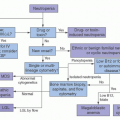
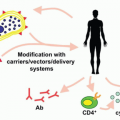
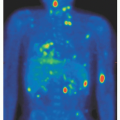
The hallmark of classical HL is Reed-Sternberg (RS) cell which most commonly derives from a neoplastic clone originating from B-lymphocytes in lymph node germinal centers, but is then embedded within a reactive infiltrate of lymphocytes, macrophages, granulocytes, and eosinophils.
27 The RS cell is a binucleated or multinucleated giant cell that is often characterized with a bilobed nucleus, with two large nucleoli, described commonly as an owl’s eye appearance.
28 Sequence analyses of RS cell clones reveal rearrangements of immunoglobulin variable-region genes resulting in deficient immunoglobulin production. RS cells then evade the apoptotic pathway, leading to the genesis of HL, and perhaps the paraneoplastic immune-mediated phenomena that sometimes accompany the disease.
4,
5 The B lymphoid cells from which RS arise have high levels of constitutive nuclear NF-
κB, a transcription factor known to mediate gene expression related to inflammatory and immune responses, and deregulation of NF-
κB has been postulated as a mechanism by which RS cells evade apoptosis.
6,
29 NF-
κB dimers are held in an inactive cytoplasmic complex with inhibitory proteins, the I
κBs.
29 B-cell stimulation by
diverse signals results in rapid activation of the I
κB kinase (IKK). The IKK complex phosphorylates two critical serine residues of I
κBs,
30,
31,
32 thereby targeting them for rapid ubiquitin-mediated proteasomal degradation. Active NF-
κB dimers are then released and translocated to the nucleus, where they activate gene transcription. Activation of NF-
κB appears to be a final common effect of co-stimulatory interactions, genetic aberrations, or viral proteins that operate in HL.
33RS cell survival is dependent on several downstream pathways. RS cells express CD40 and CD40 ligand (CD40L) is expressed on inflammatory T and dendritic cells that surround them. CD40/CD40L interactions normally provide a second signal from activated helper T-cells to normal B-cells, resulting in activation of NF-
κB. NF-
κB in turn causes proliferation and induces expression of BCL-xL, which protects B-cells from apoptosis.
34 Tumor necrosis factor receptor-associated factor 1 (TRAF 1) is overexpressed in EBV-transformed lymphoid cells and RS cells
35 and is associated with activation of NF-
κB and protection of lymphoid cells from antigen-induced apoptosis. Activation of NF-
κB, in turn, leads to expression of TRAF1, thereby establishing a positive feedback loop that maximizes NF-
κB-dependent gene expression.
36 EBV latent membrane protein 1 (LMP1) interacts with TRAF1, and tumors with TRAF1-LMP1 aggregates exhibit high NF-
κB activity.
37,
38 LMP1 activates NF-
κB by promoting I
κBa turnover.
39 RS cells express CD30 and CD30 ligation promotes proliferation of HL-derived cells with constitutive activation of NF-
κB.
40EBV genome fragments can be found in approximately 30% to 50% of HL specimens, and may play a role in the rescue and repair of RS cells, further aiding in their evasion of apoptosis and enhanced survival.
7,
41,
42,
43 Three latent viral antigens are expressed in EBV-positive HL in RS cells: Epstein-Barr nuclear antigen-1 (EBNA1), required for viral episome maintenance, LMP1 with transforming properties, and LMP2, which is nontransforming.
44,
45