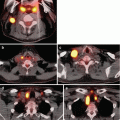
Fig. 17.1
Neck lymph nodes levels and compartments
Central Neck
As the region of the neck encasing the thyroid gland, the central neck (Level VI) is the most common location for persistent or recurrent WDTC. Of the 20 % of patients who are found to have recurrences in their lifetime, most of them are within this anatomical region. Defined as the area bounded by the carotid sheaths laterally, the hyoid bone superiorly, and the sternal notch or brachiocephalic vessels inferiorly, in addition to the thyroid gland, it holds the recurrent laryngeal nerves, parathyroid glands, and lymph node basins. The central neck lymph nodes include prelaryngeal (Delphian), pretracheal, and paratracheal basins, in which the latter extends to the carotid sheath laterally. Recurrent thyroid cancer is most commonly found here; reoperation, while safe when performed by high-volume surgeons, carries risks of injury of the regional structures. Reoperative central neck dissection has been shown to have rates of recurrent laryngeal nerve injury from 0 % permanent risk [19–25] to 21 % transiently [20]. Postoperative hypocalcemia has been reported with a large range of 0–24 % [20–26]. Table 17.1 outlines a literature review of complications from reoperative neck dissection.
Table 17.1
Complications after reoperative central compartment (Level VI) lymph node dissection (all retrospective reviews)
Author/year | Patients (N) | Recurrent laryngeal nerve palsy | Hypocalcemia | ||
|---|---|---|---|---|---|
Transient (%) | Permanent (%) | Transient (%) | Permanent (%) | ||
Farrag et al. [20] | 33 patients | 21 | 0 | 6 | 0 |
Clayman et al. [19] | 63 patients | 2 | 0 | 19 | 18a |
Alvarado et al. [23] | 193 patients | 3 | 0.6 | 11 | 2 |
Shen et al. [26] | 106 patients | 4.7 | 1.9 | 23.6 | 0.9 |
Tufano et al. [24] | 120 patients | 14.2a | 10 | 2.5 | |
Shah et al. [22] | 82 patients | 2 | 2 | 20 | 7 |
Lang et al. [25] | 50 patients | 6 | 1 | 14 | 0 |
Onkendi et al. [21] | 410 patients | 2b, 0.5c | 3 | ||
Due to the risks which are higher than first-time operations, the extent of reoperation should be dictated by disease burden. While lymph node dissection should encompass levels of the neck, specific levels and laterality should be dictated by specific recurrence patterns. If disease is limited to one side of the neck, a unilateral dissection would be recommended instead of bilateral [12]. If, however, disease is found throughout the central compartment, a bilateral procedure would be indicated, taking into consideration the recurrent laryngeal nerve and parathyroid glands which are closely related to the nodal basins.
Reoperative Lateral Neck Dissection
As mentioned, reoperative lateral neck dissection for WDTC should be performed by the neck level containing recurrent disease rather than “berry picking” single diseased lymph nodes. The most important, however, to an effective and safe dissection is the experience and judgment of the surgeon, weighing risks and benefits of the extent of surgery. Similar to the central neck, reoperation in the lateral neck carries higher operative risks than first-time surgery. Structures in the lateral neck of concern in reoperations include the carotid sheath containing the vagus nerve proximal to the recurrent laryngeal nerve, spinal accessory nerve, and other neurovascular structures surrounding the disease. Overall, compartmental neck dissection decreases structural disease burden in 80 % of patients, including lowering Tg up to 90 % of the time even though Tg levels often do not fall to negligible levels [27, 28].
Nonsurgical Therapies for Recurrent WDTC
Aside from formal surgical neck dissection, there has been an increased experience of clinicians treating recurrent WDTC with alternative local therapies. Two main modalities which have been described with good results are ethanol and radiofrequency ablation (RFA). Recent large series have been published showing treatment with ethanol and RFA can be safe and effective in recurrent WDTC. The largest study from Norway described the treatment of 109 lymph nodes with ethanol showing sustained ablation of recurrent disease in 84 % of cases at 38 months of follow-up [29]. Although many in this study needed to be retreated with ethanol, it was done as an outpatient without general anesthetic, and they described no significant adverse effects. Studies using RFA have also showed good results, with some studies showing up to 60 % disappearance of treated lymph nodes. A complication seen specifically in RFA however is heat damage to skin [30]. Some results have been promising although long-term studies are needed to evaluate the clinical effectiveness and impact on survival of these ablative therapies.
Distant Recurrence
Due to the favorable prognosis of WDTC, distant metastatic spread is rare, especially for lower-risk thyroid cancer. Unfortunately, it is sometimes difficult to predict distant metastasis, and ultimately it is up to the clinician to decide when investigation is warranted [31]. Cross-sectional imaging is most helpful in determining metastasis, specifically contrast-enhanced CT scan. As the lungs are the most common site of distant metastasis, CT scan of the neck and chest is helpful for quantifying disease burden in these patients. FDG-PET has been used also to help quantify distant disease. Recent publications suggest that those thyroid cancers which do not take up radioactive iodine due to dedifferentiation may be best seen by this method [32, 33]. Patients with distant metastasis may still have good long-term survival, depending on the differentiation of the thyroid cancer. Referral to a multidisciplinary team consisting of surgeons, endocrinologists, radiation oncologists, medical oncologists, nuclear medicine, and radiologists will facilitate optimal outcomes [34].
Conclusion
Fortunately, WDTC has a very favorable prognosis; however, patients may have recurrent disease. Most commonly, recurrence occurs in the neck and is best treated by surgical excision with low morbidity. While there are new treatment options described in the local treatment of thyroid cancer, larger longer-term studies are needed to correlate these treatments with survival. Patients with high-risk cancer or clinical symptoms of widespread disease should be worked up with cross-sectional imaging to rule out distant spread and treated accordingly. Overall, the best care for patients with recurrent thyroid cancer occurs when a multidisciplinary team is involved in a patient-centered treatment plan.