There is no cure for metastatic pheochromocytoma or metastatic paraganglioma (PPGL). The first step in the management of metastatic PPGL is to assess the rate of tumor progression and, once determined, provide a proportionate treatment. Targeted treatments are preferred over systemic treatment options in patients with a limited number of or slowly progressive metastases. Here we present the use for thermal ablation in treatment of metastatic paraganglioma.
Case Report
The patient was a 47-year-old woman who presented for evaluation of left neck lump. She first noticed the lump approximately 5 years earlier. The lesion had progressively grown since and had become apparent to her friends and family, prompting further evaluation. She was asymptomatic. Her medical history was negative and she was not taking any medications. Family history was positive for a surgery to remove a neck lesion in her father at age 78 and a possible carotid body tumor in her sister.
On physical examination, her body mass index was 27.3 kg/m 2 , blood pressure was 141/79 mmHg, and heart rate was 69 beats per minute. She had a 7 × 6–cm left upper neck mass that was mobile and nontender. There was no lymphadenopathy. The rest of the examination was normal.
INVESTIGATIONS
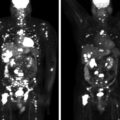
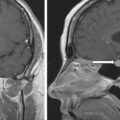
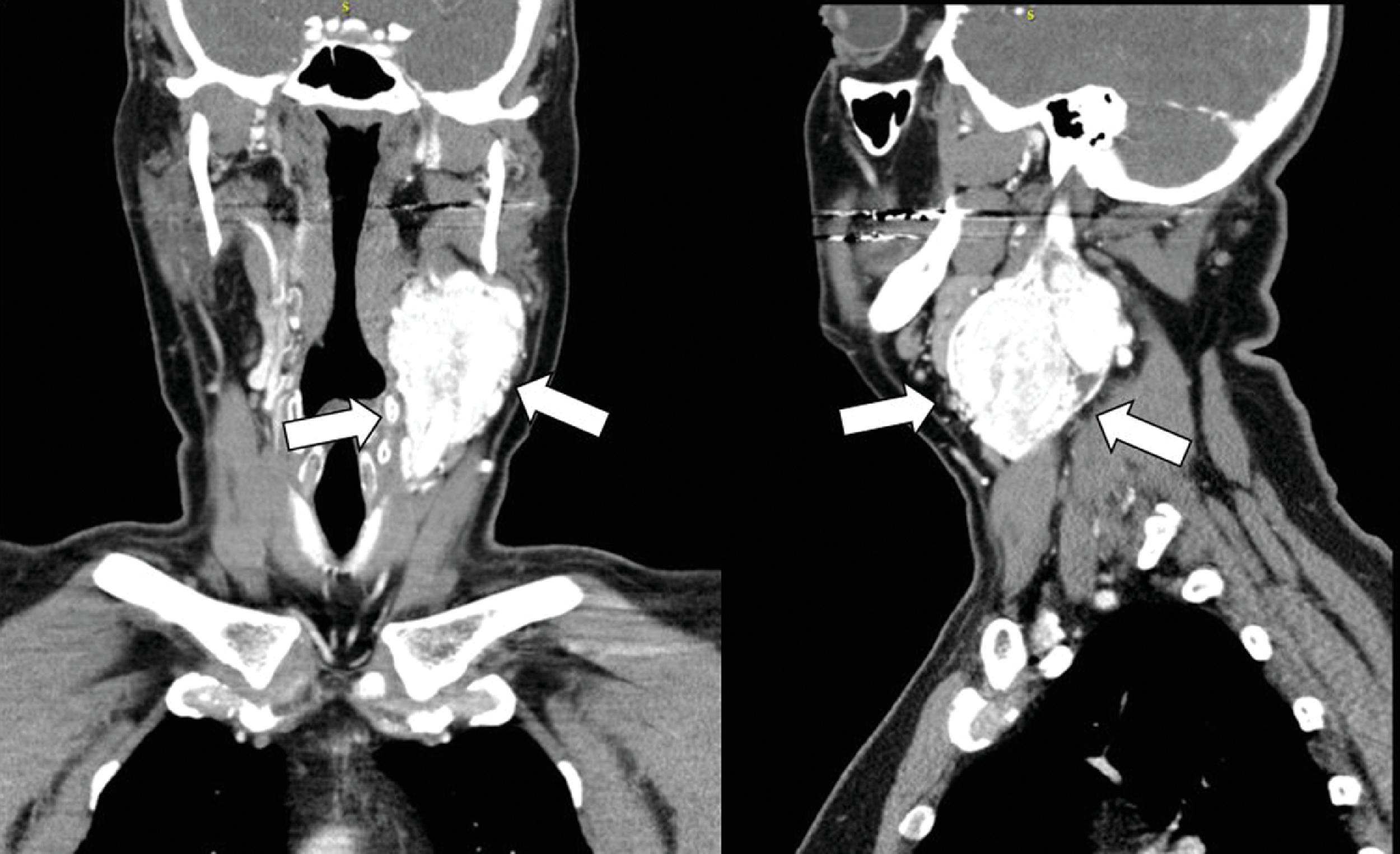
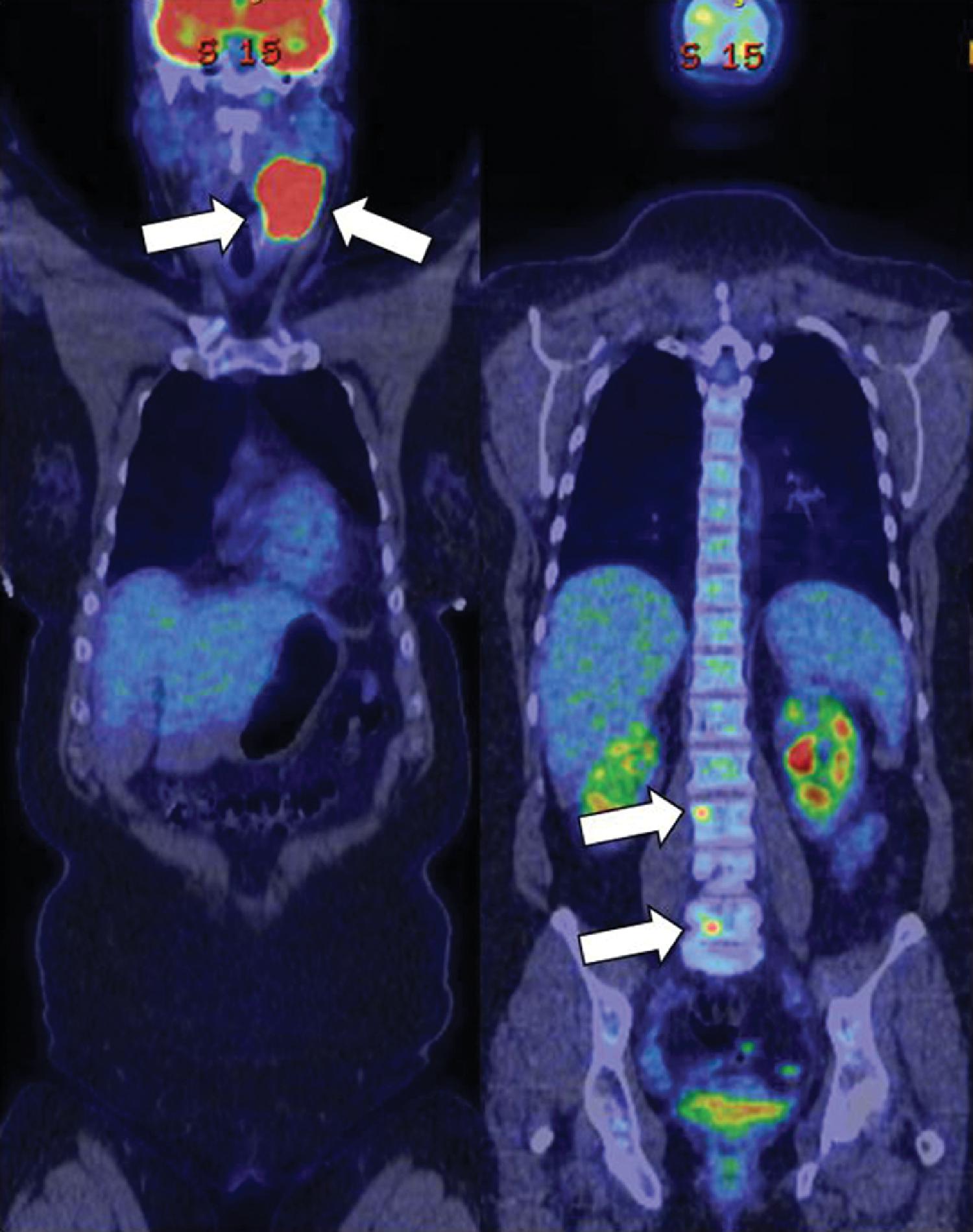
Computed tomography (CT) scan of the neck demonstrated a bilobed enhancing left neck mass measuring 6.2 × 4.2 × 9.5 cm, consistent with carotid body tumor ( Fig. 51.1 ). An F-18 fluorodeoxyglucose (FDG) positron emission tomography (PET)-CT scan showed intense uptake in the left cervical mass and hypermetabolic lesions in L3 and L5 vertebral bodies, likely representing metastases ( Fig. 51.2 ). The laboratory tests confirmed that the metastatic PGL was biochemically nonfunctioning ( Table 51.1 ).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree