Bilateral macronodular adrenal hyperplasia (BMAH) is typically a computed tomography (CT)-based diagnosis. Patients with multiple endocrine neoplasia type 1 (MEN-1) may present with normal-appearing adrenal glands, solitary adrenal adenomas, or BMAH. When adrenal nodularity is detected in a patient with MEN-1, it is important to determine if it is associated glucocorticoid secretory autonomy—either clinically evident Cushing syndrome or subclinical Cushing syndrome (also referred to as “mild autonomous cortisol excess”). When BMAH is associated with glucocorticoid secretory autonomy, adrenal venous sampling is not needed because, by definition, the disorder is bilateral. Dependent on the degree of symptomatology and comorbidities, management options include observation, unilateral adrenalectomy of the larger adrenal gland, or bilateral adrenalectomy. If the patient has subclinical Cushing syndrome (mild autonomous cortisol excess), then there is the opportunity to resect the larger adrenal gland to debulk the disease. Herein we share such a case.
Case Report
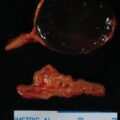
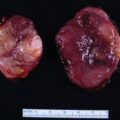
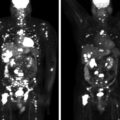
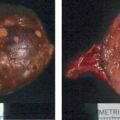
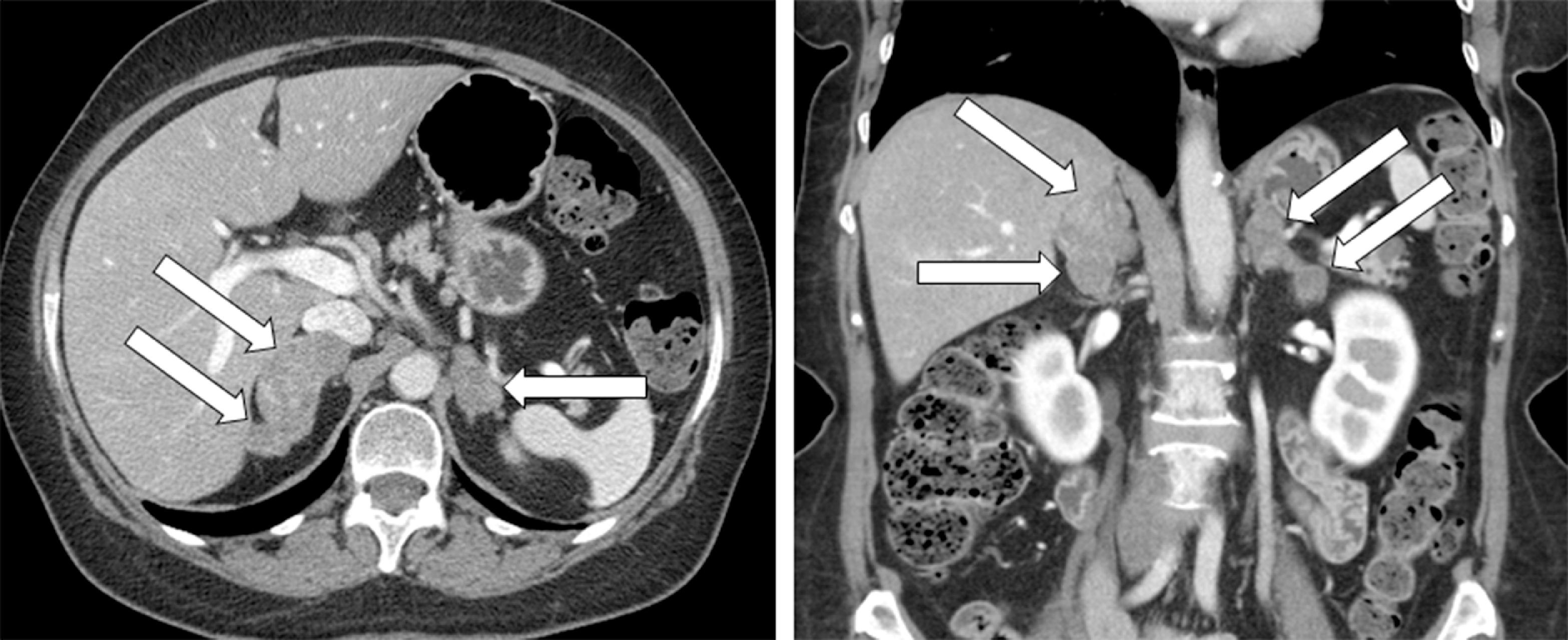
Six years before consultation at Mayo Clinic this 63-year-old woman was diagnosed with MEN-1 (based on multigland hyperparathyroidism and a family history of MEN-1). The visit to Mayo Clinic was triggered by the finding of BMAH on the abdominal CT scan that was performed to assess her pancreas ( Fig. 84.1 ). Adrenal nodularity was noted on a CT scan 7 years previously, but no evaluation was performed. Although she did not have overt clinical Cushing syndrome, she did have excessive bruising, mild facial plethora, type 2 diabetes mellitus treated with two oral agents (metformin and glipizide), and hypertension treated with two drugs (lisinopril and metoprolol). In addition, she was recently found to have osteopenia. On physical examination her body mass index was 29.3 kg/m 2 , blood pressure 148/86 mmHg, and heart rate 63 beats per minute. She did not appear clinically cushingoid. She did not have hirsutism or purple red striae. Her skin turgor was normal. Proximal muscle weakness was not evident.
INVESTIGATIONS
The laboratory test results are shown in Table 84.1 . The diagnosis of glucocorticoid secretory autonomy was based on the following: low serum corticotropin (ACTH) concentration; low-normal serum dehydroepiandrosterone sulfate (DHEA-S) concentration; mild elevation in 24-hour urinary free cortisol excretion and lack of complete suppression in serum cortisol with an overnight 8-mg dexamethasone suppression test (DST) ( Table 84.1 ).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree