Haematology of pregnancy
Pregnancy places extreme stresses on the haematological system and an understanding of the physiological changes that result is obligatory in order to interpret any need for therapeutic intervention.
Physiological anaemia
Physiological anaemia is the term often used to describe the fall in haemoglobin (Hb) concentration that occurs during normal pregnancy (Fig. 30.1). Blood plasma volume increases by approximately 1250 mL, or 45%, above normal by the end of gestation and although the red cell mass itself increases by some 25% this still leads to a fall in Hb concentration. Values below 10 g/dL are probably abnormal and require investigation.
Figure 30.1 Haematological changes during pregnancy.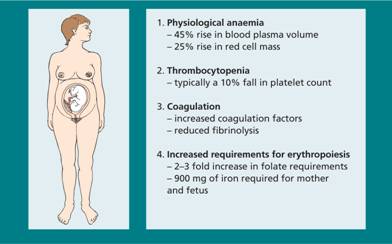
Iron deficiency anaemia
Up to 600 mg iron is required for the increase in red cell mass and a further 300 mg for the fetus. Despite an increase in iron absorption, few women avoid depletion of iron reserves by the end of pregnancy.
In uncomplicated pregnancy, the mean corpuscular volume (MCV) typically rises by approximately 4 fL. A fall in red cell MCV is the earliest sign of iron deficiency. Later, the mean corpuscular haemoglobin (MCH) falls and finally anaemia results. Early iron deficiency is likely if the serum ferritin is below 15 μg/L together with serum iron <10 μmol/L and should be treated with oral iron supplements. The use of routine iron supplementation in pregnancy is debated but iron is probably better avoided until the Hb falls below 10 g/dL or MCV below 82 flin the third trimester.
Folate deficiency
Folate requirements are increased approximately twofold in pregnancy and serum folate levels fall to approximately half the normal range with a less dramatic fall in red cell folate. In some parts of the world, megaloblastic anaemia during pregnancy is common because of a combination of poor diet and exaggerated folate requirements. Given the protective effect of folate against neural tube defects (NTDs) as well as against anaemia, 400 μ g/day folic acid (5 mg if there has been a previous NTD pregnancy) should be taken periconceptually and throughout pregnancy. Food fortification with folate is now being practised in many countries (not the UK) and has been associated with a fall in incidence of NTDs. Vitamin B12 deficiency is rare during pregnancy although serum vitamin B12 levels fall to below normal in 20–30% of pregnancies and low values are sometimes the cause of diagnostic confusion.
Thrombocytopenia
The platelet count typically falls by approximately 10% in an uncomplicated pregnancy. In approximately 7% of women this fall is more severe and can result in thrombocytopenia (platelet count <140 × 109/L). In over 75% of cases this is mild and of unknown cause, a condition referred to as incidental thrombocytopenia of pregnancy. Approximately 21% of cases are secondary to a hypertensive disorder and 4% are associated with immune thrombocytopenic purpura (ITP; Fig. 30.2).
Figure 30.2 Causes of thrombocytopenia during pregnancy.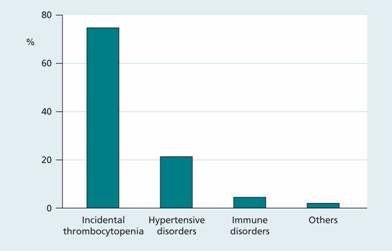
Incidental thrombocytopenia of pregnancy This is a diagnosis of exclusion and is usually detected at the time of delivery. The platelet count is always > 70 × 109/L and recovers within 6 weeks. No treatment is required and the infant is not affected.
Thrombocytopenia of hypertensive disorders This is variable in severity but the platelet count rarely falls to <40 × 109/L. It is more severe when associated with pre-eclampsia and if severe the primary treatment is as rapid delivery as possible. The platelet count falls for a day or two after delivery and then recovers rapidly. The HELLP syndrome (haemolysis, elevated liver enzymes and low platelets) is a subtype of this category. It is associated with prolongation of the prothrombin time (PT) and activated partial thromboplastin time (APTT).
Idiopathic (autoimmune) thrombocytopenic purpura (see p. 334) In pregnancy, ITP represents a particular problem, both to the mother and to the fetus, as the antibody crosses the placenta and the fetus may become severely thrombocytopenic.
Like all adults, pregnant women with ITP and platelet counts > 50 × 109/L do not usually need treatment. Treatment is required for women with platelet counts <10 × 109/L and for those with platelet counts of 10–30 × 109/L who are in their second or third trimester or who are bleeding. Treatment is with steroids, intravenous immunoglobulin G (IgG), rituximab and splenectomy as appropriate.
At delivery, umbilical vein blood sampling or fetal scalp vein sampling to measure the fetal platelet count may be offered although their exact role is unclear. In general, caesarean section is not indicated when the maternal platelet count is > 50 × 109/L unless the fetal platelet count is known to be <20 × 109/L. Platelet transfusion may be given to mothers in labour with very low platelet counts or who are actively bleeding. Caesarean section may be indicated to protect the fetus.
Newborns of mothers with ITP should have a blood count measured for the first 4 days of life as the platelet count may progressively drop. A count > 50 × 109/L is reassuring. Cerebral ultrasounds may be performed to look for intracranial haemorrhage (ICH). In newborns without evidence of ICH, treatment with intravenous IgG is appropriate if the infant’ s platelet count is <20 × 109/L. Neonates with thrombocytopenia and ICH should be treated with steroids and intravenous IgG therapy.
Haemostasis and thrombosis
Pregnancy leads to a hypercoaguable state with consequent increased risks of thromboembolism and disseminated intravascular coagulation (DIC; see p. 355). There is an increase in plasma factors VII, VIII, X and fibrinogen with shortening of PT and APTT, and fibrinolysis is suppressed. These changes last for up to 2 months into the puerperal period and the incidence of thrombosis during this period is increased. There is an association between thrombophilic conditions in the mother and with recurrent fetal loss. This is presumed to result from placental thrombosis and infarction.
Treatment of thrombosis
Warfarin has no role in management. It crosses the placenta and in addition is associated with embryopathy, especially between 6 and 12 weeks’ gestation. Heparin does not cross the placenta but a significant side-effect of prolonged use is maternal osteoporosis. Low molecular weight heparin is now the treatment of choice because it can be given once daily and is less likely to cause osteoporosis.
Normal blood count
The cord blood Hb varies between approximately 16.5 and 17 g/dL and is influenced by the timing of cord clamping (Fig. 30.3
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


