Approximately 50% of adrenocortical carcinomas (ACCs) hypersecrete adrenal steroids. When secretory, ACCs are typically plurihormonal—most commonly glucocorticoids and adrenal androgens. Rarely ACCs secrete a single steroid in excess. The case presented herein is an example of a patient with a pure aldosterone-producing ACC, a subtype of ACC that may be associated with a more indolent clinical course.
Case Report
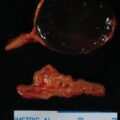
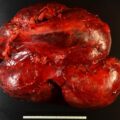
In the year 2000, this 51-year-old woman came to Mayo Clinic for refractory hypertension and hypokalemia. She had been diagnosed with hypertension and hypokalemia 23 years previously when her blood pressure was 170/115 mmHg. Body computed tomography (CT) was available at only a few medical centers in the United States in 1977. She lived outside of the United States and, instead of CT-based imaging, she underwent adrenal venography, which demonstrated asymmetric adrenal size and led to left adrenalectomy. The pathology report indicated the adrenal gland was in two pieces and weighed 3.3 g and no tumor was seen. Hypertension and hypokalemia persisted following the operation, and she was treated with a mineralocorticoid receptor antagonist (spironolactone 100 mg daily) and a β-adrenergic blocker (propranolol 80 mg daily). In 1995, her blood pressure was 230/110 mmHg and serum potassium was 2.0 mEq/L on the same two medications. Plasma aldosterone concentration (PAC) was markedly elevated and plasma renin activity (PRA) was suppressed. An abdominal CT scan showed a 4-cm left adrenal mass and she underwent her second surgery, which was an open left adrenalectomy removing a 4.5 × 4.0 × 4.0–cm tumor that weighed 31 g. Postoperatively her blood pressure and serum potassium level were normal for 3 years. In 1998, she had recurrent primary aldosteronism (PA) and she was treated with spironolactone. In 2000, due to progressive hypertension and hypokalemia despite 300 mg of spironolactone daily she underwent right adrenalectomy and a 9.2-g adrenal gland without an adenoma was found. Two months later, in April 2000, at 51 years of age she came to Mayo Clinic for the first time.
She had refractory hypertension and hypokalemia. Her medications included propranolol 160 mg daily, spironolactone 200 mg daily, fosinopril 40 mg daily, cortisone acetate 25 mg twice daily, and potassium chloride 80 mEq daily. Except for the hypertension and symptoms related to hypokalemia, she felt reasonably well. There were no signs or symptoms of glucocorticoid or androgen excess.
INVESTIGATIONS
Laboratory studies completed in April 2000 are shown in Table 29.1 . Her blood pressure averaged 160/100 mmHg on a 6-hour ambulatory blood pressure monitor. She had positive case detection testing for PA with a plasma aldosterone concentration (PAC) >10 ng/dL and the plasma renin activity (PRA) was <1.0 ng/mL per hour. In addition, PA was confirmed because when a patient has spontaneous hypokalemia and the PAC >20 ng/dL, there are no other differential diagnostic possibilities beyond PA. , Thus formal confirmatory testing with oral sodium loading or a saline infusion test was not needed for this patient. The 24-hour urine for 17-ketosteroids was normal and indicated that the patient was not producing excess adrenal androgens (see Table 29.1 ). In addition, the 24-hour urine for ketogenic steroids and cortisol was normal. Thus the patient had a pure aldosterone-secreting neoplasm.
| Biochemical Test | Result | Reference Range |
| Sodium, mmol/L | 143 | 135–145 |
| Potassium, mmol/L | 3.4 | 3.6–5.2 |
| Creatinine, mg/dL | 1.3 | 0.8–1.3 |
| Aldosterone, ng/dL | 116 | ≤21 ng/dL |
| Plasma renin activity ng/mL per hour | <0.6 | ≤0.6–3 |
| 24-Hour urine 17-ketosteroids, mg | 2.3 | 4–17 |
| 24-Hour urine ketogenic steroids, mg | 7 | 2–12 |
| 24-Hour urine free cortisol, mcg | 61.8 | <108 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree