Fig. 1
Age-standardized incidence of cancer (all sites) in different tropical areas in 2008
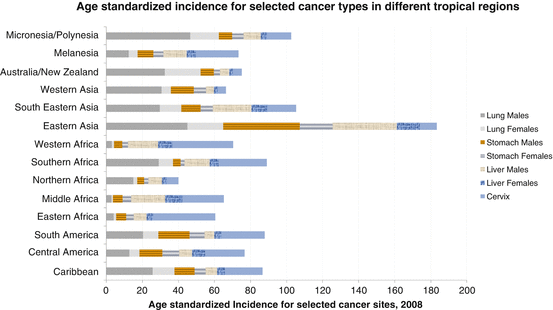
Fig. 2
Age-standardized incidence of selected types of cancer in different tropical areas in 2008
For countries with low or medium human development index, the highest incidences reported for cancer are by decreasing order lung, gastric, liver, female breast, colorectal, cervical, and esophageal. The standardized incidence for stomach, liver, cervical, and esophageal cancer is significantly higher in the low- and medium-human development index countries than in the high- or very high-human development index countries. For mortality, the main cancers for low and medium development index are lung, liver, gastric, esophageal, colorectal, breast, and cervical cancer. There again, as for incidence the standardized mortality for stomach, liver, cervical, and esophageal cancer is significantly higher in the low- and medium-human development index countries than in the high- or very high-human development index countries [2]. Recent trends extracted from the registries show a transition in low and medium human development index with prostate, breast, and colorectal cancers increasing since 1988, whereas cervical and gastric cancers tended to decrease. These trends however rely on the very rare registries in these countries.
In 2008, about 47 % of all cancer cases were from less developed areas (45 % in medium-human development index and +2 % in the low-development index areas which represented 6 % of the world population). However, GLOBOCAN projections suggest that at the 2030 horizon, assuming constant incidence rates and UN population growth estimates, the total number of cancer cases should increase 75 % mostly in the areas of lower human development index, where the number of cases should increase 93 %. Colorectal, breast, and prostate cancer should increase, whereas gastric and cervical cancer are expected to decrease [2].
Given these figures and projections, prevention and screening are of paramount importance to alleviate the burden of cancer in the tropics.
1 Primary Prevention
1.1 Infectious Causes of Cancer
1.2 Viruses
The human papillomavirus is the infectious agent that contributes to the highest number of cancer cases [5, 6]. HPV viruses cause cervical cancer, cancers of the anus, penis, vulva, and vagina and cancers of the oropharynx. Primary prophylaxis through vaccination against HPV 16 and 18 subtypes before entering sexual life could avoid about two out of three cervical cancer cases. However, it is still too expensive and logistically complex to implement for many tropical countries. Nevertheless, a study has shown that one or two vaccine doses may lead to sufficient immunity in Costa Rica [7]. If confirmed, this would reduce the costs and facilitate implementation in the most isolated areas to achieve sufficient coverage. Delaying sexual activity and reducing the number of sex partners and unprotected intercourse could contribute to reduce cervical cancer incidence. This is part of measures to reduce the burden of sexually transmitted infections and early pregnancies and thus should be easily integrated in general health promotion. Cervical cancer is an AIDS-defining illness in HIV-infected persons. Given the huge burden of HIV throughout the tropics, HIV prevention, early testing for HIV, and access to antiretroviral treatments are likely to reduce the incidence of cancers associated with HPV.
Hepatitis B viruses are responsible for 60 % of all primary cancers of the liver [5]. The prevalence of hepatitis B chronic infection is still very high in Africa and South East Asia, with up to 10 % of the population being chronically infected. Transmission may occur at different ages, from mother to child, between children during childhood, by sexual relations, or through the parenteral route. Primary prophylaxis opportunities thus reflect transmission risks. However, the most cost-effective intervention in countries of high prevalence remains routine mass vaccination with an anti-HBV vaccine, as recommended since 1992, and early vaccination of newborns from chronically infected mothers. Although most countries adopted this recommendation, vaccine coverage is still suboptimal in highly endemic areas. Moreover, a substantial proportion of infants did not receive the first dose within 24 h after birth to avoid transmission of hepatitis B from chronically infected mothers.
Hepatitis C viruses are responsible for about a quarter of all primary cancers of the liver worldwide. In Africa, it is estimated to cause up to 40 % of hepatocarcinoma, in Japan 36 %. Transmission is mostly parenteral and thus screening of blood donors and improvements in sterilization techniques for medical and nonmedical techniques (body adornments) can reduce the prevalence of chronic hepatitis C and hepatocarcinoma [5, 8]. There is no vaccine at the moment.
The human T-cell leukemia virus 1 infection is complicated with T-cell leukemia/lymphoma in 2–5 % of the cases, notably when the infection was acquired from mother to child [9]. The tropical areas with the highest prevalence are the Caribbean, South and Central America, Melanesia, and Central Africa [5]. Although in regions of higher development index, such as Japan, prevention of mother to child transmission through breast feeding avoidance has been successful, it is not applicable in parts of the world with low development index where the burden of diarrheal diseases and malnutrition may end up being far greater than that of T-cell leukemia/lymphoma. Screening of blood donors also may help reduce the prevalence of HTLV1 but most T-cell leukemia/lymphoma cases concern persons infected during infancy.
Other infections such as the Epstein-Barr virus, in conjunction with malaria, may result in Burkitt’s lymphoma or nasopharyngeal carcinomas. However, most persons are infected by EBV during childhood and specific primary prophylaxis measures against these cancers do not exist. The HHV8 virus is related to Kaposi’s disease and Castleman’s disease, notably among HIV-infected patients. Apart from antiretroviral to avoid immunosuppression, no specific primary prophylaxis exists for these tumors. HIV is also associated with an increased incidence of various cancers, notably in the most severely immunocompromised patients. There again, antiretrovirals to maintain immunity may contribute in preventing cancer.
1.3 Bacteria
Helicobacter pylori infects up to 90 % of the populations in the tropical areas. Some will develop ulcers, chronic gastritis, and rarely gastric cancer. Although, once diagnosed, H. pylori may be eradicated by antibiotics, success is not constant and reinfection may occur. General socioeconomic development, improvement of hygiene levels, increased use of refrigeration, increased availability of fresh fruits and vegetables, decreased reliance on salted and preserved foods, and increased availability of antibiotics may decrease H. pylori colonization rates in the population and ultimately reduce the burden of gastric cancer.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree