Acute Kidney Injury Incidence and Mortality Associated With SARS-CoV-2 Infection
AKI incidence has varied based on the geographic location and clinical situation during the pandemic. A meta-analysis of over 13,000 patients reported an AKI prevalence of 17%, although the range from the individual studies that made up the meta-analysis was broad at 0.5% to 80%. Critically ill patients are more likely to have AKI in the setting of COVID-19; they are also more likely to have stage 3 AKI and require renal replacement therapy (RRT). Patients with COVID-19 appear to have a higher risk for AKI compared with other patients admitted to the hospital, and it is independent of severity of illness. AKI is more common in patients with COVID-19 than in patients with influenza. When compared with other members of the Coronaviridae family, AKI incidence appears to be the highest in patients with Middle East respiratory syndrome (MERS) but is similar between patients with COVID-19 and severe acute respiratory syndrome (SARS).
Multiple studies have demonstrated that the COVID-19–associated AKI occurs soon after hospitalization and occurs temporally close to when respiratory failure occurs. , Risk factors identified for development of AKI include older age, male sex, history of diabetes mellitus, history of hypertension, presence of shock, and need for invasive ventilation. , Patients with worse inflammatory markers are also at higher risk for development of AKI.
Mortality is high in AKI in the setting of COVID-19. AKI in the setting of COVID-19 appears to be associated with more mortality than patients with AKI from other viral pneumonias, AKI from all-comers in a historical cohort, and AKI occurring during the pandemic in patients without COVID-19. A meta-analysis found that mortality in patients with AKI and COVID-19 was 52% compared with 11% for all-comers with COVID-19. Patients with severe AKI requiring RRT have the highest mortality of patients with AKI. In addition, the more organ failures a critically ill patient with COVID-19–associated AKI has, the higher is the mortality. Mortality of AKI associated with COVID-19, MERS, and SARS is similar on the basis of two meta-analyses. ,
The need for RRT is higher in patients with COVID-19–associated AKI compared with other causes of AKI. The need for RRT has varied based on geographic region studied and the patient cohort. The more severely ill patients are as evidenced by being hospitalized in the critical care unit (CCU), the more likely they are to need RRT. Overall, approximately 5% of patients with COVID-19 need RRT whereas approximately 30% of patients admitted to CCUs with COVID-19 will need RRT. ,
From the available data to date, there has been a suggestion that the incidence of AKI has decreased as the pandemic has progressed. , It is unknown why this has happened. This may reflect the evolution of improving clinical understanding and care over the course of the pandemic and the increasing availability of medications that can be used to treat COVID-19. It also may reflect that patients evaluated later in these studies had less hypoxia and fewer inflammatory markers that were less elevated.
In patients who survive COVID-19–associated AKI, persistent kidney function abnormalities often persist. In patients who require RRT, approximately 50% to 60% do not survive and 5% to 10% continue to need RRT at discharge from the hospital. , , In one study, approximately two-thirds of patients with AKI during their COVID-19 hospitalization had recovered kidney function back to their baseline by posthospitalization follow-up. However, in long-term follow-up, patients with COVID-19–associated AKI had more loss of glomerular filtration rate (GFR) after recovery than patients with AKI from other causes.
Although at the time of publication, data are still being gathered and interpreted, it seems clear that AKI in the setting of COVID-19 occurs more frequently with other illnesses and is associated with a higher mortality. As the pandemic rages on, we may be getting better at treating COVID-19 and preventing the onset of AKI. It will be important for patients who survive COVID-19–associated AKI to continue to have their kidney function monitored after hospital discharge because of long-term risks for persistent kidney dysfunction.
The causes of AKI in COVID-19 are discussed in the following section and summarized in Table 10.1 .
| Kidney Injury | Clinical Findings and Features | Proposed Mechanism of Injury | Occurrence |
|---|---|---|---|
| a Patients can have multiple types of renal injury at the same time | |||
| Glomerular | |||
| COVID-associated nephropathy (COVAN): Secondary collapsing FSGS |
| COVID-19 infection serves as a “second hit” in individuals predisposed to glomerular injury as a result of high-risk APOL1 allele variants | Overall uncommon but most reported glomerular disease in COVID-19 |
| Anti-GBM disease |
| COVID-19 infection promotes immune response to glomerular basement membrane (noncollagenous domain of α3-chain of collagen type IV) | Rare |
| ANCA vasculitis |
| Not yet well described. COVID-19 could be “second hit” in predisposed individuals | Rare |
| IgA vasculitis |
| Not yet well described. COVID-19 could be second hit in predisposed individuals, resulting in increase in circulating galactose-deficient IgA1 antibodies, production of antibodies and formation of immune complexes | Rare |
| Membranous nephropathy |
| Not yet well described. COVID-19 could be second hit in predisposed individuals. Respiratory infection could illicit an anti-PLA2R autoimmune response | Rare |
| Tubular | |||
| Acute tubular injury |
| Ischemic injury resulting from decreased kidney perfusion secondary to hemodynamic instability and/or volume depletion secondary to severe infection | Most common |
| Rhabdomyolysis (myoglobin cast nephropathy) |
| Induced by viral infection, drug-induced, or the result of electrolyte abnormalities | Rare reports in literature. Can be a cause of acute tubular injury |
| Vascular | |||
| Thrombotic microangiopathy |
|
| Rare |
Could Viral Tropism in Kidney Parenchyma Be Responsible for Acute Kidney Injury?
Evidence is mixed for viral tropism of SARS-CoV-2 in kidney parenchyma. Early autopsy studies suggest viral tropism with evidence of coronavirus-like particles in the cytoplasm of kidney proximal tubular epithelial cells and in the podocytes by electron microscopy and either immunofluorescent staining with an antibody targeting SARS-CoV-2 nucleoprotein or with in situ hybridization. ,
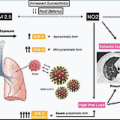
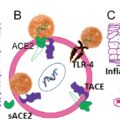
There is a pathophysiological basis for possible tropism. The angiotensin-converting enzyme-2 (ACE2) receptor is the main cellular entry point for SARs-CoV-2 and is expressed on the brush border of proximal tubular cells and podocytes.
Subsequent studies have not shown viral inclusions at the light microscopic level or viral particles at the ultrastructural level. This may be in part due to timing of biopsy, with some studies delaying kidney biopsy because detectable SARS-CoV-2 may wane with time. Other studies did not report timing between positive viral polymerase chain reaction (PCR) and kidney biopsy. One study suggested lower levels of SARS-CoV-2 organotropism outside of the lungs so viral titers and severity of illness may play a role in detection.
Tubular Injury in COVID-19
Small autopsy, biopsy series, and case reports show that acute tubular injury (ATI) is the most common histopathological finding with patients who develop AKI during their COVID-19 illness. These studies have included a variety of patients across clinical contexts from severe COVID-19 that ultimately led to the patient’s death to nonhospitalized patients presenting with abnormal kidney function and proteinuria and or hematuria. , By light microscopy, varying degrees of tubular injury have been reported with descriptions of diffuse loss of brush border, nonisometric vacuolar degeneration, frank epithelial necrosis, and cellular debris within the tubular lumens.
The largest study, an autopsy study of 42 postmortem kidneys, showed that ATI was the main pathological finding correlating with patients with AKI. This study found that the degree of ATI was mild compared with the elevation in serum creatinine. A multicenter trial of 14 native kidney biopsies and 3 transplant kidney biopsies in patients who presented with confirmed SARS-CoV-2 infection, AKI, and proteinuria/hematuria, found the most common histological finding was ATI in (14/17, 82%). Of note, most patients in this cohort had mild COVID-19 symptoms. Only three patients had severe COVID-19, and most biopsies were performed after the individuals had negative status by reverse transcription (RT)-PCR. Another single-center native kidney biopsy series of 10 hospitalized patients with AKI and COVID-19 found that all biopsy samples showed varying degrees of ATI. One patient in this series had myoglobin casts, serum creatine kinase levels greater than 92,000 and evidence of ATI, suggesting rhabdomyolysis contributing to AKI and ATI.
It is likely that insults that drive ATI and AKI in patients with severe COVID-19 are multifactorial. Patients with COVID-19 often present with acute hypoxia but also may present with nausea, vomiting, and diarrhea. These hemodynamic alterations are likely drivers of prerenal or ischemic injury. In severe COVID-19 illness, the SARS-CoV-2 virus can induce a cytokine storm leading to massive release of granulocyte colony-stimulating factor, interleukins, and interferon and lead to overt septic shock. , These patients often require pressor support and are exposed to one or more nephrotoxic medications. In these cases, hemodynamic alterations, cytokine injury, or drug effects can directly or indirectly injure the kidney. As discussed earlier and reported in other series, rhabdomyolysis with pigmented casts can also contribute to ATI and AKI. ,
In short, ATI is the most common cause of AKI in the setting of COVID-19. It is likely multifactorial from both ischemic and toxic injury. It may be seen even in the setting of mild COVID-19. Similarly, ATI is also the most common cause of AKI seen in past influenza pandemics.
Glomerular Disease and COVID-19
Although the more common kidney injury found in patients with COVID-19 is ATI, patients also can present with proteinuria and/or microscopic hematuria. In the early phases of the pandemic, a retrospective cohort study from China of 333 patients admitted with COVID-19 pneumonia detected hematuria in 41.7% and proteinuria in 65.8%. Although low-level proteinuria can be due to tubular injury, histopathological analysis of kidney tissue has revealed different patterns of glomerular injury in patients infected with SARS-CoV-2.
COVID-19–Associated Nephropathy
The predominate glomerular lesion described in the literature is collapsing glomerulopathy associated with COVID-19 infection, commonly referred to as COVID-associated nephropathy (COVAN). Multiple case reports and small case series describe patients with collapsing focal segmental glomerulosclerosis (FSGS) lesions. , , FSGS is a glomerular disorder defined as glomerular scarring in a focal (involving <50% of glomeruli) and segmental (affecting <50% of each glomerulus) pattern. One of the histological patterns of FSGS is a collapsing variant with features of glomerular-tuft collapse associated with hypertrophy and hyperplasia of the overlying visceral epithelial cells that can form pseudocrescents, as well as severe tubular injury, tubular microcysts, and severe foot process effacement. Clinically, patients often present with nephrotic syndrome, which consists of significant proteinuria (≥3.5 g/day), hypoalbuminemia (<3.5 g/dL), hypercholesterolemia, and peripheral edema. The patients selected for biopsy that showed COVAN all had AKI and/or nephrotic-range proteinuria or nephrotic syndrome.
The vast majority of patients diagnosed with COVAN are of African ancestry, with a few exceptions, including reports of COVAN in a Hispanic patient and a patient of Asian heritage. Patients of African ancestry are at risk for another viral-induced collapsing glomerulopathy, human immunodeficiency virus (HIV)-associated nephropathy, if they are homozygous for apolipoprotein L1 (APOL1) high-risk allele variants (G1 and G2). In our review of the current literature, 100% (N = 28) of patients diagnosed with COVAN who underwent genetic analysis had high-risk APOL1 genotypes (G1/G1, G1/G2, or G2/G2). a
a References , , , , , , .
This includes the case of a Hispanic patient with collapsing glomerulopathy. The high-risk APOL1 genotype can also predispose patients infected with COVID-19 to develop other podocytopathies such as minimal change disease.Reports of Other Glomerulonephritis
A variety of other glomerular lesions in patients infected with COVID-19 have been reported in the current literature. There are reports of de novo or recurrent anti–glomerular basement membrane (anti-GBM) disease, , with an additional case of de novo anti-GBM disease diagnosed by positive serum testing for anti-GBM in a patient with pulmonary-renal syndrome without a confirmatory kidney biopsy. There also have been cases of pauci-immune glomerulonephritis, membranous nephropathy, and Ig-A vasculitis. , It is unclear if these lesions are directly the result of SARS-CoV-2 infections or if the viral infection acts as a “second hit” in susceptible individuals provoking the different patterns of kidney injury. It has been hypothesized that infection or inflammation resulting in endothelial cell injury could unmask antigens, such as the noncollagenous domain of the alpha-3 chain of type IV collagen or phospholipase A2 receptor, resulting in an autoimmune response. , In one report of eight cases of anti-GBM over a 5-month period during the pandemic, the five patients tested for SARS-CoV-2 infection by viral RNA testing were all negative. However, four of the eight patients had immunoglobulin M (IgM) and/or IgG antibodies to the spike protein suggestive of recent infection. In a case of IgA vasculitis, the nephritic syndrome developed a total of 5 weeks after the patient’s COVID-19 diagnosis. These delayed presentations suggest an inflammatory reaction secondary to SARS-CoV-2 that then triggers endothelial cell and subsequent glomerular injury.
Thrombotic Microangiopathy
Thrombotic microangiopathy (TMA) has been reported in kidney biopsies from COVID-19 patients as either the primary lesion or in addition to other histological findings. , , , In six of eight described cases, patients had laboratory findings concerning for TMA, including AKI, thrombocytopenia, and hemolytic anemia. , The mechanism of injury is not definitively the result of SARS-CoV-2, because patients often were exposed to other reported causes of TMA, including malignant hypertension, cocaine use, and medications (gemcitabine, hydroxychloroquine, or calcineurin inhibitors). , , ,
Findings in the literature that suggest COVID-19 infection results in complement dysregulation, which can lead to a TMA pattern of kidney injury. , , , Complement dysregulation results in formation of the membrane attack complex, resulting in endothelial cell damage. One case report indicated alternative complement pathway activation resulting from low serum C3 levels and normal C4 levels, whereas another case report detected a complement defect based on findings of low factor H complement antigen and elevated plasma CBb and SC5b-9 levels. In a study of pediatric patients with SARS-CoV-2 infection, soluble C5b9 (sC5b9) was measured as a biomarker of complement dysregulation and TMA. They demonstrated elevated levels of sC5b9 in patients with either mild or severe COVID-19 disease or multisystem inflammatory syndrome in children (MIS-C) compared with healthy controls. In addition, they found an association with elevated plasma sC5b9 levels in patients with AKI and with clinical criteria for TMA. These findings support a complement-mediated mechanism of injury rather than TMA secondary to sepsis-induced coagulopathy.
Proposed Mechanisms
Whether there is direct viral infection of glomerular epithelial cells has been debated. There were early reports of detection of SARS-CoV-2 RNA by immunohistochemistry and virion particles seen on electron microscopy of kidney biopsies and in autopsy studies. , , , However, subsequent case reports and case series using staining for SARS-CoV-2 RNA, spike protein, and nucleocapsid protein on immunohistochemistry in addition to electron microscopy have failed to consistently detect the presence of SARS-COV-2. , , Despite the possible mechanism of cell entry by binding to ACE2 and transmembrane protease serine 2 receptors located on podocytes, there currently is no definitive evidence confirming any direct viral infection of the kidney.
Rather than acting directly on the kidney parenchyma, the viral infection also could be acting as a second hit in individuals susceptible to glomerular injury. As alluded to earlier, there is a clearer understanding of the pathological processes behind APOL1 high-risk alleles and podocytopathies. Research studies have shown that interferon is a regulator of APOL1 levels in both low- and high-risk human podocytes. Upregulation of APOL1 high-risk variants can result in disruption of autophagy and mitochondrial hemostasis, ultimately resulting in glomerular epithelial cell death. Elevated interferon levels in COVID-19 patients have been inferred from the visualization of glomerular endothelial tubulorecticular inclusions by electron microscopy. , This finding is not limited to patients with COVAN. One case series of 17 patients visualized tubuloreticular inclusions in 6 of 10 cases that had glomeruli available for electron microscopy, including cases of ATI, membranous glomerulopathy, and minimal change disease. In patients without high-risk APOL1 genotype, glomerular injury is also likely driven by endothelial cell dysfunction and cytokine storm induced by viral infection. ,
Management of COVID-19 Acute Kidney Injury
As we have discussed, the pathogenesis of AKI in patients with COVID-19 is multifactorial. There is no specific evidence that COVID-19 should be managed differently from other causes of AKI. Therefore, in all patients at high risk for AKI, using the standard of care to prevent and manage multiorgan failure is recommended. ,
Close monitoring of hemodynamics, serum markers of kidney function, individualized fluid management, and decreasing exposure to nephrotoxic drugs are important strategies to decrease risk for kidney injury.
Hypovolemia is common in the early COVID-19 infection course of hospitalized patients likely due to sepsis related to COVID-19 infection. Using balanced crystalloids over normal saline as initial management to expand intravascular volume has been shown to decrease rates of persistent kidney dysfunction and need for RRT in critically ill patients and in sepsis.
In patients who develop AKI, further considerations in AKI management include medical management of fluid and electrolyte strategies. To avoid hypervolemia, consideration of fluid restriction to 10 mL/kg per day and use of high-dose diuretics. To decrease the risk for hyperkalemia, restriction of oral potassium intake, and using potassium binders can be started early in the AKI course. Metabolic acidosis can be managed with oral or intravenous bicarbonate solutions. In the event of AKI progression, close attention to drug dosing and altered pharmacokinetics is important to avoid drug toxicity.
In the event conservative management fails, indications for RRT are the same for patients with AKI and COVID-19 as in AKI events not related to COVID-19. These include oliguria with refractory hypervolemia, hyperkalemia, severe acidosis, or azotemia.
Medication Treatment
At the time of publication, there is no strong evidence that any medication used to treat COVID-19 decreases the likelihood of development of AKI or attenuates the severity, although data analysis remains ongoing, so this may change with time. However, it is important to discuss what treatments have been studied in patients with kidney failure of any type and if there are important dose modifications based on GFR.
Antivirals: Remdesivir
As we have previously discussed, there is some evidence that SARS-CoV-2 has direct viral tropism to tubular cells and podocytes by ACE2 receptors. 19 So treatment with antivirals could theoretically be a treatment to ameliorate COVID-19–induced AKI.
Remdesivir is a nucleotide analog that inhibits viral RNA-dependent RNA polymerase. The ACCT-1 trial showed that remdesivir decreased recovery time for hospitalized patients. In that trial, the reported cases of decreased kidney function or AKI were slightly less in the remdesivir-treated group (85/532 [15.9%], 105/516 [20.3%]).
Notably, most trials excluded patients with severe AKI or end-stage kidney disease (ESKD) based on GFR cutoffs (either 50 or 30 mL/min/1.73 m 2 ). Additionally, remdesivir has limited water solubility, and the intravenous formulation requires a carrier of sulfobutylether-beta-cyclodextrin (SBECD). This carrier is also excreted by the kidneys and has been associated with nephrotoxicity.
Some small trials have evaluated the safety of remdesivir in patients with GFR cutoffs below initial trials and do suggest that there is no overt toxicity in patients with reduced GFR or in patients already on dialysis. As mentioned earlier, evidence that antivirals reduce kidney-related events is only limited or indirect.
Immunomodulatory Agents: Tocilizumab and Baricitinib
Severe SARS-CoV-2 infection is thought to be secondary to proinflammatory state with increased interleukin-1 (IL-1), IL-6, tumor necrosis factor, and other cytokines. Immunomodulatory agents can decrease cytokine production or block cytokine receptor activation, thereby decreasing the overall inflammatory response.
Tocilizumab is a humanized IgG1 monoclonal antibody that is directed against the IL-6 receptor. IL-6 is thought to be an important cytokine in COVID-19–related immune dysregulation and development of severe COVID-19 and acute respiratory distress syndrome (ARDS). Data are currently conflicting on the impact of tocilizumab in severe COVID-19 illness. , Kidney injury occurred at similar rates in the groups. Because tocilizumab is a monoclonal antibody, dose adjustment is not needed for decreased GFR.
Baricitinib is an oral selective inhibitor of Janus kinase (JAK) 1 and 2 and inhibits intracellular cytokine signaling, thereby mitigating the immune response and presumed therapeutic target for the hyperinflammatory state of severe COVID-19.
A follow-up to the ACCT-1 trial investigated treatment with a combination of baricitinib and remdesivir over remdesivir alone for the treatment of hospitalized patients with COVID-19 pneumonia. Baricitinib plus remdesivir was superior to remdesivir alone in reducing recovery time and accelerating improvement, particularly in patients receiving high-flow oxygen or noninvasive mechanical ventilation. Safety analysis showed that kidney events occurred at a similar rate in both groups in this trial.
Data are limited for baricitinib in patients with severe kidney impairment. Baricitinib is not recommended for patients who are on dialysis, have ESKD, or have AKI.
Corticosteroids
Low-dose dexamethasone was found to reduce mortality in hospitalized patients with severe or critical COVID-19 requiring supplemental oxygen or mechanical ventilation. A secondary outcome in this study was the new requirement for RRT. In this study, there were fewer patients receiving RRT at 28 days in the dexamethasone group than in the usual care group (relative risk [RR] 0.61; 95% confidence interval [CI], 0.48–0.76).
Dexamethasone is primarily metabolized hepatically, and there are no dose adjustments required in patients with kidney failure receiving dialysis.
Niacinamide
Niacinamide is the base form of vitamin B 3 and has been suggested to increase nicotinamide adenine dinucleotide (NAD+) level safely. NAD+ shortage has been proposed as a mechanism for acute tubular necrosis; thus increasing NAD+ availability theoretically could help prevent cell damage and ATN. , In a small prospective study, niacinamide use was associated with decreased frequency of RRT needs and mortality among stage 2/3 AKI, but no differences were seen in outcomes among patients with stage 1 AKI.
Monoclonal Antibodies
Bamlanivimab and etesevimab are neutralizing monoclonal antibodies that bind to spike proteins of the COVID-19 virus. The BLAZE trial showed reduction of SARS-CoV-2 viral load at day 11 among nonhospitalized patients with mild to moderate COVID-19 illness who were treated with bamlanivimab and etesevimab compared with placebo. , No dose adjustment is recommended in kidney failure. Notably, kidney failure (acute and chronic) was not an exclusion criterion for BLAZE trial participants. Currently, no data exist on whether monoclonal antibodies decrease the development of or attenuate the severity of AKI.
Renin-Angiotensin-Aldosterone System Inhibition
Normally in the body, when blood flow to the kidney is reduced, juxtaglomerular cells convert prorenin to renin. Renin then converts angiotensinogen to angiotensin-1. Angiotensin-1 is converted to angiotensin-2 by ACE. Angiotensin-2 then causes vasoconstriction resulting in increased blood pressure. The ACE2 receptor is a membrane-bound receptor that counteracts this effect by hydrolyzing angiotensin-2. ACE2, as discussed previously, is the entry point into cells by the SARS-CoV-2 virus. Acutely, angiotensin-2 decreases ACE2 receptor expression.
ACE inhibitors (ACEIs) block the conversion of angiotensin-1 to angiotensin-2, and angiotensin receptor blockers (ARBs) block the binding of angiotensin-2 to the angiotensin-1 receptor (AT1R). Experimental animal models have suggested that ACEIs and ARBs increase ACE2 expression in kidney and heart tissue. It was hypothesized early in the course of the pandemic that ACEIs and ARBs may be either beneficial or harmful in the setting of COVID-19 illness. The harm hypothesis comes from ACEIs and ARBs increasing ACE2 expression, leading to increased viral entry and injury. In the beneficial hypothesis, the decreasing of angiogenin-2 production with an ACEI or by blocking the AT1R with an ARB diminishes the inflammation and fibrosis caused by angiotensin-2.
At the time of publication, there are multiple ongoing randomized controlled trials (RCTs) investigating this area. Results have returned from the BRACE-CORONA trial, which randomized patients chronically on an ACEI or ARB hospitalized with mild to moderate COVID-19 to temporarily suspend or continue their medication. There was no difference in mortality between the two groups. Adverse events, including AKI requiring hemodialysis, were similar between the two groups. Data from large observational studies also have not supported an increased risk in patients taking ACEIs or ARBs. , Thus the recommendations from many professional societies are to continue ACEIs and ARBs unless clinically contraindicated.
Systemic Anticoagulation
SARS-CoV-2 is associated with a prothrombotic state, and thrombi in the kidney microvasculature may contribute to the risk for AKI and/or AKI progression. No data have shown decreased risk for AKI with systemic anticoagulation at this time. Systemic anticoagulation strategies in AKI requiring RRT are important for filter patency, especially in continuous RRT.
Renal Replacement Therapy
The timing of initiation of RRT can be a challenge among critically ill patients. A number of clinical trials and meta-analyses have evaluated initiation of RRT in the critically ill and have not shown a difference in mortality or kidney recovery in the absence of emergent indication. There is no current evidence to suggest a different strategy (i.e., earlier initiation) is more effective in management of COVID-19–related AKI.
We recommend conservative management of AKI and the initiation of dialysis to manage the life-threatening complications of AKI, including hyperkalemia, acidemia, and/or fluid volume overload.
Modality of RRT can be more complicated in the setting of the COVID-19 pandemic because of the volumes of patients in need and lack of dialysis resources (dialysate, dialyzer filters, anticoagulation medications), machines, and appropriately trained staff.
No study has evaluated outcomes of one modality over another in COVID-19, but there are practical concerns in the determination of modality. Selection should be based on patient needs, local expertise, and availability of staff and resources. The various modalities and their pros and cons are discussed in the following section and are summarized in Table 10.2 .