Chapter Outline
Technology and automation in blood transfusion laboratories 472
Pretransfusion compatibility systems 473
Quality assurance in the transfusion laboratory 475
ABO and RhD grouping 475
Antibody screening 479
Antibody identification 481
Selection and transfusion of red cells 482
Crossmatching 483
Emergency blood issue 485
Compatibility testing in special transfusion situations 486
Neonates and infants in first 4 months of life 486
Intrauterine (fetal) transfusion 487
Patients receiving transfusions at short intervals 487
Allogeneic haemopoietic stem cell transplantation 488
Investigation of a transfusion reaction 488
Antenatal serology and haemolytic disease of the fetus and newborn 490
Haemolytic disease of the fetus and newborn 491
Antenatal serology 491
Prediction of fetal blood group 491
Antenatal assessment of the severity of haemolytic disease of the fetus and newborn 492
Anti-D immunoglobulin prophylaxis 492
ABO haemolytic disease of the newborn 494
ABO titrations 494
Safe and effective blood transfusion requires the combined efforts of blood transfusion services, biomedical scientists and clinicians to ensure the highest standards are applied to all the systems in a complex process from ‘vein to vein’. This chapter provides a description of the laboratory framework required to provide the right blood components to the right patients at the right time. The increased awareness of what can go wrong with blood transfusion comes from national haemovigilance schemes including the Serious Hazards of Transfusion (SHOT) UK scheme, which was started in 1996. SHOT, a confidential reporting scheme for serious adverse reactions and events relating to transfusion, analyses reaction-specific questionnaires and makes a detailed root cause analysis of errors. The data, learning points and recommendations provided in an annual report have informed both national bodies and local transfusion services of measures to introduce in order to reduce risk ( Fig. 22-1 ). It is clear that multiple errors can contribute to a single adverse event and that many of these are outside the control of the transfusion laboratory.
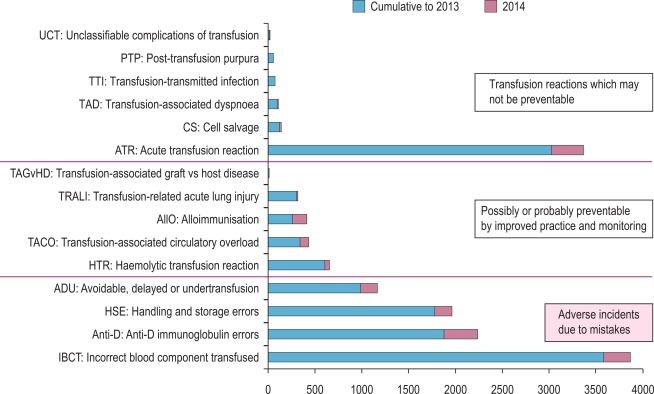
Within the laboratory setting, the application of strict protocols for sample labelling and testing, robust laboratory procedures, reliable documentation, frequent staff training and competency assessment should be used. Recognising that a high proportion of wrong blood errors arise in the laboratory, the UK Transfusion Collaborative, comprised of representatives of the professional bodies involved in UK transfusion practice, produced some recommendations about training, competency, staffing levels and automated systems in 2009 and these were upgraded to best practice standards in 2014.
This chapter is concerned with the testing of patient samples prior to the provision of appropriate compatible blood components including identification of red cell antibodies. It also covers compatibility testing, investigation of transfusion reactions and the testing required in other special situations including the antenatal and postnatal settings. National professional bodies such as the British Committee for Standards in Haematology (BCSH) issue technical and clinical guidance to transfusion laboratories, and these have been referenced where appropriate.
In the UK there is a regulatory framework governing hospital transfusion laboratory practice which was implemented after the publication of two European Union Directives: 2002/98/EC and 2004/33/EC. In the UK these are the Blood Safety and Quality Regulations 2005 (BSQR, Statutory Instruments 2005/50, 2005/1098 and 2006/2013) and they set standards for quality and safety of human blood and blood components in hospital ‘blood banks’ (hospital transfusion laboratories) as well as ‘blood establishments’ (the UK Blood Services). ‘Blood banks’ are regulated in their roles of storing, distributing and performing compatibility tests on blood and blood components for use in hospitals. The implications for hospital transfusion practice are the requirement for ‘vein to vein’ traceability of blood components, the importance of maintaining the ‘cold chain’ for all therapeutic blood components, the need to store transfusion records for 30 years and the requirement for a quality management system. UK laboratories have to assess their compliance by completing and submitting an annual compliance report to the competent authority, which is the Medicines and Healthcare products Regulatory Agency (MHRA). The MHRA carries out laboratory inspections of a proportion of ‘blood banks’ to assess compliance with these regulations.
Three UK Government Health Service Circulars entitled “Better Blood Transfusion” were published in 1998, 2002 and 2007, promoting a team approach to blood transfusion safety and good transfusion practice through a structure of Hospital Transfusion Committees and Hospital Transfusion Teams. The European Union Optimal Use of Blood Project produced a resource for anyone who is working to improve the clinical transfusion process, and this covers laboratory and clinical practice. The World Health Organisation (WHO) also provides resources to support blood transfusion safety.
Technology and automation in blood transfusion laboratories
Important changes have taken place in the blood transfusion laboratory in the last 10–15 years, as outlined in the previous edition of this book. As a result, transfusion laboratory practice is safer, largely as a result of the implementation of new technologies for testing, the introduction of automated systems to replace manual systems and the widespread use of information technology (IT) systems to support transfusion laboratory practice.
Barcoded labels on blood components, reagents, patient samples and equipment are now commonplace, and these result in safer transfer of information, free from the transcription errors associated with manual methods. It is estimated that in the UK, 97% of routine group and screens are undertaken using full automation.
Column agglutination (CAT) and solid-phase technology can be used on automated machines, and CAT can also be used by manual techniques. In UK hospital transfusion laboratories these technologies have replaced tube techniques and liquid-phase microplates for antibody screening and crossmatching.
The currently available CAT systems include Ortho BioVue ( www.orthoclinical.com ), which comprises a six-well cassette containing a glass microbead matrix, ID Bio-Rad cards utilising Sephadex gel matrix, also with six wells, and an eight-well Sephadex gel matrix card from Grifols ( www.grifols.com ). Each offers a wide range of profiles and reagent systems. Other similar formulations produced by different commercial companies are available outside of the UK.
The currently available solid-phase systems are Immucor Capture-R ( www.immucor.com ) and Bio-Rad Solidscreen II ( www.bio-rad.com ). The Immucor system utilises a range of red cell antigens that have adhered to the surface of a U-shaped microplate well. Sensitised red cells are then used as a marker. The Bio-Rad Solidscreen II is a solid-phase method for antibody screening and identification. The wells of the microplates are coated with protein A so that the reaction results in a solid-phase cell layer bound to the plate.
Individual laboratories need to make careful and informed decisions when selecting reagents for pretransfusion testing. It is vital that any abbreviated testing in an automated or semiautomated system is carefully evaluated for the risks that could ensue if important controls were omitted when using this technology for blood grouping.
Laboratory information management systems (LIMS) store patient details and results of laboratory tests, allowing timely and accurate access to important information. In the transfusion department, IT systems have a much broader use, and the updated BCSH guidelines for the specification and use of IT systems in blood transfusion practice (2015) reflect this. Where possible, using bidirectional or unidirectional interfaces to automated blood grouping analysers, IT systems are used to eliminate errors that can arise when a manual step is employed, including in interpretation of test results.
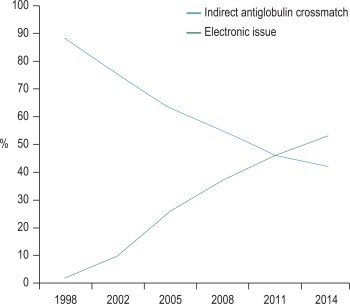
Computer algorithms support the ‘electronic issue’ of blood to patients with a negative antibody screen without the need to perform an antiglobulin crossmatch, and in the UK in 2014, 53% of laboratories were using this system for some or all of their patients ( Fig. 22-2 ). The use of automation for all aspects of compatibility testing is now recommended practice and recognised as safer than manual techniques. Automation brings several or all of the discrete activities of compatibility testing into a single-platform process. It provides various levels of increased security over manual testing and may provide justification for abbreviated pretransfusion testing (e.g. stopping duplicate D typing or reverse ABO grouping in the presence of a valid historical group). A risk assessment must be made and documented prior to any abbreviation of an established procedure, with consideration being given to the presence or absence of key functions in the automated equipment. The BCSH guidelines for pretransfusion compatibility procedures and guidance from the MHRA give a list of factors to be taken into consideration. The reader is advised to consult these prior to implementing automated or semiautomated systems.
Pretransfusion compatibility systems
The process of providing blood for transfusion involves many steps, all of which have to be reliably completed. These include the following:
- •
Blood samples have to be taken from the correct patient and labelled at the bedside in a single uninterrupted procedure. The sample must be identified by four core patient identifiers handwritten on the sample label: the correctly spelled first name and last name, the exact date of birth and an accurate unique patient number (ideally the NHS number or equivalent, but a hospital medical records number is acceptable). The sample should be dated and signed by the person taking the sample. The laboratory should have a policy for rejecting badly labelled samples. In a UK national comparative audit of collection and labelling of samples sent for pretransfusion testing, 2.99% were rejected. The hospitals participating in this audit showed considerable variation in the content and application of sample acceptance policies. UK guidelines recommend that preprinted ‘addressograph’ labels are not accepted on blood samples for pretransfusion compatibility testing, because acceptance increases the risk of ‘wrong blood in tube’ (WBIT). In an international study from the Biomedical Excellence for Safer Transfusion (BEST) collaborative, it was estimated that these miscollected samples occurred at a median rate of 0.5 per 1000, with a great variation worldwide in the reported frequency of mislabelled samples, probably resulting from variation in sample acceptance policies. Labels printed at the bedside using barcoded patient wristband and hand-held scanners are acceptable. Unless secure electronic patient identification systems are in place, it is recommended that a second sample collected at a different time is taken for confirmation of the ABO group of a first-time patient prior to transfusion, as long as this does not impede the delivery of urgent red cells or other components.
- •
A request for testing or issue of blood components can be made electronically, in writing or exceptionally in an urgent situation, by phone. In addition to the previously outlined four core patient identifiers, the request should include clear information about the source of the request and the location of the patient. Clinical details should include the justification for the request, such as the indication for transfusion. Previous transfusion history and any special considerations for the selection of blood components are also needed. Specific requirements could include antigen-negative red cells if the patient has a clinically significant antibody, extended matched red cells in a patient with a haemoglobinopathy or irradiated cellular blood components for certain groups of immunosuppressed patients. The use of ‘order-comms’ or computerised provider order entry (CPOE) systems can improve the accuracy and completeness of transfusion requests as well as being of use to challenge requests that do not comply with the hospital’s transfusion policy.
- •
An ABO and D group of the patient sample must be accurately performed.
- •
An antibody screen of the patient’s plasma (or mother’s plasma in the case of a neonate) should be able to detect any red cell antibodies of potential clinical significance. In the event of a positive red cell antibody screen, antibody identification should be undertaken to assist the selection of compatible blood.
- •
There should be a check of existing transfusion records to compare current and historical results. When LIMS are upgraded or replaced, results of previous ABO and D groups, antibody identification and specific requirements on the legacy system should preferably be migrated to the new LIMS, but alternatively should be accessible in real-time to support the correct selection of blood components for issue to named patients.
- •
The appropriate blood component should be selected and issued to a named patient using a serological crossmatch or electronic issue.
- •
Traceable documentation should exist to ensure that the results of laboratory compatibility procedures are available at the patient’s bedside to allow a check before transfusing the blood component. This should include a blood bag compatibility label ( Fig. 22-3 ) and may include a compatibility form. The patient must be identified with an identification wristband containing the four core identifiers, and the blood component should be prescribed on a drug or fluid administration chart. In some countries, an additional bedside check of the patient’s blood group is undertaken prior to commencing the transfusion.
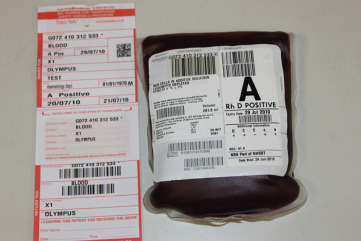
Figure 22-3
A unit of red cells showing the compatibility label.
Documentation of the transfusion process
All stages of the transfusion process must be clearly documented, and these records must be kept. In addition to guidance from the UK Royal College of Pathologists on the retention of pathological records and specimens, the BSQR 2005 regulations stipulate that the records must be accessible for 30 years. This allows any blood component to be traced from the donor to the recipient should information come to light about any potential infective risks to the recipient.
Computer records are easier to search than paper records, but LIMS are likely to become obsolete and be replaced several times within this mandatory 30-year period, so provision must be made to store historical data in an accessible format when procuring a replacement computer system. Patient-held records are useful for patients who are treated in more than one institution, particularly if they have red cell antibodies and require phenotyped blood or if they have special requirements because of their underlying disease or its treatment. Credit card-sized records with corresponding patient information leaflets are issued by some transfusion centres to patients with red cell antibodies, and similar cards exist for patients who require irradiated cellular blood components.
Blood samples and their storage requirements
Depending on laboratory practice, blood transfusion tests use a clotted (serum) sample or ethylenediaminetetra-acetic acid (EDTA)-anticoagulated blood (plasma). Most laboratories using automated systems will use a plasma sample because it is difficult to make a cell suspension from a clotted sample. An incompletely clotted blood sample may contain small fibrin clots that trap red cells into aggregates that could resemble agglutinates that could be falsely interpreted as a positive reaction in an automated system. When plasma is used, complement is inactivated by the EDTA, which may result in complement-binding antibodies (e.g. of Kidd specificity) being missed or giving weak reactions by the indirect antiglobulin test (IAT). In serum samples the presence of complement can cause lysis. If laboratory staff are accustomed to recognising agglutination as an indicator of a positive reaction they may fail to interpret the lysed red cells as an equally valid positive reaction. Therefore, when using serum for blood grouping and compatibility testing, any red cells in the test system should be washed and resuspended in saline that contains EDTA (see later). In addition, false-negative reactions may occur in immediate spin crossmatching with potent ABO antibodies, where rapid complement fixation causes a prozone effect (bound C1 inhibits agglutination). EDTA saline is not necessary when using plasma.
Throughout this chapter, for the sake of brevity, the term ‘plasma’ is used, as the majority of UK laboratories are automated and therefore plasma samples are required. If serum samples are specifically required, this will be indicated in the text.
On being received in the laboratory, the details on the request form must be checked against the blood sample. Each blood sample must be labelled with a unique sample number. Barcode labels offer the advantage of positive sample identification and reduce the number of transcription errors. Samples inadequately or inaccurately labelled should NOT be used for pretransfusion testing.
Great care must be taken to select and identify the sample prior to any testing. Transposition of samples in the laboratory can lead to an incorrect blood group being assigned to a patient, with serious consequences, including ABO incompatible transfusions.
Whole blood samples should be tested as soon as possible because they will deteriorate over time. Problems associated with storage include lysis of the red cells, bacterial contamination, decrease in potency of antibodies (particularly immunoglobulin (Ig) M antibodies) and loss of complement in serum samples. To ensure that the specimen used for compatibility testing is representative of a patient’s current immune status, serological studies should be performed using blood collected no more than 3 days in advance of the actual transfusion when the patient has been transfused or has been pregnant within the preceding 3 months, or when such information is uncertain or unavailable. The BCSH guidelines from which this advice is taken are summarised in Table 22-1 .
| Patient Type | Sample Type | ||
|---|---|---|---|
| Whole Blood at Room Temperature | Whole Blood at 2–8 °C | Plasma at − 30 °C | |
| Patient transfused or pregnant within last 3 months | Up to 48 h | Up to 3 days * | Not applicable |
| Patient not transfused or pregnant in last 3 months | Up to 48 h | Up to 7 days | Up to 3 months |
* This is the time between the sample being taken and the subsequent transfusion.
Where possible, the primary sample should be used for testing. If samples are separated, the plasma must be clearly and accurately identified. It is important to have a system to ensure that the correctly identified sample has been retrieved from the storage location. If repeated testing on a sample is anticipated, storing separate small aliquots reduces the risk of sample deterioration, which occurs with repeated thawing/freezing of larger samples. If separated samples are stored for later serological testing or electronic issue, care must be taken to ensure that the patient has not been transfused in the interim. So although antibodies are probably stable for up to 6 months, it is safer to obtain another sample after 3 months.
It has been recommended that samples should be retained for at least 3 days post-transfusion for investigation of acute transfusion reactions and where feasible stored for 7–14 days post-transfusion to enable investigation of delayed transfusion reaction. ,
quality assurance in the transfusion laboratory
Test systems used for pretransfusion testing are important because errors can and do lead to patient morbidity and mortality. Chapter 25 covers the general aspects of a laboratory quality assurance system, and specific guidance for transfusion laboratories can be found in the BCSH guidelines for validation and qualification as well as the guidelines for pretransfusion compatibility procedures in blood transfusion laboratories.
The quality management system for a hospital transfusion laboratory should include the following:
- •
Quality control: The appropriate use of internal quality controls and participation in external quality assessment exercises where available.
- •
Validation: Automated equipment and computer systems should be validated to ensure that they function as specified and back up procedures should be in place to cover the failure of automated equipment and computers.
- •
Policies and procedures: There should be standard operating procedures (SOPs) available which cover all aspects of the laboratory work, and these must be reviewed and updated regularly.
- •
Reagents, calibrators and control materials: They should correspond to the specification given in the Guidelines for the Blood Transfusion Services and should be used in accordance with the manufacturer’s instructions. As they are included under the In-vitro Diagnostics (IVD) Medical Devices Directive they must be CE (Conformité Européenne) marked ( www.gov.uk/ce-marking ).
- •
Preventative maintenance: The regular checking and maintenance of all laboratory equipment must be documented.
- •
Training and competency testing: Laboratory tasks should only be undertaken by appropriately trained staff, and there should be a documented programme for training laboratory staff, which covers all SOPs in use and which fulfils the documented requirements of the laboratory. There must be a documented programme for assessing staff proficiency, which should include details of the action limits for retraining.
- •
Quality incidents and exceptions: There should be a system in place for documenting and reviewing all incidents of noncompliance with procedures. A programme of independent audits should be conducted to assess compliance with documented ‘in-house’ procedures.
ABO and RhD grouping
Fully automated systems should be used where possible to reduce the risks of interpretation and transcription errors. ABO and RhD (D) grouping must be performed by a validated technique with appropriate controls. Before use, all new batches of grouping reagents should be checked for reliability by the techniques used in the laboratory. Grouping reagents should be stored according to the manufacturer’s instructions.
ABO grouping
ABO grouping is the single most important serological test performed in compatibility testing; consequently, it is imperative that the sensitivity and security of the test system is not compromised. The fact that anti-A and anti-B are naturally occurring antibodies allows the patient’s plasma to be tested against known A and B cells in a ‘reverse’ group. This is an excellent built-in check. Fully automated analysers linked to secure LIMS have the ability to prevent erroneous ABO grouping due to errors in either transcription or interpretation, with the consequence that some laboratories now omit the reverse group when testing samples for which a historical group is available. This should only be considered following a careful risk assessment and taking into account that the first sample taken may have been from the wrong patient. This has been estimated to be in the order of 1:2000 samples. A full group should therefore be performed on all samples from first-time patients, with the exception of those from neonates since red cell antibodies are not usually produced within the first 4 months of life, and any reactions found in the reverse group are therefore likely to arise from maternal ABO antibodies. Any discrepancy between the forward and reverse groups should be investigated further, and any repeat tests should be undertaken using cells taken from the original sample rather than from a prepared cell suspension.
Reagents for ABO grouping
Monoclonal anti-A and anti-B reagents have replaced polyclonal reagents in routine grouping tests. A 1 and B cells are used for reverse grouping; group O cells or an ‘ auto control ’ may be included to ensure that reactions with A and B cells are not a result of the presence of cold autoantibodies. A diluent control should be included where recommended by the manufacturer.
D grouping
D grouping is usually undertaken at the same time as ABO grouping for convenience and to minimise clerical errors that may arise through repeated handling of patients’ samples. In the absence of secure automation, testing should be undertaken in duplicate, as there is no counterpart of the ‘reverse’ grouping of ABO testing.
Reagents for D grouping
Monoclonal reagents do not have the problem of possible contamination with antibodies of unwanted specificities, as was the case with polyclonal reagents. With secure automation, a single IgM monoclonal anti-D reagent that does not detect DVI (see below) may be used. If secure automation is not in use, each sample should be tested in duplicate with either the same anti-D reagent or with two different IgM monoclonal anti-D reagents.
DVI is the partial D with the fewest epitopes; therefore of all the D variants, DVI individuals are those most likely to form anti-D, and a case of severe haemolytic disease of the fetus and newborn (HDFN) has been described. The use of anti-CDE reagents has led to the misinterpretation of r′ and r″ cells as D positive in UK National External Quality Assessment Service (NEQAS) exercises, and because they are of no value in routine patient typing, their use is not recommended. , Monoclonal anti-D reagents will allow detection of all but the weakest examples of weak D, negating the need to use more sensitive techniques to check the D status of apparent D negatives. However, monoclonal anti-D reagents vary widely in their ability to detect both partial and weak D, so it is helpful to use two of a similar affinity to reduce the number of discrepancies due to the detection of weak D.
Some anti-D reagents have high levels of potentiator (e.g. polyethylene glycol, PEG) and should be used with caution; a diluent control is essential to demonstrate that the diluent does not promote agglutination of the test red cells as may happen if the patient’s cells are coated in vivo with IgG; any positive reaction seen with the control, however weak, invalidates the test result. Anti-D reagents are provided by many manufacturers, and those responsible for selection and purchase should make themselves aware of the content, specificity and potentiation of the chosen reagent.
Methods
There are several techniques available for routine ABO and D grouping, including both manual tube and slide tests and liquid-phase and solid-phase microplates and columns that can be used in both manual and automated settings. Care should be taken to use the appropriate reagent, because not all reagents have been validated by the manufacturer for all techniques.
The techniques are described above (in the section on Technology and Automation in Blood Transfusion Laboratories, p. 472 ) and also in more detail in Chapter 21 . Molecular techniques for ABO blood grouping are not in routine use because serology is superior, being quicker, cheaper and accurate. ABO genotyping can be helpful to investigate anomalous ABO groups and is in use in organ transplantation where red cells from the donor are not available as well as in forensic practice and paternity testing. ,
Tube and slide tests
Spin-tube tests may be used for urgent testing, where small numbers of tests are performed at once. Slide or tile techniques are widely used in under-resourced countries for ABO and D grouping. Immediate spin tests may be used in an emergency, whereas routine tests are usually left for 15 min at room temperature (about 20 °C) before centrifugation for 1 min at 150 g. Equal volumes (1 or 2 drops from either a commercial reagent dropper or a Pasteur pipette) of liquid reagent or plasma and 2% cell suspensions are used. The patient’s red cells (diluted in phosphate buffered saline, PBS) should be tested against monoclonal anti-A and anti-B grouping reagents. The patient’s plasma should be tested against A 1 and B reagent red cells (reverse grouping). In addition, the plasma should be tested against either the patient’s own cells or group O cells (i.e. a negative control) to exclude reactions with A and B cells as a result of cold agglutinins other than anti-A or anti-B in the patient’s sample. Mix the suspensions by tapping the tubes and leave them undisturbed for 15 min. Agglutination should be read as described on p. 451.
Slide method
In an emergency, rapid ABO grouping may be carried out on slides or tiles. The method is satisfactory if potent grouping reagents are used. An immediate spin-tube test is preferable.
Liquid-phase microplate methods
Liquid-phase microplate technology provides a relatively inexpensive and secure method for batch testing when semiautomation is utilised for dispensing and reading, but it is no longer the grouping technique of choice in the UK. In 2015 a UK NEQAS survey showed that < 1% of responding laboratories were using liquid phase microplates for manual grouping, down from 41% in a similar survey in 2002.
Column agglutination techniques
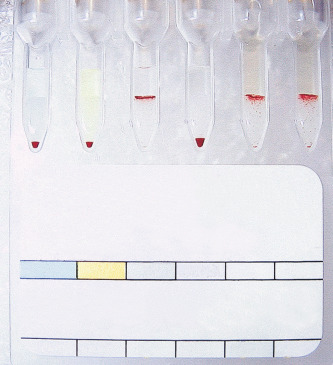
Column agglutination techniques are now the commonest method for grouping in the UK (85% of laboratories who responded to a UK NEQAS survey in 2014), especially where automated systems are in place. There are several different profiles to choose from, and some cards/cassettes include monoclonal antibodies to other blood group antigens (e.g. K). The manufacturer’s instructions should always be followed. An example is shown in Figure 22-4 , and more details can be found in Chapter 21 .
Solid-phase techniques
ABO/D grouping using solid-phase techniques would usually be part of a fully automated system, and testing should be in accordance with the manufacturer’s instructions. Bio-Rad Erytype ( www.bio-rad.com ) employs a standard agglutination technique for blood grouping performed in a microtitre plate. The reagents for the forward group are dried onto the wells. Uncoated empty wells are used with standard reagent red cells for a reverse group.
Controls for ABO and D grouping
Positive and negative controls should be included with every test or batch of manual tests. In fully automated systems, the controls should be set up at least twice in a 24-h period. The timings should take account of the length of time that reagents have been kept on the analyser. Controls should be run at start-up and when changing reagent lot numbers. Control samples should be loaded in the same way as the test samples. Where controls do not give the expected reactions, investigations should be undertaken to determine the cause of the problem and also to confirm the validity of all tests undertaken subsequent to the most recent valid control results.
Causes of discrepancies in ABO/D grouping
False-positive reactions
Rouleaux
Rouleaux may occur in various clinical conditions, where the ratio of normal albumin to globulin is altered in plasma (e.g. in multiple myeloma) and in the presence of plasma substitutes such as dextrans. The stacking of red cells on top of one another in columns may be misinterpreted as weak agglutination by inexperienced workers. Rouleaux will usually disperse on a slide if a drop of saline is added; alternatively, the reverse grouping can be repeated using plasma diluted 1 in 2 or 1 in 4 with saline.
Cold autoagglutination and cold reacting alloantibodies
Cold autoantibodies (usually anti-I) that are reactive at room temperature may lead to autoagglutination in the cell group (ABO and D) and panagglutination in the reverse group, causing a grouping anomaly (p. 262). The tests should be repeated using cells washed in warm saline and plasma prewarmed to 37 °C. An auto control should be included.
Cold reacting alloantibodies (e.g. anti-P 1 ) may cause agglutination of reverse grouping cells, and if this is suspected, reverse grouping should be repeated using prewarmed plasma or grouping cells that lack the implicated antigen.
T-activation/polyagglutination
Polyagglutination describes agglutination of red cells by all or most normal adult sera but not by the patient’s own serum. This is the result of IgM antibodies reacting with an antigen on the red cells, which is usually hidden but can be exposed by enzyme activity. The most common form is T-activation, which occurs when the bacterial enzyme neuraminidase cleaves N -acetyl neuraminic acid from the red cell membrane, exposing the T antigen.
This used to be a problem when grouping with polyclonal reagents, which contain anti-T, but tests using monoclonal reagents are not affected by this phenomenon.
Acquired B
This arises in group A 1 patients where the expected reaction with anti-A is noted but an additional weak reaction with anti-B occurs. The blood group appears to be ‘AB’ but with anti-B in the reverse group. This discrepancy between the forward and reverse grouping may be overlooked if the patient’s own anti-B is weak or if the reverse group is omitted.
The acquired B antigen is usually caused by a bacterial deacetylase enzyme acting on A 1 red cells and producing a B-like substance. Some anti-B reagents react strongly with the acquired B antigen (e.g. those derived from the ES4 clone). Such anti-B reagents are rare but should be avoided in routine blood grouping.
Potentiators
Red cells may be coated with IgG as a result of in vivo sensitisation. The use of potentiated techniques, such as the antiglobulin test for D typing, or of potentiated reagents for ABO or D typing, may result in a false-positive reaction; the latter would also result in a positive reaction with the diluent control, but UK NEQAS data have shown that some laboratories fail to include an appropriate control or fail to understand the significance of a positive control. For this reason, use of potentiated techniques or reagents for blood grouping is not advised.
In vitro bacterial contamination
In vitro bacterial contamination of reagents, patients’ red cells or reverse grouping cells may cause false-positive agglutination.
False-negative reactions
Failure to add reagents
The most likely cause of a false-negative grouping result is failure to add the reagent or test plasma. For this reason, in liquid-phase tube and plate tests, the serum or plasma should always be added first to the reaction chamber, and a visual check should be made before red cells are added. The use of colour-coded reagents for ABO grouping is helpful in this respect. Automated systems have liquid level sensors resulting in an alert indicating failure to add reagent or test plasma.
Loss of potency
Inappropriate storage or freezing and thawing may cause a loss of potency of blood grouping reagents. The regular use of controls will alert the user to this problem.
Failure to identify lysis
In the presence of complement, anti-A and anti-B may cause in vitro lysis of reagent red cells. If lysis is not recognised as a positive reaction, falsely negative results may be recorded in reverse grouping tests. To avoid this, reverse grouping cells should be resuspended in EDTA saline, where serum rather than plasma is used.
Mixed-field appearance
This describes a dual population of agglutinated and nonagglutinated red cells, which may be observed in both ABO and D grouping. It is important to recognise this as a mixed-field picture and not to confuse it with weak agglutination. The most likely cause of a mixed-field picture is the transfusion (either deliberate or accidental) of nonidentical ABO or D red cells. Investigation will be required to determine the actual blood group of the patient, who may have been transfused in an emergency or at a different establishment or who may have received an intrauterine transfusion. A mixed-field ABO group may be the first indication of a previous ABO-incompatible transfusion.
An ABO- or D-incompatible haemopoietic stem cell transplant will result in a mixed-field picture until total engraftment has occurred; the mixed-field picture may subsequently reappear if the graft is failing. Rarely, a dual population of cells is permanent and results from a weak subgroup of A (A 3 ) or a blood group chimaerism.
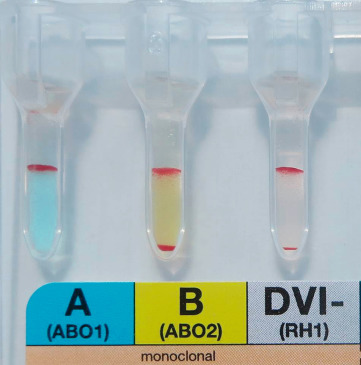
Interpretation of a dual population of red cells will depend on the technique used. In a tube, microscopic reading will reveal strong agglutinates in a background sea of free cells. In CAT cards/cassettes there will be a line of agglutinated cells at the top of the column, with the nonagglutinated cells travelling through to the bottom of the column ( Fig. 22-5 ). In liquid-phase techniques, if the reaction grade is not a strong positive or an obvious negative then the reaction requires further investigation, which may include microscopic examination. In a solid-phase technique a mixed field is seen as a dual population of cells, with the agglutination being surrounded by free cells. Automated systems should be set up to detect mixed-field pictures, and this should be used in conjunction with local policies.
D variant phenotypes
Most people are either D positive or D negative, but a minority have a variant D type, historically categorised as weak or partial D. People with a partial D antigen can make anti-D to the epitope(s) of the D antigen which they lack, when sensitised to D-positive red cells by transfusion or pregnancy. Historically, those classified as weak D, with fewer D antigen sites per red cell, but no missing epitopes, were considered unable to make anti-D, and could therefore be treated as D positive. There are two problems with using this concept to decide on whether to treat a patient as D positive or D negative: firstly, it is not always possible to distinguish serologically between weak and partial D, as many partial D antigens are also phenotypically weak; secondly, there have been many reports of patients with a variant defined as weak D having made anti-D. Daniels has suggested replacing the terms weak and partial D with a single term of D variant.
In the previous edition it was recommended that a weak reaction with a single anti-D reagent should be investigated with a second anti-D reagent before assigning a result of D positive. However, in the UK, a new patient-based algorithm has been recommended ( Fig. 22-6 ), whereby following a weak reaction with anti-D, samples from children, from women of child-bearing potential and from any patient likely to be transfusion dependent, should be investigated to determine the specificity of the D variant, with the patient being treated as D negative in the meantime. All other patients can be reported as D positive, without further investigation. Weak D types 1, 2 and 3 are the most common weak D types in a Caucasian population and rarely, if ever, make anti-D. Types 1 and 2 can be distinguished from other D variants using a panel of monoclonal antibodies, and such patients can be regarded as D positive. Identification of type 3 requires molecular testing, so if this is unavailable or not cost effective, a practical guide is to regard vulnerable patients (see above) other than those confirmed as types 1 and 2 as D negative. If in doubt, it is safer to call the patient D negative. This will be of no clinical consequence because it is safe to transfuse D negative blood to a patient who is D positive, and a pregnant woman who is D positive and her unborn child would be unlikely to be harmed by the injection of prophylactic anti-D Ig.
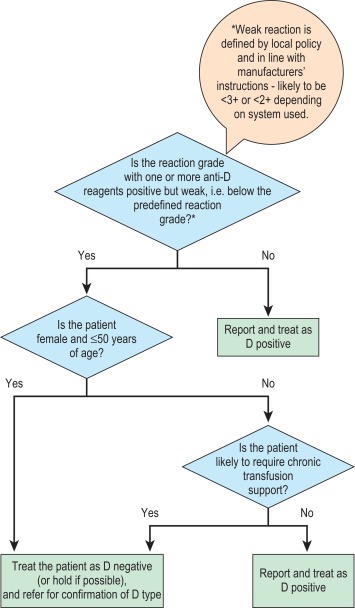
It is essential to be able to distinguish between a weak reaction and a mixed-field reaction because the latter may be the result of a patient having been transfused with blood of a different D type.
Because DVI lacks the most epitopes, such individuals are likely to make anti-D when challenged by transfusion or pregnancy. For this reason, current advice about choice of D-typing reagents is that anti-D reagents for routine grouping of patients’ samples should not detect DVI. There is little evidence to suggest that a DVI donor would elicit an immune response in a recipient who is D negative; however, weak D positive and partial D donors, including DVI donors, should be classified as D positive. There are some important ethnic differences in the frequency of different Rh haplotypes, as shown in Table 22-2 .
| Haplotype | Approximate Frequencies | ||
|---|---|---|---|
| English | Nigerian | Chinese | |
| DCe R | 0.421 | 0.060 | 0.730 |
| dce r | 0.389 | 0.203 | 0.023 |
| DcE R | 0.141 | 0.115 | 0.187 |
| Dce R 0 | 0.026 | 0.591 | 0.033 |
| dcE r″ | 0.012 | 0 | 0 |
| dCe r′ | 0.010 | 0.031 | 0.019 |
Antibody screening
Antibody screening is usually undertaken at the same time as blood grouping and in advance of selecting blood for transfusion. Antibody screening may be more reliable and sensitive than crossmatching against donor cells because some antibodies react more strongly with red cells with homozygous expression (double dose) of the relevant antigen than with those with heterozygous expression (single dose) – most notably anti-Jk a /Jk b but also anti-Fy a , -Fy b , -S and -s. Screening cells can be selected to reflect this, whereas the zygosity of donors is usually unknown and some will be heterozygous. Red cells for antibody screening are preserved in diluents shown to minimise loss of blood group antigens during storage. In addition, reagent red cells are easier to standardise than donor cells and there is potentially less opportunity for procedural error, particularly in automated systems.
Clinically significant antibodies are those that are capable of causing haemolytic transfusion reactions or haemolytic disease of the fetus and newborn (HDFN). With few exceptions, clinically significant antibodies are those that are reactive in the IAT at 37 °C; however, it is not possible to predict serologically which of these antibodies will definitely be of clinical significance, so the term ‘of potential clinical significance’ is often used.
Red cell reagents
The patient’s plasma should be tested against at least two individual screening cells, used individually, not pooled. The screening cells should be group O and encompass the common antigens of the population.
In the UK, the following antigens should be expressed as a minimum: C, c, D, E, e, K, k, Fy a , Fy b , Jk a , Jk b , S, s, M, N, P 1 , Le a and Le b ; one cell should be R 2 R 2 and another R 1 R 1 or R 1 w R 1 . The following phenotypes should also be represented in the screening set: Jk(a + b −), Jk(a − b +), S + s −, S − s +, Fy(a + b −) and Fy(a − b +) ( Table 22-3 ). These recommendations for homozygosity are based on UK data regarding the incidence of delayed haemolytic transfusion reactions, the need for high sensitivity in the detection of Kidd antibodies and the poorer performance of column agglutination techniques in the detection of some examples of Kidd antibodies using heterozygous cells. , The requirement for the expression of C w and Kp a antigens on screening cells has been the cause of much debate, but in the UK and the USA detection of anti-C w or anti-Kp a is not a requirement even in the absence of an antiglobulin crossmatch. , This is because these are low-frequency antigens and the antibodies rarely cause delayed haemolytic transfusion reactions or severe HDFN.
| Blood Group System | Antigen | Homozygous Cells Recommended |
|---|---|---|
| Rh | C | Yes (R 1 R 1 or R 1 w R 1 ) |
| c | Yes (R 2 R 2 ) | |
| D | Yes (R 1 R 1 and R 2 R 2 ) | |
| E | Yes (R 2 R 2 ) | |
| e | Yes (R 1 R 1 or R 1 w R 1 ) | |
| Kell | K | No * |
| k | No | |
| Duffy | Fy a | Yes |
| Fy b | Yes | |
| Kidd | Jk a | Yes |
| Jk b | Yes | |
| MNSs | M | No |
| N | No | |
| S | Yes | |
| s | Yes | |
| Lewis | Le a | No |
| Le b | No | |
| P | P1 | No |
* Although desirable, KK cells are unlikely to be available.
Methods
Antibody screening should always be carried out by an IAT as the primary method. Additional methods (e.g. two-stage enzyme or Polybrene) may also be used but are inferior for the detection of some clinically significant antibodies and should not be used alone. A large retrospective study showed that the vast majority of antibodies reactive only by enzyme technique are of no clinical significance. In Issitt’s study of 10 000 recently transfused patients, only one anti-c, initially unreactive by IAT, caused a delayed haemolytic transfusion reaction. There has been one SHOT report (1998–1999) of an enzyme-only anti-E that became detectable by IAT 7 days following the transfusion, causing a delayed haemolytic transfusion reaction and subsequent death of the patient due to renal failure.
For liquid-phase techniques, BCSH guidelines recommend the use of red cells suspended in low ionic strength saline (LISS), rather than in standard normal ionic strength saline (NISS), because LISS increases the speed and sensitivity of detection of many potentially clinically significant antibodies (see Chapter 21 ). There are conflicting reports about whether sensitivity can also be improved by adding PEG.
Indirect antiglobulin techniques
Column agglutination
In many countries, including the UK, column agglutination is now more commonly used than traditional tube or liquid-phase microplate techniques, because it has been shown to be at least as sensitive as a standard LISS spin-tube technique, , it is simpler to perform because it requires no washing phase, it uses small volumes of plasma and reagents, it has a more objective reading phase and it is easy to automate. The antihuman globulin (AHG) incorporated in the matrix is available as either a polyspecific or anti-IgG reagent. Red cell concentrations and volumes can be critical and it is important to follow manufacturers’ instructions at all times.
Column agglutination crossmatching tests have been shown to be less sensitive than standard tube techniques in the detection of weak ABO antibodies such as anti-A with A 2 B cells and Kidd antibodies with heterozygous red cells. It has been suggested that these failures may be the result of shear forces occurring during centrifugation, which cause weak agglutinates to be disrupted, especially when the antigen density is low.
Solid-phase systems
Solid-phase techniques (e.g. Immucor Capture-R and Bio-Rad Solidscreen II) are also becoming more popular because they have been shown to have a high level of sensitivity, and they also lend themselves to full automation. In 2014, 11% of UK laboratories were routinely using solid phase for antibody screening.
Liquid-phase techniques – tubes and microplates
Tube techniques are still used for antibody screening in some parts of the world. With LISS-suspension techniques it is important to maintain a high serum:cell ratio, without affecting the ionic strength. Equal volumes of serum and 1.5–2% cells suspended in LISS will result in a serum:cell ratio of > 60:1, ensuring optimal sensitivity. Reagents should be incubated for 15–20 min at 37 °C, and the cells then should be washed in PBS. After AHG is added, the red cells should be examined using a careful ‘tip and roll’ procedure to prevent disruption of weak agglutinates. Reading aids such a light box or concave mirror may also be used with this technique.
Liquid-phase microplate technology has never achieved a huge popularity for antibody screening because it is relatively difficult to introduce and standardise, and it cannot be automated. Because it is becoming increasingly difficult to obtain AHG reagents standardised for use in microplates, no method is detailed here.
Controls for antibody screening
A weak anti-D should be used on a regular basis to ensure the efficacy of the whole procedure, although the exact frequency will depend on work patterns as described in the blood grouping section. Additional weak controls are also recommended to confirm the sensitivity of the procedure and the integrity of the red cell antigens throughout their shelf life; anti-Fy a and/or anti-S are good examples because Fy and S antigens are protease labile and may deteriorate more quickly on reagent cells than the D antigen, and their use will also ensure that enzyme-treated cells have not been used by mistake. Consideration should also be given to selecting controls that demonstrate that the correct screening cell has been added to the batch of tests. Anti-S can be used as a control following the use of bleach to clean automated blood grouping analysers to check no cleaning fluid remains; the S antigen is very sensitive to Clorox bleach ( www.clorox.com ).
The use of red cells weakly sensitised with anti-D is essential to control the washing phase of every negative liquid-phase test because inadequate washing may result in complete or partial neutralisation of AHG by unbound globulin. Any test that does not give a positive reaction at the expected strength following addition of these cells (and subsequent centrifugation) indicates insufficient free anti-IgG and should be repeated. The washing phase of solid-phase systems is difficult to control and it may be necessary to add a weak control to every column to ensure that every probe has dispensed wash solution during each wash cycle.
Antibody identification
When an antibody is detected in the antibody screen, its specificity should be determined, and its likely clinical significance should be assessed before blood is selected for transfusion or relevant advice is given during pregnancy. It is essential to use a systematic approach to antibody identification to ensure that all specificities of potential clinical significance are identified. It may be tempting to match a reaction pattern immediately and look no further, but this is likely to result in additional specificities being missed.
Principles
As a starting point, the test plasma should be tested against an identification panel of reagent red cells by the technique with which it was detected in the screen. The next section on reagents outlines the minimum requirements for the panel. Inclusion of an autoantibody test is helpful in distinguishing between an autoantibody, an antibody directed against a high-frequency antigen and a complex mixture of alloantibodies. The positive and negative reactions should be compared with the panel profile in conjunction with the screening results.
Each antibody specificity should be considered in turn, and its presence should be systematically excluded by identifying antigen-positive cells that have given negative reactions. Wherever possible a negative reaction should be obtained with a red cell with homozygous expression of the relevant antigen. For example, if a negative reaction has been recorded against a Jk(a + b −) cell, then the presence of anti-Jk a can be excluded, but if the only negative reactions are against Jk(a + b +) cells, then anti-Jk a cannot immediately be safely excluded. This will leave a list of potential specificities that should be considered by matching the positive reactions to the antigen-positive cells to determine if any are definitely present. Once this process is complete with the initial screen and identification panel, further cells and techniques may need to be used to complete the exclusion process. For example, where anti-S has been identified as being present, an enzyme-treated panel may be required to exclude the presence of anti-E, if all of the E-positive cells were also S positive, or a K + S − cell may need to be selected to exclude the presence of anti-K. The more specificities present, the more complicated the process, and where resources are limited, samples may need to be sent to a reference centre to elucidate all specificities. If the reagents are available, phenotyping the patient’s red cells early on in the process will allow exclusion of specificities for which the patient is antigen positive.
The specificity of an antibody should only be assigned when it is reactive with at least two examples of reagent red cells carrying the antigen and nonreactive with at least two examples of reagent red cells lacking the antigen. This is because a single positive reaction could occur if the panel cell unexpectedly expressed a low-frequency antigen and a single negative reaction could occur if the panel cell lacked a high-frequency antigen.
Phenotyping
When an antibody has been identified, the patient’s own red cells should be phenotyped for the relevant antigen. If the patient’s red cells are negative for the antigen, this confirms that the patient is capable of making an antibody of that particular specificity. If the patient’s red cells are positive for the antigen this suggests one of the following:
- 1.
The antibody is an autoantibody, in which case the direct antiglobulin test (DAT) should be positive.
- 2.
The patient has been transfused recently and the reagent is detecting transfused cells rather than the patient’s own cells. Care should be taken to look for a mixed-field reaction. Evidence of a delayed transfusion reaction should be sought.
- 3.
The initial antibody identification result is incorrect.
- 4.
The patient’s red cells are Ig-coated with a positive DAT. Care should be taken, particularly when using reagents potentiated with PEG, to recognise this to prevent reporting a false-positive result.
Extended phenotyping can be helpful where a mixture of antibodies is present because it allows the exclusion of antibodies specific for antigens for which the patient is positive, reducing the number of additional reagent cells required.
Additional panels/techniques
The chances of identifying antibodies when two specificities are present are significantly improved by using a two-stage enzyme technique, if at least one of the relevant antigens is affected by enzymes. For example, Rh antibodies are enhanced by proteolytic enzymes in routine use, whereas M, N, S, Fy a and Fy b antigens are destroyed. Similarly, two different panels of reagent cells provide an increased chance of excluding further specificities where a mixture of two antibodies has been identified.
Direct agglutination at room temperature or 4 °C may be helpful to distinguish between an antibody of potential clinical significance and a cold reacting antibody; again this is particularly useful where a mixture of antibodies is present. Weak examples of Kidd antibodies are often enhanced by the use of an IAT using enzyme-treated cells, and this can be particularly helpful where the antibody is only reacting against homozygous cells by the IAT.
Reagents
An identification panel should consist of red cells from at least eight group O donors, although 10 is more common in commercial panels and allows easier elucidation of antibody mixtures. To be functional, the panel must permit confident identification of the most commonly encountered, clinically significant antibodies. The UK guidelines can be summarised as follows:
- 1.
For each of the commonly encountered clinically significant red cell antibodies, there should be at least two examples of phenotypes lacking, and at least two examples of phenotypes expressing, the corresponding antigen.
- 2.
There should be at least one example of each of the phenotypes R 1 R 1 and R 1 w R 1 . Between them, these two samples should express the antigens K, k, Fy a , Fy b , Jk a , Jk b , M, N, S and s.
- 3.
There should be at least one example of each of the phenotypes R 2 R 2 , r′r and r″r and at least two examples of the phenotype rr.
- 4.
The following phenotypes should be expressed in those samples lacking both D and C antigens: K +, K −, Jk(a + b −), Jk(a − b +), S + s −, S − s +, Fy(a + b −) and Fy(a − b +). The panel should be able to resolve as many likely antibody mixtures as possible.
Antibody cards
Delayed haemolytic transfusion reactions can occur when antibodies have not been detected in the current antibody screen or have been incorrectly identified. It has been suggested that antibody cards, produced either by the hospital or the reference centre, be carried by the patient for presentation on admission to hospital. To be effective, such cards have to be accompanied by patient information leaflets, explaining the significance of the antibodies and preferably handed personally to the patient by someone with a clear understanding of blood transfusion practice. There are potential pitfalls with this suggestion, not least that the level of proficiency in identifying antibodies and appreciating their clinical significance varies between establishments. A better long-term approach may be to have a national database of patients who have been identified as having clinically significant antibodies.
Selection and transfusion of red cells
Once the blood group of a patient has been established and any antibodies have been identified, a set of procedures is required to select units of red cells that are appropriate for transfusion. These include selecting ABO/D-compatible units, which will also need to be negative for antigens to which the recipient has clinically significant alloantibodies ( Table 22-4 ). It is also important that consideration is given to certain clinical criteria dictating specific requirements (e.g. the requirement for irradiated or washed red cells). Selection according to these criteria depends on good clinical information, accurate ABO and D typing and a sensitive antibody screen.
| System | Antibody | Recommendation |
|---|---|---|
| ABO | Anti-A 1 | IAT crossmatch compatible at 37 °C |
| Rh | Anti-D, -C, -c, -E, -e | Antigen negative * |
| Rh | Anti-C w | IAT crossmatch compatible † |
| Kell | Anti-K, -k | Antigen negative * |
| Kell | Anti-Kp a | IAT crossmatch compatible † |
| Kidd | Anti-Jk a , -Jk b | Antigen negative * |
| MNS | Anti-M (active at 37 °C) | Antigen negative * |
| MNS | Anti-M (not active at 37 °C) | IAT crossmatch compatible at 37 °C |
| MNS | Anti-N | IAT crossmatch compatible at 37 °C |
| MNS | Anti-S, -s, -U | Antigen negative * |
| Duffy | Anti-Fy a , -Fy b | Antigen negative * |
| P | Anti-P 1 | IAT crossmatch compatible at 37 °C |
| Lewis | Anti-Le a , -Le b , Le a + b | IAT crossmatch compatible at 37 °C |
| Lutheran | Anti-Lu a | IAT crossmatch compatible at 37 °C |
| Diego | Anti-Wr a (anti-Di3) | IAT crossmatch compatible † |
| H | Anti-HI (in A 1 and A 1 B patients) | IAT crossmatch compatible at 37 °C |
| All | Other active by IAT at 37 °C | Seek advice from blood centre |
* Antigen negative and crossmatch compatible.
† These recommendations apply when the antibody is present as a sole specificity. If present in combination, antigen-negative blood may be provided by the blood centre to prevent wastage of phenotyped units.
Some patients are identified as definitely needing transfusion of blood, but others may be undergoing surgery where blood is crossmatched to ‘stand by’. Audits have shown that blood is often crossmatched but not transfused. The transfusion ratio, or crossmatch index, can be used to assess how well blood stocks are managed. One option is to perform a blood group and antibody screen on a patient and then save the sample, only crossmatching blood if certain pre-agreed transfusion triggers are met. Local policy should define a maximum surgical blood ordering schedule, indicating which surgical procedures can be ‘group and screen/group and save’ and how many units of blood need to be crossmatched for procedures with a high likelihood of intraoperative transfusion. The decision as to whether blood is crossmatched in advance may relate to local factors, including the proximity of the blood transfusion laboratory to the operating theatre (or other location where blood is to be transfused) and the time it takes to provide compatible blood following a request.
Once the appropriate red cells have been selected, compatibility needs to be ensured. This is usually referred to as crossmatching, which may include an IAT to check for incompatibility as a result of IgG antibodies and ABO antibodies or an immediate spin test to check for ABO incompatibility only. Instead of a serological test, an assessment of ABO compatibility may be based on a ‘computer check’, usually referred to as ‘electronic issue’. Some transfusion laboratories, where surgery takes place in a different hospital, have extended electronic issue to the selection of compatible units, as dictated by the transfusion laboratory, from a remote issue refrigerator.
The purpose of crossmatching blood is to prevent the transfusion of incompatible red cells and a subsequent haemolytic transfusion reaction. The different types of crossmatch are outlined in the following paragraphs. Whichever crossmatch technique is chosen, it should be clear that all patients with known red cell antibodies of potential clinical significance, even if currently undetectable, should have an indirect antiglobulin crossmatch and are not suitable for electronic issue. ,
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree