IODINE-INDUCED GOITER AND HYPOTHYROIDISM
Part of “CHAPTER 37 – ADVERSE EFFECTS OF IODIDE“
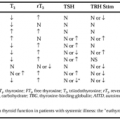
Iodine-induced goiter was first reported in 1938; since then, >200 cases have been described. Of 154 cases reviewed, euthyroid goiter accounted for 39%, hypothyroidism without goiter for 17%, and hypothyroidism with goiter for the remaining cases.11 Such goiters, often associated with hypothyroidism, have been reported sporadically in the United States for many years and more commonly in Europe. In the past, the problem was seen most often after the use of iodide-containing expectorants. Amiodarone use has been associated with hypothyroidism and, in several cases, goiter has developed with benziodarone use. The high incidence of antithyroidal antibodies in patients with goiter development suggests that these
patients have underlying Hashimoto thyroiditis with abnormal hormone synthesis and a unique sensitivity to the effects of iodine.29 It may be that iodide-induced goiter or hypothyroidism occurs only in the presence of thyroid dysfunction. The true incidence of goiter in patients exposed to iodides is unknown. The incidence is higher in women than in men, and most patients have received large amounts of iodide (several milligrams to >1 g) daily for long periods.3 Goiter also has been seen after therapy with small amounts of iodide, however.12 The interval from the institution of therapy with iodine-containing compounds to the appearance of goiter or hypothyroidism varies widely, from a few months to several years.
patients have underlying Hashimoto thyroiditis with abnormal hormone synthesis and a unique sensitivity to the effects of iodine.29 It may be that iodide-induced goiter or hypothyroidism occurs only in the presence of thyroid dysfunction. The true incidence of goiter in patients exposed to iodides is unknown. The incidence is higher in women than in men, and most patients have received large amounts of iodide (several milligrams to >1 g) daily for long periods.3 Goiter also has been seen after therapy with small amounts of iodide, however.12 The interval from the institution of therapy with iodine-containing compounds to the appearance of goiter or hypothyroidism varies widely, from a few months to several years.
EFFECTS DURING PREGNANCY
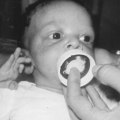
Iodides cross the placenta easily; therefore, one should expect that goiter may be seen in neonates whose mothers received iodide-containing drugs during pregnancy. Congenital goiter and neonatal hypothyroidism resulting from long-term maternal iodide use are rare and have similar manifestations as in adults, but the consequences for infants are severe and include asphyxiation from tracheal compression and potential mental retardation if the condition is not treated. Death from asphyxiation was reported in 8 of 22 infants born with goiter.11 Surgical intervention may be warranted in selected cases, although the goiters resolve over a few months in asymptomatic infants. Generally, the mothers have had no manifestations of goiter or hypothyroidism.
NEONATAL PERIOD
The frequency or magnitude of the problem of neonatal iodide-induced goiter or hypothyroidism is unknown. Iodides are secreted into breast milk, and hypothyroidism or goiter may be seen in breast-fed infants of mothers chronically exposed to high doses of iodides.11,30 Prenatal vitamins usually contain 150 μg of iodine, which should not constitute a hazard but does pose an additional risk in pregnant women who already are ingesting iodides from other sources. In an intensive care unit setting, within 1 month after the extensive topical use of 1% iodine and 3.9% iodine solutions (Polyvidone) for 4 to 8 days, goiter and hypothyroidism developed in 5 of 30 neonates.31 The affected infants had significantly increased ioduria, whereas the other infants did not, which suggests a difference in skin permeability. In all cases, the goiter resolved after brief therapy with thyroid hormone, and neither hypothyroidism nor goiter recurred subsequently. These observations suggest inadequate or undeveloped ability of the neonatal thyroid gland to “autoregulate” or control iodide uptake and binding, resulting in saturation and suppression of hormone synthesis and secretion.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree