INTRODUCTION
SUMMARY
Indolent B-cell lymphomas deriving from the marginal zone include three specific entities: extranodal marginal zone (or mucosa-associated lymphoid tissue) lymphoma (EMZL), splenic marginal zone lymphoma (SMZL), and nodal marginal zone lymphoma (NMZL). The clinical and molecular characteristics are distinctive for each of these entities, although some phenotypic and genetic features are overlapping. EMZL is the most common entity, arising at virtually any extranodal site, commonly associated with chronic antigenic stimulation either as a result of an external infection (e.g., Helicobacter pylori in the stomach) or an autoimmune disease (as Sjögren syndrome or Hashimoto thyroiditis). SMZL accounts for approximately 20 percent of all marginal zone lymphomas, with patients typically presenting with an enlarged spleen and involvement of marrow and splenic hilar lymph nodes. NMZL is the least-common entity, representing approximately 10 percent of all marginal zone lymphomas and typically presenting with lymph node-based disease without splenic or extranodal site involvement.
Acronyms and Abbreviations
AKT1, protein kinase Bα; BCL6, B-cell CLL/lymphoma 6 gene; BCL10, B-cell CLL/lymphoma 10 gene; BCR, B-cell receptor; CD, cluster of differentiation; EMZL, extranodal marginal zone lymphoma; HCV, hepatitis C virus; Ig, immunoglobulin; IGHV, immunoglobulin heavy-chain variable region gene; IPSID, immunoproliferative small intestinal disease; LDH, lactate dehydrogenase; LPL, lymphoplasmacytic lymphoma; MALT, mucosa-associated lymphoid tissue; MZL, marginal zone lymphoma; NF-κB, nuclear factor-kappa B; NMZL, nodal marginal zone lymphoma; PAX5, paired box gene 5; PIM1, protooncogene proteins pim; ROS, reactive oxygen species; SMZL, splenic marginal zone lymphoma; WHO, World Health Organization.
INTRODUCTION AND CLASSIFICATION
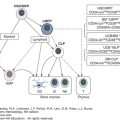
Marginal zone lymphomas (MZLs) represent a heterogeneous group of indolent lymphoproliferative disorders originating from memory B-lymphocytes, which are normally present in the marginal zone—that is, the outer part of the mantle zone—of the secondary lymphoid follicles. The spleen and the mucosa-associated lymphoid tissues (MALT) are the most frequently involved anatomic compartments; lymph nodes may also been involved, albeit rarely. The 2008 World Health Organization (WHO) Classification of Tumours of Haematopoietic and Lymphoid Tissue identifies three distinct subtypes of MZL based on the involved site, the clinical presentation and course of the disease, as well as the molecular profiles, namely, extranodal MZL of MALT type (also termed extranodal marginal zone lymphoma [EMZL]); splenic marginal zone lymphoma (SMZL); and nodal marginal zone lymphoma (NMZL).1 In addition, two provisional entities are recognized by the 2008 WHO classification: splenic diffuse red pulp lymphoma and hairy-cell leukemia variant, which represent two subtypes of splenic lymphomas with features overlapping with those of MZL.
In adults, MZLs account for 5 to 17 percent of all non-Hodgkin lymphomas (NHLs); MALT lymphoma is the most frequent overall, being the third most frequent NHL and representing 7 to 8 percent of all B-cell neoplasms. It mostly affects middle-aged adults, at a median age of 60 years, with a slight female preponderance and often in association with chronic antigenic stimulation, either as a consequence of a chronic infection or an autoimmune disease. Gastric MALT lymphoma is by far the most common clinical entity, displaying considerable geographic variability with a higher incidence in areas associated with a high incidence of Helicobacter pylori infection. SMZL and NMZL represent 20 percent and 10 percent of MZLs, respectively, accounting for less than 2 percent of all NHLs. The median age at disease onset is 65 years for SMZL, and between 50 and 60 years for NMZL.2,3
Each lymphoma subtype is presented and discussed separately in terms of epidemiology, etiology and pathogenesis, clinical presentation and treatment strategies.
EXTRANODAL MARGINAL ZONE LYMPHOMA
EMZL or MALT lymphoma is an extranodal lymphoma that arises both in organs with an anatomically well-defined MALT, such as the gut, the nasopharynx and the lung (in which MALT represents an acquired and specialized immunologic barrier associated with highly permeable mucosal sites in close contact with the external environment), and in sites which normally lack lymphoid tissue, but have accumulated B cells in response to a chronic infection or an autoimmune process, such as the salivary glands, the ocular adnexa (orbits, conjunctiva and lacrimal glands), the skin, the thyroid, the genitourinary tract (bladder, prostate, kidney, uterus), and the breasts.
MALT lymphoma accounts for at least 50 percent of primary gastric lymphomas, typically presenting in middle-aged adults, with a female predominance. Gastric MALT lymphoma is particularly common in the north-eastern part of Italy, which is an area of high prevalence of H. pylori infection. In contrast, a specific subtype of small intestinal MALT lymphoma (termed immunoproliferative small intestinal disease [IPSID]) tends to be more frequent in the Middle East, on the Indian subcontinent, and in the Cape Region of South Africa.
Sustained antigenic stimulation, triggered either by a chronic infection or by an autoimmune process, induces an initially polyclonal B-cell proliferation, as well as the development of an inflammatory response, with the attraction of neutrophils, which release reactive oxygen species (ROS). ROS are genotoxic, and may induce a wide range of genetic abnormalities. Moreover, the prolonged proliferation of B-lymphocytes induced by a chronic lymphoproliferative stimulus may increase the risk of DNA damage (double-strand breaks and translocations), as a consequence of the genetic instability of B cells during somatic hypermutation and class-switch recombination. Genetic abnormalities tend to involve those genes related to the activation of nuclear factor-kappa B (NF-κB), a key transcription factor regulating the expression of several survival- and proliferation-related genes in B cells during immune responses. The constitutive activation of this signalling pathway results in uncontrolled B-cell proliferation and subsequent neoplastic transformation of the involved tissue.
The longstanding antigenic stimulation explains how lymphoid infiltrates—or an acquired MALT—may appear in extranodal sites normally lacking MALT. The MALT that organizes in proximity to an epithelium receives stimuli from the epithelium itself (as occurs in autoimmune disorders) or from antigens entering the lymphoid tissue through the epithelium or via the afferent lymphatics (as during exogenous infections).
Microbial species thought to be associated with MALT lymphoma include: H. pylori and Helicobacter heilmannii, hepatitis C virus (HCV), Campylobacter jejuni, Borrelia burgdorferi, and Chlamydia psittaci. These entities have been found to be related with the development of MALT lymphoma of the stomach, IPSID, cutaneous MALT lymphoma and orbital MALT lymphoma, respectively.4,5,6,7 H. pylori has been documented as the etiologic agent in more than 90 percent of gastric MALT lymphoma, which arises from H. pylori–stimulated autoreactive B cells.8 H. pylori can be demonstrated by histology, polymerase chain reaction, or urea breath test, and can be isolated and cultured. H. pylori appears to be a fundamental factor for the development of the disease, and its elimination often induces a remission of the lymphoma by itself without any other intervention, thus fulfilling all four of Koch’s postulates and establishing the microorganism as the main etiologic factor. However, because only a minority of patients with an overt H. pylori infection develop the disease, it is obvious that the pathogenesis of gastric EMZL also depends on other, largely unknown factors, perhaps related to the host, the environment, or the virulence of the infecting H. pylori strain.
It has also been demonstrated that viable C. psittaci can be found not only in monocytes and macrophages infiltrating orbital MALT lymphoma, but also in patients’ blood and conjunctiva, raising the possibility of microbial eradication and disease remission by antibiotic therapy with drugs such as doxycycline.9
Autoreactive B cells found in autoimmune diseases, such as those infiltrating the thyroid in Hashimoto thyroiditis, or the salivary glands in Sjögren syndrome, organize progressively into a well-developed MALT, mimicking lymphoproliferation and eventually evolving into an overt lymphoma. Patients with Sjögren syndrome have a 44-fold increased risk of developing lymphoma, and patients with Hashimoto thyroiditis have a 70-fold increased risk of thyroid lymphoma.10,11
Recurrent genomic lesions, including chromosomal translocations and unbalanced aberrations, can be detected in MALT lymphomas in up to 40 percent of the cases, depending on the specific aberration. The t(11;18)(q21;q21) translocation is the most common structural chromosomal abnormality in MALT lymphoma, being demonstrated in 15 to 40 percent of the cases, especially in gastric and lung MALT lymphoma.12 Other chromosomal translocations include t(14;18)(q32;q21), t(1;14)(p22;q32) and t(3;14)(p13;q32), all involving the immunoglobulin heavy chain variable region (IGHV) gene on chromosome 14, and displaying a specific anatomic distribution (Table 101–1).13 The presence of any of these chromosomal alterations correlates with a lack of any further genetic instability or chromosomal imbalances.
| Lesion | Genes | Frequency | Sites | ||
|---|---|---|---|---|---|
| Translocations | t(11;18)(q21;q21) t(14;18)(q32;q21) t(1;14)(p22;q32) t(3;14)(p13;q32) | BIRC3-MALT1 IGHV-MALT1 IGHV-BCL10 IGHV-FOXP1 | 15–40% 20% <5% <5% | Stomach, lung Lung, skin, ocular adnexa, salivary gland Stomach, lung Unclear | |
| Gains | +3; +3q +18; +18q | 20–40% 20–40% | No differences in sites No differences in sites | ||
| Losses | −6q23 | TNFAIP3 | 15–30% | No differences in sites |
Current knowledge of the genetic lesions seen in MALT lymphoma suggest a model of multistage development and progression from a preneoplastic lesion to overt lymphoma. The accumulation of genetic abnormalities is associated with a loss of dependency from antigenic stimulation (with subsequent antibiotic resistance) and with possible histologic transformation.
EMZL mostly presents as Ann Arbor stage IE disease, which implies the sole involvement of the extranodal site of origin, with possible extension of the disease to tributary lymph nodes in close proximity to the affected organ. Marrow and peripheral lymph node infiltration is uncommon, observed in less than 20 percent of the cases at presentation. The stomach is the most commonly involved organ, accounting for approximately one-third of cases. Other typical presentations include the salivary glands, the orbits and the ocular adnexa, the thyroid, the lungs, the skin, the breasts, the liver, and other gastrointestinal sites, apart from the stomach. Disseminated disease can be documented in up to 25 percent of patients with gastric MALT lymphoma, although those with nongastrointestinal extranodal disease exhibit disseminated lymphoma in nearly half of the cases.14 Gastric MALT lymphoma is often multifocal, which may explain the high rate of relapse in the gastric stump after surgical excision. Synchronous involvement of gastrointestinal and extraintestinal sites is detected in approximately 10 percent of cases.
Systemic lymphoma-related symptoms are generally uncommon, and the clinical aspects and presenting symptoms generally correlate with the primary location of the disease.
Gastric MALT lymphoma presents with nonspecific dyspepsia, epigastric pain, and nausea. Chronic bleeding may become evident with progressively worsening iron-deficiency anemia. The antrum is the most frequently involved portion of the organ, although any part of the stomach can be affected: intragastric nodularities, enlarged rugal folds, thickened gastric walls, irregularly shaped superficial erosions or shallow ulcers all represent macroscopic features of this lymphoma.
MALT lymphomas of the ocular adnexa most often arise in the orbit (40 percent of cases), with masses that cause progressive proptosis, periorbital edema and abnormalities in ocular motility and vision. The conjunctiva is the site of origin in approximately 35 to 40 percent of the cases, with bilateral involvement observed in nearly 15 percent of patients. More rarely, the lymphoma originates from the lacrimal gland (10 percent of the cases) or the eyelid.
Cutaneous MALT lymphoma generally presents with papules, plaques or nodules mainly involving the trunk and the upper limbs; the occurrence of multiple lesions affecting noncontiguous regions is, however, not infrequent. Lesions may show spontaneous remissions, but cutaneous relapses are the rule.
Immunoproliferative small intestinal disease, which is considered a special variant of intestinal MALT lymphoma, usually manifests with a severe and unremitting malabsorption. The lymphoma usually remains confined to the upper intestine and the regional lymph nodes, spreading beyond the abdomen only in advanced stages of the disease and upon transformation into high-grade lymphoma.
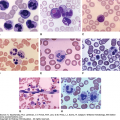
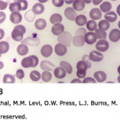
The neoplastic lymphocytes tend to infiltrate the marginal zone around reactive B-cell follicles, external to an intact follicular mantle. Their cytoplasm is pale, and they display small to medium-sized and irregularly shaped nuclei, with dispersed chromatin and inconspicuous nucleoli, either resembling germinal center centrocytes or monocytoid elements. Scattered, centroblast-like large cells may be present, although never predominant, as well as mature plasma cells in up to a third of cases. Lymphoepithelial lesions are characterized by invasion or necrotic destruction of the glandular epithelium by infiltrating lymphoma cells: they are highly characteristic of MALT lymphoma, particularly gastric MALT lymphoma (Fig. 101–1), although they are not pathognomonic. Germinal centers may also be colonized by MZL cells, thus conferring a vaguely nodular or follicular pattern; lymphoma cells may also undergo a blastic or plasma cell differentiation. Upon immunohistochemistry, cells are CD20+, CD79a+, CD21+, and CD35+, lacking CD5, CD23, and CD10, typically expressing immunoglobulin (Ig) M (less often IgA or IgG), with an immunoglobulin light-chain restriction.