(1)
Department of Surgery, Dar A lAlafia Medical Company, Qatif, Saudi Arabia
8.1 Introduction
One of the common manifestations of sickle cell anemia is vaso-occlusive crises which affect virtually all patients with sickle cell anemia.
This starts early, often beginning in late infancy and characterized by recurrent attacks that continue throughout life.
The majority of these attacks are self-limiting with full recovery and no further complications.
This however is not the case always, and sometimes these attacks can be complicated by joint effusion or bone infarction (avascular necrosis).
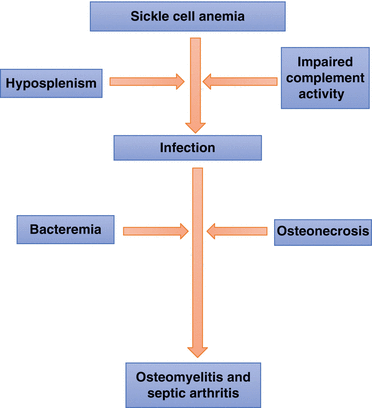
The presence of infarcted or necrotic bone in these patients makes them susceptible to develop osteomyelitis. This is predisposed to by the increased susceptibility of these patients to infections as a result of hyposplenism and impaired complement activity.
8.2 Acute Vaso-occlusive Crisis
Sickle cell anemia is characterized by periods of remissions and exacerbations. These periods of exacerbations are called crisis.
Bone and joint vaso-occlusive crisis is the most common manifestations of sickle cell anemia and a major cause of frequent emergency room visits and hospitalization.
It is also called painful crisis.
This commonly occurs in the bone marrow or epiphyses of the bones leading to bone marrow infarction.
This can affect any part of the skeleton, but there is a predilection for the long bones.
Pain caused by vaso-occlusive crisis may occur as often as every week, or these patients may go without any attacks for several months or sometimes years.
As a result of these repeated attacks, many patients with SCA develop long-term consequences including avascular necrosis of the femoral heads, avascular necrosis of the humoral head, or collapsed vertebral bodies.
The frequency and severity of these vaso-occlusive crises are variable. It has been suggested that concomitant alpha thalassemia trait and higher hemoglobin S levels in patients with sickle cell anemia appear to be associated with more frequent attacks of vaso-occlusive crisis, while high HbF levels appear to have a protective effect with less frequent and milder attacks.
Vaso-occlusive crisis can affect any bony structure in the body but typically occurs in the long bones. The commonest sites are:
The tibia/fibula (25–30 %)
The femur (20–25 %)
The radius, ulna, and humorous (20–38 %)
Pathogenesis:
The exact pathogenesis of vaso-occlusive crisis is not known and several factors may be involved.
In the bone marrow, there is slow progression of red blood cells through the bone marrow sinusoids and capillary beds. This together with the relatively hypoxic tissue environment increases the risk for RBCs sickling.
As a result, there will be activation and adhesion of leukocytes, platelets, and endothelial cells as well as hemoglobin S-containing erythrocytes leading to microvascular occlusion, impaired blood flow, regional hypoxia, and ischemia.
The inflammatory response to ischemia and infarction leads to pain in the affected area and surrounding tissues.
Clinical features:
The clinical presentation of a vaso-occlusive crisis is variable in terms of severity and duration.
The usual presentation includes:
Pain along one of the bony parts of the skeleton.
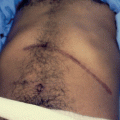
The pain is usually deep seated and sometimes very severe excruciating making the patient scream and cry for help (Fig. 8.1).
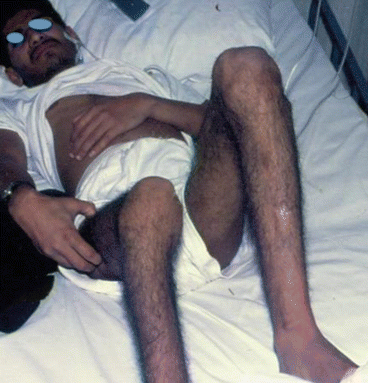
Fig. 8.1
A clinical photograph showing a patient with sickle cell anemia during a severe attack of vaso-occlusive crisis. Note the facial expressions indicating severe pain
The pain may be localized to one or more areas of the skeleton.
Others may have only mild pain that does not interfere with their daily normal activity.
The pain may be associated with localized swelling, erythema, and tenderness.
The pain may be associated with a low-grade fever and the affected area is warm.
These attacks are usually self-limiting and most patients recover with no further complications.
When these attacks affect the epiphyses of the bones, there may be an associated effusion of the adjacent joint.
It is important to differentiate this from septic arthritis.
Affection and infarction of the vertebral bone marrow lead to collapse of the vertebrae with a typical “fish mouth” appearance.
Diagnosis and investigations:
The diagnosis of a painful vaso-occlusive crisis is predominantly a clinical one.
The laboratory investigations during an acute vaso-occlusive crisis are usually normal apart from a mild leukocytosis.
It is important to differentiate acute vaso-occlusive crisis from osteomyelitis.
Febrile patients (38 °C) should have a complete blood count, ESR, C-reactive proteins, and blood cultures to evaluate for the possibility of osteomyelitis.
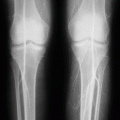
Plain radiographs initially are usually normal and do not show abnormalities, but subsequently and as a result of necrosis and remodeling, they may show areas of ill-defined translucency followed by arc-like subchondral and intramedullary lucent areas and patchy sclerosis and increased density and deformities in the vertebra of the spine.
The most useful investigation is a radioisotope bone scan using a combination of 99mtechnecium (Tc)-labeled sulfur colloid and 99MTc-diphosphonate which reliably detect areas of infarction. The bone scans with technetium-99 m methylene diphosphonate may show increased uptake, whereas a bone scan with technetium sulfur colloid often shows decreased or absent uptake in the affected area. The bone scan is however unreliable in distinguishing infarction from osteomyelitis.
Magnetic resonance imaging (MRI) is a very sensitive imaging technique for detecting bone and bone marrow infarction, but the changes seen are often difficult to distinguish from those seen in osteomyelitis.
MRI should be reserved for investigating those patients whose symptoms fail to settle with conventional management and/or where there is a high suspicion of osteomyelitis.
Treatment:
Simple and mild attacks of vaso-occlusive crisis can be treated at home, and patients with SCA should be educated how to do this.
This includes:
Pain control using acetaminophen, ibuprofen, or acetaminophen with codeine depending on the severity of pain
Bed rest
Oral hydration fluids
Warm pads
Moderate and sever attacks require treatment in the hospital emergency room and sometimes hospitalization.
Pain control is the main issue in this regard which should be prompt, and pain medications should never be withheld from these patients.
These patients should be treated in centers specialized in sickle cell anemia. To avoid delay in treating these patients in emergency rooms, there are specialized dedicated centers with experienced nurses who can provide immediate care for these patients.
The treatment of moderate and severe attacks includes:
Hydration with oral or intravenous fluids.
Warm pads to the affected area or areas.
Analgesia and anti-inflammatory medications.
Severe attacks may necessitate the use of continuous infusion or regularly scheduled opioid dosing and patient-controlled analgesia.
It is also important to use these opioids carefully as an overdose may lead to respiratory depression.
Oxygen supplementation has no role in patients with a normal oxygen saturation or whose oxygen saturation is at that individual’s baseline.
Packed RBC transfusion is given only to those with associated symptomatic anemia.
Hydroxyurea was shown to reduce the frequency of vaso-occlusive crisis, and it is used in children and adults with severe or recurrent vaso-occlusive crisis.
8.3 Osteomyelitis and Septic Arthritis
Patients with sickle cell anemia are known to be susceptible to infections at various sites.
This is predisposed to by hyposplenism and impaired complement activity.
In the presence of infarcted or necrotic bone and bacteremia, these areas can be infected causing osteomyelitis and septic arthritis.
Patients with sickle cell anemia have an increased incidence of septic arthritis and osteomyelitis as compared to the general population.
The association between osteonecrosis and septic arthritis is well documented, but there are reports of septic arthritis without well-documented osteonecrosis.
In general, osteomyelitis occurs in 18 %, while septic arthritis occurs in 7 % of patients with sickle cell anemia (Figs. 8.2 and 8.3).
Osteomyelitis most commonly affects the diaphysis of long bones.
There is an increased incidence of Salmonella osteomyelitis in patients with sickle cell anemia, where it is believed to be the most common pathogen causing osteomyelitis and septic arthritis followed by S. aureus.
Early diagnosis of osteomyelitis and septic arthritis is important to avoid chronicity and irreversible joint damage.
It is also important to be cautious as vaso-occlusive crisis affecting the bones or close to the articular surfaces may lead to a similar clinical picture to osteomyelitis and septic arthritis.
Clinical features:
Osteomyelitis usually presents with:
Pain at the site of infection.
Swelling.
Tenderness over the affected area.
Erythema and redness.
Most patients also have fever.
Sometimes there is an associated joint effusion if the infection is close to a joint.
Difficulty in walking in those with osteomyelitis affecting the lower limb.
These signs and symptoms are similar to those found in vaso-occlusive crises, making the distinction between a painful crisis and osteomyelitis extremely difficult.
The most common sites of osteomyelitis are:
The femur
The tibia
The humerus
Osteomyelitis may not be suspected until the signs and symptoms of a typical painful crisis have failed to resolve after 1–2 weeks of standard therapy.
Patients with septic arthritis usually present with:
Pain at the site of involved joint and adjacent bones
Fever
An associated effusion in the affected joint
Septic arthritis can affect any joint but there is a predilection for large joints and lower extremities.
The distribution of septic arthritis is as follows:
The hip joint (40 %)
The knee joint (25 %)
The elbow joint (20 %)
The shoulder joint (10 %)
The ankle joint (0.5 %)
The diagnosis of septic arthritis must be made early to avoid subsequent joint destruction (Fig. 8.4).
Joint fluids should be aspirated for bacteriological evaluations and the antibiotics used should be adjusted accordingly.
The microorganisms causing septic arthritis are generally the same as in osteomyelitis.
Salmonella sp. are the most common organisms causing septic arthritis in patients with sickle cell anemia.
Other organisms reported include:
Klebsiella pneumoniae
Staphylococcus aureus
Pneumococcus sp.
Causative organisms:
Osteomyelitis in patients with sickle cell anemia is different than that in normal adults in terms of causative organisms.
The most common cause of osteomyelitis in sickle cell anemia is Salmonella (Salmonella typhimurium, Salmonella enteritidis, Salmonella choleraesuis, and Salmonella paratyphi B), followed by Staphylococcus aureus and Gram-negative enteric bacilli.
This is important when considering antibiotic coverage initially before the results of cultures.
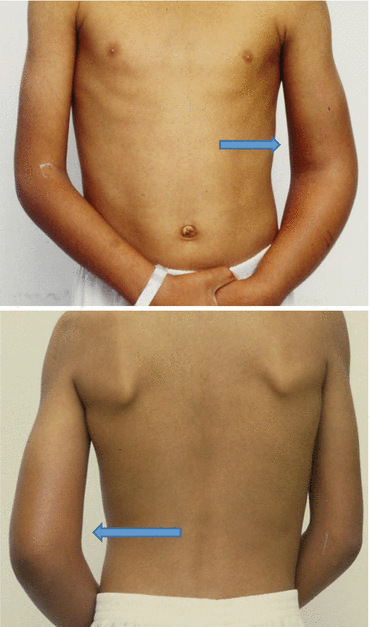
Figs. 8.2 and 8.3
Clinical photographs showing septic arthritis of the elbow. Note the swelling and redness of the elbow joint
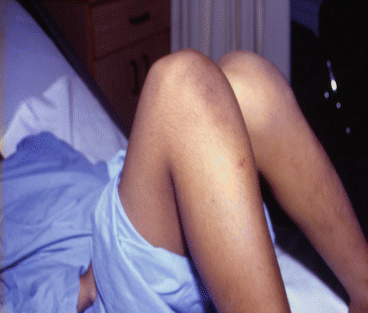
Fig. 8.4
A clinical photograph showing septic arthritis of the knee joint
Causes of Osteomyelitis and Septic Arthritis Patients with Sickle Cell Anemia
1.
Salmonella typhimurium
2.




Salmonella enteritidis
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree