Fig. 6.1
Axial (a) and coronal (b) images from CT chest with intravenous contrast demonstrating a multi-nodular goiter with an enlarged thyroid gland, thyroid nodules with calcifications, and extension into the mediastinum
Box 6.1. Indications for Preoperative CT for Initial Surgery for Thyroid Cancer
Clinical evidence of local invasion:
Hoarseness, voice changes
Stridor
Dysphagia
Fixed mass on exam
Sonographic evidence of invasion of aerodigestive or vascular structures
Large primary tumor and/or mediastinal extension
Extensive nodal extension into:
Mediastinum
Deep structures of neck
Lack of thyroid ultrasound capability/expertise
CT scanning allows better visualization of structures in the deep/posterior neck and mediastinum, i.e., those areas that lie at the limits of the acoustic window accessible by ultrasound. When extracapsular extension is suspected, CT scanning is reported to be 29–78 % sensitive and 91–99 % specific for invasion of the trachea, esophagus, carotid artery, internal jugular vein, or recurrent laryngeal nerve [14]. Additionally, CT scanning carries the advantages of being widely available, reproducible, and user independent.
Assessment of the primary tumor and lymph nodes should include scanning from the skull base to the mediastinum. Intravenous contrast is needed to facilitate visual differentiation of tissues and should be used in all cases unless specifically contraindicated by allergy or renal insufficiency.
Iodinated contrast interferes with the uptake of radioactive iodine, an important component of thyroid cancer treatment. Thus, postoperative radioactive iodine ablation should be delayed for at least one month after the administration of iodinated contrast [15]. Because of this interaction, it is important to only obtain CT scanning when indicated. Finally, if CT scanning is performed, the decision to do so should be communicated clearly between surgeon and endocrinologist.
Magnetic Resonance Imaging
MRI is principally used for patients with an indication for cross-sectional imaging that have a contraindication for CT scanning, typically patients who have a known allergy to iodinated CT contrast. Since the gadolinium contrast used with MRI scanning does not interact with radioactive iodine, MRI may also be considered in patients with a strong, urgent indication for radioactive iodine therapy. The drawbacks to MRI include long image acquisition times, which can lead to motion artifact or feelings of claustrophobia, and increased risk of nephrogenic systemic fibrosis in patients with renal failure [16].
MRI images with and without contrast should be obtained. Thyroglobulin produced in lymph node metastases is hyperintense on T1-weighted scans (see Fig. 6.2). Papillary thyroid cancer typically has lower mean T2 signal intensity ratio (SIR) and apparent diffusion coefficient (ADC) than benign nodules; using T2 SIR and ADC combined, MRI has 93 % sensitivity and 93 % specificity for discrimination between PTC and benign nodules [17].
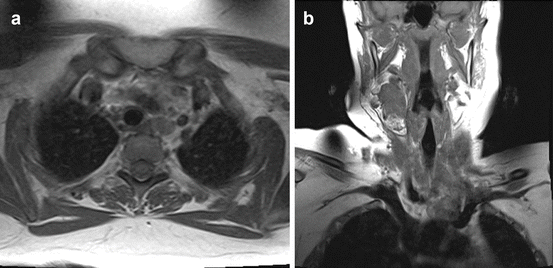

Fig. 6.2
T1 weighted axial (a) and coronal (b) images of MRI demonstrating paratracheal and neck lymphadenopathy in a patient with recurrent papillary thyroid carcinoma after total thyroidectomy
When dynamic contrast MRI was compared to US-guided FNAB in the evaluation of multinodular goiter for underlying thyroid cancer in 26 consecutive patients, Tunca et al. reported 100 % sensitivity and 100 % NPV compared to 71.4 % and 91.7 % sensitivity and NPV, respectively, for US-FNAB [18].
Positron Emission Tomography
The images generated by PET are low resolution and not suitable for operative planning. Similar to other solid organ malignancies, the primary use of PET scans is to evaluate for the presence of distant metastases (see Fig. 6.3). However, for the initial evaluation of thyroid cancer, this is achieved postoperatively with radioactive iodine scanning. Moreover, given their relatively low metabolic activity, most primary thyroid tumors and up to 70 % of metastases are non-FDG avid [19–22]. Thus, there is no role for PET or combined PET/CT scans for the initial evaluation of thyroid cancer.
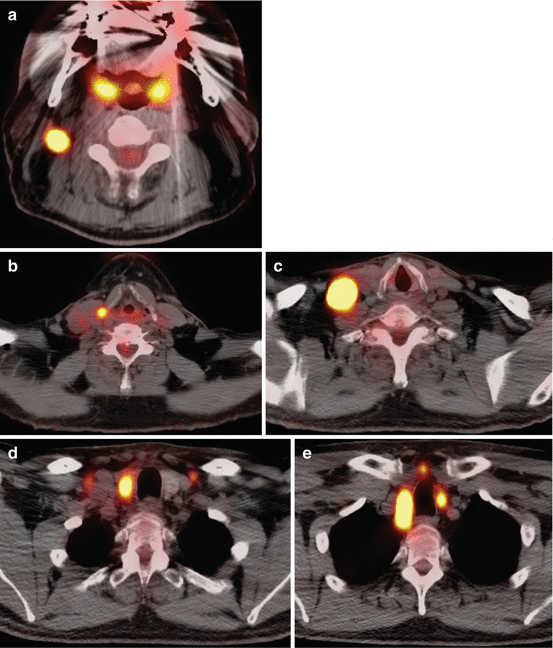

Fig. 6.3
Axial images from an 18-FDG PET/CT demonstrating (a, b, c) hypermetabolic lymphadenopathy in left neck levels II–V and a (d, e) hypermetabolic right thyroid nodule in patient diagnosed with metastatic papillary thyroid carcinoma
Surveillance for Persistent or Recurrent Thyroid Cancer
Following surgery for thyroid cancer, patients should be assessed for persistent or recurrent disease using serum thyroglobulin (either on thyroid hormone therapy or after stimulation with recombinant human TSH) in combination with a neck ultrasound at 6–12 months postoperatively. The presence of disease as indicated by serum thyroglobulin or neck ultrasound may prompt further imaging. In patients who have undergone less than a total thyroidectomy or did not undergo radioiodine ablation, the absolute value of thyroglobulin is less meaningful, but an elevation in serum thyroglobulin from baseline should raise suspicion.
Conceptually, persistent/recurrent thyroid cancer can be classified as being either cervical or extracervical, with the former usually being managed surgically and the latter often being managed nonsurgically. The degree of thyroglobulin elevation provides some guide as to the anatomic location of persistent/recurrent disease, with the most common presentation being a small-volume locoregional lymph node recurrence associated with a thyroglobulin level in the single digits [23]. For such cases, ultrasound imaging alone is adequate. Patients with suspected extracervical disease may be evaluated with (1) diagnostic whole body scanning with radioactive iodine, (2) thin-cut non-contrast chest CT, or (3) 18 F-FDG PET scanning.
18 F-FDG PET scanning is most strongly indicated in the patient with suspected extracervical disease and negative radioactive iodine imaging [24–27]. The 2015 ATA guidelines recommend PET scanning in patients with negative RAI imaging and thyroglobulin greater than 10 ng/ml [2]. As some high-grade tumors dedifferentiate, they may lose their affinity for iodine and simultaneously become more hypermetabolic on PET scan [28]. The sensitivity and specificity of PET/CT in I131-negative patients with suspicion of persistent or recurrent disease has been reported at 81 and 89 % [29]. The sensitivity of PET/CT may be improved with TSH stimulation [30].
Similar to the indications for chest CT in the initial evaluation for thyroid nodules and thyroid cancer, CT should be considered when there is extensive bulky lymphadenopathy and/or signs and symptoms of local invasion of aerodigestive structures. Additionally, chest CT should be obtained in patients with negative US and high serum thyroglobulin (>10 ng/ml) or rising serum thyroglobulin. While MRI can be considered as an alternative imaging modality for the neck, it is not as sensitive for pulmonary nodules as chest CT.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree