Acquired Aplastic Anemia
Robert A. Brodsky
HISTORICAL BACKGROUND
The earliest case description of aplastic anemia was by Dr. Paul Ehrlich in 1888.1 He described a young woman who died following an abrupt illness that manifested as severe anemia, bleeding, hyperpyrexia, and a markedly hypocellular bone marrow. The term aplastic anemia was first introduced in 1904 by Chauffard. In 1972, a patient with aplastic anemia became the first recipient of successful allogeneic bone marrow transplantation.2 The development of bone marrow transplantation and potent immunosuppressive therapy in the 1970s greatly improved the prognosis of an illness that was almost uniformly fatal within a few years of diagnosis. Although aplastic anemia remains a potentially devastating illness, with prompt intervention most patients now survive the disease.
ACQUIRED VERSUS CONSTITUTIONAL APLASTIC ANEMIA
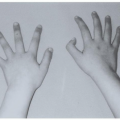
Acquired aplastic anemia can occur in any age group and is usually the consequence of an autoimmune attack against hematopoietic stem cells. Awareness of the less common inherited forms of bone marrow failure is critical in the assessment of any new patient with aplastic anemia (Chapter 37). These inherited disorders can masquerade as acquired aplastic anemia, but rarely respond to immunosuppressive therapies; management usually consists of supportive care or in severe cases bone marrow transplantation (BMT).3, 4 Inherited forms of bone marrow failure generally present in the first decade of life and are often associated with physical anomalies, (e.g., short stature, upper-limb anomalies, hypogonadism, café-au-lait spots); however, inherited forms of bone marrow failure may present well into adulthood. Some patients have a positive family history of cytopenias, highlighting the importance of taking a careful family history when evaluating aplastic anemia patients.
Fanconi anemia, the most common form of inherited bone marrow failure, is usually an autosomal recessive disorder that is characterized by defects in DNA repair and a predisposition to leukemia and solid tumors.5 Recently, a rare, X-linked form of Fanconi anemia has been described.6 Dyskeratosis congenita (DKC) is an inherited bone marrow failure syndrome that results from loss of function mutations of telomerase components and displays considerable clinical and genetic heterogeneity. Although DKC classically presents with the triad of abnormal skin pigmentation, nail dystrophy, and mucosal leukoplakia, these findings can be subtle.7, 8 X-linked recessive, autosomal dominant and autosomal recessive forms of DKC are recognized.9, 10 Telomerase reverse transcriptase (TERT) and the RNA component of telomerase (TERC) form the core of the active telomerase complex. Autosomal dominant DKC can result from mutations of TERC11 or TERT.12 The X-linked recessive DKC results from mutations in the gene DKC1, whose gene product, dyskerin, is important for stabilizing the telomerase RNA-protein complex.13, 14 Mutations of the TINF2 gene can also lead to DKC. TINF2 mutations result in dysfunction of the shelterin complex, interfering with its protection of telomeres and leading to reduced telomere length. Accelerated telomere shortening leads to bone marrow failure, genetic instability, and premature aging.
Inherited amegakaryocytic thrombocytopenia is characterized by severe thrombocytopenia and megakaryocyte absence at birth. Missense or nonsense mutations in the c-mpl gene are present in most patients. A high percentage of these patients subsequently develop multilineage bone marrow failure in the second decade of life.15 Shwachman-Diamond syndrome is an autosomal recessive disorder characterized by pancreatic exocrine dysfunction, metaphyseal dysostosis, and bone marrow failure.16 Similar to Fanconi anemia, there is an increased risk of developing myelodysplasia or leukemia at an early age. Hypomorphic mutations in the Shwachman-Bodian-Diamond Syndrome (SBDS) gene on chromosome 7 have been found in roughly 85% of cases.17 The SBDS gene is important for ribosome biogenesis, but how this leads to bone marrow failure is unclear. These inherited forms of aplastic anemia are described in more detail in Chapter 37. The remainder of this chapter focuses on acquired aplastic anemia, hereafter referred to as aplastic anemia.
EPIDEMIOLOGY
Incidence, Age, and Geographic Distribution
Precise estimates of the incidence of aplastic anemia are confounded by the imprecision in establishing the diagnosis. The International Aplastic Anemia and Agranulocytosis Study (IAAAS), conducted in Europe and Israel, is the largest and most comprehensive epidemiologic study of bone marrow failure.18 This prospective study (performed between 1980 and 1984) reported that the overall incidence of aplastic anemia was 2 cases per 1 million people; however, the incidence may be two to threefold higher in Southeast Asia.19
Aplastic anemia most commonly presents in children and young adults, but there is a second smaller peak in incidence after age 60.20, 21 Similar to other autoimmune diseases, certain histocompatibility locus specificities, especially HLA-DR2, are associated with an underlying predisposition to aplastic anemia.22 Although aplastic anemia has been causally associated with many agents, including drugs, benzene exposure, insecticides, and viruses, no etiologic agent can be identified in most cases.23, 24 A population-based case-control study of aplastic anemia in Thailand found that drugs were the most commonly implicated cause, but they explained only 5% of newly diagnosed cases.23
Benzene and Environmental Toxins
The medical literature is replete with case reports of aplastic anemia associated with environmental exposures, most notably benzene or radiation exposure. However, rigorous epidemiologic studies supporting an association between environmental toxins and aplastic anemia are lacking. A major confounder is that benzene and other toxins predispose people to myelodysplastic syndromes (MDS) and leukemia. Older literature was unlikely to have been able to distinguish different types of marrow failure, such as aplastic anemia, MDS, and hypoplastic leukemia, leading to an overestimation of the association between benzene and aplastic anemia. Although the magnitude of the risk remains uncertain, benzene is probably not a major risk factor for aplastic anemia in countries with modern standards of industrial hygiene. A large case-controlled study in Thailand employing modern diagnostic and epidemiologic methods found that individuals of lower economic status and younger age are at greater risk for developing aplastic anemia than their counterparts in other countries following exposure to solvents, glues, and hepatitis A. Grain farmers were also found to have a higher risk of developing aplastic
anemia (relative risk = 2.7) regardless of whether they used insecticides.19 These same investigators noted marked differences in incidence between northern and southern rural regions of Thailand and among Bangkok suburbs, implicating potential environmental factors in causing the disease.25
anemia (relative risk = 2.7) regardless of whether they used insecticides.19 These same investigators noted marked differences in incidence between northern and southern rural regions of Thailand and among Bangkok suburbs, implicating potential environmental factors in causing the disease.25
Radiation
Ionizing radiation is directly toxic to bone marrow stem/progenitor cells, and high doses (>1.5 Gy to the whole body) can lead to severe pancytopenia within 2 to 4 weeks after exposure; the LD50 has been estimated at about 4.5 Gy, and a dose of 10 Gy or greater is thought to have 100% mortality.26, 27 Although pancytopenia is common after a single high dose of radiation, an increased risk of aplastic anemia is not well documented as a delayed event from atomic bomb survivors.28 Although the principles of managing pancytopenia following radiation exposure are similar to those of aplastic anemia, it is important to recognize that the mechanism of bone marrow failure is different. Bone marrow failure in most cases of community acquired aplastic anemia is due to autoimmune destruction of bone marrow stem/progenitor cells; however, radiation-induced bone marrow failure is dose dependent and is a consequence of direct toxicity to stem and progenitor cells. Supportive care with blood transfusions, granulocyte colonystimulating factor, and antibiotics is the mainstay of therapy for radiation-induced bone marrow failure, inasmuch as autologous reconstitution will occur in most patients who survive the immediate consequences of radiation exposure.
Drugs and Chemicals
A plethora of case reports and small series have implicated drugs as the cause of bone marrow failure; however, proving a causal association in these rare idiosyncratic reactions is difficult. The more common classes of drugs implicated in causing aplastic anemia are listed in Table 38.1. Nevertheless, drugs were not found to be a common cause of aplastic anemia in two large, controlled, population-based studies.18, 29 An epidemiologic study in Thailand examined 541 patients and 2,261 controls. Exposures were determined by in-person interview. The investigators observed significantly elevated relative risk estimates for sulfonamides (5.6), thiazides (3.8), and mebendazole (3.0). Interestingly, no increased risk was associated with chloramphenicol, perhaps the most widely implicated drug in case reports; however, chloramphenicol use is this study was infrequent.29
When drugs are implicated in causing aplastic anemia, it is important to recognize that unlike agranulocytosis and drug-induced thrombocytopenia, stopping the putative drug does not usually lead to hematopoietic recovery. Most cases of drug-induced aplastic anemia lead to an idiosyncratic immune response directed against hematopoietic stem cells and are managed similarly to those with idiopathic aplastic anemia. Notable exceptions include patients who receive high doses of cytotoxic chemotherapy drugs (e.g., alkylating agents, antimetabolites, antimitotics) or rare individuals who have thiopurine methyltransferase deficiency (TPMT). TPMT catalyzes the S-methylation of 6-mercaptopurine, 6-thioguanine, and azathioprine.30 Most individuals have high or intermediate activity of TPMT; however, there are rare individuals (<0.1% of the population) with undetectable levels of TPMT. Exposure to even low dosages of 6-thioguanine, azathioprine, or 6-mercaptopurine, as used in inflammatory bowel disease and lupus, can result in severe bone marrow failure within weeks of starting the drug. Withdrawal of the drug usually leads to hematopoietic recovery in 2 to 4 weeks. Reliable polymerase chain reaction-based methods are now available for detecting the major inactivating mutations at the human TPMT locus.31, 32
TABLE 38.1 CLASSIFICATION OF DRUGS MOST COMMONLY IMPLICATED IN CAUSING APLASTIC ANEMIA | ||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||
Viruses
Viruses, similarly to drugs, are often implicated, but seldom proven to cause aplastic anemia. Viral infections, especially in chronically ill patients, often lead to transient cytopenias, but frank aplastic anemia is uncommon. These transient cytopenias can be due directly to infection and cytolysis of hematopoietic cells or indirectly through the elaboration of inhibitory cytokines. True aplastic anemia following viruses also appears to result usually from an idiosyncratic immune response directed against hematopoietic stem cells. Acute infection with Epstein-Barr virus (EBV) is often associated with peripheral blood cytopenias. Rarely, acute EBV infection can be complicated by the development of aplastic anemia.33, 34, 35 There is no convincing data that B19 parvovirus causes aplastic anemia, but this virus is often linked with aplastic anemia due to the unfortunate term “aplastic crisis,” used to describe the transient red cell aplasia and severe anemia that occurs in sickle cell anemia patients who are acutely infected with B19 parvovirus. The only known natural host cell of parvovirus B19 is the human erythroid progenitor.36 The receptor for the virus is a neutral glycolipid, globoside, also known as the erythrocyte P antigen.37 Globoside is expressed on erythroid progenitors, erythrocytes, fetal myocardium, placenta, some megakaryocytes, and endothelial cells; it is not present on hematopoietic stem cells. Other viruses, including a variety of herpes viruses and the human immunodeficiency virus have been implicated in triggering aplastic anemia, but convincing causal data are lacking. Spontaneous recovery, response to immunosuppression, and response to antiviral therapy have all been described; however, for those with severe disease, conventional therapy (immunosuppression or bone marrow transplantation) should be initiated early.
Seronegative (non-A through non-G) hepatitis precedes the diagnosis of aplastic anemia in 3% to 5% of cases and is recognized as hepatitis-associated aplastic anemia.38 After orthotopic liver transplantation for fulminant seronegative hepatitis, up to 30% of patients will develop aplastic anemia (HAA).39, 40 In most cases, the hepatitis resolves spontaneously; however, when severe aplastic anemia (SAA) follows, it is often fatal and presents within a few months after the onset of hepatitis.41 The pathophysiology of HAA is unknown, but is thought to be immune mediated because it responds to immunosuppressive therapy.41 Furthermore, patients with HAA have a skewed T-cell repertoire, and liver biopsies from these patients show lymphocytic infiltration.42
Pregnancy
Pregnancy-associated aplastic anemia is a rare entity, and despite numerous case reports, the association is not well understood.1, 43, 44
The onset of aplastic anemia can occur during pregnancy or shortly after delivery. Moreover, in women with a history of aplastic anemia who had been treated into remission with immunosuppressive therapy, there is an increased risk for relapse of aplastic anemia during pregnancy. The European Group for Blood and Marrow Transplantation performed a retrospective study on the outcome of pregnancy in 36 women who had received immunosuppressive therapy to treat aplastic anemia.45 Seven of the pregnancies (19%) were complicated by relapse of aplastic anemia. In contrast to idiopathic aplastic anemia, pregnancy-associated aplastic anemia is often associated with spontaneous remissions. However, in patients with severe disease, therapy should be initiated promptly, because maternal and fetal mortality are not uncommon.43, 44, 45
The onset of aplastic anemia can occur during pregnancy or shortly after delivery. Moreover, in women with a history of aplastic anemia who had been treated into remission with immunosuppressive therapy, there is an increased risk for relapse of aplastic anemia during pregnancy. The European Group for Blood and Marrow Transplantation performed a retrospective study on the outcome of pregnancy in 36 women who had received immunosuppressive therapy to treat aplastic anemia.45 Seven of the pregnancies (19%) were complicated by relapse of aplastic anemia. In contrast to idiopathic aplastic anemia, pregnancy-associated aplastic anemia is often associated with spontaneous remissions. However, in patients with severe disease, therapy should be initiated promptly, because maternal and fetal mortality are not uncommon.43, 44, 45
PATHOPHYSIOLOGY
Autoimmunity
Aplastic anemia was originally thought to result from a direct toxic effect on hematopoietic stem cells. In the late 1960s, Mathé and colleagues were among the first to postulate an autoimmune basis for aplastic anemia.46 After administering antilymphocyte globulin for conditioning, they performed bone marrow transplantation in aplastic anemia patients using partially mismatched donors. Although the transplanted marrow failed to engraft, some patients experienced autologous recovery of hematopoiesis, suggesting that growth and differentiation of the patient’s hematopoietic stem cells were being suppressed by the immune system. An analysis by the International Bone Marrow Transplant Registry of identical twin bone marrow transplants in aplastic anemia patients also suggests an autoimmune etiology for the majority of patients. Attempts to treat aplastic anemia by simple transfusion of bone marrow from an identical twin fails to reconstitute hematopoiesis in about 70% of patients.47 However, repeating the procedure following a high-dose cyclophosphamide conditioning regimen is successful in most patients.48
The first laboratory evidence of autoimmunity in aplastic anemia was provided by experiments showing that lymphocytes from aplastic anemia patients inhibit allogeneic and autologous hematopoietic colony formation in vitro.49 Subsequently, cytotoxic T lymphocytes were found to mediate the destruction of hematopoietic stem cells in aplastic anemia.50, 51 These cytotoxic T cells are more conspicuous in the bone marrow of aplastic anemia patients than in the peripheral blood,52, 53, 54 and they overproduce interferon-γ and tumor necrosis factor (TNF).55 TNF and interferon-γ are direct inhibitors of hematopoiesis and appear to up-regulate Fas expression on CD34+ cells.56 Immortalized CD4+ and CD8+ T-cell clones from aplastic anemia patients also secrete Th1 cytokines and are directly toxic to autologous CD34 cells.50, 51 There is also evidence for a humoral autoimmune response in aplastic anemia; autoantibodies against kinectin, a 1,300 amino acid molecule expressed on human hematopoietic cells, liver, ovary, testis, and brain cells have been found in approximately 40% of aplastic anemia patients.57 Antidiazepam-binding related protein-1 is another putative autoantibody found in some patients with aplastic anemia;58 however, the relevance of these autoantibodies to the pathophysiology of aplastic anemia is unclear. Studies in aplastic anemia patients examining T-cell diversity using complementarity-determining region (CDR3) spectratyping further implicate an autoimmune pathophysiology in aplastic anemia. T cells from aplastic anemia patients have limited T-cell receptor β-chain heterogeneity, suggesting oligoclonal T-cell expansion in response to a specific, but as yet unrecognized, antigen.51, 59
Stem Cells
A reduction in the number of hematopoietic stem/progenitor cells is a universal laboratory finding in aplastic anemia. CD34+ cells, assayable hematopoietic progenitors, and long-term cultureinitiating cells are strikingly reduced in aplastic anemia.60, 61 However, some healthy hematopoietic stem cells persist in most patients with aplastic anemia inasmuch as complete recovery of normal hematopoiesis can occur with effective immunosuppressive therapy.62, 63 T cells from aplastic anemia patients kill hematopoietic stem cells in an HLA-DR restricted manner50, 51 via Fas ligand.56 Hematopoietic stem cells represent several classes of cells with varying capacity for long-term production of the different hematopoietic lineages and variable expression of Fas ligand and HLA-DR.64 The most primitive hematopoietic stem cells express little or no HLA-DR64, 65 or Fas, 66, 67 and the expression of both HLA-DR and Fas increases as the stem cells mature. Thus, the primitive hematopoietic stem cells, which normally represent less than 10% of the total CD34+ cells, may be relatively invisible to the autoreactive T cells; conversely, the more mature hematopoietic stem cells may be the principal targets of the immune attack in aplastic anemia.68 The primitive hematopoietic stem cells eluding the autoimmune attack may be responsible for the slow hematopoietic recovery that occurs in aplastic anemia patients following immunosuppressive therapy.
Clonality and Aplastic Anemia
Clonal hematopoietic stem cell disorders such as paroxysmal nocturnal hemoglobinuria (PNH) and MDS frequently arise from aplastic anemia. Even before the widespread use of immunosuppressive therapy, 5% of patients with aplastic anemia progressed to clonal hematopoiesis. This suggests that the increase in MDS and PNH following immunosuppressive therapy is not a direct consequence of treatment. Rather, the increased survival following immunosuppressive therapy allows time for these underlying clones to develop and expand.69, 70
MDS is a clonal hematopoietic stem cell disorder that produces multilineage hematologic cytopenias (Chapter 79). It is associated with heterogeneous karyotypic abnormalities, often involving chromosomes 5, 7, or 8. Up to 15% of children and adults with aplastic anemia will develop MDS following immunosuppressive therapy, with monosomy 7 being the most common chromosomal abnormality to emerge.71, 72 PNH results from the expansion of an abnormal hematopoietic stem cell that harbors a somatic mutation of the X-linked gene, PIGA.73, 74 The PIGA gene product is required for glycosylphosphatidylinositol (GPI) anchor biosynthesis; consequently, PNH cells are deficient in all GPI-anchored proteins (GPI-AP). The GPI-APs (CD59 and CD55) protect cells from complement-mediated destruction; their absence explains the complement-mediated intravascular hemolysis associated with PNH.
Small to moderate PNH clones are found in up to 70% of patients with aplastic anemia.69, 75 Typically, less than 20% GPI-AP-deficient granulocytes are detected in aplastic anemia patients at diagnosis, but occasional patients may have larger clones. DNA sequencing of the GPI-AP-deficient cells from aplastic anemia patients reveals clonal PIGA gene mutations.76 Moreover, many of these patients exhibit expansion of the PIGA mutant clone and progress to clinical PNH. Although it was once thought that PNH evolving from aplastic anemia is more benign than classical PNH, this observation may be a consequence of lead time bias, inasmuch as many of these patients eventually develop classical PNH symptoms after the PIGA mutant clone expands. Interestingly, the PNH clone can regress, remain stable, or expand in aplastic anemia patients treated with immunosuppressive therapy; however, expansion of the PNH clone is commonly associated with relapse.77, 78
The mechanism whereby PNH clones expand is not entirely clear; however, a preponderance of data suggests that the PNH stem cell has a conditional growth advantage in the setting of aplastic anemia. Specifically, it has be suggested that PNH cells
may be relatively resistant to an autoimmune attack on the bone marrow, possibly because they are deficient in GPI-anchored UL binding proteins (ULBP) that serve as receptors for NKG2D, a ligand that is important for natural killer cells and T cells.79, 80 Alternatively, it has been proposed that “second hit” mutations may also give the PNH clone a growth advantage.81 These hypotheses are not mutually exclusive.
may be relatively resistant to an autoimmune attack on the bone marrow, possibly because they are deficient in GPI-anchored UL binding proteins (ULBP) that serve as receptors for NKG2D, a ligand that is important for natural killer cells and T cells.79, 80 Alternatively, it has been proposed that “second hit” mutations may also give the PNH clone a growth advantage.81 These hypotheses are not mutually exclusive.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree