Introduction
Cushing syndrome (CS) is a rare endocrine condition, which results from chronic increased concentrations of cortisol [ ]. In contrast to exogenous CS that is a common due to the administration of synthetic glucocorticoids for a variety of disorders, endogenous CS is rare and accounts for only three to four new cases per 1 million people per year; however, only 10% of those are pediatric patients [ ].
Etiology
Endogenous CS may be ACTH-dependent or ACTH-independent. ACTH-dependent CS can be caused most commonly by pituitary adenomas secreting ACTH [Cushing disease (CD)] or less often by ectopic release of CRH and/or ACTH. On the other hand, ACTH-independent or adrenal-related CS may result from adrenocortical adenomas and carcinomas secreting cortisol or from macro- or micronodular adrenocortical diseases, including bilateral macronodular adrenocortical disease, bilateral micronodular adrenocortical disease, isolated primary pigmented nodular adrenocortical disease (PPNAD) or PPNAD in the context of Carney complex, and isolated micronodular adrenocortical disease (iMAD) [ ].
ACTH-dependent Cushing Syndrome or Cushing disease
In children aged over 7 years, ACTH-dependent Cushing Syndrome or Cushing disease accounts for 75% of all pediatric cases of Cushing syndrome. The most common cause of endogenous CS in children is the increased biosynthesis and release of ACTH from the anterior pituitary lobe. It is usually caused by a corticotroph pituitary neuroendocrine tumor (PitNET, also termed as pituitary adenoma), which is usually a microadenoma with a median diameter of 5 mm, or, rarely, a macroadenoma oversecreting ACTH [ ]. Histologically, PitNETs stain positive for ACTH and do not display any potential for invading to the cavernous sinus or even other parasellar loci; however, a rare type of PitNETs with aggressive behavior, termed as Crooke’s cell adenoma, has been described in a number of pediatric patients with resistance to treatment or distant metastasis [ ].
Ectopic ACTH production and release is extremely rare in young children, and accounts for ≤1% of Cushing syndrome in adolescence. The most common sources of ectopic ACTH biosynthesis and secretion include carcinoid tumors in the thymus, bronchus, or pancreas; medullary carcinomas of the thyroid, small-cell carcinoma of the lung, pheochromocytomas, or other neuroendocrine tumors. Although never described in pediatric patients, overproduction of ACTH by the pituitary gland may be caused by oversecretion of CRH by the hypothalamus or by an extrahypothalamic lesion producing CRH [ ].
Pituitary blastomas represent a rare cause of CD in infants [ ]. These tumors consist of undifferentiated epithelium Rathke-like cells and hormone-secreting cells. In addition, pituitary blastomas oversecreting ACTH are almost exclusively associated with DICER1 gene mutations [ ].
ACTH-independent Cushing Syndrome
ACTH-independent CS is characterized by autonomous secretion of cortisol from the adrenal cortex and accounts for 10%–15% of CS [ ]. Adrenal-related CS may be caused by unilateral cortisol-producing adrenocortical adenomas or carcinomas or bilateral adrenocortical disorders.
In young children, 70% of the cases of adrenocortical tumors that present with CS are malignant; the rest are adrenocortical adenomas (AA). Most children with adrenocortical cancer (ACC) are under the age of 5 [ , ]. As in adults, the majority of pediatric patients with ACC or AA are female. ACC is usually unilateral; however, 2%–10% of patients present with bilateral ACC. AAs are usually unilateral, unless a bilateral process is suspected. In adolescents, AAs represent the most common cause of ACTH-independent CS.
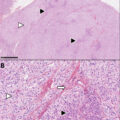
Bilateral adrenocortical hyperplasias (BAH) occur in less than 2% of all cases of CS in both children and adults [ , ]. The molecular basis of these diseases has been attributed to genetic defects in an ever-increasing number of genes that have been identified so far [ ]. BAHs are classified according to the size of the nodules identified on high-resolution computed tomography (CT): those with diameter greater than 1 cm are considered as macronodular [ ], whereas lesions with diameter less than 1 cm are micronodular. In addition to the size, BAHs are classified based on the existence or not of pigmentation on pathologic examination. In children, the most common form of BAH is micronodular adrenocortical disease, which may be further classified in primary pigmented nodular adrenocortical disease (PPNAD) and isolated micronodular adrenocortical disease (iMAD) [ , ]. In PPNAD, the adrenals are characterized by dark brown pigmented micronodules (diameter less than 1 cm) because of lipofuscin deposition, surrounded by an atrophic cortex. In contrast, iMAD is rarely associated with pigmented nodules [ , ]. Pediatric patients with either PPNAD or iMAD present frequently with cyclical or periodic forms of CS [ ]. PPNAD occurs most frequently in the context of Carney complex, which is characterized by multiple endocrine gland dysfunction, the development of cardiac and other myxomas and lentigines, as well as predisposition to several malignancies [ ].
Primary bilateral macronodular adrenal hyperplasia (PBMAH), also termed as massive macronodular adrenal hyperplasia (MMAD), is another rare cause of CS, characterized by nodules mostly larger than 1 cm [ , ]. Although most cases of PBMAH or MMAD are sporadic, the genetic basis of this form of BAH was recently described [ ]; the disease starts typically in adolescence, but may remain clinically silent until late adulthood. A number of patients with PBMAH or MMAD presents with food-dependent CS, a condition characterized by increased cortisol concentrations during food ingestion [ , ].
BAH with CS has also been associated with McCune Albright syndrome (MAS) and Beckwith–Widemann syndrome [ , ]. CS in patients with MAS usually presents in infants aged less than 6 months [ ]. There are only a few cases, all in young toddlers, of Beckwith–Widemann syndrome and CS that have been reported [ ]. BAH in cases of MAS and Beckwith–Widemann syndrome is characterized histologically by the presence of cells with fetal-like properties in the cellular zones of the adrenal cortex [ , ].
Genetics of Cushing disease/syndrome
ACTH-dependent Cushing syndrome or Cushing disease ( Fig. 10.1 )
The genetic basis of pituitary adenomas should be investigated in the context of young onset and relevant history in other family members [ ]. MEN1 and AIP remain the most commonly defective genes; however, cases with MEN1 and AIP genetic defects are very rare. As discussed above, pituitary blastomas are associated with DICER1 gene defects .
Genetics of Cushing syndrome. ACTH , Adrenocorticotropic hormone; AC , adenylate cyclase; BMAH , bilateral macronodular adrenal hyperplasia; Cα , catalytic subunit of PKA; GPCR , G-protein-coupled receptor; Rlα , type 1α regulatory subunit of PKA; PDEs , phosphodiesterases; PPNAD , primary pigmented nodular adrenocortical disease; PKA , protein kinase A.
MEN1 (multiple endocrine neoplasia type 1 syndrome) is inherited in an autosomal dominant fashion, and is caused by germline genetic defects in the tumor suppressor gene MEN1 [ ]. Children with MEN1 may present with pituitary tumors as the first presentation, with the youngest patient diagnosed at the age of 5 years. In addition to MEN1, mutations in CDKN1B gene causing MEN4 have also been identified in pediatric patients with CD [ ].
Somatic mutations in the USP8 gene have been reported in 30%–60% of adults with CD; Faucz et al. demonstrated that these mutations are also present in 31% of pediatric corticotropinomas [ ]. USP8 functions as a deubiquitinase that participates in the recycle of epidermal growth factor receptor (EGFR). Genetic defects in the hotspot region of the USP8 gene lead to increased catalytic activity of the enzyme, subsequent activation of the EGF signaling pathway, and finally increased expression of the POMC gene. Our team reported the first adolescent carrying a germline USP8 defect [ ]. The patient had severe clinical manifestations of recurrent CD unresponsive to surgical and medical treatment [ ].
ACTH-independent Cushing Syndrome ( Fig. 10.1 )
A growing body of evidence suggests that the cyclic adenosine monophosphate–protein kinase A (cAMP/PKA) pathway plays a fundamental role in the complex pathogenesis of CS ( Fig. 10.1 ). As mentioned above, MAS is caused by postzygotic activating mutations of the gene that encodes for the alpha subunit of the stimulatory guanine-nucleotide–binding protein, leading to the activation of the cAMP/PKA pathway through increased levels of cAMP. In addition to MAS, somatic mutations of GNAS1 gene have been identified so far in a small number of patients with cortisol-producing AAs or PBMAH/MMAD [ , ].
ACTH-independent CS because of PPNAD occurs in patients with Carney Complex, and is caused by germline inactivating mutations of the PRKAR1A gene encoding for the regulatory 1A subunit of PKA [ ]. These PRKAR1A mutations lead to prolonged activation of the cAMP/PKA pathway through increased availability of the PKA catalytic subunit. PPNAD patients present with a paradoxical response to dexamethasone with their urinary free cortisol concentrations increasing in response to synthetic glucocorticoids [ , ]. This phenomenon has been attributed to increased expression of the glucocorticoid receptor in the adrenal tumor cells whereby cortisol regulates its own release by the adrenal glands [ ]. This observation is very useful in the diagnostic work-up of patients with CS to clarify if the disease is bilateral, especially due to PPNAD, and to further help organize the next therapeutic steps.
In addition to PRKAR1A mutations, genetic defects in cAMP-binding phospho-diesterases (PDEs) [ ] have been identified in patients with isolated PPNAD or with other types of micronodular BAH, including iMAD. PDEs decrease cAMP levels following activation of the cAMP/PKA pathway; thereby, inactivating PDE mutations cause accumulation of cAMP and increased PKA activity. Mutations in two different PDEs ( PDE11A and PDE8B ) have been associated with iMAD [ , ].
Somatic mutations of the catalytic subunit of PKA, PRKACA, were then found in pediatric and adult adrenocortical CS. The most frequent hotspot mutation was the c.617A > G/p.Leu206Arg, leading to constitutive activation of PKA [ ]. Since then, an increasing number of PRKACA gene mutations have been reported in almost half of all cases of AAs [ , ]. Activating PRKACA mutations contribute to the formation of stable PKA holoenzymes and their constitutive activation, leading to increased biosynthesis of cortisol and uncontrolled proliferation of the tumor cells [ ].
In addition to genetic defects in the PRKACA gene, genetic rearrangements in the chromosome 19p13 locus have been associated with BAH and CS. These genetic rearrangements resulted in copy number gains encompassing the entire PRKACA gene [ , ]. The PRKACA copy number variation may occur de novo or can be inherited in an autosomal dominant fashion [ ]. The increased PRKACA gene dosage may result in both micronodular and macronodular BAH associated with CS with mild or more severe clinical features [ ].
PBMAH or MMAD may rarely occur in the context of several tumor syndromes, including MEN1 (due to MEN1 gene mutations), familial adenomatous polyposis (caused by APC gene mutations), or hereditary leiomyomatosis and renal cell carcinoma [attributed to fumarate hydratase ( FH ) gene mutations] [ , ].
Armadillo repeat containing 5 ( ARMC5 ) gene mutations on chromosome 16p11 have been identified in adolescent patients with PBMAH or MMAD who underwent adrenalectomy for CS [ , ]. Inactivating ARMC5 gene mutations were identified in the tumors; interestingly, both ARMC5 alleles were mutated: one germline mutation and the other somatic mutation. Subsequent studies have confirmed the increased frequency of ARMC5 gene mutations in patients with PBMAH or MMAD [ , ]. Food-dependent CS has not been described in pediatric patients.
Clinical presentation
The cardinal clinical manifestations of CS include weight gain with concomitant height deceleration ( Fig. 10.2 ) [ ]. These features discriminate CS from pediatric obesity, since children and adolescents with obesity display preserved height percentile. Fat deposition is generalized in pediatric CS, contrary to the prominently centripetal obesity in adult patients.
Clinical manifestations, auxological parameters, diagnostic work-up and therapeutic management of pediatric Cushing syndrome.
Skin manifestations include violaceous striae found in 60%–80% of patients, facial plethora, acne in ACTH-dependent CS, bruising, fungal infections, acanthosis nigricans due to insulin resistance, as well as supratemporal and supraclavicular fat pads [ , ]. Skin striae (stretch marks) are also almost never observed in children aged less than 5–7 years ( Fig. 10.2 ).
Children with CS may present with delayed sexual development in both sexes, secondary amenorrhea and irregular menses in females. Adolescents may present with virilization. Other problems commonly reported in pediatric CS include headaches in up to 80% of patients, hypertension in 50% of children and adolescents with CS, glucose intolerance (30% of pediatric patients), kidney stones, and fractures because of decreased bone mineral density [ ]. Sleep disruption, muscular weakness or myopathy, and memory problems are less common in pediatric patients with CS, compared with adult patients.
Diagnosis
Accurate and early diagnosis, as well as classification of CS is sine qua non for the appropriate therapeutic management ( Fig. 10.2 ). The medical history and the detailed clinical examination, especially review of auxological parameters, are fundamental to make the diagnosis of CS. If CS is suspected, laboratory examination and imaging confirmation are necessary. The Endocrine Society and the Pituitary Society published guidelines on the diagnostic evaluation of CS [ , ]. These guidelines are adjusted for pediatric patients with CS.
Confirmation of the diagnosis of Cushing Syndrome
The first step in the diagnostic evaluation of CS in children and adolescents is to document hypercortisolemia by at least two tests: 1) Measurement of midnight or late night salivary cortisol on 2–3 days; 2) 24 hour-urinary free cortisol (UFC) measured on 2–3 days, corrected for body surface area; 3) A low-dose dexamethasone-suppression test (DST; 1 mg overnight or 2 mg/day over 48 hours) for suppression of cortisol. It is worth mentioning that none of the above-mentioned tests has 100% diagnostic accuracy.
A number of studies have shown that the measurement of late night salivary cortisol has increased diagnostic performance, compared with UFC. Moreover, measuring salivary cortisol is a simple, noninvasive and accurate way to screen for hypercortisolemia in pediatric patients [ , ]; however, there is significant variation in the performance of this diagnostic test.
If measurement of salivary cortisol is not available, measuring serum midnight cortisol from an indwelling catheter might be an alternative test for documenting hypercortisolemia. The catheter should be placed at least 2 hours before blood sampling. Patients are highly recommended to turn off all screens by 10:00 p.m. Importantly, a serum cortisol level of ≥4.4 mcg/dL has a sensitivity of 99% and a specificity of 100% to distinguish pediatric patients with CS [ ]. In addition to salivary/serum cortisol, hair cortisol has been used in the diagnostic work-up of patients with suspected CS [ ].
Twenty-four-hour UFC measurement should be performed on 2–3 days for optimal sample collection, since inadequate collection of urine may result in false low UFC concentrations. On the other hand, false high UFC levels might be attributed to states of physiologic/non-neoplastic hypercortisolism (previously referred as pseudo-Cushing syndrome), including emotional and physical stress, chronic exercise, pregnancy, obesity, malnutrition, anorexia, poor glycemic control in patients with diabetes mellitus, depression, alcoholism, narcotic withdrawal, anxiety, as well as high water intake [ ]. Consequently, patients with suspected CS are advised to collect urine during days of consumption of normal amount of fluids and avoid excessive exercise [ ].
The low-dose overnight DST evaluates the ability of exogenously administered dexamethasone to suppress the activity of the HPA axis through the negative feedback loop of the neuroendocrine axis. There are many published protocols of this test recommending the administration of 15mcg/kg, 25mcg/kg, or 0.3mg/m2 (max 1 mg) of dexamethasone once at 11:00 p.m. for the overnight test or 1200mcg/kg/day (max 2 mg/day) divided by four doses for 2 days [ ]. It is of great importance to simultaneously measure serum dexamethasone concentrations to ensure the desired dexamethasone level has been achieved.
Identification of the source of hypercortisolemia
Once the diagnosis of CS is confirmed, the following step in the diagnostic evaluation of pediatric patients with CS is to identify the source of hypercortisolemia by distinguishing Cushing disease from Cushing syndrome.
Plasma ACTH concentrations of greater than 20–29 pg/mL in children with confirmed CS are highly suggestive of an ACTH-dependent CS (sensitivity 70%) [ ]. On the contrary, suppressed ACTH levels are consistent with ACTH-independent CS. In order to differentiate Cushing disease from ectopic ACTH secretion and adrenal-associated CS, the standard high-dose dexamethasone suppression test (HDDST or Liddle test) is highly recommended. In HDDST or Liddle test, 120 μg/kg of dexamethasone (maximum dose: 8 mg) is administered at 11:00 p.m. Serum cortisol is measured at 9:00 a.m. the morning before and the morning following dexamethasone administration. Upon HDDST, a 20% cortisol suppression from baseline is observed in children with Cushing disease, with a sensitivity and specificity of 97.5% and 100%, respectively [ ]. Another test to distinguish Cushing disease from ectopic ACTH secretion and adrenal form of CS is oCRH stimulation test. To set the diagnosis of Cushing disease, a mean increase of 20% above baseline for cortisol concentrations at 30 and 45 minutes and an increase in the mean corticotropin concentrations of at least 35% over basal value at 15 and 30 minutes after CRH administration should be observed [ ]. If bilateral adrenocortical hyperplasia is suspected, the classic Liddle’s test [(low-dose dexamethasone of 30 μg/kg/dose; maximum 0.5 mg/dose) every 6 hours for eight doses followed by the high dose dexamethasone (120 μg/kg/dose, maximum 2 mg/dose) every 6 hours for eight doses)] may be used. This test demonstrates a paradoxical increased secretion of cortisol in patients with PPNAD [ ].
Imaging
When ACTH-dependent CS is suspected, patients should undergo pituitary magnetic resonance imaging (MRI) with high resolution and with contrast using gadolinium. To detect small ACTH-secreting adenomas, high-resolution 18FDGPET may also be used [ ]. Adrenal CT scan should be performed to distinguish Cushing disease from adrenal-associated CS. In patients suspected to have ectopic ACTH or CRH secretion, a CT or MRI scan of the neck, chest, abdomen, and pelvis may be performed for detecting an ectopic source of ACTH secretion. Moreover, other imaging methods, such as labeled octreotide scanning, positron-emission tomography (PET), and/or 68Ga-DOTATATE PET/CT may be used in the identification of an ectopic source of ACTH. If the biochemical workup is not suggestive of a pituitary ACTH source, or if a pituitary lesion is not detectable on MRI, bilateral inferior petrosal sinus sampling (IPSS) might be performed to detect a pituitary microadenoma [ ].
Therapeutic management
Although not specific for pediatric patients, the Endocrine Society published guidelines for the therapeutic management of CS in 2015 [ ].
ACTH-dependent CS
The first line of treatment in pediatric patients with Cushing disease is transsphenoidal surgical (TSS) resection of the pituitary lesion [ ]. It is worth mentioning that TSS should be performed by experienced neurosurgeons in specialized centers to achieve the highest success rate even above 90% [ ]. There are two types of surgical approach that have been attempted; the endoscopic and the microscopic approach. The endoscopic approach is mostly preferable in cases of macroadenomas [ ]; however, in children of very young age with pituitary lesions or in cases of complex giant pituitary tumors, the transcranial approach remains the best option of neurosurgical management [ ]. Independently of surgical approach, surgical resection of the pituitary tumor may not be successful; therefore, disease may recur following the initial surgical approach. Remission is considered as postoperative nadir cortisol levels of <2-5mcg/dL [ ]. If postoperative hypocortisolemia occurs at early stages after surgery, it is considered as a sensitive biomarker of durable remission [ ]. It is noteworthy that the remission rate following surgical resection ranges between 62% and 98% depending on the types of criteria used to define remission and the cohort [ , ]. The list of postoperative complications includes diabetes insipidus (DI), syndrome of inappropriate antidiuretic hormone secretion (SIADH), panhypopituitarism (growth hormone deficiency, central hypothyroidism, hypogonadism) pituitary apoplexy, as well as bleeding and infection. The mortality rate is lower than 1%.
If remission is not achieved at early stages or recurrence develops following an initial remission, then the next therapeutic steps include pituitary radiotherapy or medical therapy. Radiotherapy is generally avoided especially in pubertal children, due to early and long-term complications of radiation, such as cerebral cortex toxicity and hypopituitarism [ , ]. The traditional dose of radiotherapy is 4500–5000 cGy administered over a period of 6 weeks. Nowadays, new methods of stereotactic radiotherapy, such as linear particle accelerator (LINAC), Gamma Knife stereotactic radiosurgery (SRS), and proton beam therapy, are now available for the treatment of CD [ ]. Although data is lacking in pediatric patients with CD, postoperative radiotherapy has not been associated with the development of second tumors and mortality in adults with pituitary adenomas [ ].
Medical therapy for patients with CD is used primarily as adjunctive following unsuccessful surgical resection. The mechanisms of action for drugs used in the therapeutic management of CD are: i) regulation of ACTH biosynthesis and release; ii) inhibition of adrenal steroidogenesis; and iii) inhibition of glucocorticoid receptor (GR) action. Currently, the U.S. Food and Drug administration (FDA) has not approved any medications for use in pediatric patients with CD; thereby some drugs are used as off-label. Ketoconazole has been approved by the European Medical Association (EMA) for children older than 12 years of age. This antifungal azole inhibits the activity of several enzymes participating in steroidogenesis; however it may cause gastrointestinal side effects and severe hepatotoxicity [ ]. In addition to ketoconazole, metyrapone (a steroidogenesis inhibitor approved by the EMA for the treatment of CS), mitotane (an adrenolytic approved by FDA for patients with adrenal tumor), pasireotide (a somatostatin analogue approved by FDA for patients with CD who may not undergo or have failed surgery), and mifepristone (a glucocorticoid receptor blocker approved by FDA for treating patients with CS and glucose intolerance or diabetes mellitus who do not meet the criteria for surgery or have unsuccessful surgery) have been used in adults [ ].
ACTH-independent CS
Surgical resection remains the best treatment for benign adrenal tumors. Pediatric patients with bilateral micronodular or macronodular adrenal disease are best treated with bilateral total adrenalectomy. Given that adrenal cancer is a rare disease in children and adolescents, treatment guidelines are lacking; however, a Children’s Oncology Group trial evaluated etoposide, cisplatin and doxorubicin combined with surgery, and showed an excellent therapeutic outcome for stage III ACC, in contrast to stage IV ACC [ ].
Early bilateral adrenalectomy in patients with Cushing syndrome unresponsive to conventional therapeutic options may minimize adverse events [ ]. A potential complication following bilateral adrenalectomy includes growth of the corticotropinoma, increased plasma ACTH concentrations, and hyperpigmentation (referred to as Nelson’s syndrome). According to two systematic reviews in adult patients, Nelson’s syndrome occurred in 21%–24% of the patients [ , ]. Importantly, patients with bilateral adrenalectomy are in high risk of adrenal crisis.
Postoperative management
Following a successful TSS in Cushing disease or after a surgical excision of a hormonal secreting adrenal adenoma, patients develop adrenal insufficiency with a median duration of almost 12 months. During this period while the HPA axis is recovering, synthetic glucocorticoids should be administered at the physiologic replacement dose (12–15 mg/m 2 /day two or three times daily) [ ]. Stress doses of hydrocortisone should be initiated immediately during and after the surgical resection. These doses should be tapered rapidly to a physiologic replacement dose. Following bilateral adrenalectomy, patients should receive lifetime replacement with both glucocorticoids (12–15 mg/m 2 /day two or three times daily) and mineralocorticoids (fludrocortisone) at a dose of 0.1–0.3 mg daily.
The patients should be routinely followed every few months. Screening for recurrence should be highly recommended, and includes measurement of at least two midnight or late-night salivary cortisol concentrations, or overnight dexamethasone suppression test once per a year [ ]. Importantly, these patients need stress doses of synthetic glucocorticoids for acute illness, any types of trauma, or surgical procedures for both cases of temporary and permanent adrenal insufficiency [ ]. Adrenal crisis has been associated with increased morbidity and mortality [ , ] and highlights the imperative need for patient and caregiver education [ , ].
Outcomes
Pediatric CS is characterized by potential long-term adverse medical outcomes because of chronic hypercortisolemia, and increased morbidity associated with surgical resection or radiation treatment [ ]. Chronic exposure to high levels of glucocorticoids is associated with impaired growth, increased weight gain/obesity, impaired glucose tolerance/diabetes mellitus, metabolic syndrome, hypercoagulability, osteopenia/osteoporosis, as well as with neuropsychiatric sequelae [ , ]. In 2017, our team reported disparities related to delayed diagnosis and treatment in the Hispanic and African-American populations, which was associated with higher risk for persistent CD or recurrent CD after surgery [ ].
Posttreatment challenges for children and adolescents with CS include growth progress and pubertal development, normalization of body composition, as well as mental health and cognitive development [ , ]. Systolic hypertension remained in 16% of pediatric patients with CD and 21% of children and adolescents with ACTH-independent CS. Importantly, diastolic hypertension was noted in 4% of all pediatric patients 1 year following treatment [ ]. In addition to hypertension, abdominal obesity, insulin resistance, and cardiovascular abnormalities may persist in pediatric patients after treatment for CS. Several studies investigating the final height and catch-up growth following treatment of CS have demonstrated conflicting results; children with poorer catch-up growth than expected should be tested to confirm ongoing remission of hypercortisolemia [ , , ].
CS has been associated with several psychiatric and psychological disturbances, including depression, anxiety and emotional lability [ ]. Furthermore, other abnormalities, such as irritability, impaired self-esteem, panic disorder, mania, psychosis, suicidal ideation, schizophrenia, obsessive-compulsive symptomatology, cognitive changes, and distorted body image may persist following remission of hypercortisolism, even after recovery of the HPA axis [ , ]. Up to 70% of adult patients reported improvement in the psychiatric symptoms gradually following correction of the hypercortisolism [ ]. Our team demonstrated that children with CS may experience a decline in cognitive and school performance 1 year after surgical treatment, without any associated psychopathology, with younger age at first evaluation associated with greater deterioration in IQ scores [ , ]. Moreover, we published that active CS, particularly in children with younger age, was associated with impaired quality of life scores and that residual impairment remained in physical function and role–emotional impact score despite improvement from before to 1 year after cure [ ]. It is worth mentioning that forgetfulness, unclear thinking, and decreased attention span did not improve after cure [ ]. Suicidal ideation has been reported in 17% and approximately 6% of adults with active CS and of children after surgical cure of CS, respectively [ , ]. Normalization of the HPA axis may uncover or even trigger psychopathological manifestations not precipitated by hypercortisolemia or vice versa. It is important to screen for risk factors for suicide attempt or suicide ideation in children before and following treatment of CS. Patients and their caregivers should be informed that changes in mood, behavior, cognitive function, and quality of life may develop for a long time after surgical treatment of CS. Early recognition of CS in children is of great importance. On the other hand, late diagnosis has been associated with increased morbidity and mortality [ ].
Concluding remarks
Pediatric Cushing syndrome results mostly from exogenously administered high doses of synthetic glucocorticoids; however, endogenous Cushing syndrome is a rare endocrine disease. Children and adolescent with Cushing syndrome present initially with increased weight gain and lack of height. The first step in the diagnostic work-up of Cushing syndrome is documentation of hypercortisolism with the 24-hour urinary free cortisol, midnight or late-night salivary cortisol, or a low-dose dexamethasone-suppression test. In children aged over the 6 years, Cushing syndrome is most commonly caused by a pituitary tumor oversecreting ACTH. In children less than 6 years old, Cushing syndrome is mostly adrenal-associated. Once the diagnosis of Cushing syndrome is confirmed, algorithms for distinguishing ACTH-dependent disease from the ACTH-independent syndrome are currently available. Surgery is the first line treatment intervention, whereas medical treatment and radiation have an adjunctive role. Importantly, Cushing syndrome in childhood has the potential for long-term adverse outcomes due to chronic hypercortisolemia as well as increased morbidity associated with surgical resection or radiation treatment; therefore, early diagnosis and treatment are imperative.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree