HCP: “You have been successful in losing weight in the past but like many patients, weight regain seems to be an issue.”
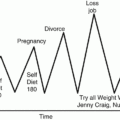
Patient: “Losing weight is the easy part! The hard part is keeping it off. I am frustrated and don’t want to live the rest of my life on a diet. I eat healthy food, but the weight comes back anyway.”
HCP: “You haven’t tried medications. Some of our newer medications have been extensively studied and are safe. Taking one can make it more likely that you will lose significant weight—5% or 10%, but importantly, as long as you take the medication, the more likely you are to sustain that hard-won weight loss. What is your initial reaction to taking a medication?”
Patient: “Aren’t medications cheating? I guess I want to hear more….”
HCP: “These medications don’t work on their own. They reinforce your body’s biology and help with hunger and fullness. There is one that doesn’t affect appetite, but helps you stay on a low-fat diet. If you are not making an effort with diet and increased physical activity, you will not get optimal results. I am going to give you a handout that describes the medications (See additional resources, below, for a handout, ‘Medications for Weight Loss’) and I want you to go home and do some internet research. The meds all have slightly different profiles. And you will need to check with your insurance company to see which ones you have coverage for. I will see you back, answer your questions and we can decide on the one that is right for you. When we choose one, we will need to monitor you monthly over the first 3 months to make sure it is working and to deal with side effects. How does this sound?”
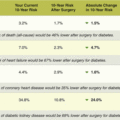
Patient: “I have a friend at work who lost 40 pounds when her diabetes medications were changed, so I know medications can make a difference in weight. It sounds like a good plan to me. Can we meet in a month?”
The 2013 American Heart Association/American College of Cardiology/The Obesity Society (AHA/ACC/TOS) Guidelines for the Management of Overweight and Obesity in Adults2 recommends that patients with obesity or overweight with cardiovascular risk factors should be counseled on diet, physical activity, and other lifestyle modifications. Unfortunately, behavioral interventions alone do not lead to sustained weight loss for many patients because adaptive physiologic responses reduce energy expenditure and increase appetite. Patients have measurable changes in resting metabolic rate, burn fewer calories with the same exercise, and have more hunger and cravings and reduced satiety at a lower weight. These phenomena, known as metabolic adaptation or adaptive thermogenesis, counteract weight loss and lead to weight regain.
Healthcare professionals should consider prescribing AOMs along with diet and physical activity to help patients achieve health goals through weight loss, especially when comorbidities are compromising health.3,4,5
The Endocrine Society’s systematic evidence review of common medications that promote weight gain and use of alternative approaches is a valuable resource; this knowledge base should be a standard of care for adult HCPs. Wherever possible, for patients with overweight and obesity, using medications that are weight neutral or associated with weight loss is advisable. See Table 8.1.
The rationale for using AOMs is to help achieve and sustain more weight loss that can be achieved with lifestyle intervention alone, thus benefitting the health of patients who need to lose weight for health reasons.
Prescribers need to be knowledgeable about ALL medications, because there is no one medication that works in every patient. If patients do not respond in the first 12 to 16 weeks with at least 4% to 5% weight loss, the drug should be discontinued, and another medication tried.
Obesity is a chronic disease. AOMs should be used long term, just like antihypertensive and lipid-lowering agents.
TABLE 8.1 Current Antiobesity Medications Approved in the United States and How They Worka | ||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||
are unsuccessful in losing weight with lifestyle changes alone, or
need to lose 10% or more body weight to achieve health benefits, or
need to maintain weight loss (regardless of the methods used to achieve initial weight loss).
AHEAD. In primary care efforts at lifestyle intervention, average weight loss is on the order of 0.9 to 2.0 kg in 6 months.9 For the many patients who are unable to achieve and sustain weight loss with lifestyle intervention alone, AOMs are needed to help achieve enough weight loss to produce improved health benefits. Additionally, for patients with more severe complications of obesity, such as type 2 diabetes (T2D) or obstructive sleep apnea, weight loss of >10% is needed to maximize health benefits. Despite the limitations of lifestyle intervention for weight loss, high-intensity behavioral treatment of obesity (≥14 visits in the first 6 months, followed by at least monthly contact for maintenance of weight loss) is recommended as a standard of care for treatment of obesity and should produce a 5% to 10% weight loss during the first 6 months of treatment. Several randomized trials using different medications have reported that the combination of intensive behavioral treatment and pharmacotherapy is additive in terms of weight loss.
for a description of contraindications and safety issues with AOMs. Choosing a medication requires matching the patient profile to the medication profile. If patients describe difficulty controlling their appetite, then common sense dictates that one of the medications that affect appetite should be chosen, rather than orlistat. Also, one should consider dual benefits: orlistat can enforce a low-fat diet and lower plasma LDL cholesterol.15 Liraglutide 3.0 mg can lower glycemic measures and, at a dose of 1.8 mg in patients with T2D, is associated with reduction in cardiovascular events in addition to affecting appetite and body weight.16 See Table 8.4 for a description of dual benefits of AOMs.
TABLE 8.2 Antiobesity Medications Approved in the United States: Dosing and Route of Administration; Efficacy (Proportion of Treated Individuals Who Achieve >5% and >10% During Phase 3 Clinical Trials)a | ||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree