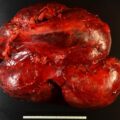
There is no cure for metastatic paraganglioma (PGL). The first step in the management ofmetastatic PGL is to assess the rate of tumorprogression and, once determined, provide a proportionate treatment. When the number of metastatic PGL lesions exceeds what can be managed with local/targeted treatments (e.g., ablation and radiation therapies) and the pace of increase in overall tumor bulk becomes excessive, systemic treatment should be considered. The first systemic treatment to consider is cytotoxic chemotherapy with the protocol of cyclophosphamide, vincristine, and dacarbazine (CVD). Although CVD chemotherapy is not curative, it can provide remarkable remissions in disease. Herein we demonstrate the role for chemotherapy with CVD.
Case Report
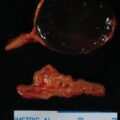
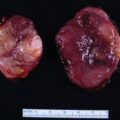
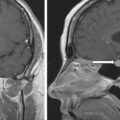
The patient was a 38-year-old man seen in endocrine consultation for an abdominal paraganglioma (PGL) diagnosed elsewhere on a computed tomography (CT)-guided biopsy. He had been experiencing low back discomfort with jogging, and a lumbar spine magnetic resonance image (MRI) was obtained. Incidentally noted was a retroperitoneal mass. A subsequent CT scan confirmed a 3.7 × 5.5 × 5.5–cm peripherally enhancing solid mass in the retroperitoneum anterior to the inferior vena cava (IVC). He had no paroxysmal symptoms or history of hypertension. He had a niece who was recently diagnosed with metastatic catecholamine-secreting abdominal PGL. On physical examination his body mass index was 29.1 kg/m 2 , blood pressure 142/78 mmHg, and heart rate 54 beats per minute. He was physically fit.
INVESTIGATIONS
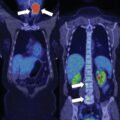
The laboratory tests showed that the PGL was nonfunctioning ( Table 50.1 ). Germline genetic testing found a large gene deletion (promotor and exon 1) in succinate dehydrogenase subunit B ( SDHB ). I-123 metaiodobenzylguanidine (MIBG) scintigraphy showed that the PGL was not MIBG-avid.
| Biochemical Test | Result | Reference Range |
| Sodium, mmol/L | 143 | 135–145 |
Potassium, mmol/L | 4.8 | 3.6–5.2 |
Creatinine, mg/dL | 1.0 | 0.8–1.3 |
Plasma metanephrine, nmol/L | <0.2 | <0.5 |
Plasma normetanephrine, nmol/L | 0.5 | <0.9 |
24-Hour urine: | ||
Metanephrine, mcg | 132 | <400 |
Normetanephrine, mcg | 418 | <900 |
Norepinephrine, mcg | 52 | <80 |
Epinephrine, mcg | 6.2 | <20 |
Dopamine, mcg | 353 | <400 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree