Androgen hypersecretion in a premenopausal woman may be due to an ovarian tumor, an adrenal tumor, polycystic ovarian syndrome, or nonclassic congenital adrenal hyperplasia. The expansiveness of the diagnostic evaluation of a woman with androgen excess is dependent on the clinical situation and the degree of androgen hypersecretion. Herein we present a case of a patient with abrupt onset of marked hirsutism as a result of a testosterone-secreting Sertoli-Leydig cell tumor of the ovary.
Case Report
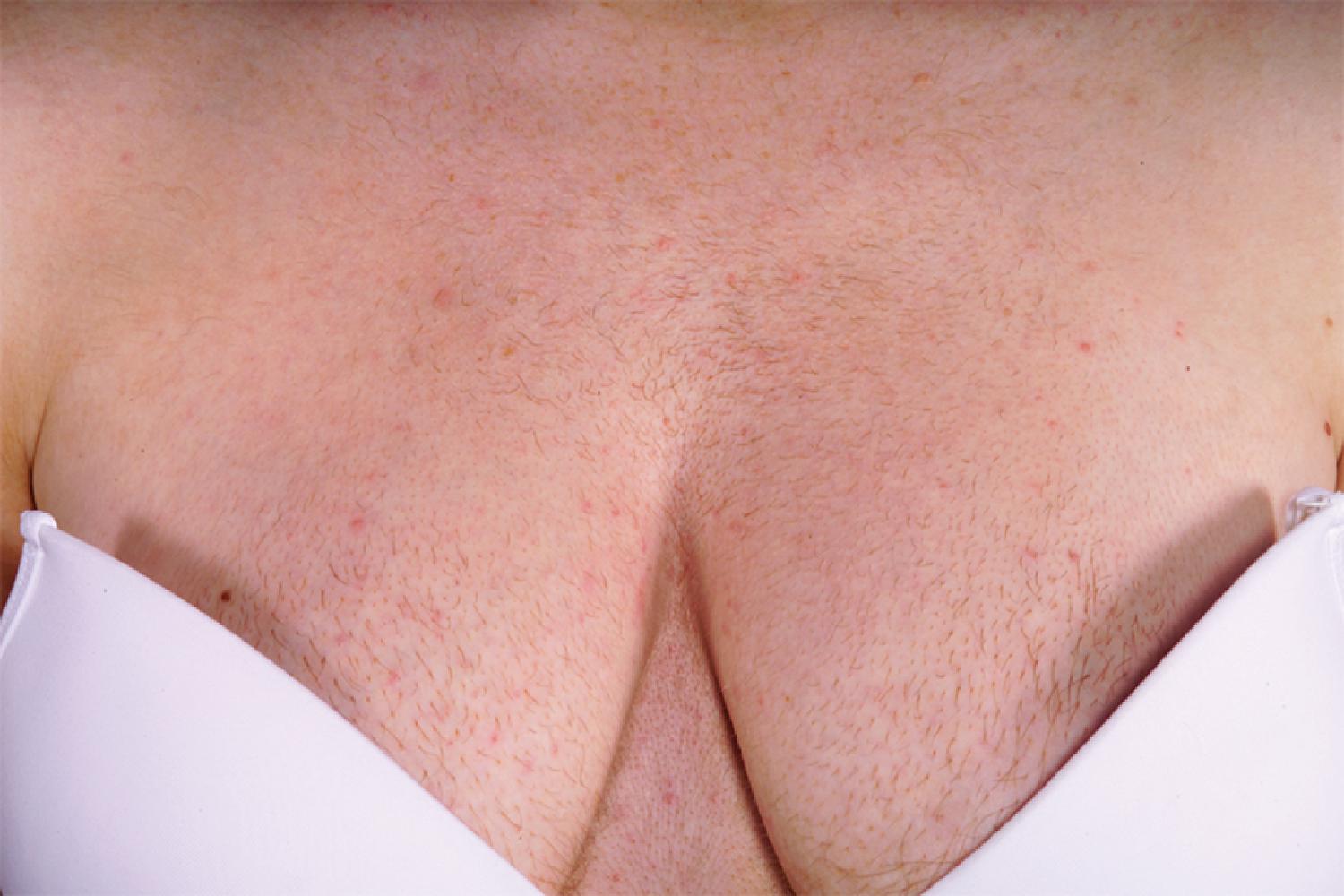
This 25-year-old woman was doing reasonably well until 18 years of age, when she noticed some increased amount of hair on her chin. Two years ago she noticed the hair was becoming significantly worse on the chin and neck, and then about 1 year ago she noticed onset of hair growth over her entire chest and abdomen, increased dense hair on her forearms, increased hair on the upper arms, and the onset of secondary amenorrhea. She had not noticed any change in scalp hair, the pitch of her voice, libido, skin oiliness, or acne. She did note that it was easier to tone her muscles with weight training. She had normal blood pressure and no signs or symptoms of Cushing syndrome. An evaluation 4 months before referral showed a total testosterone of 349 ng/dL (normal, 8–60 ng/dL) and an ovarian ultrasound that showed prominent-sized ovaries but no mass. On physical examination her body mass index was 23.7 kg/m 2 , blood pressure 115/57 mmHg, and heart rate 58 beats per minute. Her degree of hirsutism was marked with a modified Ferriman-Gallwey score of 28 (normal, <8; maximum 36) ( Fig. 91.1 ). Clitoromegaly was not present. She had no signs or symptoms of Cushing syndrome.
INVESTIGATIONS
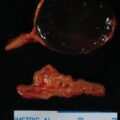
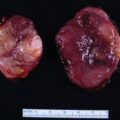
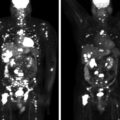
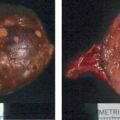
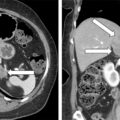
Laboratory test results are shown in Table 91.1 . Marked testosterone and androstenedione hypersecretion was documented. An abdominal computed tomography (CT) scan showed micronodular changes in both adrenal glands. Transvaginal ultrasound showed the right ovary to be enlarged and a 1.7 cm × 2.4 cm × 2–cm complex cystic area within the right ovary with an appearance consistent with a hemorrhagic corpus luteum cyst, or, in this specific patient, potentially a testosterone-producing ovarian tumor ( Fig. 91.2 ). Venous sampling of the adrenal and gonadal veins was nonlocalizing ( Box 91.1 ). In general, we have had good success with gonadal venous sampling in women with an ovarian source of androgen excess (e.g., see Case 92). However, gonadal venous sampling, just like adrenal venous sampling, lacks 100% accuracy. F-18 fluorodeoxyglucose (FDG) positron emission tomography (PET) showed mild FDG avidity in the right ovary ( Fig. 91.3 ).
| Biochemical Test | Result | Reference Range |
| Sodium, mEq/L Potassium, mEq/L Creatinine, mg/dL Total testosterone, ng/dL Free testosterone, ng/dL Bioavailable testosterone, ng/dL Androstenedione, ng/dL Estradiol, pg/mL LH, IU/L | 140 4.4 0.9 392 10.6 243 944 50 13.2 | 135–145 3.6–5.2 0.7–1.2 8–60 0.3–1.9 0.8–10 30–200 Premenopausal: 15–350 Luteal: 0.7–12.9 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree