(1)
Department of Surgery, Dar A lAlafia Medical Company, Qatif, Saudi Arabia
Sickle cell anemia (SCA), which is due to homozygous inheritance of the HbS variant, is one of the commonly inherited hemoglobinopathies worldwide.
Patients with SCA often require operative interventions to treat SCA-related complications.
This however is associated with an increased risk of perioperative complications particularly vaso-occlusive crisis and acute chest syndrome.
Anesthesia and surgery are historically associated with an increased incidence of morbidity and mortality.
Recent multicenter data still found perioperative complications in 22 % of sickle cell patients undergoing elective surgery.
Optimal surgical outcome requires careful preoperative, intraoperative, and postoperative management by a team consisting of a surgeon, anesthesiologist, and hematologist.
Acute chest syndrome (ACS) is a well-documented postoperative complication in patients with SCA with an incidence ranging from 0.4 to 10 %.
The acute chest syndrome can be mild, moderate, or severe (Figs. 18.1, 18.2, and 18.3).
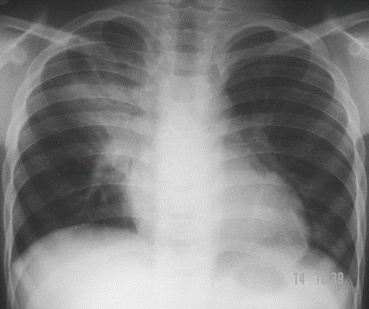
Fig. 18.1
Chest X-ray showing mild postoperative acute chest syndrome
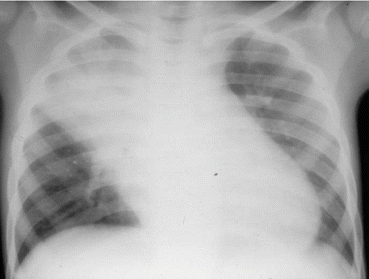
Fig. 18.2
Chest X-ray showing a moderate postoperative acute chest syndrome in patient with sickle cell anemia
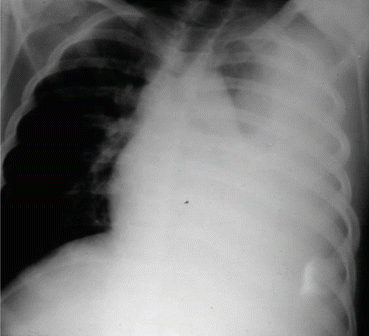
Fig. 18.3
A chest X-ray showing a severe postoperative acute chest syndrome which developed following splenectomy
A high HbF level (HbF level >20 %) has a protective effect and reduces the risk of postoperative ACS.
For many years, surgery on patients with SCA was associated with an unacceptably high complication rate, sometimes as high as 50 %.
These complications are part of the disease process and usually develop secondary to intraoperative or immediate postoperative events such as hypoxia, hypovolemia, hypothermia, and acidosis.
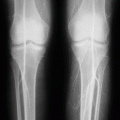
Although these complications can be seen following any operative procedure, they are more commonly seen in those undergoing thoracotomy or laparotomy (Figs. 18.4 and 18.5).
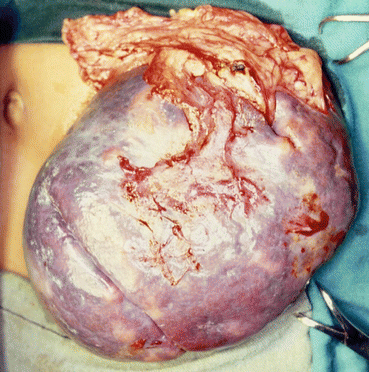
Fig. 18.4
A clinical intraoperative photograph showing laparotomy to remove a large spleen in a child with sickle cell anemia
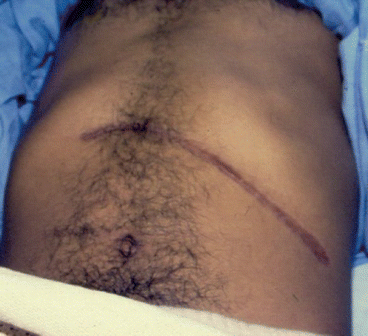
Fig. 18.5
A clinical postoperative photograph showing a large abdominal wound following splenectomy and cholecystectomy. Such a large wound may be complicated by a postoperative acute chest syndrome
Nowadays and in spite of better understanding of SCA, improved anesthetic and surgical techniques, and careful perioperative management, the perioperative complication rate in these patients is still high.
Earlier studies reported a perioperative mortality rate as high as 10 % and a postoperative complication rate of up to 50 %, and because of this unacceptably high complication rate, they advocated against surgery except in symptomatic patients.
To minimize these risks, a variety of perioperative management protocols, including different preoperative blood transfusion regimens, have been adopted.
Blood transfusion is considered part of the preoperative management of patients with sickle cell anemia.
Perioperative blood transfusion to correct the anemia and decrease the percentage of HbS level is beneficial in reducing the rate of SCA-related complications, but the amount of blood transfusion necessary for safe surgery is not known.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree