(1)
Department of Surgery, Dar A lAlafia Medical Company, Qatif, Saudi Arabia
19.1 Introduction
Sickle cell anemia is one of the common hemoglobinopathies around the world.
It results from a single change of one amino acid valine instead of glutamic acid in the sixth position among the 146 amino acids of the beta chain of hemoglobin.
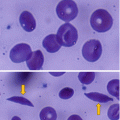
This change produces abnormally rigid, sickle-shaped red blood cells that hemolyze easily and adhere to each other blocking blood vessels and can lead to life-threatening complications.
A single change of one amino acid in the hemoglobin beta chain can lead to so much morbidity and sometimes mortality.
Currently, there is no cure for sickle cell anemia, and for many years, the treatment was symptomatic and directed to relive their pain and anemia. This as well as preventing and treating sickle cell anemia related complications.
Bone marrow transplantation is the only potential cure for these patients, but this is very expensive and not readily available.
The treatment of sickle cell anemia is directed:
To relieve the pain which is usually secondary to vaso-occlusive crisis
To treat associated anemia
To prevent infections
To prevent and manage various SCA-related complications
Pain management:
Pain is treated depending on its severity.
Usually nonsteroidal anti-inflammatory drugs (NSAIDs) are used to treat mild to moderate pain.
Sever pain requires the use of opioids.
It is important to control the dose of opioids as an overdose can cause respiratory depression and hypoventilation which can be complicated further by atelectasis and acute chest syndrome.
It is also important to monitor the use of these strong analgesics as the patients can easily become addicted to them.
Patient-controlled analgesia is an alternative and effective way to control pain in patients with severe pain.
Sickle cell anemia patients with high HbF level usually have a milder disease, and it has been suggested that hemoglobin F exhibits its favorable influence through inhibition of hemoglobin S polymerization and thus survival of hemoglobin F containing cells and less sickling.
It is important to treat these patients at specialized centers with nurses and hematologist experienced in treating sickle cell anemia.
Antibiotics:
Antibiotics are given to treat infections at various sites and also as long-term prophylaxis to infants and children and those who had splenectomy.
Penicillin is usually given as a prophylactic antibiotic to prevent infection. It can be given intramuscularly once every 3 weeks or more preferably orally twice daily.
The empirical use of antibiotics to treat infections in patients with sickle cell anemia should take in consideration the fact that these patients are prone to develop Salmonella infections at various sites. These antibiotics should be broad spectrum and cover Salmonella till the result of cultures which must be taken prior to the start of antibiotics.
Vaccinations:
Vaccinations play an important role in the management of patients with sickle cell anemia.
All children with sickle cell anemia should receive their normal immunizations regularly.
Patients who are going to have splenectomy should be immunized at least 2 weeks before splenectomy for an effective immune response. If splenectomy is performed on an emergency basis, immunization should be given as soon as possible following splenectomy. The immunizations should include:
Pneumococcal vaccine
Meningococcal vaccine
H influenza vaccine
There are however recent advances in the management of patients with sickle cell anemia. These include:
Hydroxyurea
Blood transfusion
Bone marrow or stem cell transplantation
19.2 Hydroxyurea
Normally the hemoglobin present in the fetus is called HbF. This is made up of two alfa and two gamma chains (α2γ2).
This persists in the newborn until about 6 months of age, and subsequently it is replaced by the normal adult hemoglobin.
The normal adult hemoglobin is made up of two alfa and two beta chains (α2β2).
In some patients with sickle cell anemia, HbF may persist at higher levels into adulthood.
Higher levels of fetal hemoglobin in patients with sickle cell anemia were shown to be beneficial, and these patients have a milder disease.
Fetal hemoglobin production can be reactivated pharmacologically which was shown to be useful in the treatment of sickle cell anemia.
Hydroxyurea (Droxia) is not a cure for sickle cell anemia but a drug that stimulates the production of HbF.
Hydroxyurea is recommended to treat adolescents and adults with moderate-to-severe sickle cell anemia. This is defined as a sickle cell crisis occurring three or more times a year.
Hydroxyurea was shown to reduce the frequency of these attacks and also reduces episodes of acute chest syndrome.
It is important to know that not all patients with sickle cell anemia respond to hydroxyurea, but the benefits appear to be long lasting.
There are reports of similar response to hydroxyurea treatment in children with sickle cell anemia, but there are reports of severe side effects, and so it is still being investigated as a therapy for young patients with sickle cell anemia.
Hydroxyurea however is not without side effects and these include:
Constipation
Nausea
Drowsiness
Hair loss
Inflammation of the mouth
Neutropenia
Thrombocytopenia
There have been concerns that long-term use of hydroxyurea may increase the risk of developing leukemia, but the significance of this risk remains unclear.
Hydroxyurea should not be given to pregnant women as it can cause birth defects.
19.3 Blood Transfusion
The half-life of sickled red blood cells is shorter than normal red blood cells.
As a result of early red blood cell hemolysis, these patients have chronic anemia, but sometimes excessive hemolysis can lead to acute anemia.
The normal hemoglobin levels for patients with sickle cell anemia are around 8 g/dL.
Treating sickle cell-related anemia will improve the low oxygen-carrying capacity caused by the severe anemia, and this in turn will reduce further sickling.
Blood transfusions are often necessary and form part of the management of patients with sickle cell anemia.
The indications for blood transfusions in patients with sickle cell anemia can be divided into three main groups:
To correct severe anemia
To treat specific episodes (episodic blood transfusion)
Chronic transfusion therapy to prevent life-threatening complications
The aim of blood transfusion should be to increase the hemoglobin level to around 10 g/dL after transfusion.
A higher Hb level will increase the viscosity of the blood and may precipitate vaso-occlusive crisis.
Treating severe anemia:
In general, patients should be transfused if there is evidence of physiologic derangement, such as heart failure, dyspnea, hypotension, or marked fatigue.
There is no universally accepted Hb level at which blood transfusion should be given.
A hemoglobin level less than 5 g/dL or a 20 % fall below the baseline during an acute illness is considered common indications for blood transfusion.
Simple packed RBC transfusion rather than whole blood is used to treat anemia.
Episodic blood transfusion:
This is indicated to manage sudden acute and severe complications of sickle cell anemia. These include:
Acute chest syndrome
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree