Antibiotic Prophylaxis in Obstetrics and Gynecology
Since the 1970s, a large body of data has accumulated to allow for the establishment of practical recommendations for use in many procedures. Quality standards have been published for antimicrobial prophylaxis in all surgical procedures. Because antibiotic prophylaxis has become so well-established for many procedures, we will not provide detailed and cumbersome tables but rather will provide practice recommendations.
There are special conditions regarding the use of antibiotic prophylaxis in an obstetric-gynecologic population. First, nearly all obstetric and most gynecologic patients are healthy and free of serious underlying disorders. Second, because the lower genital tract is a contaminated field, operation through or adjacent to this field leads to a moderate to high incidence of infection (in the absence of antibiotic prophylaxis), but serious infection measured by abscess or death is unusual. Third, use of certain antimicrobials for prophylaxis in pregnancy is often contraindicated because of the potential for adverse effects on the fetus, newborn, or mother. In this chapter, antibiotic prophylaxis is defined as the use of antibiotics for the prevention of infection in the absence of current signs or symptoms of infection. Characteristics of an ideal antibiotic used for prophylaxis include: high safety, good pharmacokinetics, good activity against most of organisms likely to cause an infection, and antibiotic is not commonly used to treat an established infection.
USES IN OBSTETRICS
In obstetric patients, most attention has been directed at prophylaxis of the patient undergoing cesarean delivery. Antibiotic prophylaxis for prevention of perinatal neonatal group B streptococcal infection and for use in patients having premature or prolonged rupture of the fetal membranes is discussed in Chapters 1 and 19, respectively. Other obstetrical uses considered in this chapter are with cerclage and with manual removal of the placenta.
Cesarean Delivery
As noted in Chapter 20, cesarean delivery is accompanied by more frequent and more serious puerperal infections. Indeed, cesarean delivery is the single most important risk factor for maternal postpartum infection. Patients undergoing cesarean delivery have a fivefold to 20-fold greater risk for puerperal infection than patients having vaginal delivery.
Patients having nonelective cesarean delivery (i.e., in labor with or without membrane rupture) are at more risk than patients having electively scheduled procedures. Particularly among indigent populations, the risks in this subgroup have been reported as 45% to 85%. Labor, membrane rupture, and vaginal examination increase postpartum infection, most likely because they allow ascent of bacteria into the amniotic cavity before surgery.
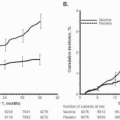
Since the early 1970s, more than 30 randomized, placebo-controlled trials have been reported on the use of prophylactic antibiotics representative in cesarean section. In a systematic analysis, it has been demonstrated that prophylactic antibiotics were found to decrease endometritis and wound infection both in nonelective (emergency) and elective cesarean delivery (without labor or ROM) (typical odds ratio [OR], 0.24; 95% confidence interval [CI], 0.18-0.32). Prophylactic antibiotics have also been shown to have profound and consistent effects in reducing wound infection (typical OR, 0.35; 95% CI, 0.28-0.44). Compared with placebo, both broadspectrum penicillins and cephalosporins are highly effective (typical ORs, 0.33 and 0.31, respectively), whereas metronidazole (in five studies) showed no significant decrease (typical OR, 0.72; 95% CI, 0.48-1.08).
Over 50 studies have compared one antibiotic with another for prophylaxis in cesarean delivery. A Cochrane Systemic Review concluded that both ampicillin and first generation cephalosporins have similar efficacy, as do ampicillin and second or third generation cephalosporins. Thus, ampicillin or a first-generation cephalosporin was recommended, as there was no benefit from use of a broader spectrum antibiotic. Subsequent to this review, a cohort study from the University of Alabama reported trends in postcesarean endometritis during 1992 to 2006. When routine use of intravenous azithromycin was added to standard cephalosporin prophylaxis (in 2001-2006), there was a significant and remarkable decrease in endometritis from 19.9% (in 1992-1996) to 6.3%. The authors attribute the effect mostly likely to coverage of ureaplasma urealyticum.
Administration of the antibiotic for prophylaxis after cord clamping became popular in the 1980s, when pediatricians expressed concern that antibiotics administered for prophylaxis before cord clamping could mask neonatal infection. Early studies comparing administration of the prophylaxis before versus after cord clamping have shown similar effectiveness. A more recent clinical trial showed that giving cefazolin prior to skin incision was superior to administration at cord clamping. For endometritis, the relative risk (RR) was 0.2 (95% CI, 0.15-0.94; absolute rates, 1% vs. 5%), and for total infectious morbidity the RR was 0.4 (95% CI, 0.18-0.87; absolute rates, 4.5% vs. 11.5%). There was no increase in neonatal sepsis (p = .99), neonatal sepsis workups (p = .96) or neonatal
length of stay (p = 1.7). In addition, the window of effectiveness for prophylaxis administered after clamping is narrow. We found that during one time period, there was often a considerable delay (and thus reduced effectiveness) in the injection of the prophylactic antibiotic. After discussion with our neonatologists, who expressed no concern about the effect of antibiotics given to the mother for prophylaxis before cord clamping, we have returned to a policy of use of prophylaxis on call to the operating room.
length of stay (p = 1.7). In addition, the window of effectiveness for prophylaxis administered after clamping is narrow. We found that during one time period, there was often a considerable delay (and thus reduced effectiveness) in the injection of the prophylactic antibiotic. After discussion with our neonatologists, who expressed no concern about the effect of antibiotics given to the mother for prophylaxis before cord clamping, we have returned to a policy of use of prophylaxis on call to the operating room.
Single-dose prophylaxis has been compared with multiple doses. Several individual studies have found equivalent efficacy between one dose and two or three doses of antibiotic for prophylaxis. In an analysis of nine studies comparing single and multiple doses, postoperative febrile morbidity was more common with single-dose prophylaxis (typical OR, 1.36; 95% CI, 0.95-1.95), but the CI includes 1.0. One review noted that cesarean section after prolonged rupture of the membranes, presumptively associated with a large intrauterine inoculum, “may be the one procedure for which single-dose prophylaxis is not so effective as two doses administered at an interval shorter than the 4 to 6 hours.” The Cochrane Systemic Review concluded that single-dose prophylaxis is as effective as multiple dose regimens and is less expensive.
As an alternative to parenteral administration of prophylactic antibiotics, there was a flurry of interest in intraoperative irrigation of the uterus and peritoneal cavity with antibioticcontaining solution. Publications 15 to 20 years ago established that this route is often equivalent to, but in some cases was less effective than, intravenous prophylaxis. Over the last 15 years, interest in this approach has waned.
Use of prophylaxis routinely (including in “low-risk” patients) had been controversial. A meta-analysis concluded that prophylactic antibiotics significantly decreased the risk of postoperative fever (RR, 0.25; 95% CI, 0.14-0.44) and of endometritis (RR, 0.05; 95% CI, 0.01-0.38) and showed a trend to decreasing wound infection (RR, 0.59, 95% CI, 0.24-1.45)—even among the population at lowest risk. The Cochrane Systematic Review similarly concluded prophylactic antibiotics have been demonstrated to decrease endometritis and wound infection after planned cesarean delivery, and the most recent ACOG Practice Bulletin recommended prophylaxis for low-risk patients (even though it was felt that the evidence was inconclusive).
Untoward effects such as changes in flora and direct toxic reactions may accompany the use of antibiotics for prophylaxis. Systematic investigations have detected significant changes in antimicrobial flora after prophylactic antibiotics. Overall, there were decreases in highly susceptible organisms and increases in enterococci and Enterobacteriaceae organisms. Although many of the Enterobacteriaceae organisms were susceptible to the prophylactic agent, some isolates of Pseudomonas sp also appeared. In these cases, the bacterial changes were without consequence. Patients who received cefazolin prophylaxis had a significant increase in enterococci (p < .015) and a significant decrease in Proteus sp (p < .05). Patients who received ampicillin prophylaxis had a significant increase in Mycoplasma species (p < .05), Klebsiella pneumoniae (p < .0001), Escherichia coli (p = .04), and any aerobic Gram-negative rod (p = .003). Ampicillin prophylaxis was associated with a decrease in Prevotella bivia (formerly Bacteroides bivius) (p < .05) and any anaerobic isolates (p < .01). Patients who received cephalosporin prophylaxis, followed by a cephalosporin for treatment, had significantly more wound infections than those who received other prophylaxis treatment combinations (19% vs. 16%; p < .01). Considerable evidence shows that antibiotic use for prophylaxis alters endometrial flora and has the potential to influence subsequent response rates to therapy. In patients who develop infection after prophylaxis, it is essential to obtain appropriate cultures to guide antibiotic therapy. Further, the antibiotic use for prophylaxis should not be used to treat a subsequent infection when one develops. In addition, extended-spectrum antibiotics should not be used for prophylaxis but should be reserved for treatment. Knowledge of the shifts in genital tract flora precipitated by antibiotic prophylaxis should be considered when selecting antibiotics to be used for therapy of postprophylaxis endometritis.
Direct toxic effects are unlikely. No serious allergic or toxic reactions were noted among 1,443 patients receiving prophylaxis in 26 studies. Less serious reactions such as rash were reported on occasion. However, several cases of fatal anaphylactic reaction to prophylactic antibiotics were reported in orthopedic patients, and two cases of fatal pseudomembranous enterocolitis have been attributed to a combination of prophylactic therapeutic antibiotics. Pseudomembranous colitis has been reported in 15 women having short-course prophylaxis. For patients who have documented immediate hypersensitivity reactions to penicillin, antibiotic choices for prophylaxis are limited. In such cases, cephalosporins are contraindicated, as are all penicillin-type antibiotics. The Cochrane Systematic Review recommends the use of single-dose clindamycin (900 mg). The Infectious Disease Society of America recommends vancomycin for prophylaxis of cesarean section endometritis in patients with an immediate hypersensitivity reaction to penicillin, but clindamycin seems a better choice (Box 24.1).
A common concern about widespread use of prophylaxis is a dangerous relaxation of standard infection control measures. Clearly, hand-washing, appropriate isolation techniques, proper disposal of infected materials and dressings, and changing of soiled scrub suits remain important elements in the control of infections and cannot be replaced capriciously by antibiotic prophylaxis. Recommendations for use of antibiotics in patients undergoing cesarean section are provided in Table 24.1 and Box 24.1.
Other Obstetric Considerations
For a full discussion of the use of prophylactic antibiotics for prevention of group B streptococcal perinatal infection and in premature rupture of the membranes, see Chapters 1 and 18, respectively.
The use of antibiotics for prophylaxis with emergency cerclage (when there is cervical dilation, cervical effacement, and membrane exposure) has appeal because of the high risk of infection and because infection probably would be fatal to the fetus. It has also been shown that the amniotic fluid may already have positive cultures in these circumstances. Yet, an ACOG Practice Bulletin concluded that evidence is insufficient to use perioperative antibiotic prophylaxis for either emergency or scheduled cerclage. Our practice has been to not use prophylaxis for elective cerclage. However, for cerclage with cervical dilation and membrane exposure (in the absence of evidence of chorioamnionitis), our practice is to use antibiotics for prevention of infection and we consider this a very special circumstance. Because establishment of infection would lead to delivery and thus be lethal to fetuses less than 23 to 24 weeks, we use a broad-spectrum antibiotic (usually a combination, such as ampicillin plus clindamycin plus gentamicin). Then, because it is desirable to achieve antibiotic levels in the amniotic fluid (not just in the blood), we begin prophylaxis well before the cerclage (such as 8-12 hours).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree