Allogeneic Hematopoietic Stem Cell Transplantation (HCT) for Hematologic Malignancies
Bipin N. Savani
Nishitha M. Reddy
Madan Jagasia
Haydar Frangoul
INTRODUCTION
The curative potential of allogeneic hematopoietic stem cell transplantation (HCT) in hematologic malignancies is well established,1 and currently acute myelogenous leukemia (AML) is the most common indication for HCT, accounting for approximately more than one-third of adult HCT.2 As the donor pool expands to include more unrelated and HLA-mismatched donors and umbilical cord blood (CB), and as treatment-associated morbidity and mortality rates decline with improvements in HLA matching, antimicrobial therapy, and management of graft-versus-host disease (GVHD), it has become increasingly feasible to offer this modality of treatment.3
HCT is offered either to increase the chance of cure in a disease that may have a low chance of cure with nontransplant approach (AML in first complete remission [CR1] with high-risk cytogenetics) or to cure an otherwise incurable disease (myelodysplastic syndrome [MDS], AML beyond CR1). Given the inherent risks of HCT, the risk-benefit ratio depends on the natural history of the disease versus the non-relapse mortality or transplant-related mortality due to the procedure itself. Although randomized control trials have been done, an ideal study of “intent to transplant analyses” is lacking in most disease types. With the advances in human leukocyte antigen (HLA) typing and supportive care, the non-relapse mortality after transplant continues to improve. The emergence of reduced-intensity conditioning (RIC) in deference to myeloablative conditioning (MST) broadens the applicability of this modality to patients who formerly would have been excluded from HCT because of advanced age or co-morbid conditions.4, 5, 6, 7 Here we discuss the indications, benefits, and risks of HCT in patients with hematologic malignancies.
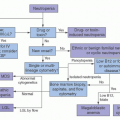
Chronic myelogenous (or myeloid) leukemia (CML) was a model disease to cure with HCT in the pre-tyrosine-kinase inhibitors (TKI) era. The introduction of TKIs led to a paradigm shift. Current indications of HCT are outlined in the National Cancer Center Network (NCCN) guidelines and addressed in Chapter 81. Consideration of HCT is recommended at 3 months post-TKI therapy if there is a >10% increase in BCR-ABL transcript as measured by quantitative PCR (QPCR) using the International Scale, or if conventional cytogenetics shows less than a partial cytogenetic response. Loss of cytogenetic response, molecular progression, or evolution of new mutations associated with TKI resistance should prompt a transplant evaluation. HCT consideration is often delayed based on response to second generation TKIs. Patients presenting in accelerated phase (AP) or blast crisis (BC)should be considered for earlier HCT.
Acute Myeloid Leukemia
In the United States, approximately 25% of AML patients younger than 70 years undergo an HCT. Median age at transplantation is 45 years; 75% of HCT recipients are younger than 55 years.2, 8, 9, 10, 11 The increasing need for HCT in adults with AML requires that all patients and their siblings undergo HLA typing early after diagnosis to determine if a matched related donor (MRD) is available and to allow for the possibility of unrelated donor (URD), haploidentical donor or umbilical cord blood (CB) searches.
Rationale of Hematopoietic Stem Cell Transplantation in First Complete Remission
Transplants should preferentially be performed on time and not reserved for relapsed disease or complete remission 2 (CR2) in high-risk patients. Although several reports of successful HCT in CR2 with a curative potential of 25% to 30% have been reported, such data are highly selective and should not influence a decision against earlier HCT, especially at experienced transplant centers. Moreover, the risk of relapse after URD HCT is higher for patients with unfavorable cytogenetics, irrespective of whether the transplant is performed in CR1 or CR2. Since the probability of achieving CR2 after chemotherapy in this group of patients is low, early HCT provides the optimal approach.9, 10, 12, 13
Indications of Hematopoietic Stem Cell Transplantation in Acute Myeloid Leukemia First Complete Remission
Several clinical features at presentation are associated with particularly poor outcome for AML patients. Age over 60 years, hyperleukocytosis, secondary AML (after antecedent myelodysplasia), or treatment-related myeloid neoplasm and, in some series, two induction cycles rather than one to attain CR1 are clinical factors that portend a worse outcome. As a result, many investigators proceed to offer HCT to such individuals.9, 12, 13
Cytogenetics, however, remains the most robust prognostic marker for risk stratification of AML at the time of diagnosis as well as in selection of post-remission treatments. On the basis of specific structural and numerical cytogenetic abnormalities, AML patients are divided into favorable, intermediate, and adverse risk groups (Chapter 75). A notable exception is the favorable cytogenetic risk group, in which HCT did not further improve outcome.
In recent years, a variety of novel molecular markers including mutations in the FLT3 (FMS-like tyrosine kinase) gene, the NPM1 (nucleophosmin) gene, and the CCAAT/enhancer binding protein alpha (CEBPA) gene have refined the risk stratification of intermediate-risk AML. Several investigators have used combinations of molecular markers to improve the patient’s risk assessment in cytogenetically normal AML.8
The most challenging group of patients with de novo AML falls within the intermediate-risk category.8, 12 Intermediate-risk patients who achieve CR1 after chemotherapy have a 50% probability of disease recurrence without HCT, and the probability that CR2 can be attained is low. With advances in the molecular classification of AML such as NPM1, FLT3-internal tandem duplication (ITD), CEBPA, and KIT, the indications for HCT can now be extended to approximately 40% of patients with AML with no chromosomal abnormalities.9, 10, 11, 12, 13 In a recent meta-analysis by Koreth et al.14 for the transplant period 1982 to 2006, a significant overall survival benefit was reported for patients with poor-risk and intermediate-risk AML who received HCT in CR1. NPM1 positivity has been considered a good-risk feature. More recently, it has been shown that only the subgroup with wild type isocitrate dehydrogenase 1 and 2 (IDH1/IDH2) along with NPM1 mutations are expected to do well.15 Thus, the prognostic impact
of known well validated mutations continues to evolve as new mutations are identified and the interactions of these mutations are understood.
of known well validated mutations continues to evolve as new mutations are identified and the interactions of these mutations are understood.
Donor Source and Outcome in Acute Myeloid Leukemia First Complete Remission
Importantly, the outcome of transplantation appears to be comparable for recipients of URD vs. MRD transplant. With improvements in transplant procedures including better donor selection (with high-resolution HLA- typing), excellent supportive care, and pre-emptive therapy in high-risk patients, we anticipate that outcomes will continue to improve.3, 16, 17, 18, 19, 20, 21
The results of 4 comparative studies together with meta-analyses of cord blood transplant (CBT) vs. URD transplant, the results of CBT appear to be as promising as those of matched URD transplant in adults with hematologic malignances.10, 12, 20, 22 In the absence of an HLA-matched donor, both CBT and haploidentical-stem cell transplantation (SCT) strategies (center dependent) are suitable options to treat high-risk patients. An upcoming blood and marrow transplant (BMT)-clinical trials network (CTN) study (BMT-CTN 1101; clinicaltrials.gov NCT01597778) will compare haploidentical-SCT with CBT.
Effect of Consolidation Therapy Pre-stem Cell Transplantation in Acute Myeloid Leukemia First Complete Remission
Relapse is the major cause of treatment failure after HCT in patients with AML10, 23; new approaches to prevent disease recurrence are being explored. A question of practical importance is whether patients undergoing transplantation in CR1 will benefit from post-remission chemotherapy prior to transplantation. There are no prospective studies demonstrating that any form of post-remission chemotherapy further reduces the risk of post-transplant relapse. However, results from two retrospective registry analyses suggest no benefit from adding further consolidation chemotherapy prior to HCT; in both studies (transplant period 1980 to mid-1990s), most patients were young and received full-intensity conditioning MRD HCT.9, 12, 14,24 The role of post-remission consolidation chemotherapy prior to RIC HCT in HR AML has not been adequately addressed.13, 25 In a recently published CIBMTR study, relapse occurred in 37% to 40%, and was higher in patients receiving RIC regimens. These findings highlight the importance of the depth of remission pre-SCT, especially in recipients in the RIC group.18 The efficacy of current chemotherapeutic regimens to achieve minimal residual disease negativity needs to be balanced against the risk of increasing co-morbidities prior to HCT.
Given the expanding use of RIC conditioning and the argument that treatment intensity may be important for cytoreduction prior to SCT, assessing the impact of pre-transplant consolidation therapy in AML CR1 on outcomes post RIC HCT is an important clinical question that remains unanswered. There is an ongoing CIBMTR analysis to determine if consolidation chemotherapy prior to RIC regimen for AML CR1 improves survival and relapse risk after RIC HCT.
Allo- vs. Auto-Stem Cell Transplantation vs. Chemotherapy in First Complete Remission
A recent summary of several clinical trials comparing HCT with alternative therapies for patients with AML CR1 showed benefits of HCT over alternative therapies.8, 9, 13, 26 Studies showed lower relapse rates for allograft recipients compared with those who received auto-SCT or further chemotherapy. None of the studies demonstrated an advantage for any of the alternative modalities (auto-SCT or further chemotherapy) as compared with HCT.
Full Myeloablative vs. Reduced-intensity Conditioning Regimen for Acute Myeloid Leukemia First Complete Remission
Conditioning regimens prior to HCT serve two purposes. One is the suppression of host immunity to allow for donor cell engraftment, and the other is the ablation of underlying malignancy. Ideally both these tasks need to be accomplished with minimal extramedullary toxicity. Conditioning regimens can be broadly classified as myeloablative (MST), RIC, and non myeloablative (NMA), based on the intensity of conditioning. MST regimens cause irreversible cytopenia and hence stem cell support is necessary. RIC regimens cause profound cytopenia and should be given with stem cells but cytopenia may not be irreversible. NMA regimens can theoretically be given without stem cell support.
MST HCTs are associated with decreased relapse but with increased transplant-related mortality (TRM). We now know that myeloablation is not as critical for engraftment as is immunosuppression. Reduced-intensity immunosuppressive approaches such as antithymocyte globulin (ATG), alemtuzumab, rituximab, and others can be used for transplant conditioning. There is a balance between reducing TRM by reducing intensity, and risking more relapse as the regimen is weakened.6, 27
No study to date has shown superiority of RIC to MST in AML4, 27, 28, 29, 30; we recommend reserving RIC (but not truly NMA) for patients thought to be ineligible for the more intense MST regimen. The importance of disease control at the time of transplant, especially for those patients undergoing the RIC condition, appears to have paramount importance when evaluating outcomes. In Martino’s large-scale retrospective analysis of AML patients undergoing SCT, those patients transplanted in CR1 had similar rates of relapse (MST: 27% vs. RIC: 32%).31 A prospective study randomizing patients to MST or RIC HCT regimens based solely on age of < or >50 years for AML patients in CR1 revealed similar non relapse mortality of 19% for MST and 20% for RIC with equivalent relapse and survival.32 These data suggest that MST conditioning may not be needed for those AML patients in CR1 at the time of HCT. Ongoing prospective randomized clinical trials (BMT-CTN 0901; clinicaltrials.gov NCT01339910) will answer this question more definitively.
Hematopoietic Stem Cell Transplantation for Patients Not in Remission and Beyond First Complete Remission
HCT for AML was first tested in patients with recurrent or relapsed refractory disease three decades ago. The transplant outcome for patients with induction failure or resistant relapse AML or for those with extramedullary disease treated with standarddose chemotherapy remains quite poor. Although the results are less than satisfactory, there is still a role for HCT for patients with advanced AML.
Difficulties in Achieving Complete Remission 2 Pre-stem Cell Transplantation
More recently, the investigators from City of Hope National Medical Center (COHNMC) reported their extended experience with 71 patients with refractory AML who were treated with HCT during a period of 22 years with 82% receiving grafts from MRD. The median age of these patients was 37 years (range 2 to 62 years) and the median follow-up was 1 year. Three-year disease-free survival (DFS) was 29% with a relapse rate of 54%. Cytogenetic data were available on 51 of the patients treated at COHNMC. Three patients had favorable, 27 intermediate, and 21 unfavorable cytogenetics. Those patients with favorable or
intermediate cytogenetics had DFS of 44% vs. only 18% in those with unfavorable cytogenetic features.33
intermediate cytogenetics had DFS of 44% vs. only 18% in those with unfavorable cytogenetic features.33
A score to predict transplantation success was developed in a retrospective survey of 1,673 patients who underwent a MST HCT for AML in relapse. In patients with low score the 3-year overall survival (OS) was 42% and those with a very high score had a dismal prognosis with only 6% alive at 3 years. The high score refers to the same group of patients in whom attempts to reinduce second remission are likely to fail. Patients with a short CR1, poor cytogenetics, and/or circulating blasts present a major clinical challenge.34, 35
Sequential Chemotherapy Followed by Reduced-intensity Conditioning Hematopoietic Stem Cell Transplantation
An interesting strategy of sequential cytoreductive chemotherapy, immediately followed by RIC and prophylactic donor lymphocyte infusion (DLI) in refractory and early relapse patients, was evaluated.36 This German protocol known as the FLAMSA (fludarabine, Ara-C, amsacrine)-RIC approach was reported in a prospective multicenter study involving 103 patients. The median survival of 16.4 months and the 4-year estimated OS of 32% were promising.36 This approach requires an HLA-matched donor available just when relapse is diagnosed. Therefore, for AML patients in CR1 even if HCT is not scheduled, a search for a donor should be initiated to enable sequential transplantation in case of early relapse.
Persistent Cytogenetic Abnormalities Pre-stem Cell Transplantation
Risk stratification is important to identify patients with AML who might benefit from HCT in CR1. An MD Anderson Cancer Center (MDACC) study analyzed 150 patients with AML and diagnostic cytogenetic abnormalities who underwent MST HCT while in CR1 to evaluate the prognostic impact of persistent cytogenetic abnormalities at HCT.37 Three risk groups were identified. Patients with favorable/intermediate cytogenetics at diagnosis (n = 49) and patients with unfavorable cytogenetics at diagnosis but without a persistent abnormal clone at HCT (n = 83) had a similar 3-year leukemia-free survival of 58% to 60% despite the higher 3-year relapse incidence in the latter group (32.3%, versus 16.8% in the former group). A third group of patients with unfavorable cytogenetics at diagnosis and a persistent abnormal clone at HCT (n = 15) had the worst prognosis, with a 3-year relapse rate of 57.5% and 3-year leukemia-free survival of only 29.2%. These data suggest that patients with AML and unfavorable cytogenetics at diagnosis and a persistent abnormal clone at HCT are at very high risk for relapse after HCT.37,38 These patients should be considered for clinical trials designed to optimize conditioning regimens (e.g., clofarabine-based regimen, see below) and/or to use preemptive strategies (e.g., chemotherapy [azacitidine], DLI, early withdrawal of immunosuppression if no GVHD, etc.) in the post-transplant setting, aimed at decreasing relapses.
Acute Myeloid Leukemia Complete Remission 2 and Beyond
Although the results of HCT in CR1 indicate an overall improved outcome compared with chemotherapy, many patients do not undergo transplantation while in CR1 based on either non-severe disease symptoms and/or on the patient desire, or mainly due to physician/patient preferences.
The currently available data suggest that patients with AML with untreated first relapse can expect an outcome following MST HCT similar to that of those patients proceeding to transplantation during CR2.10 Studies evaluating patients who receive an HCT in second or subsequent relapse, or third or later remissions following standard therapy, have demonstrated very few long-term survivors.
Relapse Prevention and Management of Relapses after Hematopoietic Stem Cell Transplantation
Monitoring of Relapse
Although HCT can be curative, even in advanced disease, treatment failure is commonly manifested by relapse of disease, for which treatment is successful in only a minority of patients.23 Detection of minimal residual disease in post-transplant surveillance is felt to be a necessary component of any strategy.39, 40 Past strategies for relapse prevention have focused on the use of DLI with variable success. Peritransplantation intervention and maintenance therapies (e.g., azacitidine) are under current investigation.41, 42
Traditionally, the detection of impending relapse in the post-transplant period had been based on donor chimerism analysis (e.g., poor donor chimerism has been associated with increased risk of relapse), but the lack of specificity remains a problem. In AML, the development of post-transplant minimal residual disease strategies is more complex because of the genetic heterogeneity of these disorders. Nevertheless, for some genetic subtypes, for example, reciprocal translocations or NPM1-mutated AML, minimal residual disease monitoring in the post-transplant period has already been realized.39, 43, 44, 45
Walter et al.24 investigated 99 AML patients receiving MST HCT CR1 by 10-color flow cytometry before transplantation. minimal residual disease-positive patients had lower 2-year estimates of survival (30.2% versus 76.6%) and higher 2-year estimates of relapse (64.9% versus 17.6%), compared with minimal residual disease-negative patients. After adjustment for other prognostically relevant parameters, a positive minimal residual disease status pre-HCT was significantly associated with increased overall mortality and relapse relative to minimal residual disease-negative HCT. Kebriaei et al.46 found a trend toward improved outcomes in 68 patients in cytogenetic remission compared with those with residual cytogenetic abnormalities at the time of HCT.
In the conservative treatment setting of AML, many minimal residual disease studies confirmed the potential of real-time PCR to predict the relapse risk in patients with reciprocal rearrangements. Some studies investigated the potential of molecular minimal residual disease monitoring for patients with reciprocal rearrangements also in the post-transplant period.39, 43, 47
Novel Conditioning Regimen
Incorporating novel agents in the conditioning regimen with potent antileukemic activity is a strategy that is currently under investigation.48 Clofarabine is a novel nucleoside analog that has potent antileukemic activity. It has shown efficacy in refractory disease as well as upfront scenarios. Geyer et al.49 combined total-body irradiation (TBI) with clofarabine and cytarabine for HCT in pediatric patients with refractory or multiply relapsed leukemia in a phase I/II study. The early results show the probability of a 1-year progression-free survival of 57.4%. Andersson et al.50 reported on a clofarabine/fludarabine/busulfan-based RIC regimen for advanced MDS and AML in 42 patients, which included children. In this high-risk patient population, 20 patients are alive at median survival of 23 months, which is an encouraging early result and warrants further studies.
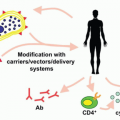
Targeted immunotherapy post-SCT: One of the strategies for the prevention of relapse of AML/MDS post-SCT is to use targeted immunotherapy as part of the conditioning regimen such as the employment of vaccines, and DLI. Additionally, natural killer cells
could be transferred for the treatment of leukemia relapse both during and after SCT.23, 51, 52
could be transferred for the treatment of leukemia relapse both during and after SCT.23, 51, 52
Post-transplant Therapy
The posttransplant therapeutic approach has been limited to TKI in patients with BCR-ABL1-positive leukemia. However, other strategies, including the use of interleukins, monoclonal antibodies, immunomodulatory agents (bortezomib), DNA methyltransferase inhibitors, and histone deacetylase inhibitors, are currently being explored in AML.39 The goal of these approaches is to treat minimal residual disease while minimizing adverse side effects and avoiding the impediment of donor cell engraftment. The use of hypomethylating agents (e.g., azacitidine) in patients with AML/MDS has drawn increased interest because of their demonstrated efficacy and relatively acceptable toxicity profile.41, 42,53
As our ability to monitor minimal residual disease post-HCT improves, along with identification of actionable molecular mutations, it will allow for the development of clinical trials aimed at prevention of relapse in a targeted fashion. Therapeutic interventions will be needed not only to prevent relapse but allow for simultaneous favorable modulation of the GVHD-graft versus tumor (GVT) balance.
Relapse after HCT for AML carries a very poor prognosis. Second HCT, although curative, is not an appropriate treatment option for a large number of relapsing patients (only 2% to 20% patients receive a second HCT), and efforts to increase the number of patients who may benefit from a second HCT are ongoing.23
Incorporating Novel Agents
The development of novel agents is expected to gather momentum as new actionable mutations are identified. A mutation in FLT3 is well known to be a poor prognostic marker in newly diagnosed and relapsed AML. Specific inhibitors of FLT3 such as sorafenib, lestaurtinib (CEP-701), and quizartinib (AC220) have been studied in relapsed or refractory AML.10, 39, 54 FLT3 inhibitors need to be investigated post-SCT in patients with FLT3 + AML to prevent relapse, a most common cause of transplant failure.55
Hypomethylating agents are active in high-risk MDS, and to a lesser degree in highly proliferative AML. 5-Azacitidine was shown in one study to prolong survival in elderly AML patients with low proliferative disease (expected disease course after HCT), and hence has drawn attention as an agent that may control low proliferative relapses after HCT.53
Summary
The initial approach for patients should be determined by cytogenetic risk factors, molecular markers, availability of a donor/ stem cell source, and response to induction chemotherapy. Patients with cytogenetic features associated with a good prognosis who achieve a CR with induction followed by consolidation chemotherapy should be observed without immediate transplantation, although HLA typing of these patients and their siblings is warranted at diagnosis. Patients with intermediate or poor markers who achieve a CR with induction/consolidation chemotherapy should undergo an HCT procedure early during CR1 if a histocompatible donor is available or any other stem cell source is available with low risk for transplant procedure. For those patients who do not enter a CR or who relapse after standard therapy, an HCT should be performed sooner rather than later. The transplant approach should be individualized for all patients based on remission status, performance status, and coexisting medical problems, i.e., MST vs. RIC regimens.
The treatment outcome of patients who have suffered a relapse of AML following HCT remains poor. Additional chemotherapy and second transplants are associated with exceptionally high morbidity and mortality and have generally resulted in short remissions. Chemotherapy followed by second non-myeloablative stem cell transplant (NST) HCT or DLI is a reasonable option for patients with late relapse after HCT. Relapse remains a major cause of transplant failure. We believe that the outcome of AML will be further improved by an innovative approach to reducing relapse risk, and that enrollment in clinical trials is the way to go and should be encouraged for all HCT recipients.
Myelodysplastic Syndrome
MDS is primarily a disease of older patients, with a median age at diagnosis in the eighth decade of life. Despite new therapeutic interventions, HCT remains the only curative option for this disease, with long-term survival probabilities ranging from 25% to 70%.56, 57, 58, 59 There is a significant selection bias for HCT as illustrated by the age difference between the average MDS patients and those who ultimately receive a transplant.
Rationale of Hematopoietic Stem Cell Transplantation in Myelodysplastic Syndrome
MDS originates in hematopoietic stem or precursor cells, and a logical approach is, therefore, to replace the clonal MDS cells by healthy donor cells via HCT procedure. Successful HCT requires that the infused cells from the healthy donor establish themselves (engraft), and that the malignant cells of the patient’s disease are eliminated by graft-versus-tumor (GVT) effects.
Over the past decade the approach to treating MDS has undergone major changes, at least in part related to the Food and Drug Administration (FDA) approval of several drugs for MDS and the development of new concepts for HCT. The drug therapy has improved the prognosis of patients with MDS, with 35% to 65% of patients achieving clinically relevant hematologic responses which may last from a few months (for high-risk MDS) to several years (predominantly for low-risk diseases). Concurrently, the emphasis with HCT has shifted from high-dose therapy, aimed at maximum tumor cell kill, to low- or reduced-intensity conditioning, relying heavily on donor cell-mediated immune effects to eradicate the disease (GVT effect). This GVT effect eliminates residual cells of the patient’s disease via recognition of minor histocompatibility antigens.
Patient Selection for Hematopoietic Stem Cell Transplantation
Since age is a major factor determining the decision about HCT, many patients younger than 60 years of age are likely to be considered for transplantation sooner and more often than older patients.60 Kuendgen et al. recently presented registry data that included 232 patients less than 50 years of age and 2,496 patients more than 50 years of age, where approximately 42% of the younger patients underwent transplantation compared to only 8% of the older patients.61
The International Prognostic Scoring System (IPSS) and World Health Organization prognostic score (WPSS) (discussed in the MDS chapter) are generally thought to identify patients in whom HCT should be considered sooner rather than later.62 In a retrospective registry-based analysis, Cutler and collaborators showed that upfront transplantation was associated with a greater number of added life years for intermediate-2 and high-risk IPSS patients.63 Delaying HCT offered the longest life expectancy in patients in IPSS categories low and intermediate-1. In the MDACC experience in 89 MDS patients who underwent HCT from 2002 to 2008, the 3-year OS rates were 79%, 49%, and 27%, respectively, for patients with WPSS low-intermediate-, high-, and very-high-risk categories, respectively.56
The European Group for Blood and Marrow Transplantation (EBMT) analyzed the post-transplant outcome of 692 patients with MDS according to their cytogenetic status. The overall survival and relapse rates were 47% and 34% for good-risk, 40% and 35% for intermediate-risk, and 31% and 57% for high-risk cytogenetics.64 A recent analysis showed that patients with secondary MDS had a post-transplant prognosis comparable to patients with de novo MDS once the data were adjusted for cytogenetic risk. In a small series of 47 patients with high-risk MDS, the 3-year OS was better in patients who received HCT than in those who did not (71% v 31%).65
Novel genetic factors are being studied to determine possible predictors of transplant outcomes.56 A significant correlation between HLA-DR15 and tumor necrosis factor (TNF) polymorphisms at position 308 among patients with MDS has been observed. The TNF-308 AG genotype conferred an increased risk of TRM compared to the GG genotype. Conversely, the TNF-863 AA genotype was correlated with decreased overall mortality and TRM compared with the CC genotype.66
Timing of Hematopoietic Stem Cell Transplantation
Determining the optimal timing of HCT for MDS has proven difficult, although all available data indicate that patients transplanted at an early stage of their disease have superior outcomes. Al-Ali et al.67 observed that HCT outcome was best if SCT was performed between 6 and 12 months after diagnosis, the negative effect of later HCT being possibly related to frequent blood transfusion, longer duration of pancytopenia, and disease progression while waiting for HCT. If SCT is delayed, for example because of a lengthy search for an unrelated donor, bridging treatment with hypomethylating agents may delay progression to AML.68
It is expected that incorporation of newer prognostic tools such as flow cytometry or molecular markers will improve our ability to select patients for transplantation at an earlier time period.69, 70 Newer risk models and individual risk factors (such as co-morbidities) will hopefully identify covariates that are likely to affect outcomes across non-transplant and HCT therapies.59, 71, 72, 73, 74
Pre-transplant Disease Status
In an attempt to improve chances for post-SCT success, patients with a high marrow myeloblast count, (e.g., >5-10%), typically will receive pre-SCT therapy with a hypomethylating agent or with more classical induction-type chemotherapy.56, 58, 68 The clinical impression is that pre-SCT therapy may select chemosensitive patients since it appears that patients who do respond to such therapy have a superior outcome, and patients who fail to respond have a poorer outcome than do untreated patients.75
The CR status at the time of transplant may impact relapse and TRM rates favorably; however, CR in chemotherapytreated patients with MDS is infrequent. Warlick et al.76 studied 84 patients undergoing HCT, and observed a 1-year cumulative incidence of relapse of 18% in patients in CR compared to 35% for those transplanted with active disease. In a retrospective analysis of 49 MDS/AML patients treated with T cell-depleted grafts, the 2-year cumulative incidences of TRM were 23%, 38%, and 40%, respectively, dependent upon response status prior to HCT (responsive disease, untreated, and refractory).77 Oran et al. also documented the benefit of minimal tumor burden at HCT in patients with high-risk MDS/AML undergoing RIC HCT. CR at SCT was associated with day-100 and 2-year TRM rates of 0% and 20%, respectively. Estimates of 2-year OS were 66% for those in CR, 40% for patients with active disease without circulating blasts, and 23% for patients with circulating blasts.78
Nakai et al.79 compared the outcomes of 283 adult patients with MDS (n = 215) or secondary AML (n = 68) who received (n = 188) or did not receive (n = 95) induction chemotherapy prior to HLA-identical sibling donor HCT, and showed no difference in survival rates between the two groups, with 5-year OS rates of 54% and 57%, respectively. Similarly, Scott and collaborators in Seattle failed to demonstrate a clear survival advantage for a cohort of patients studied retrospectively that received induction chemotherapy pre-transplant, although the risk of relapse was somewhat reduced.80
In the absence of controlled data, the decision to use pre-SCT induction therapy should be made on an individual basis. The treatment strategy should also take into account the fact that promising novel drugs are becoming available, although it is unclear if this approach will change long-term outcomes.
CURRENT OUTCOME DATA
An analysis by Warlick et al.76 showed a 1-year OS of 48%, a cumulative relapse incidence of 23%, and a DFS of 38%. The EBMT registry analyzed results in a cohort of 374 patients with <5% myeloblasts who received HCT from HLA-matched donors after various conditioning regimens.81 At 4 years, DFS was 48%, the relapse incidence 15%, and deaths not related to relapse 37%. The risk of relapse was increased after RIC compared to MST conditioning (HR 2.8), but overall survival did not differ significantly. Patients transplanted from URD had a lower relapse risk (HR 0.6), but a higher risk of non-relapse mortality (NRM) (HR 1.4), and OS did not differ significantly between related and unrelated HCT. T cell depletion of the transplanted cells resulted in higher NRM. Younger patients and patients transplanted within 12 months of diagnosis had superior outcomes.
The Fred Hutchinson Cancer Research Center (FHCRC) published results in 257 patients transplanted for secondary MDS. At 5 years, 19% of patients with tAML were surviving in remission, compared with 25% of patients with refractory anemia with excess blasts (RAEB), and 41% of patients with refractory anemia/refractory anemia with ringed sideroblasts (RA/RARS). Two-thirds of patients developed acute GVHD grades II—IV and 57% developed chronic GVHD. After adjusting for karyotype, there were no significant differences in outcome between the cohort with secondary MDS and the cohort of 339 patients with de novo MDS. The probability of relapse and DFS correlated significantly with disease stage (P < 0.001) and cytogenetics (P < 0.001). As in many other studies, patients transplanted from unrelated donors (n = 122) had a lower risk of relapse (P = 0.003) and superior DFS (P = 0.02) compared to patients transplanted from related donors.58 These results were confirmed in principle in a more recent analysis of CIBMTR data.82 These studies emphasize the importance of cytogenetics on HCT outcome.
Martino et al.83 analyzed HCT results in an EBMT cohort of 215 patients with MDS conditioned with RIC and 621 patients who received MST conditioning and were transplanted from HLA-matched related donors. For the MST and RIC cohorts, NRM at 3 years was 32 versus 22%, OS was 45% versus 41%, and DFS 41% versus 33%. Lack of remission before HCT (P = 0.001), poor-risk cytogenetics (P = 0.03), transformation to AML, and older age were risk factors for inferior DFS.
A British trial84 evaluated the results in 75 patients conditioned with an alemtuzumab-based RIC regimen and transplanted from unrelated donors. After 3 years transplant-related mortality (TRM), DFS, and OS for patients with refractory cytopenia with multilineage dysplasia (RCMD) were 24%, 55%, and 59%, respectively; the corresponding numbers for patients with RAEB (1 and 2) were 44%, 18%, and 18%, respectively. HLA-mismatch negatively affected all endpoints, as did disease status at HCT and patient co-morbidities.
Strategies to Improve Transplant Outcome after Hematopoietic Stem Cell Transplantation
Pre-transplant Use of Hypomethylating Agents
Field et al.85 presented data in 54 consecutive patients with MDS or chronic myelomonocytic leukemia (CMML) who underwent HCT from HLA-matched donors. Thirty patients had received azacitidine for one to seven (median 4) cycles, and 24 patients had not received azacitidine. At 1 year after HCT with conditioning involving high-dose busulfan and fludarabine, 47% of azacitidine-treated patients were alive, compared with 60% of patients not given azacitidine, but relapses were 20% and 32%, respectively. The authors concluded that outcome was consistent with a trend toward a lower incidence of relapse in azacitidine-treated patients.
In a study by De Padua Silva et al.86 17 patients with MDS underwent HCT after having received decitabine. At 1 year, 11 patients were alive, whereas six had died: four from disease progression, one from GVHD, and one with septicemia. Lubbert et al.87 presented data on 15 similarly treated patients who then underwent HCT following RIC regimen. At the time of reporting, 6 patients were alive in remission, whereas four had died from progressive disease and five from transplant-related complications while in remission.
FHCRC recently reviewed results in 68 patients who underwent HCT for MDS or AML transformed from MDS (tAML). Thirty-five patients had received cytoreduction with azacitidine prior to SCT followed by either an MST (40%) or RIC (60%) regimen, and 33 patients had undergone induction-type chemotherapy followed by SCT with MST conditioning. The 1-year overall survival was 57% in the azacitidine group, and 36% in the group given induction chemotherapy. Although the risk of post-SCT relapse and NRM was lower in the azacitidine group, none of the differences were statistically significant.88
Hypomethylating Agents Post-transplantation
Post-SCT relapse has remained a major cause of failure, particularly in high-risk MDS. Earlier studies had shown that intensification of the transplant conditioning regimen reduced the relapse frequency, though the associated increase in NRM may prohibit such use. It may be advantageous to allow for recovery from the conditioning-related effects, and then administer additional agents. As most of the post-transplant relapses occur within the first 1 to 2 years, addition of hypomethylating agents may have immunomodulatory effects that could potentially increase the GVT response.68
In a phase I dose-finding study, de Lima et al.53 at the MDACC started azacitidine at 6 to 7 weeks after HCT and determined that a dose of 32 mg/m2 given for 5 consecutive days was well tolerated. Forty-five patients with high-risk MDS/AML were treated and 1-year RFS was 58%. In addition, the authors noted that the incidence of chronic GVHD was lower in 5-azacitadine-treated patients than in historical controls. This observation was confirmed in a study at Washington University, which emphasized, in addition, that the beneficial effect on GVHD did not compromise the GVT effect.89
Similarly, Platzbecker et al.41 reported a prospective study of patients receiving HCT for MDS and AML. If the donor chimerism fell below 80%, patients were offered treatment with 5-azacitidine. This event occurred in 25 of 59 screened patients at a median of 169 days, and azacitidine was initiated at 75 mg/m2/day for 7 days. Sixteen patients responded with an increase in donor chimerism or stabilization at 80%. Eleven patients were given additional 1 to 11 (median 4) cycles of azacitidine. Hematologic relapse eventually occurred in 13 patients (65%), but was delayed to days 56 to 558 (median 231). Therefore, preemptive azacitidine treatment may be effective in delaying hematologic relapse.
Other Post-stem Cell Transplantation Interventions
DLI may improve transplant outcomes in high-risk MDS by decreasing relapse rates. Kolb et al.90 investigated escalating doses of DLI to treat a subset of patients with high-risk MDS (n = 67) or patients with secondary AML (n = 90) after RIC HCT. Relapse appeared less likely in patients given DLI. Another approach under investigation by several groups is the use of vaccines against leukemia-specific antigens such as Wilms tumor gene 1 (WT1) and proteinase-3-derived PR1 peptide (or the use of antigen-specific cytotoxic T-lymphocytes). Peptide-based vaccination has been shown to elicit immunologic T cell and clinical responses in myeloid leukemia.51, 52
Relapse after Hematopoietic Stem Cell Transplantation
Post-SCT relapse remains a challenging problem, particularly in patients prepared for HCT with RIC regimens.23, 57, 60 Multiparameter flow cytometry has been used effectively to show that aberrancy of marrow blasts pre-SCT can influence outcome after SCT.69 However, the definition of minimal residual disease in patients with MDS has not been clarified.39
The infusion of donor lymphocytes in patients with relapse has shown only limited efficacy, as has withdrawal of immunosuppressive therapy (IST).23, 58 Early administration of hypomethylating agents may be more effective.23, 41, 53, 89 The prophylactic use of drugs such as hypomethylating agents or small molecule inhibitors that are coming into use in patients with high-risk disease may be even more effective. Intensive chemotherapy has generally been disappointing, and second allo-SCT in adults has yielded low-success rates.23, 91
Summary
HCT continues to be the only curative option for MDS. Since the majority of patients with this disease are often older and frail, treatment-related mortality and morbidity remain major obstacles to be overcome. The development of reduced toxicity regimens has allowed HCT to be offered to older patients and those with clinically relevant co-morbid conditions.
Post-transplant relapse and GVHD remain problems requiring further research in this area. Ongoing studies are exploring the incorporation of novel agents (used in non-transplant therapy) during the peri-transplant period.
Acute Lymphoblastic Leukemia
HCT is a potentially curative therapeutic modality for acute lymphocytic leukemia (ALL). Unlike the dramatic advances made in the treatment of childhood ALL with 5-year survival at more than 80%, therapeutic progress for adult ALL has been relatively slow, with long-term survival being achieved in only about 30% to 40% of patients.92, 93
As modern induction regimens can obtain CR rates in up to 80% to 90% of patients, the major barrier to improved results in the treatment of ALL in adults remains the high relapse rates in patients with CR1. Among the various post-remission therapies, HCT remains the single most effective modality for consolidation and prevention of relapse.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree