supports matching behavioral counseling strategies to different stages of change.6 For example, patients who are not interested in actively working on their weight would be identified in the precontemplation stage of change. For these patients, simply mentioning that weight loss may help them achieve improved health and that you are there to assist when they are ready is sufficient. In contrast, some patients present in the preparation stage, having already downloaded a smart phone app to track their diet and joined a health club. These patients are ready and interested in receiving further guidance on how to take action to lose weight.
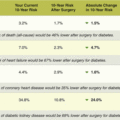
dinner options for the week. A link to examples of meal plans is available in the Practical Resources section of this chapter. In summary, the HCP should recommend that the patient monitor diet as a first step to weight loss (“Ms. Jones, I recommend that you start recording all food and liquid intake and aim for 1,200 cal/day.”) For the clinician, it is important to keep in mind that patients often underestimate their calorie intake. Thus, the patient who is struggling with calorie intake despite a low-calorie count can be encouraged to lower their target by 200 to 300 kcal/day.
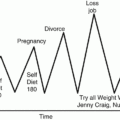
heads home after a long day and decides not to stop for groceries, even though she does not know what she will make for dinner (6). She opens the refrigerator and sees a few slices of leftover cake (7). Very hungry, she eats the cake while surfing the web, telling herself that she needs something delicious to make herself feel better (8, 9). The patient could have broken the chain by eating a go-to frozen meal option that she knows fits within her calorie goal, calling a friend instead of turning to the cake for comfort, or saving a slice of cake for after dinner and putting the rest in the freezer so it requires defrosting. The patient eating the cake might lead to negative self-talk or drastic recovery measures like skipping meals the next day to make up for calories, ultimately leading to feeling very hungry at dinner and overeating (10-13). Breaking chain links here could occur through meal planning for the following day, as skipping meals would only make one feel hungrier later. Ideally, an intervention should occur as early as possible in the chain. However, providing multiple strategies to break the link in several places is beneficial as patients can get an idea of what would be the “weakest link” for them to break.
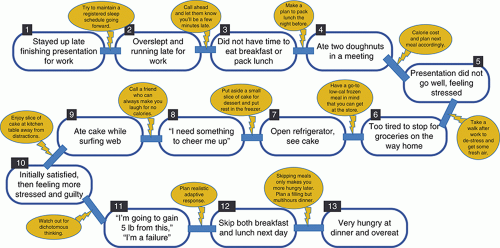 FIGURE 7.1 Example of a behavioral chain. Each chain represents a process that can lead to unhealthy eating behaviors. Examples of interventions are in yellow bubbles. |
brainstorm potential solutions; (3) consider the pros and cons of each option; (4) choose a solution and develop plans for implementing it; and (5) test the efficacy of the strategy for a specific period of time. The process can be repeated if the problem was not successfully solved.
TABLE 7.1 Problem-Solving Steps | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
or skipping exercise for a week. A relapse is a return to frequent problematic weight control behaviors and is associated with weight regain. It is essential that patients learn to reverse small weight gains or lapses as they occur. These instances can be viewed as opportunities to learn and get back on track. Using relapse prevention techniques, HCPs teach patients to identify and describe potentially risky situations in which overeating or underexercising may occur. Patients and providers discuss strategies and step-by-step plans to flexibly manage these situations. For example, a patient may identify a high-risk situation as going out for lunch with coworkers. The HCP and patient may discuss several strategies such as bringing lunch, suggesting a healthier restaurant, or making sure to look at the menu beforehand to pick a lower calorie lunch option and then sticking with that choice. Discussions should also include scenarios in which the patient does have a lapse, say by going to lunch but consuming more calories than anticipated. Patients should be encouraged to spot the problem early and to restart self-monitoring (if they have stopped) and other weight control behaviors, to ask for social support, and to identify and address the trigger of the setback.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree