Nodule features on ultrasound
Recommended FNA based on nodule size
High and intermediate suspicion for malignancy
≥1 cm
Low suspicion for malignancy
≥1.5 cm
Very low suspicion for malignancy
≥2 cm vs observation without FNA is also an option
Benign features (cystic)
No FNA unless symptomatic or cosmetic reasons
In the author’s opinion, smaller nodules with suspicious features should be biopsied if the diagnosis of malignancy would lead to surgical intervention, especially nodules close to the thyroid capsule, isthmus, or in the upper thyroid pole next to the cricothyroid muscle, which are known for metastasizing early on. The current guidelines do not strongly indicate more aggressive FNA biopsy of these small lesions in patients at a higher risk for thyroid cancer such as in patients with history of thyroid cancer in one or more first-degree relatives, exposure to ionizing radiation in childhood or adolescence, personal history of thyroid cancer, PET-positive nodules, multiple endocrine neoplasia 2/familial medullary thyroid cancer history, RET proto-oncogene mutation, or calcitonin >100 pg/mL. Again, in the author’s opinion, these patients can be considered for biopsy earlier if the clinician would treat surgically if a small lesion was found to be positive on FNA.
The American Association of Clinical Endocrinologists, Associazione Medici Endocrinologi, and European Thyroid Association Medical Guidelines for diagnosis and management of thyroid nodules suggest that solid and hypoechoic thyroid nodules should be biopsied when larger than 1 cm or at any size if the patient presents with any risk factor for thyroid cancer as described above [17].
Materials for Thyroid Nodule Fine-Needle Aspiration Biopsy
The ultrasonographer will require the following materials for fine-needle aspiration: a 10-cc syringe, a 25- or 27-gauge sterile needle usually 1–1.5 inches in length depending on the patient’s body habitus and location of the thyroid nodule, alcohol pads, gauze to wipe the excess gel, sterile probe cover, gloves, and lidocaine without epinephrine for local analgesia. Some clinicians prefer using a biopsy gun for ease of aspiration (Fig. 4.1). Larger bore needles should be avoided to prevent bleeding from the site of the biopsy and to avoid aspirating excess blood with the sample. For specimen processing, glass slides and 95 % ethanol solution for fixation along with ThinPrep or Hanks solution to wash the needle content are required (Fig. 4.2). For the clinicians who also assess the sample adequacy, a microscope with a set of Diff-Quik stains for slide preparation is necessary.
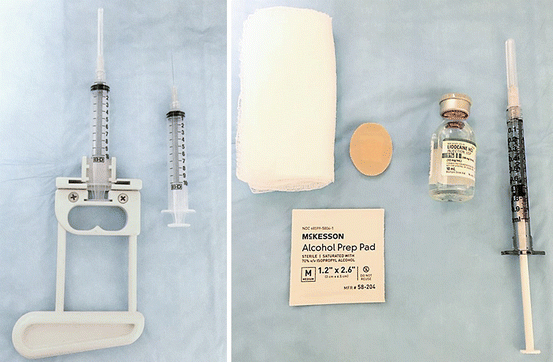
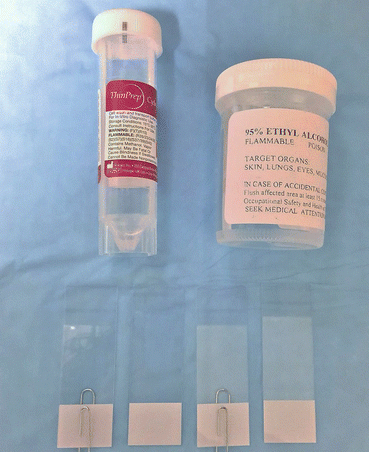

Fig. 4.1
Material for fine-needle aspiration biopsy of the thyroid gland. Picture from left to right: biopsy gun, 10-cc syringe with 27-gauge needle, gauze, alcohol pad, Band-Aid, lidocaine without epinephrine, and tuberculin syringe for local anesthesia injection

Fig. 4.2
Material for specimen preparation following fine-needle aspiration biopsy of thyroid nodule picture from top to bottom: ThinPrep solution, 95 % ethanol for fixation, and glass slides with paper clips placed on every other slide
Fine-Needle Aspiration Biopsy Techniques
Fine-Needle Aspiration Biopsy Guided by Palpation
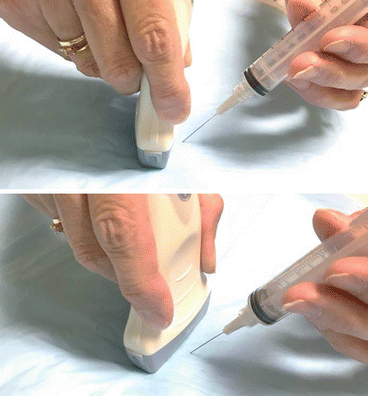
During this procedure, the patient is lying down with cervical hyperextension, using a pillow placed behind the patient’s shoulders (Fig. 4.3), while the clinician holds the thyroid nodule between his or her fingers (Fig. 4.4). The person performing the fine-needle aspiration will be standing on the opposite side of the lesion, so the needle is introduced from the neck midline in an effort to avoid going through large muscles and blood vessels. The patient is asked not to swallow or speak during the procedure to preclude movement of the thyroid. As mentioned above, one of the disadvantages of this technique is the imprecise needle placement due to lack of direct nodule visualization during the procedure.
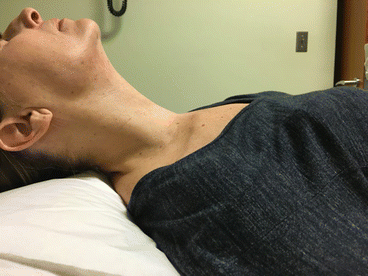
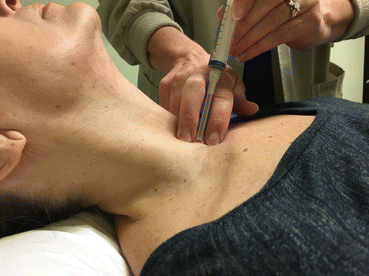

Fig. 4.3
Patient positioning for thyroid nodule biopsy with cervical hyperextension

Fig. 4.4
Demonstration of fine-needle aspiration of a thyroid nodule guided by palpation
Fine-Needle Aspiration Biopsy Guided by Ultrasonography
There are two main methods of aspiration of thyroid nodules under US guidance: transverse and longitudinal approaches.
With the transverse approach, the US probe is placed anterior to the nodule in question which should be positioned in the middle of the screen. A small button of local anesthetic (usually lidocaine without epinephrine) is injected in the subcutaneous area. The use of local anesthesia is optional, since the pain of injection is at times more uncomfortable than the fine needle puncture itself. The ultrasonographer would then introduce the fine needle exactly in next to the middle of the probe transversely, which should coincide with the middle of the screen where the nodule is located (Fig. 4.5). With this technique, the entire length of the needle cannot be visualized. The ultrasonographer should look for the subtle appearance of the needle on the screen at the time it enters the lesion in question. At this point, the needle is moved in and out with short and quick movements, back and forth inside of the nodule which can be done while aspirating the nodule or not. When the sample is collected, the aspiration should be released and the needle should be removed smoothly. This movement is the key for FNA of the thyroid and this repetitive motion should occur for approximately 10 seconds during each pass. The fine needle will collect the tissue in the bore by capillary action even if no active aspiration is applied, which is an important technique to decrease the blood in the aspirate, especially in hypervascular lesion biopsies. For most thyroid FNA guided by US, an adequate specimen is obtained with three passes. The advantage of the transverse technique is that it requires slightly less precision in the placement of the needle when compared to the longitudinal method; however, it can also be less accurate because the exact location of the tip of the needle is unknown unless the ultrasonographer can identify the needle tip appearing and disappearing from the screen while inside of the thyroid lesion with these short movements in and out of the imaged nodule.