Introduction
Chemotherapy can affect skin in various ways, and several chemotherapeutic agents have been linked to distinctive cutaneous side effects. Although these side effects are rarely life-threatening, they can cause considerable distress and discomfort to patients (alopecia, hyperpigmentation), negatively impacting their quality of life and sometimes leading to interruptions of treatment. Occasionally, cutaneous reactions may be associated with more serious systemic toxicity. Characteristics of these adverse events vary, depending on the chemotherapeutic drug and type of cancer. Some dermatological adverse effects, such as phototoxicity, can occur when chemotherapy drugs are combined with radiotherapy. Recognition of these reactions is important to both dermatologists and oncologists to allow for prompt initiation of appropriate management and for maintaining uninterrupted administration of chemotherapy. In this chapter, we discuss the specific dermatological complications associated with various chemotherapeutic agents and describe the general principles for the diagnosis and treatment of these complications.
Chemotherapy-Induced Alopecia
- ■
Hair growth cycle: The hair growth cycle consists of three distinct phases: the growth phase (anagen phase), the deconstruction phase (catagen phase) and the resting phase (telogen phase). Chemotherapy treatment can often result in alopecia affecting the scalp and other body hair attributed to the fact that most hair follicles are in the anagen phase, and chemotherapy can damage these actively dividing cells.
- ■
Chemotherapy-induced alopecia (CIA) : CIA is a distressing side effect common tonumerous treatment regimens in oncology. It has a negative influence on body image, psychosocial well‐being, and may sometimes influence treatment decisions. A number of chemotherapy agents have been reported to cause CIA, as listed in Table 9.1 . Various classes of drugs, including alkylating agents, anthracyclines, antimetabolites, antitumor antibiotics, vinca alkaloids, and taxanes are known to cause alopecia more readily. Alopecia following chemotherapy occurs in two distinct patterns: anagen effluvium and telegenic effluvium.
- ■
Anagen effluvium: Anagen effluvium is the most commonly observed pattern. It occurs due to chemotherapeutic drugs targeting the active hair follicle in the anagen phase, inducing premature catagen transformation. This results in weakening of the hair shaft, making it prone to breakage and stops hair shaft formation. It presents as complete destruction of hair, thinning of hair, or hair becoming brittle. Because approximately 70% to 85% of hairs of an adult scalp are in anagen phase of hair growth, anagen effluvium can be quite distressing to patients.
- ■
Telegen effluvium: Telegen effluvium occurs due to malnutrition, fever, stress, and emotional distress following chemotherapy and presents as global hair loss.
TABLE 9.1
Chemotherapy Agents That Cause Alopecia and Their Severity
Occurrence
Severe Alopecia
Moderate Alopecia
Mild Alopecia
Frequent
Doxorubicin
Daunorubicin
Cyclophosphamide
Ifosfamide
Docetaxel
Paclitaxel
Etoposide
Busulphan
Methotrexate
Mechlorethamine
Bleomycin
Cisplatin
Infrequent
Vincristine
Vinblastine
Vinorelbine
Mitomycin
Actinomycin
5-Fluorouracil
Hydroxyurea
- ■
- ■
CIA usually begins 2 to 4 weeks after the start of therapy, commonly at 7 to 10 days and peaks at around 1 to 2 months. Hair loss occurs in a diffuse or patchy pattern, depending on the distribution of hairs in the active anagen growth phase. Diffuse or patching alopecia is noticeable when 25% to 40% of scalp hairs are shed. It may be sometimes associated with symptoms of pruritus or pain but is usually asymptomatic. Generally scalp hair is affected, but axillary, pubic hair, eyebrows, and body hair can also be affected. Near complete hair loss is often present by 2 to 3 months and continues for the duration of chemotherapy. A fraction of hairs may be spared that were in the telogen phase at the time of treatment. After chemotherapy is discontinued, the vast majority of patients will naturally regrow hair within 1 to 3 months.
- ■
The severity or degree of alopecia depends on several factors, including the specific agent(s) used, chemotherapy dose, duration of therapy, and serum half-life of the drug. In general, CIA is more severe in patients on multi-agent regimens. In addition, intravenous administration of chemotherapy is generally more deleterious than oral administration at an equivalent dose.
- ■
Hair loss caused by chemotherapy is almost always reversible, although there have been reports of permanent alopecia after treatment with cyclophosphamide and busulfan before bone marrow transplantation. , More recently, cases of severe and irreversible alopecia following chemotherapy with taxanes have been reported in patients with breast cancer. , Although hair regrowth is generally the rule, it is important to counsel patients that regrowth is unpredictable and the thickness, color, or texture of their new hair may be different. ,
- ■
Prevention and treatment of CIA: So far, there has been limited success in the prevention and treatment of CIA. Use of a scarf or a wig seems to be the best practice adopted by patients. The use of scalp-cooling methods has been investigated for the past few decades in an attempt to lessen the severity of alopecia. , Scalp cooling is hypothesized to prevent chemotherapy-related alopecia by limiting blood flow to hair follicles during anticancer treatment, thus decreasing exposure to the chemotherapy. It is also hypothesized to decrease the metabolic rate of hair follicles, which may help reduce their susceptibility to the cytotoxic effects of chemotherapy. The primary concern that had limited the use of scalp hypothermia was the risk of scalp micro-metastases and it is generally advised that scalp hypothermia should not be used for patients with circulating malignant cells, such as leukemia or lymphoma, who are undergoing chemotherapy with curative intent. More recently, two prospective studies of scalp-cooling systems have added evidence supporting the efficacy and safety of scalp cooling in the prevention of CIA, leading to US Food and Drug Administration (FDA) clearance of two scalp-cooling devices to prevent chemotherapy-related alopecia in patients with solid malignancies. , In both studies, patients with breast cancer undergoing treatment with taxanes-based therapy were randomized to receive scalp cooling or placebo; scalp cooling was associated with prevention of significant hair loss in approximately 50% of patients. The adverse effect profile of scalp-cooling devices includes discomfort, headache, scalp pain, and chills, but these are generally tolerable for most patients, as observed in clinical trials.
- ■
Pharmacologic interventions: Multiple pharmacologic interventions for the prevention of CIA have been tested, including minoxidil, bimatoprost, and calcitriol. Minoxidil has been shown to decrease the duration of CIA and may be of some benefit in certain patients. , Further research is needed to determine significant improvements with the use of pharmacological agents for the treatment of CIA.
Hypersensitivity Reactions
Essentially all chemotherapy drugs have the potential to cause allergic or hypersensitivity reactions. However, in general, cutaneous hypersensitivity reactions occur infrequently and have been documented in approximately 5% of patients. Certain chemotherapy agents such as l -asparaginase, paclitaxel, and mitomycin-C exhibit a high incidence of hypersensitivity reactions and may be severe enough to cause dose-limiting toxicity. Table 9.2 lists chemotherapeutic agents associated with hypersensitivity reactions.
- ■
Clinical presentation and treatment: Hypersensitivity reactions are typically immune-mediated and have been divided into type I, II, III, and IV reactions. Most chemotherapy reactions are thought to be type I, immunoglobulin E (IgE)–mediated reactions. Clinically, patients with type I hypersensitivity reactions can present with a local reaction of erythema or pruritus that may or may not proceed to a life-threatening systemic, anaphylactic reaction. This type of reaction most often occurs within 1 hour of chemotherapy administration, but can occur up to 24 hours after exposure. Patients may also complain of nausea, tightness of the chest, respiratory distress, urticaria or rash, and sometimes erythematous streaks along the affected vein. Type III hypersensitivity reactions, in contrast, are mediated by the formation of circulating antigen–antibody immune complexes and are delayed drug reactions. l -Asparaginase and procarbazine have been noted to cause urticarial reactions via a type III–mediated reaction pattern. Allergic contact dermatitis represents a well-known type IV cell-mediated reaction. Mechlorethamine ranks as one of the major causes of type IV hypersensitivity reactions. In the case of paclitaxel and several other chemotherapeutic agents, the diluent or solvent used to enhance the stability or solubility of the drug for intravenous administration may be responsible for the hypersensitivity reaction rather than the drug itself. These reactions are anticipated and standard prophylaxis with corticosteroids, H2 antagonists, and antihistamines is generally required.
- ■
Skin testing: An intradermal skin test should be performed before the initial administration of certain chemotherapy drugs such as bleomycin or asparaginase because hypersensitivity reactions are frequently observed with these agents. However, it should be noted that a negative skin test reaction does not preclude the possibility of development of a hypersensitivity reaction. If reactions occur frequently enough, the agent may require routine prophylaxis using H1-antihistamines, H2-antihistamines, and systemic corticosteroids.
- ■
Continuation or cessation of therapy: Once a hypersensitivity reaction is recognized, the issue of continuation and completion of therapy is raised. In the case of mild reactions, readministration by lowering the infusion rate and using premedication therapy can be considered. If equally efficacious non–cross-reacting alternative agents are available, they should be used. For example, replacement of carboplatin with cisplatin has been shown to allow for an efficacious continuation of platinum-containing chemotherapy after intradermal skin testing elicited positive and negative reactions to carboplatin and cisplatin, respectively. ,
| Drug | Hypersensitivity Reaction |
|---|---|
| l -Asparaginase | Type I |
| Bleomycin | Type I |
| Carboplatin | Type I |
| Cisplatin | Type I, II |
| Chlorambucil | Type I, II |
| Cyclophosphamide | Type I |
| Cytarabine | Type I |
| Docetaxel | Type I |
| Daunorubicin | Type I |
| Doxorubicin | Type I |
| Dacarbazine | Type I |
| Etoposide | Type I, III |
| 5-Fluorouracil | Type I |
| Ifosfamide | Type I |
| Mechlorethamine (topical) | Type IV |
| Methotrexate | Type I, III |
| Mitomycin | Type I, III, IV |
| Paclitaxel | Type I |
| Procarbazine | Type III |
Acral Erythema
Acral erythema, palmoplantar erythrodysesthesia (PPE), or hand-foot syndrome is an adverse event caused by many classic chemotherapy agents and molecular targeted therapies. Doxorubicin, capecitabine, cytarabine, docetaxel, and 5-fluorouracil are the most commonly implicated agents. Liposomal doxorubicin has also been associated with PPE, and as many as 48% of patients receiving the drug may be affected. It is reported that this syndrome develops more often in patients when these agents are administered as continuous infusions compared with administration as bolus infusions. Other drugs causing acral erythema include bleomycin, cisplatin, cyclophosphamide, etoposide, gemcitabine, fludarabine, idarubicin, methotrexate, paclitaxel, and vinorelbine. Table 9.3 lists the chemotherapy agents most commonly associated with acral erythema. The frequency varies from 6% to 42% of patients, and occurs almost exclusively in adults, but may also occur in children receiving high-dose methotrexate therapy.
- ■
Pathophysiology: It has been postulated that the pathophysiology of acral erythema is related to the small capillaries in the palms of the hands and the soles of feet that rupture due to significant exposure to friction and trauma from walking or use, resulting in an inflammatory reaction. PPE seems to be dose-dependent, and both the peak drug concentration and cumulative dose correlate with occurrence and severity. Lesions may develop 1 to 90 days after chemotherapy, and onset of symptoms is typically within 2 to 3 weeks of drug initiation.
- ■
Clinical presentation: The patient typically complains of a tingling, numbness, or burning sensation of the palms and soles after initiation of chemotherapy, followed by intense tenderness and/or pruritus and swelling. Subsequently, discrete red plaques develop on the thenar and hypothenar eminences and on the distil fat pads, which may spread to the dorsum of the hands and feet ( Fig. 9.1 ). Periungual erythema and erythematous bands over the joint surfaces may occur. In severe cases, it may be followed by the formation of desquamative vesicles or bullae. The palms are typically affected more than the feet and may be the only location of the syndrome in some cases. Re-epithelization can occur as part of the healing process, after withdrawal of the offending agent.
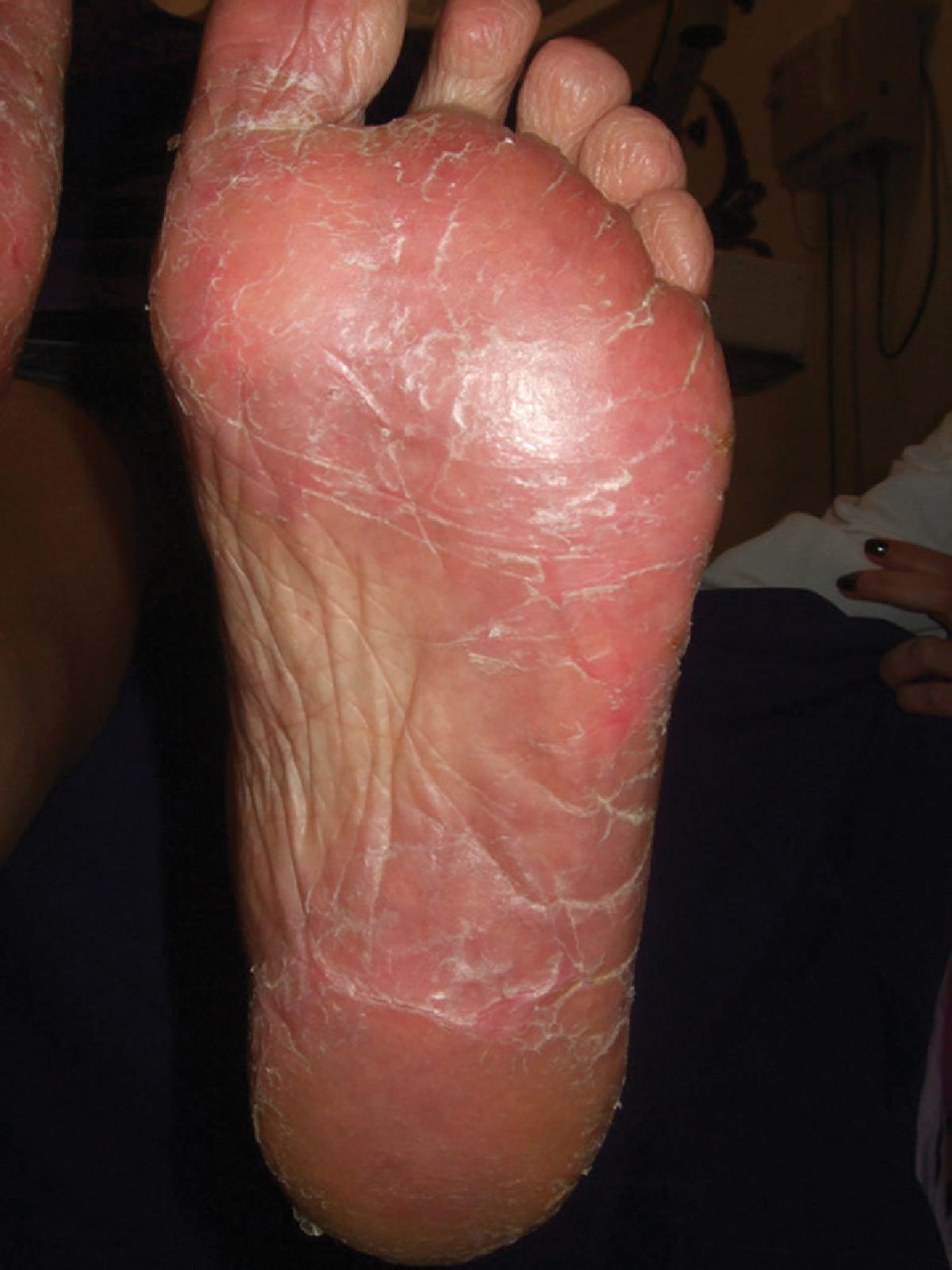
Fig. 9.1
Hand-foot syndrome as a result of 5-fluorouracil in a patient with breast cancer. (From Miller KK, Gorcey L, McLellan BN. Chemotherapy-induced hand-foot syndrome and nail changes: a review of clinical presentation, etiology, pathogenesis, and management. J Am Acad Dermatol . 2014;71[4]:787–794.)
- ■
Differential diagnosis: Early graft-versus-host disease of the hands and feet should be considered in the differential diagnosis and is sometimes difficult to distinguish, especially in patients who have undergone bone marrow transplantation. Serial biopsies performed 3 to 5 days apart may help in differentiating the two disorders, allowing for appropriate management.
- ■
Treatment: The management of acral erythema is largely symptomatic with reduction of drug doses where appropriate. Administration of analgesics, elevation of the extremities, and regional cooling with ice packs, may help ease symptoms. Cold immersion of the hands and feet may also decrease the severity of the syndrome, presumably secondary to vasoconstriction resulting in a lower peak drug concentration being delivered to the extremities. The use of emollients, creams containing lanolin, or urea, or protective gloves may also be helpful in prevention and treatment of acral erythema. The use of pyridoxine and corticosteroids has been reported to be beneficial anecdotally in relieving the associated dysesthesia. Patients should be encouraged to communicate all signs of PPE because early recognition and intervention are essential. In addition, patients should be advised to avoid activities that may increase pressure on the soles and palms. Some patients may resume their chemotherapy regimen after symptom improvement, potentially with chemotherapy dose reduction. There are usually no long-term effects of acral erythema.
| Type | Drug |
|---|---|
| Alkylating agents | Cyclophosphamide |
| Melphalan | |
| Thiotepa | |
| Anthracyclines | Daunorubicin |
| Doxorubicin (including liposomal doxorubicin) | |
| Idarubicin | |
| Antimetabolites | 5-Fluorouracil |
| Capecitabine | |
| Methotrexate | |
| Cytarabine | |
| Hydroxyurea | |
| Mercaptopurine | |
| Vinca alkaloids | Vincristine |
| Vinblastine | |
| Platinum compounds | Cisplatin |
| Taxanes | Docetaxel |
| Paclitaxel | |
| Other mitotic inhibitors | Bleomycin |
| Etoposide | |
| Mitomycin |
Extravasation
Extravasation refers to the escape of a chemotherapeutic drug from a blood vessel to the surrounding tissues, either by leakage or by direct infiltration, causing significant damage to the skin. The true incidence of chemotherapy extravasation varies greatly due to underestimation, but the prevalence of such events is estimated to be 0.1% to 6%, with a higher frequency in children. The severity of tissue injury is dependent on the chemotherapeutic agent used and the concentration of the administered drug. Cytotoxic agents can be classified based on their potential for local toxicity as irritants or vesicants.
- ■
Irritants: An irritant is defined as an agent that produces a local inflammatory reaction, aching, tightness, pain, or phlebitis, at the injection site or along the vein. Clinical signs and symptoms include local sclerosis and hyperpigmentation as well as burning, warmth, erythema, and tenderness in the extravasated area. Necrosis is rare. These symptoms are usually short-lived and self-limited, and most resolve without any long-lasting sequelae. The drugs most frequently associated with this complication are bleomycin, carboplatin, docetaxel, etoposide, topotecan, and dexrasoxane.
- ■
Vesicants: Vesicants are chemotherapeutic agents that have the potential to cause more severe and lasting tissue injury, including the ability to induce tissue necrosis. A number of chemotherapy agents such as actinomycin D, daunorubicin, doxorubicin, mitomycin C, vinca alkaloids, cisplatin, and paclitaxel are classified as vesicants. The early manifestations are often subtle and the full effect of the extravasation injury may be delayed for several days to weeks. The initial signs and symptoms may resemble those of an irritant extravasation injury, including local burning, mild erythema, pruritus, and swelling. An alteration in the rate of infusion or cessation of blood return on aspiration are additional indications of potential extravasation injury. Within 2 to 3 days, increased erythema, pain, induration, dry desquamation, or blistering may appear. If the amount of extravasated material is small, these symptoms may disappear over the ensuing weeks. If the extravasation is significant, necrosis, eschar formation, and ulceration with raised, red, painful edges and a necrotic yellow base may appear ( Fig. 9.2 ). Studies have estimated that about one third of vesicant extravasation injuries may eventually progress to tissue ulceration. Ulceration after vesicant extravasation is typically marked by delayed healing. In severe cases, necrosis may involve underlying tissues such as tendons, nerves, and vessels, with the possibility of serious complications, including nerve compression syndromes, contractures, permanent joint stiffness, and residual sympathetic dystrophies. Other rare manifestations include cellulitis, abscess formation, and squamous cell carcinoma. ,
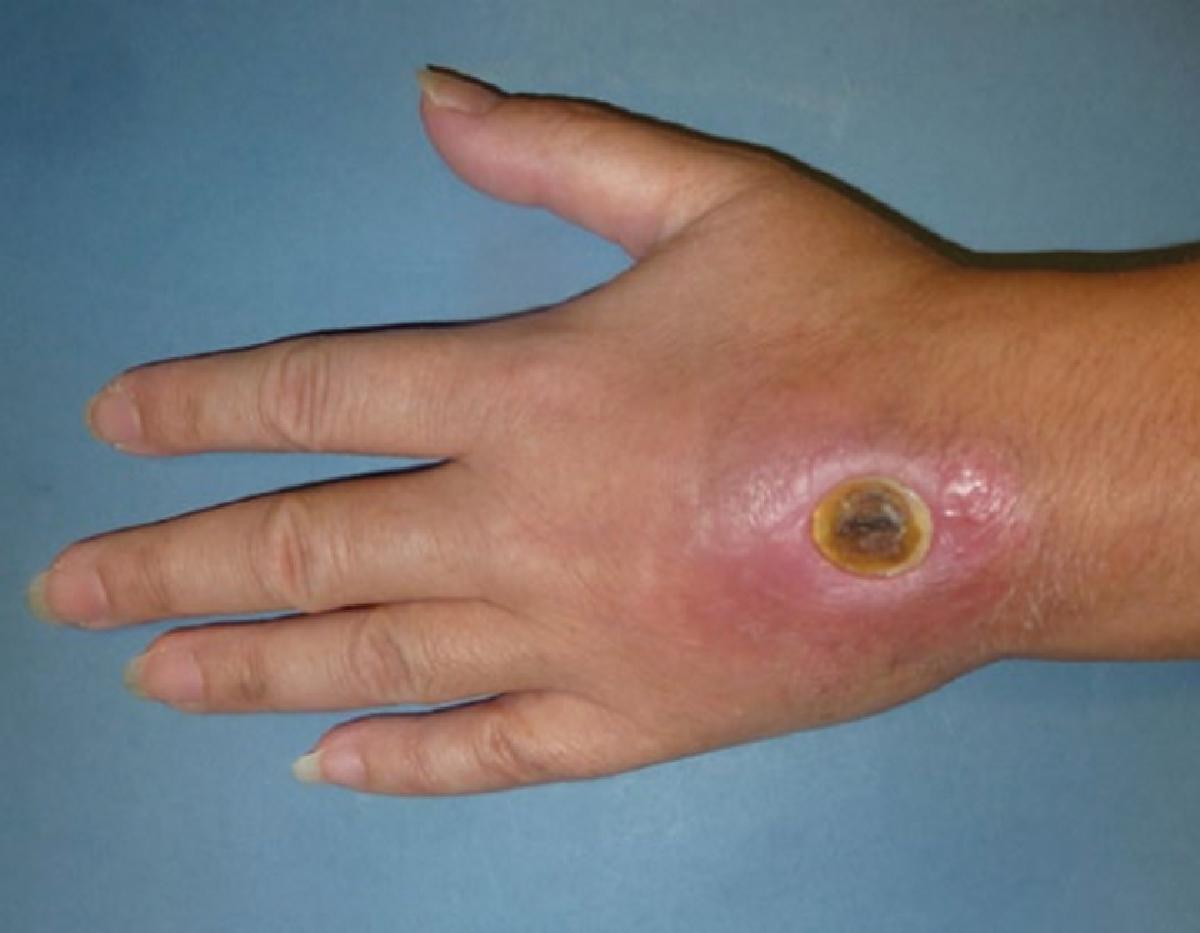
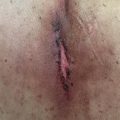
Fig. 9.2
Full-thickness skin necrosis presenting 48 hours following chemotherapy extravasation. (From Goutos I, Cogswell LK, Giele H. Extravasation injuries: a review. J Hand Surg Eur . 2014;39:808–818.)
- ■
Evaluation and treatment: Extravasation injury should be presumed in any patient with persistent swelling, erythema, or pain and prompt recognition and treatment of extravasation injury are necessary to prevent the development of delayed complications. Evidence of extravasation injury requires immediate cessation of the infusion. The site should be aspirated for the residual drug before removing the intravenous catheter. Additionally, attempts at aspiration of the extravasated agent in the surrounding tissue should be made to limit the extent of tissue damage. Elevation of the affected limb and local application of hot or cold packs have been shown to be helpful in limiting the extent of tissue damage. The application of hot packs is hypothesized to cause local vasodilation, leading to dilution of the extravasated drug. Conversely, cold packs may cause increased degradation of toxic metabolites through vasoconstriction and localization of the drug, in addition to reducing local inflammation and providing pain relief. In the event of extravasation of vinca alkaloids heat should be applied to the affected site. Cold packs should not be administered because cold has been found to increase ulceration after vinca alkaloid extravasation in animal models.
- ■
Antidotes: Many studies have investigated the usefulness of antidotes to different chemotherapeutic agents for the prevention of necrosis and ulceration at the site of extravasation. These include topical dimethylsulfoxide (DMSO) for anthracycline extravasation, hyaluronidase for vinca alkaloid and etoposide extravasation, and sodium thiosulfate for mechlorethamine, concentrated dacarbazine, and concentrated cisplatin extravasation. , Currently, dexrazoxane hydrochloride is an FDA–approved treatment for anthracycline extravasation and has been reported to produce significant wound healing activity. High-dose steroids can be used for the extravasation of oxaliplatin but are contraindicated for etoposide and vinca alkaloids, because steroids can worsen skin damage associated with these agents.
- ■
Surgical intervention: For persistent or progressive local symptoms, a surgical consult should be obtained because the treatment of unresolved tissue necrosis or pain lasting more than 10 days is surgical debridement. Such a procedure should consist of wide excision of all necrotic tissue until bleeding occurs and only healthy tissue is left for would coverage. Once the wound is clean, immediate or delayed surgical reconstruction and skin grafting can be employed.
Hyperpigmentation
Hyperpigmentation of the skin, hair, mucous membranes, and nails is another common cutaneous manifestation of chemotherapy. It may occur in various anatomic locations and increased pigmentation may be present locally, such as at the site of drug infusion, or diffusely.
- ■
Mechanism: The mechanism of this adverse effect has not been fully elucidated, but is believed to be a result of direct toxic effects on melanocytes, stimulating increased melanin secretion.
- ■
Patterns of hyperpigmentation: A variety of patterns of hyperpigmentation have been described in association with different chemotherapy agents ( Table 9.4 ).
TABLE 9.4
Chemotherapeutic Agents Associated With Hyperpigmentation
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree