(1)
Department of Surgery, Dar A lAlafia Medical Company, Qatif, Saudi Arabia
17.1 Introduction
Sickle cell anemia is a common hemoglobinopathy seen in many parts of the world.
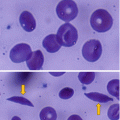
It is characterized by periods of remissions and exacerbations called crisis. These are secondary to deoxygenation which results in aggregation and polymerization of HbS tetramers in the red blood cells, leading to distortion of the red blood cells forming sickle-shaped red blood cells.
Sickling of RBC is seen more commonly in areas with low blood flow including the splenic sinusoids, the bone marrow, and the penile corpora during an erection. This will result in a vicious cycle of inflammation, hypoxia, and acidosis resulting in more sickling, vessel occlusion, and ischemia. One of these devastating complications is priapism.
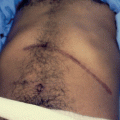
Priapism is a sustained, painful penile erection in the absence of sexual activity or desire (Figs. 17.1 and 17.2, 17.3 and 17.4, 17.5 and 17.6).
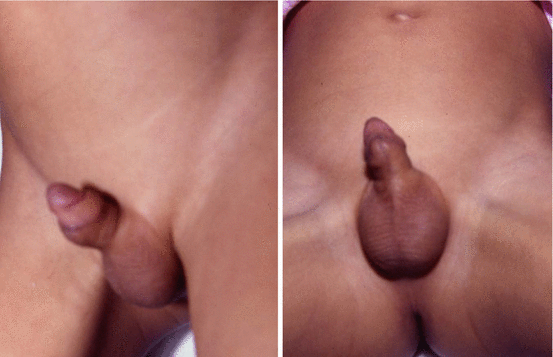
Figs. 17.1 and 17.2
Clinical photographs showing priapism in a child with sickle cell anemia
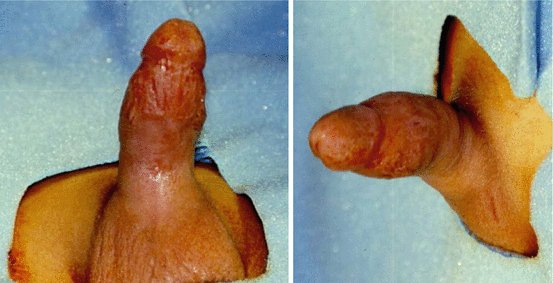
Figs. 17.3 and 17.4
Clinical photographs showing priapism in a child that did not respond to conservative treatment
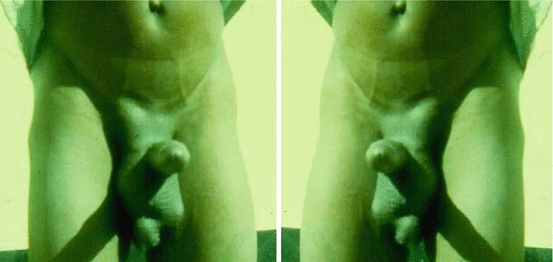
Figs. 17.5 and 17.6
Clinical photographs showing priapism in an adult with sickle cell anemia
The exact prevalence of priapism in SCA is not known and ranges from 2 to 35 %.
It has been estimated that up to 35 % of men with sickle cell anemia are affected by priapism.
Early recognition and appropriate treatment of priapism in males with SCA is critical, as prolonged and/or repeated attacks of priapism can lead to ischemia and fibrosis in the corpora cavernosa of the penis. This ultimately leads to impaired sexual function and impotence.
17.2 Classification
Priapism is prolonged painful erection of the penis often starting in the early hours of the morning.
Priapism develops when there is excess arterial inflow to the penis or when there is persistent venous outflow obstruction to the penis.
Priapism is classified into two types:
High-flow arterial priapism. This is also called nonischemic priapism.
Low-flow priapism. This is also called ischemic priapism.
High-flow priapism is usually seen following trauma causing injury to the cavernosal artery.
The penis in high-flow priapism is neither fully rigid nor painful and does not require an emergency treatment.
Low-flow priapism is the classic type seen in patients with SCA where there is stasis leading to hypoxia and acidosis of venous blood in a normally erected penis. This will lead to sickling of RBCs within the corpora cavernosa venous sinusoids, venous outflow obstruction, and engorgement of the corpora cavernosa. The corpora spongiosa and glans of the penis are spared.
The corpora cavernosa becomes rigid and tender to palpation.
Low-flow priapism is considered a medical and surgical emergency.
The two types of priapism can be differentiated using color duplex Doppler ultrasonography and analysis of blood aspirated from the corpora cavernosa.
Color duplex Doppler ultrasonography measures blood flow. This typically shows little or no blood flow in the cavernosal arteries in those with low-flow priapism.
Analysis of blood aspirated from the corpora cavernosa is done at the time of aspiration and irrigation.
In patients with high-flow priapism, the aspirated blood is bright red and has a pO2 >90 % mmHg, pCO2 <40 mmHg, and a pH of approximately 7.40.
In patients with low-flow priapism, the aspirated blood is dark in color and has a pO2 <30 mmHg, pCO2 >60 mmHg, and a pH <7.25.
Priapism is also classified in two types:
Stuttering priapism: this lasts 2–4 h, often recurrent and may precede a severe attack.
Severe priapism: this lasts longer than 4 h and can result in impotence.
17.3 Pathophysiology of Priapism
Anatomically, the penis is composed of two corpora cavernosa and one corpora spongiosum.
The two corpora cavernosa are made up of smooth muscles and covered in a tunica albuginea. This is made up of two layers, an inner layer that supports the cavernous tissue and an outer layer that runs longitudinally from the glans to insert onto the pubic rami.
The inner and outer layers of the tunica albuginea are connected by emissary veins.
The corpora spongiosum on the other hand has no tunica albuginea and, therefore, serves as an arteriovenous fistula with less rigidity than the corpora cavernosa. The urethra runs within the corpora spongiosum.
Normally, erection results from corporal smooth muscle relaxation secondary to the release of neurotransmitters.
The principal neurotransmitter for erection is nitric oxide (NO), which is released by both nerve terminals and endothelial cells. The NO then diffuses into both trabecular cells and arterial smooth muscle cells. This activates guanylate cyclase, which catalyzes the formation of cGMP from GTP, and results in a cascade that decreases intracellular calcium and opens potassium channels to cause smooth muscle relaxation.
This results in increased blood flow and filling of the corpora cavernosa sinusoids with blood and ultimate compression of venous outflow and trapping of blood.
Alternative pathways generate cAMP, which enhances this effect.
Detumescence follows degradation of cGMP and cAMP. cGMP is degraded by phosphodiesterase-5 (PDE5).
Stasis and low blood flow rates within the sinusoids of the erectile tissue make the penis a site at high risk for developing a veno-occlusive crisis in SCA.
Typically, in priapism, the corpora cavernosa are tense, congested, and tender to palpation, while the glans and corpus spongiosum are usually soft and uninvolved.
Classically, in priapism, the primary mechanism is thought to be obstruction of venous drainage resulting in viscous, hypoxic blood leading to interstitial edema and fibrosis of the cavernosa, ultimately resulting in impotence.
It was shown that the length of time of ischemia directly correlates with the likelihood of return of erectile function, and therefore, ischemic priapism is considered a urologic emergency.
It was shown that all patients with ischemic priapism episodes of greater than 12 h duration had reduction in erectile function and no patients with priapism lasting greater than 36 h had return of spontaneous erectile function.
In patients with SCA, several factors contribute to the development of priapism including anatomic factors and a low-flow state.
In males with SCA, the basic pathology of priapism is venous obstruction of the corpora cavernosa blood flow.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree