Chapter 39 Cutaneous Carcinoma
Cutaneous basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) are the most common malignant neoplasms in the world and occur at epidemic rates in some countries such as Australia.1 Collectively, these two carcinomas account for most (95%) patients with nonmelanoma skin cancer (NMSC) and are markedly more common than malignant melanomas, which account for only 5% of all skin malignancies. Most BCCs and SCCs occur in individuals older than 50 years old with fair complexions or outdoor occupations mostly on the sun-exposed head and neck or extremities, although NMSC does occur in younger people. Skin cancers may be disfiguring and associated with local morbidity in certain locations but are rarely lethal. The frequency of BCC is four times that of SCC, and BCCs tend to be more indolent and rarely metastasize.
Other NMSCs that are infrequently encountered include Merkel cell carcinoma (MCC) and adnexal cancers. MCC, also known as primary cutaneous neuroendocrine carcinoma, is a rare small cell carcinoma originally described by Toker in 1972.2 Sebaceous gland carcinomas account for less than 1% of all skin neoplasms.3 Eccrine or sweat gland carcinomas are very rare, estimated to account for less than 0.01% of malignant epithelial neoplasms of the skin.
Etiology And Epidemiology
The main etiologic factor for cutaneous carcinoma is sun exposure in individuals, usually whites, whose skin is susceptible to the chronic carcinogenic effect of ultraviolet (UV) light.4 Approximately 90% of NMSC can be attributed to excessive sun exposure. Other, less common etiologic factors include exposure to chemical carcinogens (e.g., arsenic, tar, anthracene, and crude paraffin oil), chronic irritation or inflammation, and ionizing radiation.
The incidence and aggressiveness of SCC and MCC (both immunogenic carcinomas) are markedly increased in individuals with compromised immune function, including patients with non-Hodgkin’s lymphoma and chronic lymphocytic leukemia5 and organ transplant recipients with iatrogenic immunosuppression.6 In contrast, the incidence of BCC is not increased and the outcome is similar as for immunocompetent patients.
Some genetic syndromes are also associated with a higher risk of developing skin carcinoma. Individuals with xeroderma pigmentosum are prone to developing BCC and SCC at a very young age because of defective repair of UV light–induced DNA damage.7 These patients usually die in their early 20s from disseminated SCC or melanoma. The basal cell nevus syndrome (or Gorlin syndrome) is a genetic form of BCC inherited through an autosomal dominant gene.8 Individuals with epidermodysplasia verruciformis tend to develop nodules of SCC within large verrucous plaques in the 3rd and 4th decades of life.
Prevention And Screening
Unprotected sun exposure, especially during the summer, is the main determinant for the subsequent development of skin cancer. Children and adolescents should be especially educated in regard to sun protection. The damage of excessive UV exposure is irreversible, but despite this adults can still reduce their risk by avoiding further excessive UV exposure. Authorities worldwide have made recommendations regarding appropriate measures. A panel of the American College of Preventive Medicine issued practice policy statements with regard to skin cancer prevention, as summarized by Hill and Ferrini,9 and recommended preventive measures to reduce skin cancer to include avoidance of sunlight exposure—particularly limiting time spent outdoors between 10 A.M. and 3 P.M.—and wearing protective physical barriers, such as hats and clothing. If sun exposure cannot be limited because of occupational, cultural, or other factors, the use of sunscreens that are either opaque or that block UVA and UVB radiation is recommended. The use of tanning booths is also a factor in the risk of developing skin cancer, and guidelines regarding their appropriate use should be followed.
Clinical Manifestations, Pathobiology, And Pathways Of Spread
Basal Cell Carcinoma
Clinical Presentation and Pathology
BCC constitutes approximately 80% of all NMSC and is the most common malignancy worldwide. Most BCCs arise on the sun-exposed head and neck (80% to 85%); lesions occur less frequently on the trunk or extremities. Lesions may manifest as an asymptomatic nodule, a pruritic plaque, or a bleeding ulcer that characteristically waxes and wanes.10,11 Many patients treated for BCC develop at least one or more further BCCs.12 Careful evaluation of sun-exposed skin should be part of any follow-up examination.
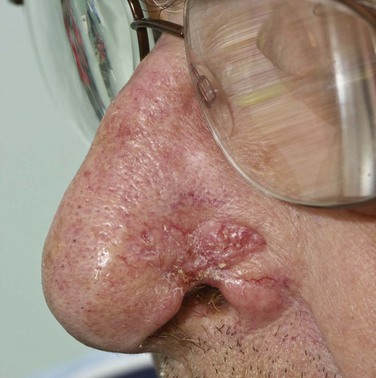
BCC has numerous variants, each of which has distinctive clinical and histologic features and natural history. The characteristics of commonly occurring types are briefly summarized. Nodular BCC, colloquially referred to as rodent ulcer, is the most frequently observed variant and accounts for approximately 50% of all lesions (Fig. 39-1). This type of skin cancer begins as a distinct papule that may develop central umbilication, progressing to central ulceration as the lesion grows. The margins of the lesion appear pearly (pale and translucent) and contain enlarged capillaries (telangiectasia). Histologic features include the presence of large islands of monomorphous basaloid cells, varying in size and shape, embedded in a fibroblastic stroma in the dermis. The basaloid cells have large, oval hyperchromatic nuclei, scant cytoplasm, and no intercellular bridges. The peripheral cell layer of the aggregate frequently shows palisading, whereas central cells are less organized. Nodular BCC may show a varying degree of pigmentation (blue, brown, or black), depending on the number of melanocytes present in the lesion, and may be difficult to differentiate clinically from malignant melanoma.13
Superficial BCC manifests as red, scaly macules with indistinct margins, usually located on the trunk (Fig. 39-2). It enlarges into a crusted, erythematous patch without induration that may be difficult to differentiate clinically from solar keratosis, psoriasis, SCC in situ, or extramammary Paget’s disease. Histologic examination shows multiple foci of buds of neoplastic cells with peripheral palisading originating from the undersurface of the epidermis.10
Morpheaform (sclerosing) BCCs appear as single, flat, indurated, ill-defined macules. The lesions generally have a smooth, shiny surface that becomes depressed as it grows into a plaque. It is characterized histologically by the presence of small groups and narrow strands of basaloid cells embedded in a dense, fibrous connective tissue; there is little peripheral palisading.14 Perineural invasion is often reported to be present.
Infiltrative BCC has an opaque yellowish appearance and blends subtly with the surrounding skin.14 Histologically, the lesion is characterized by poorly circumscribed spiky cell aggregates in the superficial portion and the main bulk, consisting of strands of neoplastic cells infiltrating the reticular dermis and subcutis.
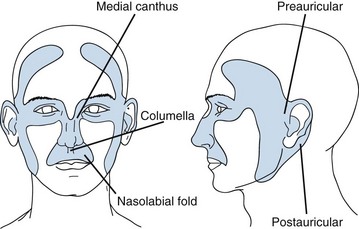
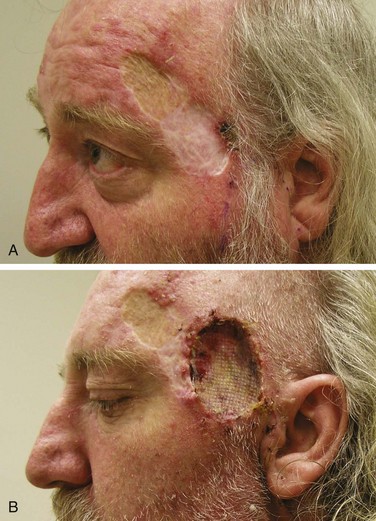
Location is important in defining high-risk BCC. The midface, or so-called H zone (Fig. 39-3), including the periauricular region, glabella, medial canthus, nose, nasolabial region, and columella, contains embryonal fusion planes.15 The extent of tumors in this region is frequently underestimated, leading to inadequate surgical excision, especially deep, and a higher rate of local recurrence. Histologic examination often reveals extensive infiltration of deeper structures by small nests of undifferentiated basal cells. This type of lesion may invade the orbit, nose, and maxilla, resulting in significant deformity. It should be readily recognized and treated promptly often necessitating extensive surgery with or without adjuvant RT.
Biology and Pattern of Spread
The biologic behavior of BCC varies with the histologic type. A superficial BCC may remain stable for a long time or enlarge gradually over many years to become a nodulo-ulcerative variant. Nodular BCC grow slowly over many years by peripheral and deep invasion, particularly along embryonal fusion planes, and perineural spread. Morpheaform, infiltrative, and terebrant BCCs are more aggressive variants that may spread through peripheral invasion or infiltration of deeper structures, or both. Perineural (or neurotropic) invasion in BCC is rare, occurring in only 2% to 3% of patients, and generally occurs in the setting of recurrent disease or in morpheaform histology.16 Lesions located around the orbit may gain access to the orbit via the first or second division of the trigeminal nerve (or fifth cranial nerve).
BCCs rarely spread to the regional lymph nodes or distant organs with an overall incidence of metastasis less than 0.01%.17 Most metastases occur in the regional lymph nodes with distant spread usually preceded by regional metastasis. Regional disease typically develops with large, ulcerated lesions in the head and neck that have recurred after repeated surgery and RT.
Squamous Cell Carcinoma
Clinical Presentation and Pathology
SCC arises from keratinocytes of the epidermis. This type of NMSC most commonly develops from skin exhibiting solar (or UV) damage. Actinic (or solar) keratosis (intradermal malignant neoplasm) is generally a precursor or premalignant lesion; at least 50% to 60% of all invasive SCCs arise from actinic keratoses. Despite this, only a few (<5%) actinic keratoses actually progress to invasion. In a large study of 169 patients with 7784 documented actinic keratoses, the risk of malignant progression was reported in 2.6% at 4 years.18 Less frequently, SCC occurs from other preexisting skin lesions, such as arsenic keratosis, a thermal burn scar, or a chronic ulcer. Rarely, it arises from normal-appearing skin.13
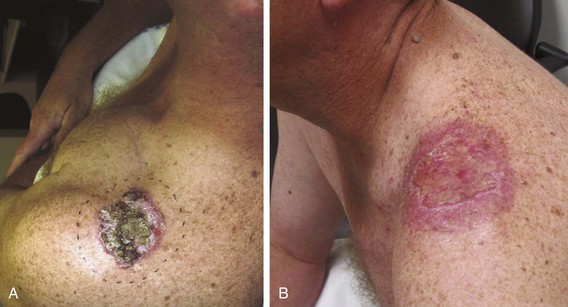
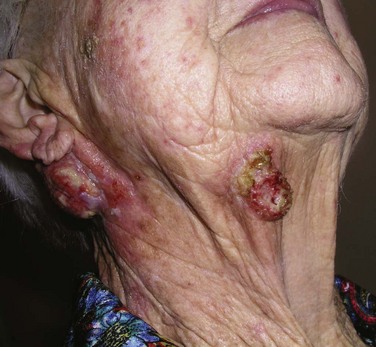
Clinically, SCC in situ (Bowen’s disease) manifests as a soft, erythematous, scaly, well-circumscribed patch (Fig. 39-4). Superficial carcinoma manifests as a scaly, crusted plaque or ulcer with a verrucous or papillate border, and infiltrating SCC manifests as a firm, ulcerated mass with an elevated nodular border (Fig. 39-5).
Biology and Pattern of Spread
SCC generally has a more aggressive course than BCC. Carcinoma in situ (or Bowen’s disease) may evolves gradually into superficial carcinoma in 5% of cases.19 Untreated, it may progress further into an infiltrating type that invades the surrounding and underlying structures. The rate of progression depends on the degree of cellular differentiation.
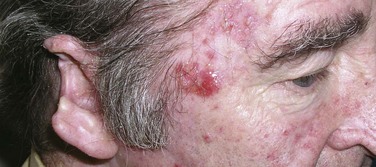
The risk of developing metastases, usually nodal, is markedly higher in SCC than in BCC. However, most immunocompetent patients with small (<2 cm), thin (<4 to 5 mm thick), nonrecurrent lesions are at low (<5%) risk of developing nodal metastases. Patients not meeting these criteria can be considered high-risk patients (>10% risk), and appropriate awareness and management are required.20 Recurrent lesions in close proximity (forehead, temple, ear, cheek) to the parotid gland increase this risk (Fig. 39-6). Data suggest that tumor thickness greater than 6 mm is a powerful, independent predictor of patients at risk for regional metastases.21
The most frequent sites for the development of metastatic cutaneous SCC are the parotid gland, the cervical lymph nodes, or both.22 In 20% to 25% of cases, an obvious index lesion is not identified. Invariably, these patients have a long-standing history of actinopathy with previous NMSC. The development of distant metastases (e.g., lung, liver) rarely occurs as a first site of relapse and is more often encountered after initial treatment for nodal metastases.
Metastatic cutaneous SCC occurs less frequently in other nodal regions, such as the axilla and groin. Although difficult to quantify, the ratio of metastatic head and neck SCC to non–head and neck SCC is approximately 9 : 1. There are much fewer published data on the management of these patients, but analogous generalizations from the evidence on parotid and neck nodal metastases suggest operable patients should have surgical resection, and many have unfavorable features, such as extranodal spread and incomplete margins, and require adjuvant RT.23 The combination of surgery and adjuvant RT often leads to extremity lymphedema, and patients should be warned about this.
Merkel Cell Carcinoma
Clinical Presentation and Pathology
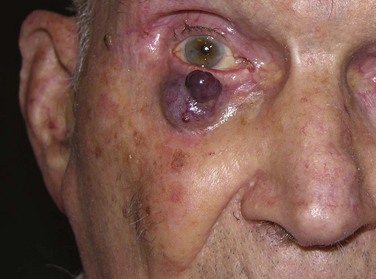
MCC is a small cell cutaneous malignancy that often manifests as a rapidly enlarging firm, painless, pink-red, dermal-based nodule, most frequently on the head and neck or extremities in older (>60 to 70 years old) individuals (Fig. 39-7). In contrast to other types of NMSC, MCCs frequently arise in women. Diagnosis is often delayed by clinicians because of the uncommon nature of this disease. The median size of the primary lesion at diagnosis is approximately 2 cm, and the incidence of clinical nodal involvement at presentation is approximately 20% to 25%, although the risk of harboring occult nodal disease is high (30% to 40%).24 Based on the U.S. Surveillance, Epidemiology, and End Results (SEER) database, the annual incidence in men is 0.34 per 100,000 with most patients older than 65 years and white (94%). In this study, slightly less than half (46%) of all lesions occurred in the head and neck, and at diagnosis half of all patients had localized disease with nodal metastases present in approximately 25%.25
The cell of origin of this neoplasm is thought to be the dermal neurotactile cell arising from the neural crest first described by Merkel.26 The lesion usually involves the reticular dermis and subcutaneous tissues, with minimal extension to the papillary dermis and sparing of the epidermis. Vascular and lymphatic permeation is common, and clinically such permeation often manifests as in-transit metastasis. The neoplastic cells exhibit cytoplasmic extensions and small, uniform, membrane-bound neurosecretory granules on ultramicroscopic examination.27 Several immunohistochemical markers have been identified in MCC. The neoplastic cells stain most consistently with polyclonal antisera to neuron-specific enolase and calcitonin, monoclonal antibody to neurofilament, and cytokeratin (CK 20 positive).28 More recent evidence suggests a possible viral association in the development of MCC. In the study by Feng and colleagues,29 8 of 10 tumors were found to contain Merkel cell polyomavirus compared with only 8% in control tissues.
Biology and Pattern of Spread
The results of many retrospective studies confirm that MCC has an aggressive course characterized by propensity for contiguous spread, reflected in high local recurrence rates after wide surgical excision alone and a high incidence of nodal involvement and hematogenous dissemination.29 Most series document a cancer-specific death rate of around 30%.30 Patients may also present with metastatic nodal disease without an obvious index lesion. In one large study, 19% of patients had metastatic disease to nodes from an unknown primary.31 MCC is a highly immunogenic carcinoma, and immunosuppressed patients (organ transplant recipients) and patients diagnosed with non-Hodgkin’s lymphoma and chronic lymphocytic leukemia are at higher risk of developing MCC and having a poor outcome. In a study of 41 organ transplant recipients with MCC, many were younger, most (68%) had nodal disease at diagnosis, and almost 60% died of their disease.32
Adnexal Carcinoma
Sebaceous Carcinoma
Clinical Presentation and Pathology
Sebaceous carcinomas are rare (approximately 400 reported) and arise most commonly (75% of cases) from the sebaceous glands of the ocular adnexa, the meibomian glands in the tarsus or glands of Zeis at the lid margin, and the caruncle. Extraocular locations, in decreasing frequency, are head and neck region, trunk and extremities, and external genitalia.3 Histologically, these carcinomas are composed of dermal-based lobules and cords of tumor cells, with varying degrees of sebaceous differentiation and infiltration into the surrounding tissues. Differentiated cells contain foamy or vacuolated, slightly basophilic cytoplasm, whereas less differentiated cells contain more deeply basophilic cytoplasm. Clinical and pathologic features that indicate a poor prognosis include size of the primary lesion (>1 cm is associated with 50% mortality rate), vascular and lymphatic invasion, poor sebaceous differentiation, highly infiltrative growth pattern, and intraepithelial carcinomatous changes in the overlying epithelia.33
Biology and Pattern of Spread
Sebaceous carcinoma behaves more aggressively than SCC, with a propensity for nodal and hematogenous spread.34 Of the 104 patients registered by the Ophthalmic Pathology of the Armed Forces Institute of Pathology, 23 patients (22%) experienced local recurrence once, and 11 patients experienced local recurrence two or more times. Metastatic disease was the cause of death in 23 patients.33
Eccrine Carcinoma
Clinical Presentation and Pathology
Histologically, eccrine or sweat gland carcinomas may resemble carcinomas of the breast, bronchus, and kidney and are difficult to differentiate from cutaneous metastases. Many histologic variants are reported and include ductal eccrine carcinoma, mucinous eccrine carcinoma, porocarcinoma, syringoid eccrine carcinoma, clear cell carcinoma, and microcystic adnexal carcinoma.35
Biology and Pattern of Spread
Eccrine carcinoma also has more aggressive behavior than BCC and SCC. In a series of 14 patients who underwent surgical excision with free microscopic margins, 11 developed at least one local recurrence, and 5 failed at regional nodes or distant sites. One patient died of uncontrolled local relapse, and four died of distant metastasis 2 months to 10 years after diagnosis.35 Apocrine carcinoma arises most commonly from apocrine glands of the axilla, but it can originate from apocrine glands of the vulva and eyelids and from ceruminal glands of the external auditory canal. It manifests clinically as a red-purple single or multinodular, firm or cystic dermal mass in elderly individuals. Because of its rarity, the natural history of apocrine carcinoma is not well known. Nodal and distant spread has been reported.36,37