Chapter Outline
Plain Language Summary 375
Introduction 376
Reducing Cancer Diagnoses 379
Changing Terminology 380
Less Surgery for In Situ Breast Cancer 382
Reduced Treatment for DCIS 384
Limiting Radiotherapy in Patients with DCIS 384
Neoadjuvant Endocrine Therapy for DCIS 387
Anti-HER2 Therapy 387
Reducing Mastectomy for Invasive Cancer 387
Reducing the Number of Patients Who Get Radiotherapy After Breast Conserving Surgery for Invasive Breast Cancer 389
Reducing Surgery in the Axilla in Women With Screen-detected Invasive Breast Cancer 390
Is Axillary Node Dissection Necessary in All Node-Positive Patients? 392
Do Patients Require Any Axillary Surgery? 394
Systemic Therapy in Overdiagnosed Cancers 394
References
Plain Language Summary
Women with screen-detected breast cancers have better survival than those with symptomatic breast cancers. Many screen-detected cancers are low risk because they are unlikely to recur or to cause death, with between 11% and 19% of screen-detected cancers considered as being overdiagnosed, that means that these women have been diagnosed and treated for breast cancer but if they had not been screened then they would not have known they had breast cancer (nor required treatment for it) in their lifetime. As well as overdiagnosis, some screen-detected breast cancers are probably overtreated, meaning women receive more aggressive treatment than necessary to control their cancer. There is a need to better match treatment not only to the patient’s characteristics and the tumor stage but also to the tumor biology. Some patients with noninvasive cancers–known as ductal carcinoma in situ (DCIS)-are overtreated and ongoing studies are looking at whether low grade DCIS needs any treatment at all. Although the numbers of patients having breast conserving surgery has increased over time, many patients are unnecessarily treated with mastectomy. Whole breast radiotherapy after breast conserving surgery is the standard for women with invasive cancer but not all women with screen-detected invasive breast cancer need it. Likewise not all women with screen-detected invasive cancer need axillary surgery. Similarly systemic therapies after a diagnosis of screen-detected breast cancer may be over used in some women. The increased use of molecular profiling should limit the use of chemotherapy but the threshold for using adjuvant endocrine treatment is such that few women are not prescribed this. Chemotherapy and hormone therapy are not without morbidity. It is essential that overdiagnosis and overtreatment of screen-detected breast cancer are addressed in future studies.
Introduction
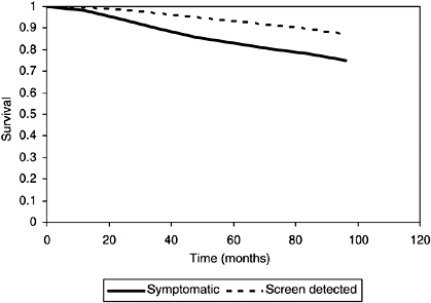
The method of detection of breast cancer appears in a number of studies to be an independent prognostic variable. When controlled for age, nodal status, and tumor size, a study of 1983 Finnish women with invasive breast cancer reported that screen-detected cancers had a lower risk of relapse compared with symptomatic cancers and had an improved overall survival after adjusting for other prognostic factors. Women whose cancers were detected outside screening had an increased death rate (HR) 1.90 (95% confidence interval (CI), 1.15–3.11) compared to women with screen-detected breast cancer, even though symptomatic women were more likely to receive adjuvant systemic therapy. In another study of three randomized screening trials (Health Insurance Plan, National Breast Screening Study NBSS-1, and NBSS-2) in the analysis adjusted for known prognostic parameters, patients whose cancer was found via screening had a more favorable prognosis than women with symptomatic cancers. The relative risks for death were 1.53 (95% CI, 1.17–2.00) for interval and incident cancers, compared with screen-detected cancers and 1.36 (95% CI, 1.10–1.68) for cancers in the symptomatic group, compared with screen-detected cancers. A study of 5604 English women with breast cancer diagnosed between 1998 and 2003 also found that women with screen-detected cancers fared better than their symptomatic counterparts ( Fig. 15.1 ). The HR for survival of screen-detected versus symptomatic women was 0.79 (95% CI, 0.63–0.99). These various observations are consistent with the view that many screen-detected breast cancers are low risk and that some of these cancers require less or even no treatment because they would not have caused problems in the patient’s lifetime. It is well recognized that a proportion of screen-detected breast cancers do indeed represent overdiagnosis and that this is of the order of 11% from a population perspective, or approximately 19% from the perspective of a woman invited to screening. Chapter “Challenges in Understanding and Quantifying Overdiagnosis and Overtreatment” of this book provides additional information on estimates of overdiagnosis from breast screening.
There is also clearly overtreatment of screen-detected breast cancer. Overtreatment can be considered to occur in two ways, although these are related. First, in overdiagnosed cases, since by definition these cancers did not need to be found (as they would not have become clinically apparent in the absence of screening), any treatment is unnecessary in these women and so represents overtreatment. Diagnosing less low risk cancers or renaming some of these cancers are potential methods of limiting overtreatment. There has been renaming of cancers at other sites, such as the bladder and the cervix, and this has produced less overdiagnosis and has reduced overtreatment . It has also reduced anxiety and improved the quality of life in these women.
The second aspect of overtreatment is the administration of therapies that are unnecessary to treat the early stage cancers detected through breast screening. The one-size-fits-all philosophy of treating in situ or invasive breast cancer based on tumor size and node status is inappropriate and takes no account of the range of biology of cancers seen within the screen-detected population. There is a real need to tailor treatment not only to the patient and tumor stage but also to the biology of the cancer, both for screen-detected as well as nonscreen-detected cancers.
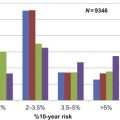
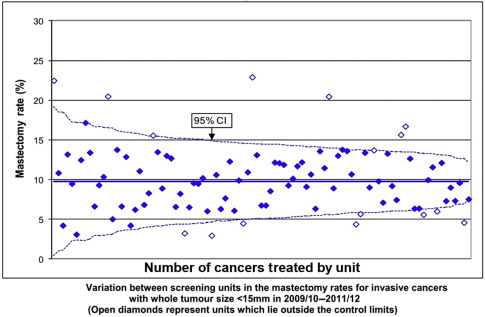
There is some evidence that tailoring treatment to the cancer is occurring in terms of surgical treatment. The absolute numbers of breast conserving surgery episodes has increased over time and the absolute numbers of mastectomies has fallen. Nonetheless, there remains enormous variation in the rates of breast conserving surgery for cancers with a total size less than 15 mm throughout the UK and North America, and the message of reducing the extent of surgery has not reached all surgeons ( Fig. 15.2 ). Some of this variation may be patient driven but thus there is a need to ensure patients are educated that more extensive surgery is not beneficial. The rate of mastectomy in the UK is actually higher for noninvasive breast cancers (27% in 2011/12) compared with invasive breast cancer (23%). As a result of breast screening the actual numbers of women having mastectomy for noninvasive cancer has increased every year in the UK for the past 15 years. The incidence of DCIS increased from 5.8 per 100,000 women in the 1970s to 32.5 per 100,000 women in the US in 2004 and then reached a plateau. Over 60,000 women will be diagnosed with DCIS in the USA in 2015. This needs to be addressed by the surgical community. Most women detected with breast cancer through screening are node-negative and there has been a move to reduce the number of women having axillary clearance even in patients with 1 or 2 positive sentinel nodes. Sentinel node is a step in the right direction but do women with small low risk cancers require any axillary surgery?
Whole breast radiotherapy after breast conserving surgery is now standard but do all screen-detected women require whole breast radiotherapy? Is there any role for partial breast radiotherapy and can some women avoid radiotherapy altogether? Ongoing studies are providing evidence that one can identify women at low risk in whom radiotherapy can be omitted. Whole breast radiotherapy is used following breast conserving surgery for DCIS but again not all women need it. This means that many women receive treatment they may not need and experience the associated side effects, yet have little potential gain. Current evidence shows that the breast cancer specific mortality at 20 years is only 3.3% and was not influenced by the use of radiotherapy. Using genomic tests to identify women with low risk DCIS is one avenue of research that is showing promise. There is also an onus on the oncological community to ensure that systemic adjuvant therapies are administered on the basis of tumor characteristics rather than just stage at diagnosis. Systemic therapies can produce significant and long-term adverse effects on quality of life so it is essential that these treatments are tailored to the patient and their cancer.
Reducing Cancer Diagnoses
Many core biopsies are performed for calcifications detected on mammography that have a low risk of being invasive cancer or DCIS, but a high likelihood of being benign. Should these really be a target for screening? If lesions that had a greater than 50% risk of representing DCIS or greater than 10% risk of being invasive cancer were targeted, would it be possible to reduce overdiagnosis and also the numbers of interventions? A study by Flowers and Esserman using these criteria found that the biopsy rate fell by almost half from 100% to 52%. The cancer to biopsy yield rose from 28% to 47% and only a single invasive cancer would have been missed: a 3 mm Grade 1 invasive cancer. Redefining what lesions are biopsied is one potential method of reducing overdiagnosis and thus reducing over treatment.
Lobular carcinoma in situ (LCIS) is a rare form of mammary cancer first described in 1941 by Foote and Stewart. LCIS was initially considered a form of breast cancer and was treated by mastectomy but later it became reclassified as a marker of generalized breast cancer risk with a relative risk of breast cancer of between 8 to 10 times that of the women of the same age without LCIS. The rate of invasive breast cancer in women with LCIS is approximately 1% per year. Atypical lobular hyperplasia (ALH) is diagnosed when there is a lesser degree of lobular expansion with the same cells as seen in LCIS and has an increased risk of invasive breast cancer, between 4–5 times that of the general population. Because of the difficulties of separating LCIS and ALH, the term lobular intraepithelial neoplasia (LIN) has been introduced to include both lesions. LCIS is diagnosed by screening in somewhere between 0.5% and 2% of all core biopsies. The current North American NCCN guidelines and the UK guidelines are that patients with LCIS or ALH on core biopsy should have surgical excision. This is based on studies that have shown upgrade rates to invasive cancer or to DCIS as high as 50%. The logic of excision is that there is likely to be a worse lesion in the breast. There are however problems with the studies investigating women with LCIS on core biopsy because they have contained small numbers of women and have reported a huge variation in upgrade rates varying from 0% to 50%. More recently there has been an attempt to correlate radiology with pathology and two groups can be identified: a concordant group where the histologic findings in the core biopsy adequately explain the findings on imaging and a discordant group where the histological findings on the core biopsy do not adequately explain the findings on imaging studies. The upgrade rate of core biopsy diagnosed LCIS and ALH in patients with concordant imaging findings is small. A recent prospective multi-institutional study by Nakhlis enrolled 79 patients. In 74 women who had LIN as the worst lesion on core biopsy with concordant imaging, 73 had no upgrade on surgical excision with only one upgrade to DCIS. From a total of 335 cases from five different publications in the literature where there was concordance between histology and imaging there have been just six upgrades (1.8%). Five of these were to DCIS (1.5%) and one was a 2 mm grade I invasive cancer. There is now growing evidence that excision biopsy can be avoided in patients diagnosed with LIN on core biopsy where there is concordance with imaging. If however there is atypical ductal hyperplasia (ADH) or pleomorphic LCIS is diagnosed on core biopsy then excision is still required. The upgrade rate for pleomorphic LCIS is much higher than for nonpleomorphic LCIS and varies from 17% to 46% in three small series.
Similar arguments can be made for avoiding excision of radial scars and papillary lesions that have been adequately sampled with a large core vacuum assisted device. Radial scars are found in association with low or intermediate grade DCIS or low grade invasive breast cancers in between 3% and 40% of patients. If these lesions are adequately sampled however the upgrade rate following surgical excision is small enough to believe that excision is unnecessary unless there are concerns of malignancy on large bore biopsy. The same is true for papillary lesions and formal excision is required only where a large bore core biopsy shows atypia. Radial scars and papillary lesions diagnosed on 14 gage core biopsy should be further sampled by a large gage vacuum assisted device and only where there is concern histologically should excision be advised. This would avoid a significant number of the excision biopsy procedures currently performed in women with radial scars and papillary lesions.
Changing Terminology
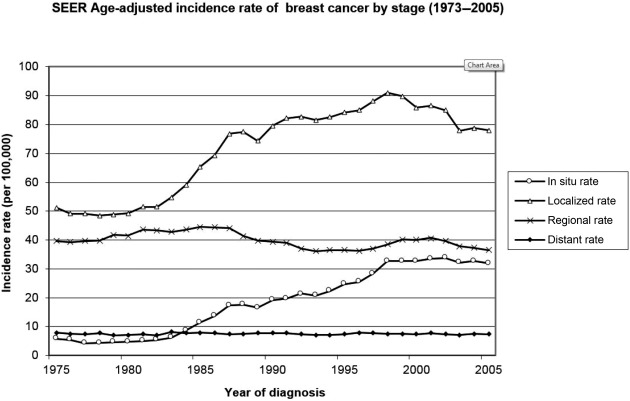
DCIS was uncommon before mammographic breast screening was introduced but since the introduction of breast screening there has been a 500% increase in the number of DCIS cases diagnosed ( Fig. 15.3 ). Between 20–30% of all cancers diagnosed through screening are now DCIS. What happened to these women with DCIS before breast screening? A study by Welsh et al. looked at seven series of women who died without breast cancer and had their breasts examined at autopsy. The prevalence of invasive cancer in this population was 1.3% with a range of 0% to 18%. The prevalence of DCIS was 8.9% with a range of 0% to 14%. In women aged 40–70 who had more than 50 slides examined the prevalence of DCIS was 14.5%. Currently, as a result of breast screening many of these women with DCIS are identified even though many would have died of other causes and the DCIS would never have become symptomatic. The reason for detecting DCIS is that this should in theory reduce the rate of subsequent breast cancer development. There is, however, limited evidence that there has been a major reduction in the subsequent rates of invasive cancer or any a reduction in the numbers of women with advanced disease has not been as large as one might have hoped.
The current dilemma relates to whether all patients with DCIS require treatment and should all DCIS be considered cancer? A cancer or a neoplasm is defined as an abnormal mass of tissue whose growth is in excess of, or uncoordinated with that of surrounding normal tissue and whose growth continues in the same excessive manner after the removal of the stimulus which evoked the change. Not all DCIS progresses and not all DCIS lesions continue to grow in an excessive manner after development. The question is can we identify those DCIS cases that are true neoplasms and those that continue to grow and progress to cancer?
DCIS is diagnosed if histologically there are two complete spaces filled or there is greater than 2 mm of an intraductal proliferation with significant atypia. If there are less than 2 complete spaces in the terminal duct lobular unit or less than 2 mm of disease even if significant atypia is present, then this is classified as ADH. There is no real scientific basis for this definition of DCIS based on number of spaces or size of the lesion. Not all pathologists adhere to this definition and this has led to significant variation in how small areas of epithelial proliferation within the terminal duct lobular unit are classified. Studies show up to a third of pathologists will diagnose DCIS if a single 1.5 mm ductal space is filled with low grade atypical epithelium with no necrosis and a classical cribriform architecture, yet based on the currently agreed criteria this should be diagnosed as ADH. The problem is that there is a lack of diagnostic concordance between pathologists in interpreting these difficult lesions. A recent study showed excellent concordance in the diagnosis of invasive cancer (96%) but a lower concordance in DCIS (84%) and a lower still concordance in atypia (48%). Variation in diagnosis potentially leads to variation in treatment for women with histologically identical lesions.
There have been huge advances in molecular pathology and when the genomics of ADH is compared with DCIS, ADH has most of the features of DCIS. ADH is not reversible, is often clonal and it can progress to invasive cancer, although this is rare. Genomic studies have shown that ADH and low grade DCIS are more closely related to LCIS than to high grade DCIS. This has led some to argue that low grade DCIS and ADH should be reclassified together as a single entity-ductal intraepithelial neoplasia or DIN as they are clearly different abnormalities compared to high grade DCIS. Distinguishing ADH from low grade DCIS does appear somewhat illogical. The term LIN was introduced to combine LCIS an ALH because the two are so obviously related and there was a lack of consistency between pathologists. Classifying low grade DCIS as neoplasia rather than cancer does seem sensible based on what we know. This reclassification would follow the lead from other organs. Areas of atypia and carcinoma in situ (CIS) in the cervix are now incorporated into the condition of cervical intraepithelial neoplasia or CIN. Is it time for a similar approach to low grade and some intermediate grade DCIS?
The 5-year risk of developing ipsilateral invasive breast cancer among women diagnosed with LIN but having no treatment is about 3–5% and the 10 year risk between 5–10%. For ADH and low risk DCIS without treatment the rate is pretty similar at 3–5% at 5 years and 5–10% at 10 years. The risk associated with intermediate risk DCIS is a little higher at about 4–5% at 5 years and 7–12% at 10 years. The risk is much higher for high risk DCIS and without treatment is about 7–5% at 5 years and 15–20% at 10 years. It is thus evident that different grades and risk categories of DCIS have differences in their natural history and yet they are all classified together as DCIS.
There is also concern that some lesions classified currently as DCIS may be invasive cancers. Tabár and colleagues have reported that patients who have extensive DCIS and have casting-type calcification have a high rate of developing invasive recurrence after mastectomy. How does this happen? Pathologists argue that they examine only a fraction of the disease and that invasion can be present in the breast but that this is missed because only a small proportion of disease is sampled. In some patients tumor cells are seen in lymphatics and even in lymph nodes yet there is no histological evidence of invasion identified in the breast. Is this just a sampling issue or is it that histological assessment cannot differentiate in situ from invasive cancer? Patients that have invasive cancer that is missed are at risk of being undertreated. There is an urgent need to develop better ways of assessing the presence of invasion and the likely biological behavior of DCIS, so that both overtreatment and undertreatment are avoided.
Less Surgery for in Situ Breast Cancer
One of the consequences of the increase in the number of women with DCIS detected through breast screening is that over the period 2001–2015 the number of women in the UK having mastectomy for DCIS has more than doubled. There is also evidence from the USA that mastectomy rates have increased. The explanation is that although a higher percentage of women with DCIS are now having breast conserving surgery, the number of women diagnosed with DCIS over this period of time has more than doubled. In 2011–12 the mastectomy rate for invasive cancer was 23% but for non or micro invasive cancer it was 27%. There were relatively few cases of low grade DCIS so it is difficult to estimate the numbers having mastectomy for low grade DCIS. The counterargument is that patients who have extensive DCIS in association with invasive cancer are treated by mastectomy, so if all women with DCIS eventually develop invasive disease mastectomy might not be overtreatment. Post-mortem studies suggest however that not all DCIS becomes symptomatic. There needs to be greater effort in DCIS to minimize treatment and this is the basis of the upcoming trials of low grade DCIS discussed later. The whole ethos behind screening is to detect disease early so as to improve outlook and to reduce the treatment required. There is an urgent need to reduce the number of women with DCIS having more extensive surgery and to reduce the overall burden of treatment for this condition that in some women would never have caused problems in their lifetime.
Within the UK screening program the Sloane project collected prospectively, surgery, pathology, and radiotherapy data on patients with in situ cancers diagnosed and treated between 2003 and 2012. Approximately 50% of all DCIS cases have been captured in this data set. Patients who had successful breast conserving surgery at one operation had a mean pathology size of 12 mm and the size increased to 17 mm for patients who had successful breast conserving surgery at two operations. For those who had breast conserving surgery and then subsequently went on to mastectomy, their average pathology size was 40 mm. There were 1969 women who had a mastectomy for DCIS over 20 mm and 510 women who had mastectomy for DCIS that measured less than 20 mm. In patients who had a mastectomy for DCIS under 20 mm, radiology often overestimated tumor size. The average overestimate in these patients was 19.86 mm. The Sloane data set shows clearly that many women who currently have mastectomies for DCIS could be treated by breast conserving surgery. It would appear that up to a half of women in the UK who have a mastectomy for screen-detected DCIS, based on size alone, do not require it. There is also a huge variation in the percentage of women having unnecessary mastectomies between hospitals. Women with DCIS diagnosed through screening should have biopsies at both ends of the mammographic lesion and have a careful evaluation of the extent of disease before any decision is made on surgery. Performing a mastectomy routinely on the basis of the calcification measuring 4 cm or more, with a single biopsy demonstrating DCIS, is inappropriate. National guidelines on an acceptable rate of mastectomy for small areas of DCIS are required and centers that have rates that fall well outside these guidelines need to provide an adequate explanation.
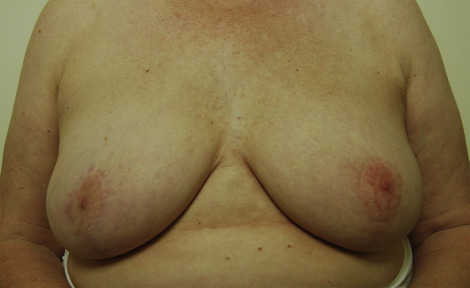
Although the international standard care for patients with DCIS measuring 4 cm in size or over has been mastectomy, wide excision and radiotherapy offers equivalent outcomes providing all the DCIS is adequately excised. A number of units scattered throughout the UK have developed methods for excising large areas of DCIS and conserving the breast in women with DCIS >40 mm in extent. This involves multiple wire localizations to mark all visible disease and combining the excision with a therapeutic mammaplasty. Such procedures produce excellent cosmetic results ( Fig. 15.4 ), have a high rate of complete excision and to date a low rate of subsequent recurrence. In Edinburgh these are performed as bilateral procedures by a team of a breast and plastic surgeons operating simultaneously. Complications are infrequent and complete excision rates over 90%. Follow-up is limited but there have been no recurrences in the Edinburgh series so far. This approach is becoming more widespread in Europe, in North and South America, and in Australasia. The issue for many of these women is that even if they are treated by mastectomy and breast reconstruction to get symmetry, a contralateral procedure is required. Bilateral therapeutic mammaplasty can be performed without drains as a day patient or a short stay procedure and recovery is quicker, complications are fewer, and overall costs reduced compared with mastectomy and whole breast reconstruction.
The role of MRI in DCIS has recently been reviewed. The results of MRI in DCIS are similar to those of MRI in invasive cancer. MRI has a high false-positive rate and so cannot be relied upon with any certainty to delineate the extent of disease. DCIS is frequently over treated surgically as a consequence of MRI false-positives and overestimation of disease extent. Recurrence rates after breast conserving surgery are falling and for all women diagnosed with DCIS, a multidisciplinary approach is required with mastectomy being indicated only where breast conservation is not feasible or the patient herself choses this option.
Reduced Treatment for DCIS
There are now a number of national and international trials looking at reducing treatment for women with low risk DCIS. Data from the UK Sloane Project which includes over 10,000 cases showed that 66% of DCIS is high grade, 25% intermediate, and 9% low grade. Grading of DCIS by pathologists is inconsistent and many classify anything other than high grade as low risk DCIS. The UK trial of low risk DCIS study (LORIS) requires that all pathology is reviewed centrally and those deemed to have low grade, or DCIS at the boundary between low and intermediate grade, are eligible for entry into the study. Eligible patients with low risk DCIS are offered randomization to surgery, endocrine therapy, or observation alone. A recent US study has shown that the benefit of any surgery in low grade DCIS is very limited. Of 57,222 cases of DCIS, for low grade DCIS the 10-year breast cancer specific survival of the nonsurgery group was 98.8% and for the surgery group was 98.6% ( p = 0.95). Further prospective studies, such as the one ongoing in the UK, will provide better insight into the natural history of low risk DCIS diagnosed through breast screening treated by endocrine therapy or managed by observation alone. It should provide a better evidence base for identifying those women with DCIS who need excision with or without radiotherapy. Other similar trials of low grade DCIS are underway in Europe and in the USA.
Limiting Radiotherapy in Patients with DCIS
Numerous randomized trials have shown the benefits of whole breast radiotherapy in patients with DCIS following breast conserving surgery. The first trial was performed by the NSABP, but large trials have also been performed in Europe. The largest European study enrolled over 1000 patients with DCIS less than 5 cm in size, 50% of whom received radiotherapy after surgical excision. The 15-year cumulative incidence of DCIS recurrence in the surgery group was 14.9% compared to 7.5% in those patients who had both surgery and radiotherapy. The rates of development of invasive disease in the treated breast was 15.5% in the surgery-only group and 9.8% when surgery was combined with radiotherapy . The rate of DCIS or invasive cancer in the treated breast in this trial was thus over 1% per year even after wide excision and radiotherapy. It is perhaps surprising therefore that no survival advantage for radiotherapy was found, because it reduced the rate of invasive cancer development and the women who developed invasive cancer had a significantly worse survival compared with women who had DCIS recurrence or no recurrence at all. The majority of DCIS recurrences occurred within the first 5 years after treatment and the greatest effect of radiotherapy on reducing invasive recurrence was also in the first 5 years. The risks of developing any recurrence was however more or less continuous over 15 years of follow-up and this may explain the lack of any impact of radiotherapy on long-term outcome. The lack of a survival benefit for radiotherapy is clear even when all the randomized studies are combined. Since these initial trials, the rates of local recurrence in invasive cancer have fallen over time and there is now evidence that the rates of local recurrence following breast conservation for DCIS is also falling. Thus a 1% per year rate of recurrence in the European trial with surgery and radiotherapy is no longer seen and the rate is closer to 0.5% per year. The relevance of these older trials to current practice is thus not entirely clear.
Tamoxifen has been shown in randomized trials to reduce the rates of DCIS recurrence and invasive breast cancer development in patients with ER positive DCIS. Similarly aromatase inhibitors reduce recurrence rates. These agents are used widely in the US in ER positive DCIS but their use, at least in the UK, is not routine. Given the low rate of mortality from DCIS at 20 years and the morbidity of these treatments it is easy to understand why endocrine therapy use in DCIS is not in routine use in many centers.
An initial analysis of factors related to recurrence after DCIS treatment was undertaken in the European Organisation of Research and Treatment of Cancer (EORTC) study and showed that there was a higher rate of local recurrence in patients who presented symptomatically compared with being screen-detected. Those with close or positive versus clear margins, who had cribriform, solid, or comedo DCIS versus other types, had intermediate or high grade DCIS versus low grade DCIS, or were younger than 40 versus over 40 all had higher rates of recurrence. It is now common in Europe and North America for lower risk groups of patients with screen-detected DCIS to be treated by wide local excision alone and to add radiotherapy only for higher risk women. There have been some studies of wide excision alone that have shown reasonable rates of local control. The ECCOG-5194 study enrolled 670 women with grade 1 or 2 DCIS of noncomedo type of less than 2.5 cm or grade III and comedo DCIS <1 cm in size treated by excision alone without any radiotherapy. Women had to have a negative margin width of greater than 3 mm and tamoxifen treatment after surgery was optional. This study was published and reported a 5-year recurrence rate of 6.1% in those stratified as low or intermediate risk. The median tumor size of the low and intermediate grade DCIS was 6 mm and for the high grade DCIS it was 5 mm. In the high grade DCIS group even though they were relatively small lesions the recurrence rate was 15.3% at a median follow-up period of 6.7 years.
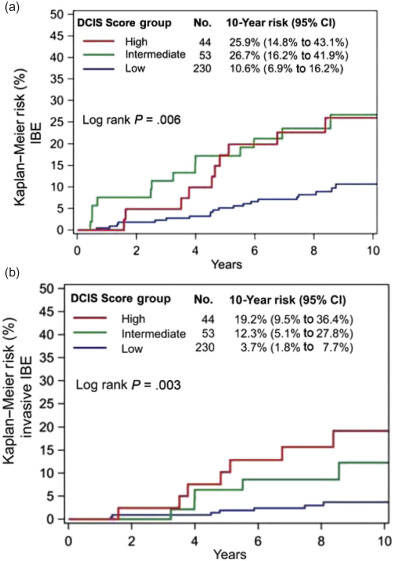
Following the success of tumor profiling of invasive cancers and the development of a 21 gene recurrence score for predicting in-breast tumor recurrence and breast cancer survival, a 12 gene DCIS score has been developed and been evaluated in two separate studies. These 12 genes, a subset of the 21 genes, include five proliferation genes, the progesterone receptor gene, and GSTM1 or glutathione S transferase, as well as five reference genes. Three groups of patients can be defined at low, intermediate, and high risk of recurrence. In the ECOG 5194 study the low risk group comprised 146 patients who had a 10-year risk of recurrence of 12%. In the 45 women in the intermediate group the 10-year risk was 24.5% and in the 36 patients in the high risk group the 10-year rate of recurrence was 27.3% ( Fig. 15.5a and 15.5b ). The invasive breast cancer rate was 5.1% in the low risk group, 8.9% in the intermediate group, and 19.1% in the high risk group. In a multivariate analysis the 12 gene recurrence score, tumor size, and postmenopausal status were significant predictors of recurrence in ECOG 5194. A validation study presented at San Antonio 2014 from Canada confirmed the utility of the DCIS recurrence score. Although traditionally pathologic features have been used to predict patients likely to get recurrence, this genomic based assay has the ability to identify a group of women who have a low risk of recurrence and may therefore avoid radiation after wide local excision.