, described in 1975, and later LC-MS/MS, in 2001, allowed to circumvent previous limitations of RIA and measure more accurately cortisol alongside other steroid hormones [ , ].
In the 1960s, salivary cortisol evaluation emerged because of its ease to identify abnormal cortisol circadian rhythm and because its level reflects plasma concentration changes rapidly [ ]. However, lack of precision at very low cortisol levels in saliva rendered this approach difficult at that time [ ]. In 1978, salivary cortisol was successfully measured for the first time by RIA, opening the way for further development of this technique [ ]. Two main challenges persisted: (1) cross-reactivity with salivary cortisone and (2) cortisol concentrations falling under detection threshold during certain periods of time, especially for late night measurement [ ]. Introduction of LC-MS/MS in 2003 presented an interesting solution to these caveats [ ].
Measurement of cortisol in hair was first performed using LC-MS in 2004 to document chronic abuse of corticosteroids in athletes [ ]. This provided several advantages: noninvasive ease of collection and storage of samples, long-term retrospective assessment of cortisol exposure [ ]. Cortisol incorporation into hair was thought to be by passive diffusion from the bloodstream into the hair shaft; this was confirmed by using a radiolabeling technique in rhesus monkey hair [ ].Cortisol was also present in sweat, indirectly increasing cortisol concentration in hair [ ].
Quantification of ACTH concentration in blood in the 1950s was challenging using animal antiserum to ACTH and because high concentrations were needed for detection [ , ]. RIA techniques in the 1960s markedly improved the accuracy of ACTH measurement in blood sample, even at lower concentrations [ , ]. Accurate measurement of CRH in blood was performed in the mid-1980s, after discovery of the analog ovine peptide by Vale in 1981 and the rat peptide by Rivier in 1983 [ , ]. In 1985, Suda confirmed the presence of CRH in human plasma with RIA and documented that it was affected by stress, negative feedback by cortisol on the hypothalamus and by circadian rhythm [ ]. One year later, Charlton also found that bedtime CRH alongside cortisol levels was elevated in depressed patients and that only cortisol levels were suppressible by dexamethasone in those cases [ ]. Unfortunately, determination of CRH levels in blood has remained in the field of research and not commercially available.
In the 1950s, new tests focused on the evaluation of the pituitary–adrenal feedback mechanism. The first test to suppress the HPA axis was developed by Liddle in 1960, using 0.5–2.0 mg of Δ′-9α-fluorocortisol, an analog comparable with dexamethasone, administered orally every 6 hours for 48 hours while measuring 24 hours production of urinary 17-hydroxycorticoids (17-OHCS) [ ]. In his observations, he noted that a “low-dose test” was useful to differentiate CS from normal patients, while a “high-dose test” was more useful in separating patients with bilateral adrenal hyperplasia from patients with adrenal tumors, as the former achieved a degree of partial suppression, while the latter did not. Five years later, Nugent proposed an effective “single dose” dexamethasone suppression test using 1 mg of dexamethasone at 11 hours or 12 hours pm, before measuring plasma 17-OHCS the next morning at 8 hours am; he noted that results could be falsely positive in acutely ill patients or individuals taking estrogens [ ].
Metyrapone, a 11b-hydroxylation inhibitor, was developed in 1958 as a pituitary function reserve test, measuring the compensatory elevation of adrenal precursors of cortisol via increased levels of endogenous ACTH in response to inhibition of cortisol production [ ]. Liddle also proposed its alternative use for differential diagnosis of CS etiology by observing the various responses to the drug in patients with confirmed hypercorticism [ ]. Notable differences in 11-deoxycortisol (compound S) and urinary 17-OHCS were found levels in response to 24 hours metyrapone exposure between CD, ectopic ACTH source, and adrenocortical tumor etiologies for CS [ ].
Use of CRH in the evaluation of ACTH source was first described by Chrousos in 1984, who observed a significant elevation in ACTH and cortisol in patients with CD following administration of ovine CRH. As a similar response was generally absent in patients with EAS, this test became utilized for the etiologic evaluation of CS [ ]. A simplified CRH test performed in less than 1 hour during morning was developed in 1993 [ ]. Another test using desmopressin, a long-acting analog of vasopressin developed in 1967 for its affinity for AVPR2 and treatment of diabetes insipidus, was also found of interest in the evaluation of CS [ , ]. Coslovsky reported in 1974 that it had a direct stimulatory effect on the corticotrophic axis with the increase of urinary 17-OHCS in patients with CD [ ]. In 1993, Malerbi observed ACTH levels stimulation following intravenous desmopressin administration in patients with CD, while most normal subjects did not experience the same effect [ ]. This response was later explained by the activation of ectopic AVPR2 or overexpressed AVPR1B receptors in CD tumor tissue (a finding also presents in some EAS tumors) [ ]. Desmopressin test became increasingly utilized as a stimulation test in the diagnostic procedures for CD diagnosis and follow-up, including as an alternative stimulatory agent (to unavailable CRH) during bilateral inferior-petrosal sinus sampling (BIPSS) [ ].
Etiologies of CS from description to molecular basis
Cushing’s disease
“Basophil adenomas of the anterior lobe of the pituitary” as the cause of Cushing’s disease were mostly sporadic, but rare cases of ACTH-producing pituitary tumors were later identified as part of genetic syndromes, including MEN: MEN1 with identification of the causal gene in 1997 (loss of function mutation in MEN1 gene encoding for menin), MEN 4 (mutations in the CDKN1B gene encoding for the cell cycle inhibitor p27/Kip1) and most recently in MEN2A and MEN2B (mutations in the RET oncogene) [ ]. Cases were also described with mutations in AIP, DICER1 , or in patients with Carney complex (inactivating mutations in the PRKAR1A gene) and Lynch syndrome (mismatch repair genes such as MSH2, MLH1, MSH6, PMS2 , and EPCAM ) [ ]. Advances in molecular techniques established the monoclonality of sporadic corticotroph tumors in 1992 [ ]. Only a few mutations in genes encoding for corticotroph physiology regulation were found in the 1990s: GR mutations ( NR3C1 ; CS preceded by GC resistance) and only most recently, CABLES [ , ].
In 2014, a breakthrough finding in the molecular cause of CD occurred when Reincke identified somatic USP8 deubiquitinase gene mutations in approximately ∼50% of corticotroph adenomas. His team described elevated expression levels of EGFR in mutant corticotroph cells associated with high ACTH synthesis and secretion via stimulation of POMC gene transcription [ ]. The advent of next-generation sequencing and whole-exome sequencing efforts revealed many other previously unsuspected genetic events in sporadic corticotroph tumors in the past decade in the following genes: USP48, BRAF , TP53, ATRX , PIK3CA , DAXX and HCFC1 [ ]. Increased expression of 11β-HSD2, HSP90, or TR4, and loss of expression of BRG1 or CABLES1 have also been found to be involved in glucocorticoid resistance, therefore contributing to corticotroph pathogenesis. However, the precise mechanisms underlying the altered expression of these products and their potential link with CD remain unclear [ ]. It was also found that corticotropinomas exhibit increased or aberrant expression of AVPR1b or AVPR2, which is associated with a significant ACTH secretion response to desmopressin. More recently, epigenetic profiling and methylome analysis of functional corticotroph tumors identified few areas of hypomethylation that include the POMC promoter as well as high expression of cell cycle–related genes [ ].
Cushing’s syndrome secondary to ectopic ACTH and CRH secretion
Impaired glucocorticoid negative feedback due to deficiency in GR signaling could contribute to some cases of ectopic ACTH-secreting tumor pathogenesis in which ACTH is not suppressed following high-dose exogenous dexamethasone, in contrast to most cases of CD [ ]. However, this is not universal as GR expression is present in several cases of ectopic ACTH syndrome (EAS), mostly from benign neuroendocrine tumors (NETs), such as lung carcinoids [ ]. In one case of ACTH-secreting pheochromocytoma, a paradoxical increase in ACTH levels postglucocorticoid administration was observed and appeared to be mediated by demethylation of the E2F-binding site in the POMC promoter [ ]. Lack of ACTH response to desmopressin is observed in most EAS patients in contrast to the positive response in most CD patients, consistent with the lack of overexpression of AVPR1b in tumors with ectopic ACTH secretion. However, similar to CRH response, some ectopic ACTH-secreting tumors express AVPR1b [ ]. Germline mutations of NF1, VHL, RET, and MEN1 have been associated with the development of ectopic ACTH-secreting tumors [ , ]. Until this day, the mechanisms underlying the ectopic expression of ACTH in NET remain to be elucidated.
Cortisol-producing adenoma
In the 2000s, the teams of Bertherat and Bourdeau identified alterations of beta-catenin, coded for by the CTNN1B gene on 3p22.1, as playing an important role in adrenocortical cell proliferation as a transcriptional cofactor for T cell factor/lymphoid enhancer factor via the Wnt pathway [ , ]. CTNN1B mutations were identified in 15% of cortisol-producing adenomas [ ]. In 2014, Beuschlein et al. first identified somatic L206R mutation in the PRKACA gene on 19p13.12 (involved in the pathway cAMP-dependent protein kinase A pathways responsible for adrenal steroidogenesis) as the most common mutation in ∼50% cortisol-producing adenomas with CS, but rarely in those with mild cortisol excess [ ]. In 2017, Kamenicky’s team found somatic microduplications and chromosomal rearrangements of the 19q13 region where the GIPR locus is mapped in adrenocortical adenomas from patients with GIP-dependent CS [ ].
Primary bilateral macronodular adrenocortical hyperplasia
In 1956, Cohen et al. hypothesized that micronodular adrenal, macronodular adrenal hyperplasia and adrenal adenoma could be a continuum of the adrenal hyperstimulation secondary to ACTH [ ]. Later, reports by Kirschner and Lipsett reinforced the possible primary nature of nodular adrenal disease [ , ]. In 1967, Meador et al. proposed the name “primary adrenocortical nodular dysplasia” to distinguish these disorders from the more common form of ACTH-dependent bilateral hyperplasia [ ]. After the 1970s, many findings lead to the general acceptance of the concept of primary adrenal hyperplasia as a cause of CS, as it became clear that it was different from nodular hyperplasia secondary to longstanding corticotropin hypersecretion by a corticotroph adenoma. The most interesting findings were (1) presence of atrophy (both focal and more generalized) between the nodular tissue, (2) absence of pituitary corticotroph adenoma demonstrated in autopsies of patients with nodular adrenal hyperplasia, and (3) undetectable ACTH in plasma from petrosal sinus or peripheral blood after metyrapone, insulin-induced hypoglycemia, or corticotropin-releasing hormone infusion in patients with CS and adrenal nodular disease [ ].
In the following decades, efforts to clarify its etiology led to new findings of molecular mechanisms. In 1991, Weinstein et al. first reported the presence of activating mutations of the heterotrimeric G-protein alpha subunit (Gs-α, coded GNAS) in adrenal nodules of patients with CS and the McCune-Albright syndrome [ ]. In 1992, the groups of Lacroix and Reznik simultaneously reported the aberrant regulation by GIP of cortisol secretion by adrenal tissue of patients with primary bilateral macronodular adrenocortical hyperplasia (PBMAH) and food-dependent CS, suggesting that it resulted from ectopic expression of GIPR, which was later confirmed [ ]. This led the way to the demonstration by several teams including those of Lacroix, Bertagna, Lefebvre, and others that expression of various aberrant G protein–coupled receptors was highly prevalent in sporadic or familial cases of PBMAH such as β-adrenergic receptors, vasopressin (V2–V3 vasopressin receptor), serotonin (5-HT7 receptor), angiotensin II (AT1R), and glucagon [ ]. In some other cases, the hypersecretion resulted from an altered expression of eutopic receptors for vasopressin (AVPR1), luteinizing hormone/human chorionic gonadotropin (LH/hCGR), serotonin (5-HTR4), and leptin [ ]. One PBMAH case was reported for overexpressing GIPR due to a duplication of chromosome 19q13.32 including GIPR gene [ ]. Dysregulation of PKA signaling has also been identified in PBMAH tissue while mutations in the MC2R gene leading to an activation of PKA pathway have rarely been reported in PBMAH [ ].
In 2013, Assié et al., using integrated genomics approaches, found that biallelic germline and second somatic mutations of the Armadillo repeat containing protein 5 ( ARMC5 ) tumor suppressor gene are responsible of the development of PBMAH in 25%–50% of apparently sporadic or familial cases [ , ]. Recently, Wu identified that ARMC5 forms homodimers and anchors a multiple subunit RING-type ubiquitin ligase (E3) specific for RPB1 the largest subunit of DNA-dependent RNA polymerase II (Pol II); ARMC5 loss leads to a huge accumulation of RPB1 and enlarged Pol II pool size, thus dysregulating several genes involved in steroidogenesis and cell proliferation [ ].
In 2022, the teams of Kamenicky and Bourdeau identified that germline and somatic KDM1A inactivation was responsible for ectopic GIPR expression in 17 cases of sporadic or familial cases of GIP-dependent PBMAH and CS; this was rapidly confirmed by Bertherat’s group who also found germline KDM1A pathogenic variants and somatic 1p deletions in 10 cases of GIP-dependent PBMAH, which can also predispose to multiple myeloma and MGUS [ , ]. Some cases of PBMAH were associated with other endocrine neoplasias of thyroid, parathyroid, gastro-pancreatic, and uterine leiomyomatous tumors [ ]. In the last 25 years, analysis of familial cases of PBMAH leads to the detection of germline genetic defects associated with syndromes involving multiple endocrine or nonendocrine neoplasias, specifically MEN1 , FH (hereditary leiomyomatosis and renal cell carcinoma), and APC (familial adenomatous polyposis), or with isolated GNAS mutations [ , ] .
Micronodular adrenocortical disease
The first report of CS associated with small pigmented nodules of the adrenal gland was by Chute et al. in 1949 [ ]. For decades, it was debated if micronodular and macronodular hyperplasia was a continuum of the same entity. Ruder et al. first suggested that this condition represented a distinct entity with striking differences, both macro- and microscopic of the tumors, but also in their epidemiology and clinical course [ ]. Carney et al. reported a series of 40 patients in which primary pigmented nodular adrenal disease (PPNAD) was associated with spotty skin pigmentation, myxomas, and endocrine tumors, which later inherited its name as the “Carney complex” [ ]. In 2000, Stratakis group identified mutations of the gene encoding the protein kinase A type I-alpha regulatory subunit ( PRKAR1A ) as the most prevalent responsible in sporadic and familial forms of PPNAD [ ].
Over the years, several forms of micronodular bilateral adrenal hyperplasia were not caused by germline inactivating mutations of PRKAR1A ; many included micronodules that were nonpigmented and hyperplasia of the internodular tissue. The name “isolated micronodular adrenal hyperplasia” was later proposed by Stratakis [ ]. An inactivation of phosphodiesterase (PDE) sequencing defects with consequent high cellular cAMP levels was found; a genome-wide association study later identified inactivating PDE11A sequencing defects as low-penetrance predisposing factors for iMAD and related abnormalities [ ]. The same group also described a mutation (c.914A > C/H305P) in cAMP-specific PDE8B , in a patient with iMAD [ ].
Progress in imaging for CS
In 1919, Dandy introduced ventriculography and pneumoencephalography (PEG), injecting air as a contrast agent with X-rays [ ]. This technique allowed the visualization of suprasellar extension of pituitary tumors, but it was a difficult and risky procedure, limiting its use [ ]. The emergence of computed tomography (CT) in the 1970s facilitated the diagnosis of both suprasellar and subsellar growth of pituitary adenomas, opening the modern era of radiologic evaluation of intrasellar tumors. This allowed the development of the Hardy-Vezina classification of pituitary tumors [ ]. However, despite its enhanced spatial resolution, this technique achieved low diagnostic accuracy and sensitivity for corticotroph tumors [ ].
In 1973, Brown et al. reported the first biochemical confirmation of ACTH excess source from a large pituitary adenoma [ ]. An ACTH gradient of 1.4 and 1.5 between right jugular vein and peripheral blood, the first case of “selective venous sampling,” was found [ ]. In 1977, Corrigan et al. performed inferior petrosal sinus venous sampling for the first time, which is now a cornerstone technique for differentiating ACTH source between EAS and CD [ ]. In 1984, Doppman et al. reported the first BIPSS with CRH stimulation, increasing the sensibility of the procedure [ ]. Conventional CT (10-mm contiguous slices) available at that time could not localize the source of ectopic ACTH in 30%–50% of suspected cases of EAS [ ].
Adrenal gland imaging techniques were also limited before CT using plain abdominal radiography. The first attempts at specific adrenal imaging were by retroperitoneal gas insufflation or pyelography [ , ]. In 1955, caval venous sampling was first performed to measure catecholamines [ ]. This led to the development of selective adrenal venous sampling (AVS) technique. However, phlebography was associated with serious complications such as adrenal rupture or gland infarction [ ]. In 1978, Bierwalters et al. developed scintigraphy with radiolabeled iodocholesterol to identify the source of steroid excess in the diagnosis of functioning tumors or hyperplasias of the adrenal cortex [ ]. Major imaging advances occurred with the arrival of CT in the 1970s and development of the magnetic resonance imaging (MRI) in the 1980s [ ]. These new imaging modalities allowed for reliable identification of adrenal lesions or pituitary tumors >5 mm [ ]. With its highly detailed images and avoidance of X-rays exposure, MRI became the better alternative for pituitary evaluation, and further technology improvement in the 2000s led to increased performance in detecting pituitary corticotroph adenomas.
The development of functional imaging in the late 1980s brought a new perspective in the evaluation of CS and localization of neuroendocrine tumors. In 1989, Krenning et al. showed successful accumulation of radioiodinated compounds in several endocrine-related tumors [ ]. The utility of ( 111 In-pentetreotide) scintigraphy (Octreoscan) for ACTH-secreting tumors identification was of limited value for corticotroph tumors but showed benefits in ectopic ACTH-secreting tumors not visible in CT scan [ ]. In the 1990s, positron emission tomography (PET) initially showed disappointing results in the identification ectopic ACTH-producing neuroendocrine [ ]. In 1990, however, De Souza reported positive FDG uptake in ACTH- and GH-secreting pituitary tumors, suggesting potential diagnostic value, although evidence showed low sensitivity and specificity in detecting CD compared with other techniques (less than 50% in cases of CD) [ ].
In the 2000s, interest in the radiopharmaceutical Ga-68 labeled somatostatin analogs for the diagnosis of NETs increased. The utility of 68Ga-DOTA peptide PET in both nonfunctioning and functioning pituitary adenomas was investigated but showed limited use in differentiating corticotropinomas from normal pituitary uptake [ ]. 68Ga-tagged CRH was recently demonstrated to localize CD adenomas when they are not visualized on MRI. [ ]. 68Ga-DOTATATE combined with PET/CT or PET/MRI was shown to be of great utility in the detection and localization of ectopic ACTH-producing tumors [ ]. Introduced in the 2000s, MET-PET imaging using 11C-methionine was reported as a useful modality for confirming MRI-equivocal pituitary lesions [ , ]. O-(2-18F-fluoroethyl)- l -tyrosine (18F-FET) and 68Ga CRH PET have recently been proposed as novel tools for localization of corticotropinomas in MRI-negative cases [ , ].
Surgical and non pharmacological therapies of CS
Pituitary surgery
CD current treatment of choice is selective corticotropinoma resection by transsphenoidal pituitary surgery, but widespread use of this method became in use only in the latter half of the 20th century. Horsley was the first to use subfrontal craniotomy in 1889 for pituitary surgery, although his technique was quickly replaced by a much safer subtemporal approach [ ]. Surgical mortality and morbidity rates were high, but greatly improved in the early 1950s with the use of antibiotics and corticosteroids [ ]. Transsphenoidal approach, an alternative technique to pituitary tumor resection, was pioneered by Schloffer in the 1910s; his technique involved resection of the sphenoid and ethmoid sinuses through lateral rhinotomy [ ]. Several surgeons contributed to perfectioning this technique: Krause employed an extradural approach to avoid brain damage, Giordano proposed the transglabellar-nasal approach and Hirsch improved the technique via endonasal approach [ ]. Around the same time, Halstead successfully attempted oronasal rhinoseptal approach through a sublabial gingival incision, which Cushing perfected and described in his large series of transsphenoidal surgeries from 1910 to 1925 [ , ]. In 1929, he abandoned this technique for the transfrontal approach as it provided better visualization of the tumor and easier decompression of optic nerve [ ]. Interestingly, despite having described the concept of basophil adenoma in CD, Cushing never actually performed transsphenoidal surgery for its treatment. Rather, it was his pupils who made the first attempts: Pattinson, who accomplished implantation of radon seeds into the pituitary sella, and Naffziger, who achieved partial hypophysectomy in 1933. Unfortunately, these procedures were met with discouraging or transitory response in patients, and rationale for targeting the pituitary in the treatment of CD was reconsidered [ ]. Improved approaches for pituitary surgery appeared in the 1950s when Dott proposed the use of radiofluoroscopic control and pneumoencephalocisternography and, many years later, when Guiot introduced first to use the endoscope in transsphenoidal surgery (TSS) [ ]. In 1963, Hardy was the first to perform microscope-assisted TSS approach in CD, allowing microadenectomy of the pituitary [ ]. After perfecting his technique in the late 1970s, he, alongside Laws Jr. and Wilson, published results of their successful surgical series in patients with CD. They showed promising outcomes of this approach, even in patients with completely negative pituitary imaging, finally achieving treatment of choice for CD [ ]. In 1995, the first clinical series of purely endoscopic pituitary surgery was reported [ ]. Since then, a gradual shift happened toward endoscopic endonasal approach for pituitary and parasellar tumors, now considered the technique of choice for treating CD [ ].
Radiotherapy
New devices able to emit higher energy X-rays were developed in 1946, allowing Cushing to achieve the first successful treatment of a patient with CD using conventional radiotherapy on the pituitary [ ]. Subsequently, radiotherapy and bilateral adrenalectomy became the two common forms of curative treatment for CD [ , ]. In 1953, Olivecrona proposed pituitary electrocoagulation as a successful treatment for CD when adrenal surgery is not possible [ ]. The use of gamma unit, called the stereotaxic method introduced by Leksell in 1951, aimed to achieve better results and minimize the adverse effects of conventional radiotherapy [ ]. Originally designed to treat trigeminal neuralgia, it became useful to treat other surgically inaccessible intracranial targets including pituitary adenomas with significant advantages: great precision and accuracy, higher treatment dose delivered on tumors and sparing of the optical nerves. Further development of 3D imaging technology in the 1980s allowed for better treatment planning and significant reduction in side effect rates [ ]. Cyberknife and proton radiation radiosurgery are modern examples of technological advances in the radiosurgery field, providing alternative tools when surgery is not possible or ineffective at achieving CD’s cure [ ]. Following the widespread application of radiolabeled somatostatin analogs for identification of somatostatin-positive tumors, the use of therapeutic radionuclides was investigated. [ ]. In 2017, the somatostatin analog 177Lu-octreotate (Lutathera) was shown to have favorable tumor response rates and progression-free survival in some patients with advanced midgut neuroendocrine tumors. [ ]. Later, reports have also shown favorable outcomes in ectopic CS from gastroenteropancreatic tumors [ , ].
Adrenalectomy
The first successful adrenalectomy for suprarenal tumor was performed in London by Thornton in 1889 [ ]. The patient, a 36-year-old woman with hirsutism, survived 2 years following resection of her 20 pounds tumor until the disease recurred. Later, 10 reports of adrenalectomy performed in CS were published in 1934 by Walters and Priestley, describing a high associated mortality rate of 30% [ , ]. The first recorded perioperative use of cortisone following adrenalectomy for CS was in 1949, and with its use, the mortality rate fell to zero for the subsequent 18 reported cases. Through the early to mid-1900s, multiple changes in surgical technique for the adrenal were proposed. However, little progress for adrenal surgery occurred until the first minimally invasive technique of transabdominal laparoscopic adrenalectomy was developed by Gagner in 1992, resulting in decreased morbidity and improved quality of life [ ]. Many variants and improvements to this initial technique were developed in the following decades, and the minimally invasive adrenalectomy (MIA), laparoscopic transabdominal or retroperitoneoscopic approach, remains nowadays the surgical technique of choice for most benign adrenal masses [ ]. In more recent years, robotic adrenalectomy, first described by Piazza in 1999, can be utilized in selected cases with shorter hospital stays and less postoperative complications compared with MIA [ ].
Medical therapies for CS
The first articles describing forms of medical treatment in CS appeared in 1941, when Albright described exogenous testosterone effect in reducing tissue catabolism and Rakoff and Cantarow shared their experience with prolonged therapy with estrogens in CS patients [ ]. A decade later, the development of steroidogenic inhibitors brought a remarkable change in the medical treatment of hypercortisolism. In 1949, Nelson found that dogs exposed to the insecticide dichloro-diphenyl-dichloroethane (p,p’-DDD) developed adrenal cortical atrophy [ ]. Amphenone B, a toxic derivative from this insecticide, was synthesized in 1950 and found to induce adrenal hyperplasia, while inhibiting steroidogenesis [ ]. Analogs of amphenone B like metyrapone and mitotane (o,p’-DDD) were developed in the late 1950s to early 1960s and showed better tolerability profiles, making those drugs useful in the treatment of CS [ , ]. Aminoglutethimide was introduced in 1960 as an anticonvulsant, but was rapidly found to have a cortisol-lowering effect causing adrenal insufficiency in an 8-year-old female who developed a skin pigmentation typical of Addison’s disease [ ]. Soon after, reports were published confirming its inhibitory effect of corticosteroid synthesis [ ]. Due to its property as an aromatase inhibitor, it was mostly used as a treatment of breast and prostate cancer before its withdrawal in 2000 due to its toxicity. In the 1970s, new drugs with steroidogenesis inhibitory effects were developed: the most notable ones being imidazole derivates such as ketoconazole and etomidate [ ]. The former was found to reduce serum cortisol by inhibition of a variety of cytochrome p450 enzymes, including the side-chain cleavage complex, 17,20-lyase, 11/3-hydroxylase, and 17a-hydroxylase and was first used in CS in 1982 [ ]. Etomidate, an agent used to induce anesthesia, was also identified as a possible therapeutic agent in CS given its ability to cause transient adrenal insufficiency. This effect was initially described by Ledingham in critically ill patients who experienced increased mortality with lower cortisol levels associated with etomidate infusion [ ]. Later on, it was proven that low nonsedative doses could also inhibit cortisol secretion in patients with hypercortisolemia [ ]. More recently, Constantinescu et al. reported etomidate’s effectiveness in rapidly normalizing cortisol levels in patients with severe hypercortisolism outside intensive care [ ]. In the early 1990s, Levoketoconazole was discovered and, much later, used for the treatment of CS [ ]. Osilodrostat (LCI699) is another novel agent with a similar action to metyrapone via inhibition of 11β-hydroxylase (CYP11B1 and CYP11B2). Although it was originally developed in the 1980s as a treatment for hypertension via its aldosterone lowering properties, newer studies revealed its potent effect on cortisol steroidogenesis inhibition and its quite high efficacy in CS [ , ].
Therapies aimed at the hypothalamic or pituitary function were explored in the 1970s with agents such as cyproheptadine, valproic acid, and reserpine, but studies showed a lack of consistent efficacy in lowering ACTH [ ]. The success of dopamine agonist therapy in treating PRL- and GH-secreting pituitary tumors has led to study of such treatment in CD [ ]; retrospective studies and metanalysis data suggested biochemical normalization of cortisol in 25%–40% of patients, with subsequent loss of control in 20%–40% initially normalized [ ]. In the mid-1970s, Tyrrell and Fehm reported that somatostatin had a marked ACTH-lowering effect in hypersecretory states such as Addison’s disease and Nelson’s syndrome [ , ]. Following the synthesis of octreotide in 1982, its usefulness in CS was studied and showed no effect over placebo for lowering ACTH in seven patients with CS [ ]. However, Bertagna’s team demonstrated in 1989 the efficacy of long-acting octreotide for suppression ACTH in EAS [ ]. In the 1990s, evidence suggested that chronic glucocorticoid exposure downregulates SSTR2, but not SSTR5 expression [ ]. Consequently, in the early 2000s, a multiligand somatostatin receptor ligand with affinity for SSTR5, pasireotide, was tested as a potential treatment for CD [ ]. In 2012, it became the first drug approved for treatment of CD in patients with unsuccessful pituitary surgery or inoperable pituitary tumors [ ].
The introduction of the glucocorticoid receptor antagonist (GRA) mifepristone in the 1980s was a novel approach to the pharmacotherapy of hypercortisolism. Originally developed by Roussel-Uclaf as an antiprogestin, its glucocorticoid antagonist activity was recognized early during drug development [ ]. Its first reported use in CS was published in 1985, showing clinical and biochemical improvement in a patient with inoperable ectopic ACTH secretion secondary to a carcinoid tumor [ ]. Relacorilant is a new GRA devoid of antiprogesterone effects recently developed for which preliminary evidence suggests good efficacy in the control of hypertension and impairment of glucose metabolism, as well as a good safety profile in CS [ ].
Conclusion
Since the first report of suspected CS in the late 1800s, extraordinary progress has been made in the fields of physiology, biochemistry, radiology, surgery, pharmacotherapy, and nuclear medicine. These advances provided major improvement in diagnostic methods and treatment modalities for CS and its various etiologies. To this day, many promising studies are underway to further improve our understanding of this multifaceted disorder and optimize the treatment of affected patients.
References
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree