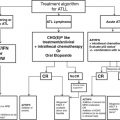
Fig. 1
Proposed management for patients with glioblastoma
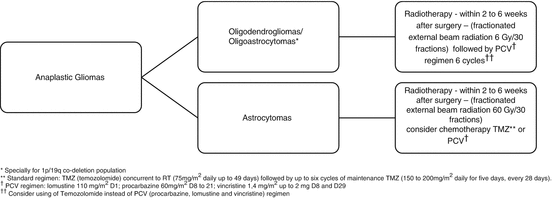
Fig. 2
Proposed management for anaplastic gliomas in patients with good performance status after maximal, safe resection of the tumor with preservation of neurologic function
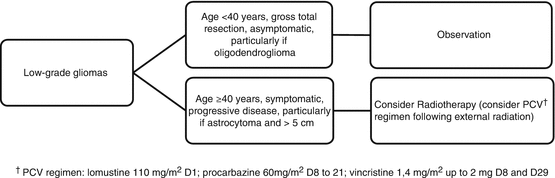
Fig. 3
Proposed management for patients with low-grade glioma
In the recurrent setting, re-operation and re-irradiation may be the primary option since chemotherapeutic agents have proven modest activity. Thus, the therapeutic strategy must be tailored individually. Antiangiogenic therapy, such as the anti-VEGF monoclonal antibody bevacizumab, has been used due to its dramatic radiological response and improved progression-free survival [26]. However, the short-lasting response, the absence of a clear benefit in OS, the potential for inducing changes in the biological behavior of the tumor resulting in a more invasive and aggressive tumor, and its excessive cost make this approach still debatable, particularly in under developing countries.
Age, performance status, and extent of resection are important prognostic factors for glioma patients. For instance, elderly patients are expected to present shorter OS and higher treatment-related toxicity. In this age group, treatment options include best supportive care, short course radiotherapy, TMZ alone (especially in patients with MGMT methylated) [27], and chemoradiation. However, it is usually recommended that treatment decisions should not be based exclusively on chronological age but mostly on the patient’s performance status [28].
References
1.
Stupp R, Hegi ME, Mason WP et al (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10:459–466. doi:10.1016/S1470-2045(09)70025-7 CrossRefPubMed
2.
Darefsky AS, King JT, Dubrow R (2012) Adult glioblastoma multiforme survival in the temozolomide era: a population-based analysis of Surveillance, Epidemiology, and End Results registries. Cancer 118:2163–2172. doi:10.1002/cncr.26494 PubMedCentralCrossRefPubMed
3.
Loureiro L, Pontes LB, Callegaro-Fiho D et al (2014) Initial care and outcome of glioblastoma multiforme patients in 2 diverse health care scenarios in Brazil: does public versus private health care matter? Neuro Oncol 16:999–1005PubMedCentralCrossRefPubMed
4.
Lorenzoni J, Torrico A, Villanueva P et al (2008) Surgery for high-grade gliomas in a developing country: survival estimation using a simple stratification system. Surg Neurol 70:591–597. doi:10.1016/j.surneu.2007.08.004, discussion 597CrossRefPubMed
5.
Idowu OE, Apemiye RA (2009) Delay in presentation and diagnosis of adult primary intracranial neoplasms in a tropical teaching hospital: a pilot study. Int J Surg 7:396–398. doi:10.1016/j.ijsu.2009.07.001 CrossRefPubMed
6.
Lynch JC, Welling L, Escosteguy C et al (2013) Socioeconomic and educational factors interference in the prognosis for glioblastoma multiform. Br J Cancer 27(1):80–83. doi:10.3109/02688697.2012.709551
7.
Paravati AJ, Heron DE, Landsittel D et al (2011) Radiotherapy and temozolomide for newly diagnosed glioblastoma and anaplastic astrocytoma: validation of Radiation Therapy Oncology Group-Recursive Partitioning Analysis in the IMRT and temozolomide era. J Neurooncol 104:339–349. doi:10.1007/s11060-010-0499-8 PubMedCentralCrossRefPubMed
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree