Most patients with corticotropin (ACTH)-dependent Cushing syndrome (CS) will have an ACTH-secreting pituitary microadenoma. Approximately 15% of patients with ACTH-dependent CS have an ectopic source of ACTH secretion. The most common neoplasms associated with ectopic ACTH secretion are bronchial carcinoid (≈25%), pancreatic neuroendocrine tumor (≈16%), occult and unlocalized tumor (≈16%), small cell lung cancer (≈11%), medullary thyroid carcinoma (≈9%), other neuroendocrine tumors (≈7%), thymic carcinoid (≈5%), and pheochromocytoma (≈3%). The main clues that a patient may have ectopic ACTH-dependent CS include severe CS as evidenced by spontaneous hypokalemia and 24-hour urinary free cortisol (UFC) >1000 mcg, rapid onset of CS (sometimes so rapid that there is not time to develop the typical physical stigmata of CS), previous diagnosis of a neuroendocrine tumor, and male sex. Herein we present a case of cyclical ectopic secretion of ACTH.
Case Report
The patient was a 71-year-old woman who was referred for management of ACTH-dependent CS. Evaluation was prompted by the new-onset symptoms of several months duration that included resistant hypertension, bilateral lower extremity edema, uncontrolled diabetes mellitus, and proximal myopathy. She also noticed hirsutism, facial puffiness, thinning of the skin, and easy bruising. Because of muscle weakness, she sustained several falls and was no longer able to live independently. CS was suspected, and she was referred to our institution for further evaluation and management.
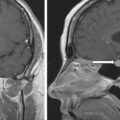
The patient’s history was remarkable for resolved ACTH-dependent hypercortisolism 2 years prior. At that time, she presented with similar symptoms of difficult to control hypertension, uncontrolled diabetes mellitus, and hypokalemia. Workup at that time confirmed ACTH-dependent hypercortisolism ( Table 60.1 ). Magnetic resonance imaging (MRI) of the pituitary gland was performed at that time and did not reveal a pituitary adenoma. Computed tomography (CT) of the chest and abdomen, as well as In-111 pentetreotide scintigraphy at that time did not reveal a neuroendocrine tumor. Inferior petrosal sinus sampling (IPSS) was scheduled but was cancelled, as repeated workup no longer revealed hypercortisolism (see Table 60.1 ). Her symptoms resolved several months later and she had no concerns until 2 years later.
| Biochemical Test | 30 Months Prior | 27 Months Prior | 25 Months Prior | Current Evaluation | Reference Range |
| 8 am serum cortisol, mcg/dL | 27 | 11 | 14 | 93 | 7–25 |
8-mg overnight DST, mcg/dL | 27.4 | <1 | |||
ACTH, pg/mL | 254 | 35 | 366 | 10–60 | |
DHEA-S, mcg/dL | 211 | 15–157 | |||
24-Hour urine free cortisol, mcg | 86 | 3.9 | 9 | 683 | <45 |
On physical examination, the patient was sitting in a wheelchair. Her skin was found to be thin, with multiple bruises. She had moon facies, facial plethora, supraclavicular pads, and a mild dorsocervical pad. She had no striae. Facial hirsutism and mild androgenic alopecia were observed. She had proximal myopathy on examination in both upper and lower extremities. Bilateral 1+ lower extremity edema was noted.
INVESTIGATIONS
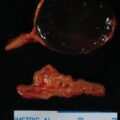
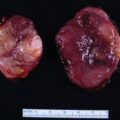
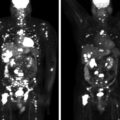
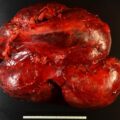
ACTH-dependent hypercortisolism was confirmed (see Table 60.1 ). IPSS was performed to determine the subtype of ACTH-dependent hypercortisolism ( Box 60.1 ) and pointed toward an ectopic source. CT of abdomen was performed and revealed a 1.8-cm pancreatic lesion ( Fig. 60.1 ). When compared to the CT scan from 2 years prior, the pancreatic lesion had grown by 1 cm. It was In-111 pentetreotide negative on the initial scan.