16118
Lung Cancer
Shreya Sinha, Mariam Alexander, and Ajeet Gajra
INTRODUCTION
Lung cancer is the leading cause of cancer death in the United States (1). It was estimated that 224,390 new cases of lung cancer would be diagnosed in 2016, with 158,080 deaths expected. Even though lung cancer accounts for 14% of all new cancer diagnoses, it is the leading cause of cancer-related mortality in both men and women. In addition, more than 50% of lung cancers are diagnosed in patients aged 65 and older; less than 2% of cases occur in individuals less than 45 years of age (1,2).
PATHOPHYSIOLOGY
Lung cancer can be broadly divided into non–small-cell lung cancer (NSCLC) and small cell lung cancer (SCLC) based on the cell type of origin. Malignant transformation of neuroendocrine cells leads to SCLC, whereas NSCLC originates from epithelial cells. Based on histopathological analysis, NSCLC is further classified into broad categories of adenocarcinoma, squamous cell carcinoma, and large cell carcinoma, with adenocarcinoma accounting for more than half of all cases of lung cancer (3). There are numerous molecular pathways involved in the pathogenesis of NSCLC. Of these, mutations in genes encoding epidermal growth factor receptor (EGFR) and anaplastic lymphoma kinase (ALK) are best characterized for targeted therapies (4). Other proteins that are currently targeted in NSCLC, albeit at lower frequencies, include ROS1, HER2, BRAF, MET, and RET (5,6). While EGFR mutations are commonly encountered in older patients, especially women with no smoking history, recent data analyzing NSCLC suggest that overall, older patients may be more likely to harbor MET mutations than EGFR or KRAS mutations (7). There are no currently available inhibitors against the MET pathway, though trials are ongoing.
CLINICAL FEATURES
Signs and symptoms that are initially encountered in the patient will depend on the subtype, location, and distant metastasis. Presenting symptoms in the elderly may include weight loss, chest pain, ongoing cough, dyspnea, chronic pneumonia, or hemoptysis (8). Mediastinal involvement can manifest as superior vena cava syndrome, pericardial effusion, pleural effusion, and dysphagia. Apical growth or Pancoast tumor can 162cause brachial plexus compression and Horner syndrome. Paraneoplastic syndromes can be seen in both SCLC (e.g., Cushing syndrome, syndrome of inappropriate antidiuretic hormone secretion [SIADH]) and NSCLC (hypercalcemia, hypertrophic osteoarthropathy, and digital clubbing) (9). Frequent sites of metastasis are brain, bone, liver, and adrenal glands.
INITIAL EVALUATION AND STAGING
All patients with lung cancer, especially those with early stage, potentially operable disease, should undergo a PET/CT scan to evaluate mediastinal and occult disease. A cytologic or histopathological evaluation of the tumor is necessary for diagnosis and molecular analysis of the cancer. Tissue can be obtained through flexible bronchoscopy, transthoracic needle biopsy, or pleural fluid analysis. Mediastinal nodal sampling can be accomplished by mediastinoscopy or endobronchial ultrasound (EBUS)-guided nodal sampling. Tumor factors (stage, histological subtype, specific molecular profile) and patient factors (performance status [PS]; comorbidity, nutritional, cognitive, and psychological status; as well as social support) dictate treatment options, likely outcomes, and overall prognosis, especially in the elderly. This is the reason geriatric assessment (GA) tools, as described later in the chapter, can assist clinicians and patients with treatment decisions. Lung cancer is staged based on the TNM system where T defines the extent of the tumor, N is regional lymph node involvement, and M is metastasis (10). Historically, SCLC was staged as limited and extensive stage. Limited stage is defined as tumor being confined to one hemithorax and ipsilateral lymph nodes, which can be included in a single radiation port; tumor extent beyond this definition is designated as extensive stage.
MANAGEMENT
Management strategies for NSCLC vary depending on the stage (Table 18.1).
Early Stage NSCLC: Stages I and II
The primary modality of treatment for stage I disease is surgical resection. In a Surveilance, Epidemiology, and End Results (SEER) database study, lobectomy was found to have better long-term survival rates compared to sublobar resection, conventional radiation, observation, and stereotactic body radiation therapy (SBRT) (10). However, the elderly population is offered surgery less often due to poor postsurgical outcomes secondary to age (11,12).
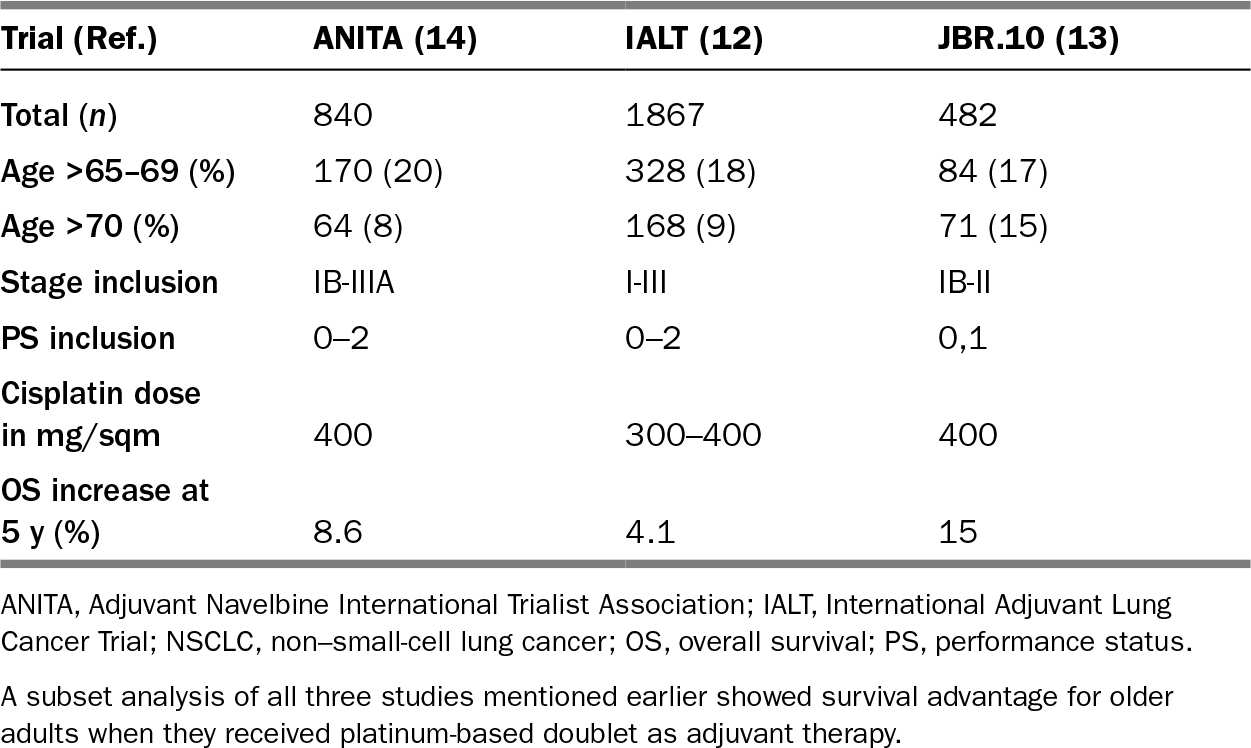
Stage II disease has limited regional spread of the tumor and is still amenable to surgery with the addition of adjuvant platinum-based chemotherapy. All patients with stage II or III and stage IB (≥4 cm) should be offered platinum-based adjuvant chemotherapy for four cycles. Of the trials done to establish the efficacy of adjuvant chemotherapy in patients with early stage NCSLC, none had adequate representation of the elderly (13–15). Age-based post hoc analysis of the patients from these trials did demonstrate an overall survival benefit in the elderly patients who received adjuvant platinum-based therapy (Table 18.2). A separate pooled analysis of elderly patients receiving adjuvant cisplatin-based chemotherapy revealed no difference in toxicity rates in the elderly (>70) compared to young patients (<65) (16). There was significant benefit despite reduction in dose due to toxicity. Platinum-based chemotherapy is now the standard of care in elderly patients except in patients aged 80 or older, a group that has not been studied (17,18). It is reasonable to consider carboplatin-based chemotherapy in the elderly who have contraindications to cisplatin (19).
TABLE 18.1 Treatment Options for NSCLC Based on Staging for the Elderly
163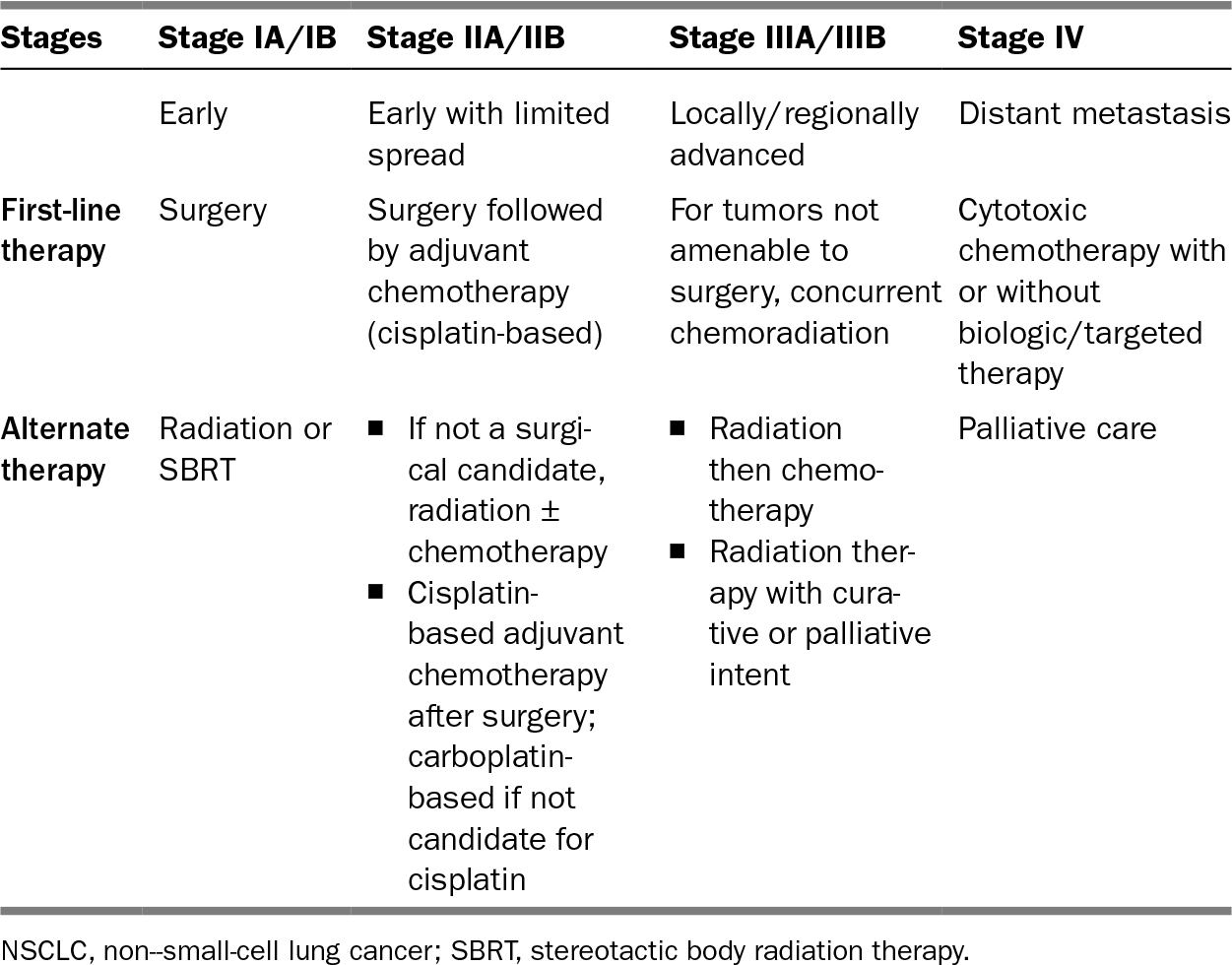
TABLE 18.2 Major Trials of Adjuvant Chemotherapy in NSCLC
164SBRT: SBRT is a treatment option for inoperable early stage NSCLC. SBRT uses small, focused radiation beams tracking the tumor, typically in three to five treatments. In a study of elderly patients with T1-T3N0M0 NSCLC, SBRT was shown to lower risk of death compared to those who did not receive any treatment; thus, SBRT should be offered to patients who are not candidates for surgical resection (20).
Locally Advanced Disease: Stage III
Almost a third of NSCLC patients have stage III or locally advanced disease (2). In the United States, a minority of such patients undergo resection depending on tumor volume, lung function, comorbidity, and PS, and these patients should be offered adjuvant chemotherapy. The gold standard for patients with good PS irrespective of age is concurrent chemoradiotherapy. In age-unspecified trials, older patients with good PS have shown improved survival with chemoradiation compared to radiation alone, although elderly-specific prospective trials are scarce (21–23). Concurrent chemoradiation can be complicated by radiation esophagitis; thus, special attention to nutritional status is essential. Other acute complications include myelosuppression and infections, and esophageal stricture, malnutrition, and radiation pneumonitis can occur later in the course. Frail elderly with high comorbid burden are not candidates for concurrent chemoradiation and should be treated with radiation therapy alone (24).
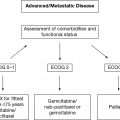
Metastatic/Palliative Disease: Stage IV NSCLC
Treatment options for stage IV disease are either single-agent chemotherapy or platinum-based doublet cytotoxic therapy based on the patient’s PS. It has been shown that single-agent chemotherapy improves outcomes in elderly patient compared to best supportive care alone (25). Data are conflicting regarding benefit of chemotherapy doublets, although one trial limited to the elderly did demonstrate benefit for a paclitaxel and carboplatin combination compared to single-agent chemotherapy in fit elderly (26–29) (Table 18.3). There are no data specific to the elderly regarding the use of maintenance chemotherapy. The role of bevacizumab is limited because older patients do not appear to derive the same amount of benefit as younger patients and suffer more toxicity (30). All patients with advanced adenocarcinoma of the lung should be tested for mutations in the EGFR, ALK, and ROS1 genes. If such driver mutations are detected, then an appropriate oral targeted agent should be the first line of therapy: EGFR (erlotinib, gefitinib or afatanib), ALK (crizotinib, ceritinib, or alcetinib), and ROS1 (crizotinib).
Immunotherapy in Older Adults for NSCLC
The recent advent of immune checkpoint inhibition for NSCLC has offered additional treatment options. These inhibitors work to enhance the response of the immune system to tumor cells by targeting proteins that regulate the immune system, such as programmed cell death protein 1 (PD-1). In two recently reported trials, one limited to patients with squamous NSCLC and the other to nonsquamous NSCLC, patients with progression after chemotherapy were randomized to a PD-1 antibody (nivolumab) or docetaxel (31,32). In these trials, 42% to 44% of patients were aged more than 65 and 7% to 11% were older than 75 years of age. Nivolumab was associated with improved overall survival in both trials (9.2 vs. 6 months in squamous, P < .001 and 12.2 vs. 9.4 months in nonsquamous trial, P = .002). Pembrolizumab, another anti-PD-1 monoclonal antibody, was recently approved as first-line treatment of untreated advanced NSCLC with PD-L1 expression on at least 50% of tumor cells, based on higher progression-free survival and response rates when compared to platinum-based chemotherapy (33). In this trial, 54% patients were age 65 or older and experienced the same benefit with immunotherapy as younger patients. Although the toxicity profile of these agents differs from that of cytotoxic chemotherapy, these are fairly well tolerated in older adults with good PS.
TABLE 18.3 Important Trials Specific to Elderly in Advanced NSCLC
165
Small Cell Lung Cancer
Although SCLC has a lower rate of incidence (12%–15% of all lung cancer), it is more aggressive and has higher rates of recurrence. There has been little improvement in the enrollment of older adults to trials in SCLC over the past two decades (34). SCLC is more chemosensitive compared to NSCLC. The cornerstone in the treatment of SCLC is chemotherapy with a platinum agent (cisplatin or carboplatin) combined with a topoisomerase inhibitor (etoposide or irinotecan). Thoracic radiation is added concurrently for limited-stage disease in patients with good PS. Given the high toxicity associated with cisplatin (emetogenecity, ototoxicity, neuropathy, and nephrotoxicity), carboplatin 166is commonly substituted for older adults. SCLC has a high propensity to metastasize to the brain and hence prophylactic cranial irradiation is recommended in patients with limited disease with good response to chemotherapy. The Food and Drug Administration (FDA)-approved second-line agent topotecan has limited efficacy and high toxicity. Other agents, like taxanes and gemcitabine, may be used with palliative intent in the relapse setting. The combination of immunotherapeutic agents nivolumab and ipilumumab has shown some early promise in relapsed disease (35).
GA TOOLS
GA and its abridged versions can assist in risk stratification and thus improve decision making and outcomes in elderly patients with lung cancer. Various GA domains have been associated with poor survival in lung cancer, including Eastern Cooperative Oncology Group (ECOG) PS, instrumental activity of daily living (IADL) I dependency, dementia, depression, weight loss, albumin level, and frailty (36). In a study specific to elderly with advanced NSCLC, higher scores for pretreatment quality of life and IADLs were associated with better prognosis, whereas another found association between comorbidity and survival (26,37). In early stage disease, preoperative GA can predict postoperative morbidity and mortality: In a prospective study, preoperative cognitive dysfunction increased the risk for postoperative complications, delirium, and dependency for activities of daily living (ADLs) (38). In one study, it changed therapeutic decisions in half of the vulnerable patients with lung cancer (39). Though not specific to lung cancer, other GA-based tools have demonstrated the ability to predict chemotherapy-associated toxicity in the elderly, allowing for improved decision making and limiting toxicity (40,41). A multicenter trial confirmed that there is decreased toxicity with no decrement in survival when GA-based treatment allocation strategy is used in elderly patients with advanced lung cancer (42). Because these assessment tools have shown good predictive ability for toxicity, it is recommended that some form of GA be included in the initial assessment of an older adult.
ROLE OF PALLIATIVE CARE
Currently, palliative care is typically consulted only in later stages and late in the course of disease. However, studies have shown that early utilization of palliative care is associated with improvement in mood, quality of life, and survival (43). These findings may have some variations based on age and gender (44).
SCREENING RECOMMENDATIONS
Smoking causes 85% to 90% of lung cancers (45). The National Lung Screening Trial found that low-dose CT screening significantly reduces mortality from lung cancer (46). The United States Preventive Services Task Force now recommends annual low-dose helical CT scan of the thorax for patients age 55 to 80 with a history of smoking at least 30 pack-years, or if they were previous smokers and have quit within the past 15 years (47). Plain chest radiograph has been shown to be an ineffective tool for screening and should not be used (48).
TAKE HOME POINTS
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree