Neoplasms of the small intestine, vermiform appendix, and peritoneum and carcinoma of the colon and rectum
Georgia M. Beasley, MD  Zhifei Sun, MD
Zhifei Sun, MD  Daniel P. Nussbaum, MD
Daniel P. Nussbaum, MD  Douglas S. Tyler, MD
Douglas S. Tyler, MD
Overview
Cancers of the small bowel, large bowel, and appendix compromise a multitude of distinct pathologic entities and clinical presentations. While tumors of the small bowel are uncommon with <3% of all alimentary tract tumors and 0.4% of all malignancies arise in the small bowel, colon cancer is the third most common malignant tumor and the fourth most common cause of cancer death worldwide. Although adenocarcinoma remains the common pathology, many advances have been made regarding our diagnoses and management of carcinoid tumors and even to a larger degree in gastrointestinal stromal tumors. Additional advances include our understanding of genetics, new imaging modalities, and minimally invasive surgeries. This chapter will provide a comprehensive review of the management and treatment of cancers of the small bowel, large bowel, and appendix.
Tumors of the small intestine
The estimated number of new small bowel malignancies in the United States was 9160 in 2014. The small intestine represents 75% of the total length of the gastrointestinal (GI) tract and comprises 90% of its mucosal surface area, yet rarely does this region develop malignant tumors.1 Recent figures show that <3% of all alimentary tract tumors and 0.4% of all malignancies arise in the small bowel.2
Several mechanisms have been postulated to explain the low incidence of neoplastic transformation within the small intestine. The most important of these are the rapid transit of content through the small bowel, which provides a shorter exposure of its mucosa to carcinogens, increased lymphoid tissue in the small intestine with a high level of immunoglobulin A (IgA) expression, and a lower bacterial load in the small bowel that results in a decreased conversion of bile acids into potential carcinogens by anaerobic microorganisms.3, 4 In addition, the liquid contents of the small bowel may cause less mucosal irritation than the more solid contents of the large intestine, and there is the presence in the small intestine of mucosal detoxifying enzymes such as benzopyrene hydroxylase.5
Adenocarcinomas comprise 30% to 50% of small bowel malignant tumors, followed by carcinoids (25–30%), lymphomas (15–20%), and, to a lesser extent, sarcomas. Leiomyomas account for 25% of all benign tumors, while others include adenomas and lipomas and rarer neoplasms such as fibromas, fibromyxomas, neurofibromas, ganglioneuromas, hemangiomas, and lymphangiomas.6
Clinical presentation
Because the small intestine is relatively inaccessible to routine endoscopy, diagnosis of small intestinal neoplasms is often delayed for months after onset of symptoms. Many small bowel tumors are asymptomatic until late in their course because of their relatively slow growth and the ease with which the liquid contents of the small bowel can pass even a partially obstructing lesion.6 The remainder are usually found as a result of the symptoms of partial obstruction: nausea and vomiting if the lesion is proximal, as well as crampy abdominal pain, or other nonspecific findings such as weight loss. Hemorrhage is frequently found in those tumors that penetrate beyond the submucosa, but almost always is occult, presenting as microcytic anemia or stool that is positive on guaiac testing. Certain small bowel tumors have more specific presenting symptoms, such as jaundice (ampullary carcinoma) and fever, diarrhea, and weight loss (lymphoma). Endocrine tumors of the gut, the most common of which are carcinoid tumors, may present with their own set of classic symptoms, such as flushing, diarrhea, cyanosis, and intermittent respiratory distress. Only a small proportion of patients with carcinoid tumors have these symptoms, the vast majority being asymptomatic or having symptoms secondary to mass lesion effects.
Eventually, malignant tumors cause enough symptoms for the ensuing medical work-up to reveal the tumor. Unfortunately, some time may pass between the first symptom and diagnosis. In one series, almost one-third of the patients had symptoms for 5 years or more prior to definitive diagnosis.7 Another study demonstrated a mean duration of symptoms of 7 months prior to diagnosis.8 Many patients eventually diagnosed with small bowel tumors present as an emergency with either bowel obstruction or perforation.
Diagnostic imaging
Radiographic studies often aid in the diagnosis of these lesions, especially in advanced disease. However, such studies, on many occasions, are not useful for early diagnosis of curable malignancy. Small bowel radiology has undergone dramatic changes in the past 2 decades. Plain films, the small bowel follow-through, and double-contrast modality of enteroclysis may be useful in certain situations but have largely been replaced by cross-sectional imaging techniques (computed tomography (CT) and magnetic resonance imaging (MRI)), which can be used to investigate both extraluminal abnormalities and intraluminal changes. CT scanning with oral contrast has led to nearly 100% recognition of small bowel tumors in some series, although it has limited ability to differentiate among tumor types.9 This modality appears to be most useful for preoperative staging and metastatic evaluation.10 In one series, the sensitivity for CT in determining T (tumor) stage was 57%, compared with 61% and 42% for colon and gastric cancers, respectively.11, 12 MRI techniques clearly highlight endoluminal, mural, and extramural enteric details and provide vascular and functional information, thereby enhancing the diagnostic value of these techniques in small bowel diseases. MRI offers detailed morphologic information and functional data of small bowel diseases and provides reliable evidence of normalcy, thereby allowing the diagnosis of early or subtle structural abnormalities and guiding treatment and decisions in patient care. MRI has many properties that make it ideal for imaging of the small bowel: the ability to perform real-time imaging, functional imaging, the lack of ionizing radiation, and the improved tissue contrast that can be achieved by using a variety of pulse sequences.13–15 Magnetic resonance (MR) enteroclysis has yielded a 96.6% accuracy in the detection of small bowel neoplasms.16, 17 In addition to CT and MR, angiography and nuclear scanning may be useful in the case of a bleeding tumor or a suspected hemangioma. Endoscopic ultrasonography (EUS) is used to detect and stage small bowel tumors and allows real-time interventional diagnostic procedures, mainly in the periampullary region. EUS has been shown to be superior to CT and MRI in predicting vascular invasion and overall assessment of T stage of ampullary neoplasms.18, 19 In the past decade, small bowel endoscopy has become increasingly useful as a diagnostic tool. There are three main types of small bowel endoscopy: push enteroscopy, intraoperative or laparoscopically assisted enteroscopy, and, most recently, double-balloon enteroscopy. Push enteroscopy involves an intestinal intubation of a 220- to 250-cm instrument, usually with fluoroscopic assistance, and can be used to examine the jejunum for mean lengths of 120 cm beyond the ligament of Treitz.20 During intraoperative endoscopy, the surgeon manually manipulates through the small bowel wall with either a push endoscope (anterograde) or a colonoscope (retrograde) to examine the entire small bowel. The surgeon can mark the lesions of interest, usually by suture, and resect at the completion of the enteroscopy. These techniques are particularly useful in prophylactic polypectomy of small bowel large polyps (>15 mm) for conservative approach in management of PJS patients.21 The recent addition of laparoscopically assisted enteroscopy provides a less invasive technique than interoperative enteroscopy but still requires general anesthesia and both a surgeon and endoscopist.22 In double-balloon enteroscopy, an endoscope and a soft flexible overtube, each of which has an inflatable balloon attached to its distal end, are employed together. The two tubes are advanced over one another repeatedly using alternating inflation of the balloons to hold position, allowing deep advancement into the small intestine. The entire small intestine can be examined using this method with less discomfort than experienced with the push method.23 After receiving the Federal Drug Administration (FDA) approval in 2001, a small, swallowable imaging capsule was introduced by Swain and colleagues that is propelled by peristalsis through the intestinal tract and transmits data to a receiver that captures video images.24 However, the use of capsule endoscopy to evaluate small bowel tumors, particularly submucosal forms, has several limitations.25, 26 Indeed, capsule endoscopy may fail to depict neoplastic disease in as many as 18.9% of cases,27 and capsule retention occurs in 10–25% of small bowel tumor cases.27, 28
Treatment
The treatment of small bowel tumors is generally surgical, with simple resection for benign lesions and an aggressive approach for malignant lesions. Overall, the survival for adenocarcinomas, carcinoids, lymphomas, and sarcomas was better in 328 cases from a population-based registry than that for all other organs, except the breast, colon, prostate, and uterus.29 In rare cases, radiation or chemotherapy may precede surgery. Duodenal tumors may require pancreaticoduodenectomy if malignant, whereas tumors of the terminal ileum may require right hemicolectomy to ensure complete resection and adequate margins.
Malignant neoplasms of the small bowel
Adenocarcinomas
Adenocarcinomas are the most common malignant tumors in the small bowel, accounting for approximately 30–50% of all malignant small bowel tumors.30, 31 They most commonly arise in the seventh decade of life and are seen slightly more often in men than in women.32 Cohort studies suggest that increased body mass index and alcohol use may increase risk of small bowel cancer.33 While primary tumors arise most often in the duodenum (48–52%) and jejunum (23–25%) and less commonly in the ileum (13–16%), the reason for this distribution is unclear.34, 35 Some have postulated that the richness of IgA-secreting cells in the ileum accounts for its relative sparing from adenocarcinoma by neutralizing luminal carcinogens.4 Others have noted that the abundance of the enzyme benzopyrene hydroxylase may play a protective role by detoxifying potential carcinogens.36 Adenocarcinoma is staged using the American Joint Committee on Cancer (AJCC) TNM system, and as expected small bowel carcinomas that are well differentiated with only local invasion and no lymph node metastasis tend to have the best prognosis. Unfortunately, little progress has been made in the treatment of small bowel adenocarcinoma. There have been improvements in diagnostic modalities and insights into the molecular basis, but the prognosis is still generally poor.
The histogenesis of small bowel adenocarcinoma most likely follows the adenoma–carcinoma sequence described initially for large bowel cancer.37 As a result, the single most important risk factor for small bowel adenocarcinoma is preexisting adenoma, either single or multiple, as associated with multiple polyposis syndromes.38 Small bowel adenocarcinomas have also been associated with alcohol (but not tobacco), nontropical sprue, regional enteritis, celiac disease, and urinary diversion procedures such as ileal conduit.39–43
Familial adenomatous polyposis (FAP) is known to be a powerful risk factor for adenocarcinoma, with small bowel cancer being the most common cancer after colon cancer itself.44 The relative risk (RR) of small bowel carcinoma in these patients has been described as being greater than 100.45 Other hereditary syndromes associated with small bowel tumors include Peutz–Jeghers (PJ) syndrome (increased incidence of hamartomatous polyps in the jejunum and ileum), Gardner syndrome (adenoma and adenocarcinoma), and von Recklinghausen disease (paraganglioma). Small bowel inflammatory disorders are associated with increased malignancy, including, most notably, Crohn’s disease.46 Crohn’s disease is a risk factor for future small bowel adenocarcinoma. An RR of 33 (95% CI: 15.9–60.9) was reported in a 2006 meta-analysis.47 As with ulcerative colitis (UC) and tumors of the colon, the diagnosis of Crohn’s disease precedes small bowel tumors by about 10 years. Several risk factors have been identified in patients with Crohn’s disease who develop adenocarcinoma of the small bowel: duration of Crohn’s disease, male gender, fistulization, presence of strictures, and surgical creation of blind excluded loops of intestines.48, 49 Other disorders associated with increased risk of malignancy are celiac disease (lymphoma and adenocarcinoma) and immunoproliferative disease (diffuse intestinal lymphoma and immunoproliferative small intestinal disease.5
Celiac sprue, while well known to predispose to intestinal lymphoma, is also associated with adenocarcinoma of the small bowel.40 The numbers cited in case reports are few, but the presence of disease in otherwise noncharacteristic locations seems to lend credence to the theory that gluten-mediated jejunoileitis is also an independent risk factor for the development of adenocarcinoma of the small bowel as well as lymphomas.31 Adenocarcinoma of the small intestine, often aggressive, can affect children and is usually associated with degeneration of a PJ hamartoma.38
The genetic mechanisms involved in the carcinogenesis of the small bowel remain unknown, most likely because of the small number of cases. Blaker and colleagues from Germany showed that although small intestinal carcinomas reveal complex genetic changes, a significant number of tumors share karyotypic instability and losses of chromosome 18q21-q22. 18q deletions often target the SMAD4 gene and disrupt tumor suppression through TGFβ-signaling.50 Svrcek and colleagues, using tissue microarray analysis, determined that inactivation of the SMAD4/DPC4 gene is involved in small intestinal adenocarcinoma tumorigenesis and that overexpression of TP53 and abnormal expression of β-catenin are two common events in small intestinal adenocarcinoma.51 Other pathways include Notch3 signaling associated with MUC5AC expression.52 There is also recent evidence suggesting DNA mismatch repair genes are involved; the frequency of the dMMR phenotype is variable, ranging from 5% to 35% of cases.53
Symptoms of adenocarcinoma of the small bowel range from obstructive symptoms, such as vomiting and jaundice for those with duodenal tumors, to indistinct abdominal pain, weight loss, and anemia for more distal lesions. Weight loss is also common, occurring in more than 50% of patients. Obstruction is found in 40% to 70% of patients prior to presentation. In the collected Mayo series, 71% of patients had either overt or clinical evidence of blood loss.54 Adenocarcinomas, especially duodenal tumors, usually become symptomatic earlier than other small bowel tumors, allowing for earlier diagnosis and intervention. Despite this, 30–35% of small bowel adenocarcinomas are metastatic at the time of diagnosis.34, 35
In a recent study conducted by the American College of Surgeons on 5000 small bowel adenocarcinomas, the overall 5-year disease-free survival (DFS) was 30.5%.55 The median survival in this series was 19.7 months. The primary treatment of adenocarcinomas is wide surgical resection, with removal of lymph nodes and the vascular pedicle. Margins of 5 cm are considered acceptable. Recent reports indicate that even this treatment does not yield good survival rates for node-positive patients. In a recent study examining 217 patients with small bowel adenocarcinoma followed over a 10-year period at MD Anderson Cancer Center, patients with stage IV disease had a shorter 5-year overall survival (OS) than those with I–III disease (5% vs 36%).35 The 5-year survival was significantly shorter if the positive lymph node ratio (number of positive lymph nodes/number of total lymph nodes) was greater than 75% versus <75% (12% vs 51%).
All attempts should be made to resect the primary lesion to prevent mucosal bleeding. For patients deemed unresectable at the time of laparotomy, some have advocated the use of intraoperative radiation therapy.56–58 The lack of clinical trials makes this therapy difficult to recommend in a setting other than specialized centers. Data regarding the role of adjuvant chemotherapy are limited, with no evidence of significant benefit in survival in patients with adenocarcinoma of the small intestine treated with adjuvant chemotherapy. An attempted Cochrane review in 2007 failed to find any studies eligible for meta-analysis.59 Despite this, adjuvant chemotherapy is frequently used because small bowel cancer tends to recur systemically, similar to CRC, and because colon cancers respond to adjuvant therapy. A 2009 retrospective multicenter study suggested that an adjuvant folinic acid, 5-FU, and oxaliplatin (FOLFOX) regimen prolonged OS by around 5 months compared to patients treated with other regimens, but the findings of this small study were not statistically significant.53 For advanced unresectable disease, a recent phase II study of modified FOLFOX as first-line chemotherapy in advanced small bowel adenocarcinoma reported an objective response rate of 48.5% [95% confidence interval (95% CI): 31–67%], with one complete response in patients with advanced small bowel adenocarcinomas.60
Carcinoid tumors
Carcinoid tumors represent approximately 25–30% of malignant tumors of the small bowel.58, 61 Obendorfer used the term “karzinoide” in 1907, but the exact nature of the tumor was not determined until 1928 when Masson described its origin as the chromaffin cell.62, 63 The frequency of carcinoid in large autopsy series, before the era of increased detection by CT and endoscopy, indicated that about 85% were undiagnosed during life.64 US data show that the incidence of GI carcinoid has increased at a rate of 3%–10% per year over the past three decades.64, 65 The most frequent sites for carcinoids were the GI tract (54.5%) and the bronchopulmonary system (30.1%). Within the GI tract, most occurred in the small bowel (44.7%), rectum (19.6%), and appendix (16.7%). In contradistinction to adenocarcinoma, the carcinoid tends to arise in the distal small intestine rather than in more proximal sites. In the series reported by Moertel, all surgically confirmed, 3% were in the duodenum, 5% in the jejunum, 32% in the proximal ileum, and 60% in the distal ileum.66 The median age at discovery is 60.9 years, and females constitute 54.2% of patients.67 The overall 5-year survival rate for patients with GI carcinoid is about 58%, with little change over the past 30 years.64 However, in the subgroup of patients with well-differentiated carcinoid with distant spread, the 5-year survival rate has improved from 15% to 52% over this time period.64
The most useful marker of neuroendocrine cells in tissue sections is chromogranin A (CgA), a glycoprotein stored in secretory granules of neuroendocrine cells. Plasma CgA levels correlate with tumor burden and may be useful for monitoring treatment.68 Twenty-four-hour measurement of urinary 5-hydroxyindole-3-acetic acid (5-HIAA), the degradation product of serotonin, can also aid in diagnosis. The specificity of 5-HIAA as a marker for these carcinoids is 88%, although tryptophan/serotonin-rich foods (bananas, avocados, plums, eggplants, tomatoes, plantains, pineapples, and walnuts) can provide false elevations, and several drugs can result in increased or decreased 5-HIAA levels.69 Higher concentrations of 5-HIAA in urine are consistent with a worse prognosis, while persistently low levels predict a more favorable outcome in disseminated disease.68 Mitotic count and Ki-67 index [a marker of cell proliferation] provide some indication of prognosis.68
A unique feature of carcinoid tumors is their ability to produce a variety of protein and peptide products, the most characteristic of which is serotonin. Systemic serotonin is thought to cause most of the symptoms of the carcinoid syndrome, including diarrhea, flushing, wheezing, and right-sided heart disease. Carcinoid syndrome is seen in 5–7% of patients with large tumor burdens and metastatic disease.54 It is believed that the metastatic component is necessary to ensure drainage of the compounds involved in the syndrome into the systemic circulation and to provide an adequate tumor mass to produce large amounts of peptidergic products.
The clinical manifestations of carcinoid are often vague or absent, and the definitive diagnosis is often not made prior to surgery. Patients with small intestine carcinoid often present at a late stage, and the prognosis is poor once tumors have spread beyond the intestine. In a series of 145 patients with GI carcinoid tumors, only 12 had a proper diagnosis before surgery, and those 12 had definite symptoms of carcinoid syndrome.54, 70 Most often, patients are operated on for signs of bowel obstruction, not by the tumor itself but by a desmoplastic reaction that leads to shrinking of the mesentery as a result of fibrosis and kinking of the bowel.71 Scintigraphy with radiolabeled octreotide has been successfully used to localize undetected primary and metastatic lesions.72 Two large European studies show carcinoid lesion detection with a sensitivity of 89% by using this diagnostic tool.73
The metastatic potential of a carcinoid tumor correlates closely with its size. In the Moertel series, there were no metastases in tumors <0.5 cm in diameter, 15% in tumors 0.5 to 0.9 cm in diameter, 72% in tumors 1.0 to 1.9 cm in diameter, and 95% metastases in tumors larger than 2 cm.66 However, small bowel carcinoids may still metastasize when <1 cm. Recent evidence based on 5-HIAA levels suggests that most cases of metastatic carcinoid of unknown primary probably arise from small ileal tumors.74, 75 Extent of disease, which mainly comprises either lymph node (regional) or liver (metastatic) involvement, is a definite predictor of outcome. In Maggard’s analysis of 11,427 carcinoids, 5-year survival for localized, regional, and distant disease of the small intestine was 70.4%, 64.1%, and 32.4%, respectively.65
Primary surgical resection of the tumor and regional lymph nodes is the only curative treatment for GI NETs; this is usually possible in about 20% of patients. Surgery remains the only approach that allows definitive histopathologic staging, resection of occult lymph node metastasis, and prevention of local complications caused by a desmoplastic resection.76 Referral for surgical management should not be influenced by the inability to localize the primary tumor. As midgut tumors are difficult to localize on imaging, one study found the primary tumor could be identified intraoperatively in a majority of patients with metastatic NETs, irrespective of preoperative localization status.77 Careful intraoperative examination is mandatory, because most series report that 30% of these tumors are multicentric.66 Primary duodenal carcinoids account for only 2.6% of carcinoid tumors in the United States; although they are increasingly recognized with the more widespread use of upper GI endoscopy.78 Because of the rarity of this disease, management recommendations for duodenal carcinoids have been extrapolated from the experience with midgut and hindgut carcinoids. A recent study by Mullen and colleagues however demonstrated successful margin negative endoscopic resection in six patients with tumors <1.5 cm.78 Interestingly, this study found lymph node metastases to be present in 54% of patients with duodenal carcinoid, including two patients with tumors smaller than 1 cm and limited to the submucosa. The impact of lymph node metastasis in duodenal carcinoids is uncertain, however, in that no patient developed distant metastases or carcinoid syndrome in this series. In the case of advanced disease, there may be some benefit to debulking procedures, but this remains controversial, because the absolute size of the tumor does not correspond well with the degree of symptoms.54, 79, 80 Some authors recommend aggressive treatment even in patients with widely metastatic disease, including resection of all intra-abdominal tumor deposits, segmental liver resection as needed, and hepatic arterial embolization. Cholecystectomy also has been performed to prevent gallbladder necrosis during hepatic embolization. Although it has not been proven whether this aggressive surgical approach increases survival, it has yielded biochemical remission in up to 25% of patients and regression of hepatic metastases for long periods.69, 81 In the MD Anderson experience of 81 patients with carcinoid disease metastatic to the liver who underwent hepatic artery embolization or chemoembolization, 67% experienced a partial response with a mean duration of response of 17 months. Overall, 63% of patients had reduction in their tumor-related symptoms and the OS time was 31 months.82 Importantly, many patients diagnosed with carcinoid have other malignancies. Using the surveillance, epidemiology, and end results (SEER) database to identify patients diagnosed with small intestine carcinoids between 1973 and 2007, almost one-third of patients with small bowel carcinoid had an associated metachronous primary tumor. The most common sites were prostate (26.2%), breast (14.3%), colon (9.1%), lung/bronchus (6.3%), and bladder (5.3%).83
Medical therapy in the form of somatostatin analogues is effective in relieving symptoms of the carcinoid syndrome, though demonstrated tumor regression is rare. Octreotide is an eight amino acid, long-acting somatostatin analogue that binds to receptor subtypes 2, 3, and 5 and has been widely used for both detection and treatment of carcinoid tumors.84 The currently available SSAs—Sandostatin LAR (octreotide; Novartis) and Somatuline Autogel (lanreotide; Ipsen)—display high-affinity binding for receptor subtypes 2 and 5, low affinity for subtypes 1 and 4, and medium affinity for subtype 3. SOM230 (pasireotide; Novartis), a more recently developed SSA, now in phase III trials, has a wider range of activity against somatostatin receptors and may offer a therapeutic advantage, especially in resistant disease.85 In one study, octreotide was delivered subcutaneously at a dosage of 150 µg three times a day, showing improved symptoms in 88% of patients and decreased urinary 5-HIAA in 72% of patients.86 Advances in the understanding of the mechanisms underlying tumor progression have led to the identification of several potential therapeutic targets (including the vascular endothelial growth factor (VEGF) and mammalian target of rapamycin (mTOR) signaling pathways). In a randomized phase 3 trial of everolimus plus octreotide LAR compared with placebo plus octreotide LAR improved progression-free survival in patients with advanced neuroendocrine tumors. However, progression-free survival was still poor at 16.4 (95% CI 13.7–21.2) months in the everolimus plus octreotide LAR group and 11.3 (8.4–14.6) months in the placebo plus octreotide LAR group.87 Several other agents are being studied, including the use of novel SSTa, VEGF and mTOR inhibitors, and agents that interfere with insulin growth factor 1 receptor and AKT signaling. Another treatment modality is peptide receptor radionuclide therapy. Peptide receptor radionuclide therapy delivers tumoricidal doses of radiation to carcinoid cells highly selectively, with few adverse effects (nausea and occasional bone marrow and renal toxicity). By linking a radioactive isotope (111Indium, 90Yttrium, or 177Lutetium) to a somatostatin analogue, carcinoid cells, with their often high density of somatostatin receptors, may be specifically targeted. Tumor regression rates of up to 50%, with a disease-free response approaching 3 years, have been reported in some studies.88
Prognosis of patients with carcinoid disease varies according to several factors. Size of the primary tumor is an important predictor of metastasis and survival. Carcinoid tumors >2 cm in diameter portend a worse prognosis than those <2 cm.89 In a recent series of 603 patients, lymph node metastasis was also not surprisingly prognostic.90 In the Maggard series, increased tumor size was associated with a greater likelihood of lymph node involvement.67 In the carcinoid series at Duke University, a direct correlation was found between size of the primary tumor and extent of disease at presentation.91 In addition, after controlling for stage of disease, region of origin of primary tumor predicted prognosis in this series of patients. In patients with distant metastases at presentation, those with midgut tumors had markedly better prognosis than did patients with foregut or hindgut tumors. In addition to traditional pathologic determinants, expression of cocaine- and amphetamine-regulated transcript (CART) in small bowel carcinoid tumors is associated with worse survival.92
Composite tumors, those that display characteristics of both carcinoid tumors and adenocarcinomas, are well described in the appendix but are less well known in the small intestine. These tumors are relatively rare, with most reports to date encompassing only one or two cases. They are aggressive tumors with a metastatic potential similar to that of adenocarcinoma and should be treated as adenocarcinomas. Lymphatic metastasis appeared histologically to be adenocarcinoma in two cases and carcinoid in one; thus, it seems that these tumors may arise from cells with pluripotential patterns of differentiation.93
Gastrointestinal stromal tumors
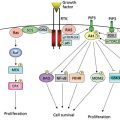
Gastrointestinal stromal tumor (GIST) is the current nomenclature for a diverse group of benign or malignant GI neoplasms derived from embryonic mesoderm. There are three histologic subtypes of GIST. The spindle cell form is the most common (70%) and consists of uniform, intersecting fascicles with eosinophilic cytoplasm. The epithelioid (20%) and the rare mixed type (10%) forms show more rounded cells with nuclear atypia.94 Malignant GISTs constitute 15–20% of the malignant tumors found in the small bowel.95 The annual incidence in the United States is reported to be approximately 5000 cases per year which seems to be rising due to increased awareness and histopathologic diagnosis.96, 97 GISTs affect men and women equally.98 Most patients diagnosed with GIST are between 40–80 years old with a median age at diagnosis of 60.99 The most commonly encountered GIST is the sporadic form. Familial GISTs occur and result from a germline mutation in either the KIT or platelet-derived growth factor receptor alpha (PDGFRα) proto-oncogenes.100, 101 The cellular origin of GIST is proposed to be the interstitial cell of Cajal, an intestinal pacemaker cell.95 GISTs are characterized by mutations in the proto-oncogene C-kit that lead to constitutive activation of its glycoprotein product KIT and the subsequent tyrosine kinase activity.102 The tyrosine kinase inhibitor, imatinib, has revolutionized the treatment of GIST tumors. More than 95% of GISTs express KIT and biochemical evidence of KIT can be found in almost all GISTs.103 The most common sites of KIT mutation include exon 11 (70%) and exon 9 (10%) although other regions have been described.104, 105 Other commonly expressed markers include CD34 (70%), smooth muscle actin (30%), and desmin (<5%).106 Because other malignancies can stain positive for KIT include metastatic melanoma, angiosarcoma, and Ewing’s sarcoma, IHC alone is not sufficient for diagnosis.94 The diagnosis of GIST is based on both morphology and IHC. GIST can also occur in patients with neurofibromatosis type-1 (NF1) and in young women as part of a syndrome that includes, paragangliomas, pulmonary chondromas, and gastric GISTs.107, 108
GISTs can occur anywhere in the GI tract from the esophagus to the rectum. Stomach represents the most common site (60%), followed by the small bowel (30%), rectum (∼5%), and esophagus (∼5%).99 Up to 50% of patients will present with metastatic disease at the time of diagnosis, with the liver and peritoneum being the two most common sites.109 Most GISTs present as an abdominal mass causing bowel obstruction evidenced as nausea, vomiting and abdominal pain, or as GI bleeding. GISTs usually grow rapidly, with masses 5 cm in diameter or greater being common.110 This rapid rate of growth explains the propensity for GI blood loss, because these tumors may outgrow their blood supply, become necrotic, and ulcerate. Blood loss is usually chronic, with laboratory studies revealing a microcytic anemia.110 Fistulas and abscesses are also caused by tumor necrosis. The primary mode of diagnosis and assessment of extent of disease is by contrast-enhanced CT scan of the abdomen and pelvis. Characteristic findings on CT scan include an enhancing, exophytic mass in close association with the stomach or bowel wall. Like other sarcomas, GISTs tend to displace rather than invade adjacent structures. While positron emission tomography (PET) is not used to diagnose GIST, it can be used to assess the response to tyrosine kinase therapy. GIST appears as a submucosal mass on endoscopic evaluation. Endoscopic or percutaneous biopsy is recommended in cases in which neoadjuvant therapy is planned or metastasis is suspected.111
The primary treatment of GIST is surgical resection with wide margins. However, there is current debate about the management of tumors <2 cm. Current National Comprehensive Cancer Network (NCCN) guidelines for the management of gastric GISTs <2 cm without high-risk features on EUS include surveillance endoscopy every 6–12 months.112 For tumors >2 cm, surgical resection included en bloc resection when other organs are involved is advocated. Because lymph node involvement is not common, extensive lymphadenectomy appears to provide no added survival benefit. The role of laparoscopy in the management of patients with GIST continues to expand. Those undergoing laparoscopic resection of GIST up to 8 cm at MSKCC had equivalent perioperative and oncologic outcomes when compared with case-matched controls undergoing open resection.113 With a median follow-up of 34 months, oncologic outcomes were similar with no positive microscopic margins and one recurrence in each group. Bischof et al. also reported that a minimally invasive approach for gastric GIST was associated with low morbidity, and a high rate of R0 resection, based on their review of nearly 400 patients undergoing surgical resection for GIST.114 Periampullary GIST tumors of the duodenum represent a more challenging surgical approach. A meta-analysis demonstrated that local resection should be the procedure of choice for duodenal GIST whenever technically feasible, because it is associated with good oncologic outcomes and lower morbidity compared with pancreaticoduodenectomy (PD). The use of imatinib in patients with duodenal GIST may potentially allow a proportion of patients who would otherwise require a PD to undergo local resection instead.115
Even after surgical resection, may tumors recur. One study analyzing 200 cases of GIST over a 16-year period found that in patients with primary disease who underwent complete resection of gross disease, the 5-year actuarial survival rate was 54%.99 Even with complete surgical resection, the majority of tumors recurred, often involving the liver and peritoneal surface. In the largest series of GIST recurrences, the group from Memorial Sloan Kettering Cancer Center retrospectively analyzed 69 such patients.99 Local recurrence was seen in 76% of patients, of which half had synchronous liver lesions. Surgical resection for recurrent disease was completed in one-third of cases with median survival of 15 months. The advent of tyrosine kinase inhibitors has revolutionized treatment of GIST. Although the mechanism of tumor response was believed to be predominantly inhibition of KIT-driven cells, recent data suggest the immune system contributes substantially to the antitumor effect. Imatinib therapy was shown to induce regulatory T cell apoptosis within the tumor by reducing tumor cell expression of the immunosuppressive enzyme indoleamine 2,3-dioxygenase.116 This data is critical to devising future treatment strategies that may involve immune modulators to increase response.
Due to high recurrence rates, adjuvant imatinib has been explored in several trials. There have been two American College of Surgeons Oncology Group (ACOSOG) trials looking at the role of adjuvant imatinib mesylate after resection for those patients at intermediate or high risk of recurrence. ACOSOG Z9000 was the first phase II trial studying the efficacy of adjuvant imatinib following complete resection of GIST at high risk of recurrence.117 Patients underwent complete gross resection of a KIT-expressing primary GIST that was at high risk of recurrence (tumor size >10 cm, tumor rupture, or <5 peritoneal metastases). Following resection, patients received oral imatinib 400 mg/day for 1 year. At a median follow-up of 4 years, the 1-, 2-, and 3-year OS rates were 99%, 97%, and 97%, respectively. The 1, 2, and 3-year recurrence-free survival rates were 94%, 73%, and 61%, respectively. These results compared favorably with historical controls for both recurrence-free survival and OS. ACOSOG Z79001 was a follow-up phase III trial in which patients were randomized to 1 year of oral imatinib or placebo following resection.118 Imatinib taken once a day for 1 year following surgery for localized, primary GIST (≥3 cm) was compared with placebo in 713 patients. Recurrence-free survival was significantly higher in the imatinib arm (98%) when compared with the control group (83%) while there was no difference in OS. Subsequently, disease survival was found to be longer with 3 years versus 1 year of adjuvant imatinib.119 However, only a few percent of low-risk patients developed recurrence, and more than 70% of patients appeared to be cured by surgery alone based on recurrence-free survival in the placebo arm. Thus, the value of adjuvant imatinib in patients with resected primary GIST 3 cm should be considered carefully. Risk stratification systems can be used to identify patients who have a low likelihood of recurrence in whom adjuvant therapy is not indicated; risk stratification can also identify patients who should get therapy.120 For example, patients with KIT exon 11 deletions assigned to 1 year of adjuvant imatinib had a longer regression-free survival.121 Furthermore, specific mutations have been found to be resistant to imatinib; patients with PDGFRA D842V mutations do not respond to imatinib. Another risk stratification score showed that patients with nongastric GIST with a high mitotic count are at a particularly high risk for recurrence.121
The future focus of research for the use of adjuvant imatinib is which patients should be treated and what is the optimal duration.122 The PERSIST5 trial is an ongoing phase II trial testing 5 years of adjuvant imatinib therapy in patients at moderate to high risk of recurrence (NCT00867113). Expert opinion suggests that currently mutation testing of the tumor should be performed to exclude patients with a PDGFRA D842V mutation or wild-type tumor. In the remaining patients, a discussion should ensue about the goals and current results of adjuvant therapy.123
The role of neoadjuvant imatinib in the setting of locally advanced disease has been investigated. Neoadjuvant imatinib mesylate holds much promise because it can lead to marked shrinkage in tumor size, which can frequently be predicted within 2 to 4 weeks of initiating therapy using PET scans. The cytoreductive potential of imatinib in the preoperative setting may enable surgeons to obtain R0 resections with less extensive resections. This is most applicable to GIST tumors near the gastroesophageal junction, ampulla, and in the rectum. Recent results from a phase II trial led by the Radiation Therapy Oncology Group (RTOG) revealed that imatinib is well tolerated in the neoadjuvant setting.124 The groups were divided into whether disease was locally advanced and >5 cm (Group A) or recurrent/metastatic and >2 cm (Group B). Imatinib administered at 600 mg per day for 8 weeks preoperatively was followed by surgery and an additional 2 years of imatinib. Response rates after 8 weeks of preoperative imatinib were similar between groups A and B (4–7% partial response, 83–90% stable disease, and 4–5% progressive disease).124 Another phase II trial from MD Anderson Cancer Center investigated either 3, 5, or 7 days of neoadjuvant imatinib in 19 patients.125 This regimen was tolerated well and response rates by FDG-PET were 69%. The duration of neoadjuvant therapy and patient selection remain to be defined. Current NCCN guidelines suggest that in patients on neoadjuvant imatinib, once two successive CT scans fail to show any radiographic response, surgical resection should be considered.112
In the metastatic setting, there is strong evidence of the effectiveness of imatinib mesylate. Up to 80% of patients with metastatic GIST attain a partial or complete response with imatinib.118 A recent meta-analysis of two, large, randomized studies126, 127 comparing the efficacy of imatinib given either once (400 mg) or twice daily revealed that the higher dose confers a progression-free survival advantage among patients with exon 9 mutations.128 The second-line agent for patients with imatinib-resistant disease is sunitinib.129 Sunitinib targets KIT and PDGFRα, as well as the vascular endothelial cell growth factor receptor (VEGFR). In patients with advanced disease resistant to imatinib, sunitinib is a safe and effective second-line agent.130 Molecular studies suggest that imatinib is most effective in patients with exon 11 C-kit tyrosine kinase mutations, and sunitinib may be more effective in patients with exon 9 mutations.128 Other studies have recently been completed examining third-line agents. Regorafenib was shown to significantly improve progression-free survival compared with placebo in patients with metastatic GIST after progression on standard treatments.131 Although a relatively rare clinical entity, the treatment of GIST is continually evolving and represents an area of active developments.
Lymphoma
Lymphoma accounts for 15–20% of all malignant small bowel tumors.132 The stomach is the most common site of GI lymphoma (>60%), followed by an equal distribution between the large and small intestines.133 There is a slight male predominance of approximately 1.5 : 1, and the median age is lower than that of persons with other small bowel tumors (49 years in one large series).134, 135 Lymphomas are the most frequent malignant neoplasms in transplant recipients, appearing on average 20 months after the initiation of cyclosporine.135 Prognosis is better than for other forms of intestinal lymphomas with two-thirds cured with resection, radiotherapy, acyclovir, and reduction of immunosuppression.136, 137 Small bowel lymphomas also occur in AIDS. Virtually all lesions are B lymphocyte in origin. The prognosis is poor but is dominated by the HIV-related disease such that life expectancy for these patients is not significantly inferior to similar HIV-positive patients without lymphoma.136
The clinical presentation of GI lymphoma includes abdominal pain, nausea, vomiting, fatigue, weight loss, and GI bleeding, which may be occult. A mass with bulky adenopathy on CT scan is highly suggestive of abdominal lymphoma.138 Multiple staging systems have been proposed for GI lymphomas, including the Ann Arbor, Musshoff, and the European–American classification system. Each of these major staging systems recognizes four major stages of small bowel lymphoma: stage I for local disease, stage II for regional involvement, and stages III and IV for advanced disease with metastasis. Imaging is also now included in some staging systems after the 11th International Conference on Malignant Lymphomas (ICML) in 2011.139
Resection of small bowel lymphoma is important for local control but rarely eradicates the disease. Disease is often advanced so that fewer than 30% of intestinal tumors are amenable to primary curative resection.140 Adjuvant therapy is an essential part of the treatment. Surgical resection should be attempted for localized disease and should involve removal of the bowel segments, with wide margins, and the involved mesenteric lymph nodes, if possible. Margins need to be completely clear of tumor since lymphomas may spread for long distances in the submucosal plane. Adjuvant chemotherapy in patients after potential curative resection is advocated.141 In patients with unresectable lymphoma, radiation therapy and chemotherapy are recommended.142 Additionally, rituximab, the chimeric monoclonal antibody against the protein CD20, has also shown some promise in B cell lymphomas.143
Forty years ago, an unusual immunoproliferative small intestinal disease was reported to be particularly common in the Middle East, especially in southern Iran. This Mediterranean lymphoma is found in children and young adults and carried a poop prognosis.144 Patients tend to be from lower socioeconomic groups with a background of malnutrition. The tumor progenitor cell is believed to be the perifollicular B cell, which produces IgA. The tumor releases an excess of alpha heavy chains, which are detectable in the serum.145 However, recent epidemiologic reports from southern Iran suggest that distribution of NHL in the GI tract is similar to Western countries.146
Metastatic neoplasms
Metastatic neoplasm involvement of the small bowel is more frequent than primary small intestinal neoplasia. Primary tumors of the colon, ovary, uterus, and stomach involve the small bowel, most often by direct invasion or peritoneal spread. Primaries from the breast, lung, and melanoma metastasize to the small intestine hematogenously. A large review of autopsies from Memorial Sloan Kettering Cancer Center previously found the incidence of GI metastases from metastatic melanoma was 58% small bowel.147 Within the GI tract, the small bowel is the most frequent site of metastasis of melanoma most likely because of its rich blood supply. A retrospective study of 103 cases of malignant melanoma performed by the Armed Forces Institute of Pathology stated that small bowel involvement by melanoma, even in the absence of a known primary, is usually metastatic.148 If possible, surgery to remove disease should be offered. Ollila et al. reported on a retrospective review of 124 of 6509 melanoma patients who had GI tract metastases at the John Wayne Cancer Institute from 1971 through 1994.149 Of these 124 patients, 69 (56%) underwent surgical exploration of the abdomen, of which 46 (67%) had curative resection and 23 (33%) had a palliative procedure only. Almost all (97%) of the 69 surgical patients experienced symptomatic relief postoperatively. The median survival of patients undergoing curative resection was 48.9 months compared with only 5.4 months in patients undergoing palliative procedures and 5.7 months in patients undergoing nonsurgical interventions. Metastatic lesions to the small bowel can be treated with resection in selected cases and/or tumor-specific systemic therapy.
Tumors of the appendix
Neoplasms of the appendix are found in as high as 5% of specimens obtained by appendectomy for acute appendicitis.150 Most of these lesions are benign, including mucosal hyperplasia or metaplasia, leiomyomas, lipomas, neuromas, and angiomas. Malignancies of the appendix are rare, making up less than 0.5% of all intestinal neoplasms.151 Among 71,000 appendectomy specimens taken over a 40-year period, Collins found 958 malignant tumors, with an overall incidence of 1.35%.150
Broadly, appendiceal malignancies are divided into those of neuroendocrine origin (carcinoid) or epithelial origin. Malignancies of epithelial origin include mucoceles, pseudomyxoma peritonei (PMP), goblet cell carcinomas, and primary adenocarcinomas. In a large series of 5655 appendiceal tumors observed from the SEER database of the National Cancer Institute between 1973 and 2007, malignant carcinoid comprised of 11% of specimen but had the best 5-year disease-specific survival of 93%.152
Tumors of the appendix often present in the setting of appendicitis, which may lead to a pathological diagnoses after appendectomy. However, in the setting of perforated appendicitis complicated by phlegmon or abscess, the paradigm of management has shifted from interval appendectomy towards nonsurgical management. This trend is important because in 2% of patients where nonsurgical management is undertaken, there is an associated underlying cancer diagnoses or Crohn’s disease, especially in patients over 40 years old.153
Carcinoids
Carcinoids are the most common appendiceal tumors, comprising 32% to 85% of all appendiceal neoplasms, which include both benign and malignant types.154, 155 Malignant carcinoids comprised of 11% of appendiceal malignancies, derived from the SEER study. The SEER study also revealed a sex predominance for appendiceal carcinoids, with tumors from females comprising 68% of the cases. This female predominance may reflect the increased number of pelvic procedures performed in women, leading to more incidental findings, including carcinoids of the appendix. Peak incidence occurs in the third to fourth decades of life, averaging 32 to 42 years in the literature.156, 157
Most of carcinoids occur in the distal 1/3 of the appendix, where they are unlikely to cause obstruction.158 Symptoms are more likely with larger tumors and with metastases beyond the regional lymph nodes. Approximately 10% of appendiceal carcinoids are located at the base of the appendix, where they can cause obstruction, leading to appendicitis.155 Similar to other intestinal carcinoids, appendiceal carcinoids can be vasoactive substances, which are responsible for carcinoid syndrome. Carcinoid syndrome symptoms are rare but indicate metastatic disease, typically to the liver.159
In general, metastases from appendiceal carcinoids <2 cm in diameter are uncommon. Moertel and colleagues, in their evaluation of 150 appendiceal carcinoids over a period of 51 years, noted that 4.7% of the cases metastasized but none of the tumors <2 cm exhibited metastatic spread.160 Extension into the mesoappendix, if present, correlates with nodal metastases and tumor size, and those with high mitoses and Ki67 positivity correlate with tumor aggressiveness.161, 162
Small (<2 cm) carcinoids at the tip of appendix may be treated with a simple appendectomy.163 At laparotomy, these tumors appear as small yellow nodules, usually in the distal third of the appendix. Histologically, the cells are small and uniform, and contain a central nucleus with few mitoses. Almost all carcinoids show invasion of the muscular layer of the wall of the appendix, and involvement of lymphatic vessels adjacent to the tumor is essentially universal.163 Despite this microscopic finding, few patients have regional or distant dissemination of disease. Large (>2 cm) carcinoids and those at the base of appendix require a right colectomy, which removes the draining lymph nodes and any residual disease that might remain at the base of the appendix or in the mesoappendix.
Based on consensus guidelines in 2010 and 2012 from the North American Neuroendocrine Tumor Society (NANETS) and European Neuroendocrine Tumor Society (ENETS), completion colectomy is also recommended for tumors between 1 and 2 cm that also have mesoappendiceal invasion, positive or unclear margins, higher proliferate rate, angioinvasion, and mixed histology consistent with goblet cell carcinoid or adenocarcinoid.164, 165
In 2010, the AJCC included a TNM staging for appendiceal carcinoid for the first time, which is different from TNM staging systems for carcinoids arising from other intestinal sites and lung. Overall outcomes for early-stage appendiceal carcinoids are optimistic. Based on analysis of 900 appendiceal carcinoid tumors observed from the SEER database, five-year disease-specific survival rates for appendiceal carcinoids were 100% if tumor size <3 cm without regional nodal or distant metastases, 78% if tumor size between 2 and 3 cm with regional nodal metastases or tumor size >3 cm with or without nodal or distant metastases, and 32% if there is distant metastases.166
Mucocele
An appendiceal mucocele is any one of a number of lesions that are characterized by dilation of the appendiceal lumen, alteration of the mucosal lining, hypersecretion of mucus, and occasional extension outside of the appendix.167 The underlying pathology may be a hyperplastic polyp; a benign neoplasm, such as cystadenoma; or a malignant tumor, such as cystadenocarcinoma. Many authors support the use of a system based on histologic findings rather than on the presence of a cystic lesion.167 In this system, mucoceles of the appendix are classified into simple (obstructive) and mucoceles with proliferative epithelial changes. Benign neoplastic proliferative changes may be localized, as in adenoma of colonic type, or diffuse, as in mucinous adenoma or mucinous cystadenoma. Malignant proliferative groups may be classified as colonic-type adenocarcinoma, mucinous cystadenocarcinoma, and mixed carcinoidadenocarcinoma.168 The preneoplastic potential of hyperplastic epithelium and the premalignant nature of adenomatous epithelium are seen by the coexistence of hyperplastic, adenomatous, and carcinomatous epithelia all in the same lesion.168 A consequence of mucoceles of the appendix (cystadenomas and cystadenocarcinomas) is PMP. This lesion, characterized by large quantities of mucus-like material in the peritoneal cavity, is considered to represent dissemination of mucinous cystadenocarcinoma within the peritoneal cavity (see the section on PMP).169
Though the diagnosis of appendiceal mucocele is usually an incidental finding at celiotomy, mucinous cystadenomas and cystadenocarcinomas are among the few appendiceal tumors that may be diagnosed preoperatively.163 CT strongly suggests a mucinous tumor if a mass is present in the right lower quadrant with near water density. Ultrasound shows a diagnostic variable sonographic echogenicity because of the combination of mucin with more anechoic fluid. Although both imaging techniques may be helpful in diagnosing a mucocele, other cystic lesions of the peritoneal cavity, such as ovarian cysts, duplication cysts, mesenteric and omental cysts, or an abscess, may have a similar appearance.170
Surgical resection should be pursued, even for a benign-appearing appendiceal mucocele, since lesions that appear to be benign on imaging studies may harbor a cystadenocarcinoma. The extent of resection is dependent on the underlying histology. In the case of hyperplastic polyps or cystadenoma, a simple appendectomy is considered curative. In the series reported by Higa and colleagues, 36 of the 46 patients with mucinous cystadenomas were treated with appendectomy alone with no recurrence.167 In patients with mucinous cystadenocarcinoma, a substantial number will present with extensive abdominal metastases or PMP. Treatment of the primary lesion includes a formal right hemicolectomy with removal of draining lymph nodes.171 Stephenson and Brief reviewed 53 appendiceal mucinous cystadenocarcinomas treated by either simple appendectomy or right hemicolectomy. At 10 years, survival was 65% among patients treated with hemicolectomy in contrast to a 37% rate among patients who had received an appendectomy alone.172 Surgical debulking of metastatic deposits and evacuation of mucus collections are also recommended.
Pseudomyxoma peritonei
PMP is a condition characterized by diffuse collections of gelatinous material in the abdomen and pelvis and mucinous implants on the peritoneal surfaces, originating from ruptured mucinous neoplasms. As the primary tumor grows and occludes the lumen, mucus accumulates leading to appendiceal rupture. The peritoneum is then seeded with mucus-producing cells, which continue to proliferate and produce mucus.173 Accumulation of intraperitoneal mucus eventually progresses to intestinal obstruction, nausea, vomiting, and starvation, which is fatal. Over the years, the term PMP has begun to be used more generally by clinicians to signify not only intraperitoneal mucinous dissemination from rupture of a benign cystadenoma, but also peritoneal dissemination of mucus-producing adenocarcinomas of the appendix, large and small bowel, as well as lung, breast, pancreas, stomach, bile ducts, gallbladder, and fallopian tubes/ovary.174, 175
PMP is found incidentally in approximately 2 of 10,000 laparotomies, with a female predominance.174 The most common presenting symptom in both men and women is increasing abdominal girth; in men the second most common symptom is an inguinal hernia, while for women it is an ovarian mass palpated at the time of a routine pelvic examination.173 On CT scan, the mucinous material is similar in density to fat and appears heterogeneous. Scalloping of the liver, spleen, and mesentery is found, and calcifications are common. The undersurface of the diaphragm may be greatly thickened by large cystic masses of mucinous tumor. A striking early finding is the characteristic peripheral location of tumor within the abdomen and pelvis and relative sparing and central displacement of the small bowel and mesentery.173
Traditionally, treatment for PMP is repeated surgical debulking for symptomatic disease.174 Debulking is not curative but aims to limit the buildup of mucus and its pressure effect. Invariably, disease recurrence requires repeated and progressively more difficult surgery due to adhesions and fibrosis, with five-year survival of 50%.176 Cytoreduction and intraperitoneal chemotherapy is a more aggressive approach that includes radical surgical removal of all intra-abdominal and pelvic disease and the administration of intraperitoneal heated chemotherapy. Drug penetration is enhanced by heating the perfusate containing chemotherapy, an approach termed intraperitoneal hyperthermic chemotherapy (IPHC).177–180 This approach is best suited to patients with minimal residual disease (deposits smaller than 2–2.5 mm) after surgical cytoreduction. It is unlikely that even a heated solution of chemotherapy could penetrate large tumor deposits.
Sugarbaker et al. have written most extensively about treatment of peritoneal surface malignancy with aggressive surgical debulking and IPHC.179 His group uses four clinical assessments to select patients who are most likely to benefit from combined treatment. First, histopathologic assessment in which noninvasive malignancies such as true PMP or cystic mesothelioma are more likely to be made visibly disease-free through a peritonectomy procedure and are less likely than other invasive histologies to have spread to regional nodes, liver, or other systemic sites. Second, preoperative contrast-enhanced CT of the chest, abdomen, and pelvis not only to exclude liver or other systemic metastases but also to determine if small bowel obstruction or tumor nodules greater than 5 cm are present, which portends a poor prognosis. Two other clinical indices, the peritoneal cancer index (PCI, a quantitative indicator of prognosis derived from the size and distribution of nodules on the peritoneal surface) and the completeness of cytoreduction score (the size of persisting tumor nodules after maximal cytoreduction), are derived intraoperatively. A 2001 report by Sugarbaker and colleagues included 108 patients with PMP treated over a 10-year period (1983–1993) with surgical debulking and intraoperative intraperitoneal heated mitomycin followed by intraperitoneal 5-FU during postoperative days 1 to 6 and three subsequent courses of adjuvant intravenous mitomycin and intraperitoneal 5-FU.181 Of the 65 patients with true PMP, 5-year survival was 75% and 10-year survival was 68%. Those with carcinomatosis had a poorer outcome with 5- and 10-year survival rates of 26% and 9%, respectively. Morbidity associated with combination of cytoreductive surgery and IPEC is high (37.75%).182 However, studies have shown that this rate is still acceptable in terms of cost–benefit ratio to patients.176
Adenocarcinoma
Primary adenocarcinoma of the appendix is a rare neoplasm, accounting for 4–6% of primary appendiceal neoplasms, arising in preexisting adenomas.183 The mean age of presentation is 50 years, and a male predominance is noted of anywhere from 4 : 1 to 2.8 : 1.184–186 The clinical presentation in the majority of patients in the literature is acute appendicitis or an abdominal mass, though the diagnosis is rarely made preoperatively. Perforation may complicate the clinical picture, occurring in up to 40% of cases, but perforation alone has little effect on OS.187
Histologically, primary adenocarcinoma is distinguished from an adenoma by invasion of the wall of the appendix by the neoplastic tissue. Lymph node metastases are noted in 25% of cases at presentation.188 Adenocarcinoma of the appendix has a metastatic potential between that of appendiceal carcinoid and colonic adenocarcinoma, with metastases developing in 20% of patients, often to the ovary.183 The degree of metastatic involvement varies with the histologic grade; about 30% of the well-differentiated tumors are found to have metastasized, whereas nearly 70% of the poorly differentiated tumors are metastatic at the time of laparotomy.184, 185 The overall 5-year survival rate is 55% and varies with Dukes stage (A 100%, B 67%, C 50%, D 6%).189
The literature suggests that surgical treatment of adenocarcinomas should involve more than just an appendectomy. Hesketh reported that the 5-year survival rate was 20% with appendectomy alone compared to 63% with right hemicolectomy.186 Hopkins et al. reported rates of 20 and 45%, respectively.190
Carcinoma of the colon and rectum
Epidemiology
Colorectal cancer (CRC) remains an important global health issue. It is the third most common malignant tumor and the fourth most common cause of cancer death worldwide.191 CRC is most common in developed nations. In the United States alone, an estimated 130,000 people were diagnosed with CRC in 2014, and approximately 50,000 died from the disease.192 It is thought that dietary and lifestyle habits, in conjunction with genetic factors, account for the increased incidence in developed countries. Research shows that individuals who migrate from regions where CRC is less common to regions of high incidence will inherit the risk of the host country.193
There are disparities in CRC incidence and mortality among genders, races, and ethnic groups. While CRC is the third most common malignancy in the United States for both men and women, and the incidence of colon cancers is similar between the sexes, rectal cancer is more common in men. Right-sided/proximal colon cancers are more common among women compared to distal tumors in men.191 Moreover, mortality is approximately one-third higher in men.194 African-Americans have the highest rates of both incidence and mortality when compared to the White, Asian-American, American Indian, and Hispanic populations.195 The reasons for the disparities are not entirely known; however it has been postulated that differences in access to high-quality regular screening, timely diagnosis and treatment, dietary and lifestyle factors, and socioeconomic status could play a role.195, 196
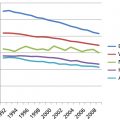
Despite the high prevalence of CRC in the United States, both the incidence and overall mortality from CRC have been declining over several decades. These declines have accelerated recently; as for both males and females, the incidence rates decreased at a rate of approximately 4% between 2008 and 2010, and mortality rates decreased by about 3% over the same time period.197 Studies have shown that increased screening and detection can reduce the chance of developing or dying from CRC by 10–75%, depending on which screening tests are used and how often they are performed.198 This increased screening could also be a reason for the shift in anatomic distribution of CRC from rectum and left-sided cancers to more right-sided cancers. Data from the National Cancer Data Base from the years 1988 and 1993 show an increase from 51% to 55% of all CRC to be proximal to the splenic flexure.199 Multiple studies have confirmed a higher rate of proximal colon cancer rates compared to distal colon or rectal carcinoma rates, both in the United States and globally.199–202
Risk factors
Age and racial background
Age is a known risk factor for CRC. The vast majority of cases of CRC occur in people over age 50, with incidence continuing to increase thereafter.198 In fact, fewer than 10% of all new CRC diagnoses and deaths occur in patients younger than 50.192 As discussed previously, African-American individuals have a higher incidence and mortality rate of CRC compared to other racial and ethnic populations.195, 198, 199.
Personal or family history
Patients with a personal history of adenomatous polyps or previous CRC have an increased risk of developing colon cancer in the future. Size, number, and histology of polyps are important prognostic factors, with size >1 cm, villous or tubulovillous histology, and multiple polyps conferring a greater risk for CRC.203 Patients with an isolated tubular adenoma of <1 cm do not appear to be at an increased risk of developing CRC.203 In patients with previous CRC, the incidence of metachronous CRC is 6%, and the incidence of metachronous adenomas is 25%.204
Family history of CRC in a first-degree relative increases the risk of developing CRC two- to threefold, while cancer in a second-degree relative increases the risk of CRC by 25–50%.205, 206 In addition, risk increases if there are more than one first-degree relative with colon cancer or if they are diagnosed before age 55.207 Family history of colonic adenoma also increases the risk of CRC, especially if the adenoma is diagnosed early.
Inflammatory bowel disease
UC and Crohn’s disease are well-known risk factors for colorectal carcinoma. For UC, the extent of disease and the duration of disease are the primary prognostic factors. Patients with pancolitis have a 5- to 15-fold increased risk of developing CRC compared to a threefold increased risk with colitis limited to the left colon.208 The risk also increases the longer the disease is present.209 Similar characteristics and incidence of CRC have been reported in Crohn’s disease.210–212
Diet and lifestyle
Westernized dietary habits, including an increased consumption of red meat and fat with a decreased consumption of fruits and vegetables, are associated with CRC. There is conflicting evidence regarding the effect of diets high in fruits and vegetables, but the general consensus is that while there may not be a protection associated with increased consumption, very low consumption does increase risk of developing CRC.213–215 A high-fat diet containing mixed lipids and saturated fat has been shown to promote colon carcinogenesis.216, 217 Alternatively, high intake of poultry and fish appears to be protective.218
Obesity has been associated with an increased risk of CRC in both men and women, and people with a BMI ≥30 kg/m2 appear to have nearly a 20% increased risk of CRC compared to nonobese patients.219, 220 In contrast, physical activity and exercise are correlated with a decreased risk of CRC.221
Diabetes mellitus and hyperinsulinemia
There is increasing evidence that diabetes mellitus and insulin resistance are risk factors for CRC. A meta-analysis of 15 studies found the estimated risk of CRC in diabetics was 30% higher than nondiabetics.222, 223 A possible explanation is the hyperinsulinemia associated with diabetes or even chronic insulin treatment for diabetes, resulting in growth signals to colonic mucosal cells via insulin-like growth factor 1.223, 224
Alcohol and tobacco
Heavy alcohol consumption is correlated with a moderately increased risk of CRC. The association is dose dependent and is irrespective of the type of alcoholic beverage consumed.225, 226 The association between smoking and CRC is not as straightforward, and cigarette smoking may have a greater impact depending on specific somatic polymorphisms.227
Genetics
Colorectal tumorigenesis follows a distinct genetic pattern, with accumulation of genomic alterations and progressive waves of clonal expansion of cells that have a growth advantage over their progenitors. Three major categories of genes have been implicated in the development of CRC, namely, oncogenes such as K-ras; tumor suppressor genes such as adenomatous polyposis coli (APC), deleted in colorectal carcinoma (DCC), p53, and mutated in colon cancer (MCC); and the mismatch repair genes hMSH2, hMLH1, hPMS, and hPMS2.
CRC develops from a multistep gene mutation sequence termed loss of heterozygosity (LOH) that can be observed in inherited and sporadic CRC. Fearon and Vogelstein first postulated in 1990 that at least five genes had to be mutated in order to progress in the adenoma to carcinoma sequence.228 Further studies showed that at least seven genetic alterations take place before the development of cancer. Important genes in the LOH model include APC, K-ras, DCC, and p53. An entirely different pathway of cancer development is initiated by defects within the mismatch repair genes. In this case, replication errors (RERs) increase, leading to microsatellite instability and malfunction of the gene. This pathway is referred to as RER and occurs in 20% of all colorectal tumors.229
APC gene
The APC gene is located on the long arm of chromosome 5 (5q). It is mutated in FAP and Gardner syndrome and in most cases of Turcot syndrome. A mutated APC gene is detected in 63% of adenoma and carcinoma, but not in the surrounding tissues, indicating that this is a somatic mutation. Because APC is a tumor suppressor gene, inactivation of the second allele must occur for the cell to lose the tumor-suppressing activity of the APC protein. There is considerable evidence that APC mutations occur early and may be the first event in sporadic colorectal mutagenesis.
DCC gene
The DCC gene is located on the long arm of chromosome 18 (18q). The gene product is involved in cell–cell adhesion and cell–matrix interactions, which may be important in preventing tumor growth, invasion, and metastasis. In sporadic CRC, DCC seems to play a critical role in the ability of a tumor to metastasize.
p53 gene
The p53 is located on the short arm of chromosome 17 (17p). p53 seems to be the most important determinant of malignancy during colorectal tumorigenesis. As a tetramer, p53 binds sequences of DNA in the promoter region of other genes to enhance their transcription.230 Most genes activated by p53 are thought to be involved in the inhibition of growth. Mutations of p53 can be found in more than half of all human cancers.231
K-ras proto-oncogene
K-ras is an oncogene, which acts in a classic dominant fashion and is located on the short arm of chromosome 12 (12p). The K-ras protein interacts with putative effector molecules, conveying a growth response. The signal transduction process is perturbed with a mutant K-ras protein leading to tumor formation. In sporadic colorectal tumors, K-ras mutations have been found in approximately 50% of carcinomas and large adenomas.232
Mismatch repair gene
Mismatch repair genes are needed for cells to repair DNA RERs and spontaneous base repair loss. The four DNA mismatch repair genes found in humans are hMSH2 (chromosome 2p), hMSH6 (chromosome 2p), hMLH1 (chromosome 3p), hPMS1 (chromosome 2q), and hPMS2 (chromosome 7p). They are regarded to contribute to hereditary nonpolyposis syndrome in various percentages.233
Inherited syndromes
Even though the vast majority of cases of CRC are sporadic rather than familial, inherited susceptibility results in a dramatic increase in risk of developing CRC. The genetic syndromes are typically inherited in an autosomal dominant fashion and are associated with a very high risk of developing CRC.
FAP is an autosomal dominant process characterized by numerous colonic adenomas which appear during childhood. This syndrome has penetrance approaching 100% with the onset of symptoms and diagnosis generally around age 15 years.234 If left untreated, FAP will invariably become CRC with a mean age of diagnosis and death of 39 and 42 years, respectively.235 An attenuated form of APC (AAPC) is a milder variant of FAP with a similar risk for developing CRC. AAPC is characterized by fewer adenomatous polyps and an older average age of diagnosis (usually in the early 50s). Both of these inherited syndromes are caused by different germline mutations in the same APC gene, which is located on chromosome 5.236
Hereditary nonpolyposis colorectal cancer (HNPCC) is another autosomal dominant inherited syndrome which accounts for 1–5% of all colorectal carcinomas. Also known as Lynch syndrome, this disease is characterized by an early age of onset (some patients can present in their 20s, while the mean age of diagnosis is 48 years), right-sided predominance, multiple synchronous or metachronous colonic tumors, and extracolonic manifestations. The extracolonic neoplasms can include endometrial cancer, renal pelvis and ureter cancer, bladder cancer, small bowel cancer, and skin lesions.237 As described above, HNPCC is caused by a mutation in one of the mismatch repair genes.238
MYH-associated polyposis (MAP) is a recently described autosomal recessive polyposis syndrome associated with a somewhat attenuated phenotype compared to other familial polyposis syndromes.239 Mutations in MYH, a base excision repair gene, are associated with an increased risk of multiple adenomas or polyposis coli.240 In patients where no APC gene mutation is found, especially in those patients with 10–15 or more adenomas, work-up for an MYH gene mutation is indicated for diagnosis.240, 241 In addition, these patients are at high risk for synchronous GI cancers.
PJ syndrome is an inherited hamartomatous polyposis syndrome that predisposes to CRC. The two major manifestations of PJ are pigmented mucocutaneous lesions and multiple colonic polyps which have the ability to undergo malignant transformation. PJ is associated with an increased risk of both GI and non-GI malignancies including ovarian, breast, pancreatic, uterine, Sertoli cell, and cervical neoplasms.242–244 Juvenile polyposis (JP) is another inherited hamartomatous polyposis syndrome that can predispose to CRC. Patients with JP are also at increased risk for gastric, duodenal, and pancreatic cancers.245, 246
Polymorphisms
Numerous genetic polymorphisms (normal variations in genes) have been found to be associated with developing CRC. Changes in genes such as carcinogen metabolism genes, methylation genes, and tumor suppressor genes can lead to either an increase or decrease in cancer risk. Cytochrome P450 genes, Glutathione-S transferase genes, N-acetyltransferase genes, and tumor suppressor genes have all been implicated in CRC. Cytochrome P450A1 (CYP1A1) is a phase I enzyme which acts on carcinogens found in tobacco smoke.247 Polymorphisms such as A—>G at Ile462Val, exon 7 in the gene for CYP1A1 puts patients at an increased risk for developing CRC.248 Patients who smoke cigarettes are especially at risk when they carry a polymorphism in this gene.
Glutathione-S-transferases are phase II enzymes responsible for the detoxification of mutagenic electrophiles, including polyaromatic hydrocarbons.247 Glutathione-S-transferase Mu (GSTM1) and Theta (GSTT1) have both been discussed in relationship to CRC. In addition, N-acetyltransferases are phase II enzymes involved in detoxifying arylamines, which are found in cooked meat.247 Both GSTT1 and NAT2 rapid acetylator phenotype have been identified as causing an increased risk for CRC.249
The most common tumor repressor gene associated with CRC is the APC gene. A polymorphism at I1307K, found predominantly in the Ashkenazi Jewish population, confers a twofold increase in CRC risk.250 Another polymorphism in the APC gene, I1317Q, also increases the risk of CRC.251
Some polymorphisms have been shown to be protective against CRC. Patients who eat a low-fat diet and who are homozygous for a variant APC gene at codon 1822 have a reduced risk of colon cancer compared to those patients who are wild type and eat a high-fat diet.252 In addition, variations in a methylation gene for methylenetetrahydrofolate reductase (MTHFR) have been shown to influence CRC risk. Patients who carry the MTHFR 677TT genotype have a reduced risk of CRC.253
Presentation, screening, and surveillance
Signs and symptoms
The presentation of large bowel malignancy generally falls into three categories: insidious onset of chronic symptoms, acute onset of intestinal obstruction, or acute perforation. The most common presentation is that of an insidious onset of chronic symptoms (77–92%), followed by obstruction (6–16%), and then perforation (2–7%).254–256
Bleeding is the most common symptom of colorectal malignancy.257 Unfortunately, patient and physician alike often attribute the bleeding to benign conditions. Bleeding may be occult or it may be seen as stool that is black, maroon, or bright red depending on the location of the malignancy.
Change in bowel habits is the second most common complaint, with patients noting either diarrhea or constipation.257, 258 Constipation is more often associated with left-sided lesions because the diameter of the colon is smaller and the stool is more formed than on the right side. Patients may report a gradual change in the caliber of the stool or may have diarrhea if the narrowing has progressed sufficiently to cause obstruction. Carcinomas of the right side of the colon do not typically present with changes in bowel habits, but large amounts of mucus generated by a tumor may cause diarrhea, and large right-sided lesions or lesions involving the ileocecal valve may cause obstruction.
Abdominal pain is as common a presentation as change in bowel habits.259 Left-sided obstructing lesions may present with cramping abdominal pain, associated with nausea and vomiting, and relieved with bowel movements. Right-sided malignancies may result in vague pain that is difficult to localize. Rectal lesions may present with tenesmus, but pelvic pain is generally associated with advanced disease after the tumor has involved the sacral or sciatic nerves. Less common symptoms include weight loss, malaise, fever, abdominal mass, and symptoms of urinary tract involvement. Bacteremia with Streptococcus bovis is highly suggestive of colorectal malignancy.260, 261
Physical exam is often unrevealing because the abdomen is distended, and masses, primary or metastatic, are not palpable. Tympany, ascites, and distention may be all that is noted on abdominal exam. Rectal exam will only rarely reveal an obstructing tumor. Colorectal malignancy should always be considered when patients present with large bowel obstruction. The diagnosis may be confirmed with contrast enema, rigid or flexible endoscopy, or CT scans of the abdomen and pelvis.
Perforation may result in localized or generalized peritonitis or, if walled off, it may present with obstruction or fistula to an adjacent structure such as the bladder. Perforation occurs in 12–19% of patients with obstruction due to CRC.262, 263 When the perforation occurs proximal to the obstructing lesion, the patients present with diffuse peritonitis and sepsis. Emergent surgical intervention after adequate fluid resuscitation is clearly indicated. However, perforation at the tumor, possibly secondary to tumor necrosis, may follow a more indolent course, and thus may be confused with alternative diagnoses such as appendicitis, diverticulitis, or Crohn’s disease.
Screening and surveillance
Cancer screening refers to the testing of a population of apparently asymptomatic individuals to determine the risk of developing CRC. Surveillance refers to the ongoing monitoring of individuals who have an increased risk for the development of the disease. For CRC, surveillance is reserved for patients with inflammatory bowel disease, family cancer syndromes, and those with a previous history of CRC or colorectal adenomas. Various screening and surveillance modalities are available to detect CRCs and adenomatous polyps. Current screening and surveillance recommendations are listed below (Table 1).
Table 1 Screening recommendations, National Comprehensive Cancer Network
| Risk category | Screening and surveillance recommendations |
| Average risk: Asymptomatic, age 50 or greater; no history of adenoma, sessile serrated polyp, or colorectal cancer | Starting at age 50, colonoscopy every 10 years or flexible sigmoidoscopy every 5 years (with interval stool-based testing at 3 years) or yearly stool-based testing (guaiac or immunochemical based) |
| Increased risk without personal history: First-degree relative with CRC or adenomatous polyps at age 60 or greater, two second-degree relatives affected with CRC, or one second-degree relative with CRC at age younger than 50 | Colonoscopy every 5 years starting at age 50 or 10 years younger than earliest family diagnosis |
| First-degree relative with CRC or adenomatous polyps at age younger than 60 or two or more first-degree relative with CRC | Colonoscopy every 3–5 years starting at age 40 or 10 years younger than earliest family diagnosis |
| Gene carrier or at risk for familial adenomatous polyposis | Flexible sigmoidoscopy or colonoscopy every year beginning at age 10–15 |
| Gene carrier or at risk for hereditary nonpolyposis colorectal cancer | Colonoscopy every 1–2 years beginning at age 25–30 or 2–5 years younger than earliest family diagnosis |
Stool-based screening methods
The advantage of fecal occult blood testing includes availability, convenience, and low cost. Limitations include low sensitivity, low specificity, low compliance, and inability to detect adenomas. Sensitivity is affected by slide storage, ascorbic acid, lesions not bleeding at the time of testing, and degradation of hemoglobin by colonic bacteria. Specificity is adversely affected by exogenous peroxidase activity by red meat and uncooked vegetables and medications that may induce bleeding from noncolonic sources such as aspirin and other nonsteroidal anti-inflammatory drugs. In five large controlled studies including more than 300,000 patients, an increased detection of CRC at earlier stages was demonstrated with the proper use of stool-based screening,264, 265 and testing was also associated with a significant reduction in mortality.264–268 Stool-based screening techniques include high-sensitivity guaiac-based testing, immunochemical-based testing, and most recently stool DNA tests. DNA testing detects the presence of genomic alterations that are known to occur in CRC oncogenesis; the best tests have demonstrated sensitivities as high as 95%.269 Currently, DNA tests have not yet been FDA approved, and thus they do not represent a first-line option for screening. As of 2014, high-sensitivity guaiac-based and immunochemical-based stool testing as standalone screening methods are considered appropriate so long as they are performed annually by a healthcare provider and a prescribed diet is followed. Any abnormal test requires follow-up invasive screening. Recently, immunochemical-based testing has proven to have increased sensitivity compared to guaiac-based tests.270 Stool-based screening is a particularly good option for those who refuse more invasive options.271
Flexible sigmoidoscopy
Both rigid and flexible sigmoidoscopies are inexpensive, require no conscious sedation, and afford direct visualization and biopsy of polyps and cancers.272 The advantage of the flexible sigmoidoscope over the rigid is that it can reach the descending colon and even the splenic flexure. The disadvantage of sigmoidoscopy is that the entire colon is not visualized, and lesions may be missed in the proximal colon. Current National Comprehensive Cancer Network and American Cancer Society Guidelines recommend sigmoidoscopy with or without stool-based screening every 5 years, with subsequent full colonoscopy if adenomatous disease is found.273
Barium enema
Barium enema combined with sigmoidoscopy allows for evaluation of the entire colon and rectum. Single-contrast barium enema is significantly less sensitive and specific than double-contrast barium enema (DCBE) and should not be used as a screening tool. DCBE has a sensitivity of 50–80% for polyps <1 cm, 70–90% for polyps >1 cm, and 55–85% for stage I and II carcinomas.274–276 When combined with sigmoidoscopy, the sensitivity reaches 98% and 99% for carcinomas and adenomas, respectively.277 Perforation as a result of DCBE has been reported at a rate of 1 per 25,000 studies.278 Current ACS screening recommendations are for a barium enema every 5 years with subsequent colonoscopy if test results are positive. The NCCN does not include barium enema as a screening option.273
Colonoscopy
Examination of the entire colon by colonoscopy is the gold standard screening method. When performed by trained endoscopists, colonoscopy with polypectomy is a safe procedure with a perforation incidence of 0.1%, hemorrhage incidence of 0.3%, and a mortality of 0.01–0.03%. The cecum is visualized in up to 98.6% of patients, and a DCBE may be performed when the cecum is not reached.279–284 Studies have shown that detecting and removing polyps reduce the incidence of colorectal malignancy, that detecting earlier lesions decreases disease-related mortality, and that fewer carcinomas develop in patients who have colonoscopy and polypectomy.285, 286 Colonoscopy is better than DCBE in detecting lesions <1 cm.276 Furthermore, a tissue diagnosis or therapeutic intervention may be made at the time of initial evaluation. Colonoscopy also compares favorably with sigmoidoscopy because the entire colon may be directly visualized. In one study, a prevalence of 24% of new adenomas was found when 226 patients underwent colonoscopy within 1 year of flexible sigmoidoscopy. Advanced lesions proximal to the descending colon were found in 6% of these patients.287 Current ACS screening recommendations are for a colonoscopy every 10 years.
CT colonography
CT colonography (virtual colonoscopy) is an emerging technique that uses three-dimensional reconstruction of the air-distended colon. At the National Naval Medical Center, in 1223 average-risk adults who underwent CT colonography followed by conventional colonoscopy, virtual colonoscopy was as good or better at detecting relevant lesions.288 However, it may be less accurate in surveillance populations, and subsequent multi-institutional studies have failed to confirm the excellent results from this series. The major limitations include uncertain accuracy, need for full bowel preparation, and follow-up colonoscopy for tissue diagnosis of radiographic abnormalities. CT colonography as the primary method of screening also results in repeated radiation exposure to the patient. Because virtual colonoscopy is considerably time and labor intensive from the standpoint of the radiologist, active investigations into methods of automating the evaluation process are ongoing. Current ACS screening recommendations are for a virtual colonoscopy every 5 years with subsequent colonoscopy if a lesion is found. The NCCN does not include CT colonography as a screening option.273
Preoperative work-up and staging
The general physical examination remains a cornerstone in assessing a patient preoperatively to determine the extent of local disease, disclosing distant metastases, and appraising the general operative risk. Special interest should be paid to weight loss, pallor as a sign of anemia, and signs of portal hypertension. In addition, a complete work-up should include routine lab work, colonoscopy, chest X-ray, CT of the abdomen and pelvis, and transrectal ultrasound (TRUS) for those with rectal cancer.
Routine laboratory work
A complete blood count (CBC) may reveal the presence of anemia. Liver function tests (LFTs) may be abnormal in the case of liver metastases. Carcinoembryonic antigen (CEA) levels should be obtained as a baseline against which further values may be compared. Metastatic disease to the liver is often accompanied with very high levels of CEA, and levels surpassing 10 to 20 ng/mL are associated with increased chances of treatment failure.289
Colonoscopy
Colonoscopy remains the single most important investigation in the evaluation of colonic diseases. It allows assessment of tumor size, but not depth of invasion, as well as localization in the colon. Further histology from the tumor can be obtained, synchronous tumors are detected, and synchronous polyps may be removed. Synchronous carcinomas occur in 2–7% of patients and synchronous polyps 29.7% of the time.290 It has been suggested that preoperative colonoscopy alters the operative procedure in 30% of patients.291
Radiologic evaluation
A chest X-ray evaluates for pulmonary lesions and serves as a rough guideline for cardiac as well as pulmonary status. The use of CT of the abdomen and pelvis in the preoperative evaluation of patients with colon cancer is controversial. It is our practice to obtain a CT in order to detect involvement of contiguous organs, paraaortic lymph nodes, and the liver. Abnormal LFT’s are present in only 15% of patients with liver metastases and may be elevated without liver metastases in up to 40%.292 Therefore, we do not believe LFT’s are a useful screening tool for determining the need for obtaining a CT scan. Abdominal ultrasound can be used in select patient to identify liver metastases, ascites, and gross adenopathy.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree