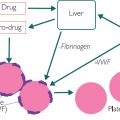
Figure 10.1: Flow diagram of insulin-mediated storage of glucose as glycogen
Glucose causes insulin to be released from beta cells in the pancreas. Insulin converts glucose to glycogen (in a process called glycogenesis), and the glycogen is subsequently stored in the liver. Failure to recognise glucose or make insulin will lead to glucose in excess. Glucose levels can therefore, in a normal state, be affected by stress, pancreatitis and liver damage ( adrenaline, amylase (raised in pancreatitis) and LFTs, especially following trauma or in patients with poor liver function).
adrenaline, amylase (raised in pancreatitis) and LFTs, especially following trauma or in patients with poor liver function).
Diabetic complications
Most of the complications in diabetes are caused by excess glucose binding to, and then interfering with the actions of, specialised cells and proteins.
There is raised cardiovascular risk caused by excess glucose binding to the vascular wall. This increases stiffness and oxidises any excess low-density lipoprotein (LDL), which – under the action of macrophages – becomes foam cells and forms atherosclerotic plaques. The glucose also binds directly to the cardiac muscle and nerve endings.
In diabetic neuropathies, the excess glucose binds directly to the nerve cells and suppresses nerve conductivity, inducing vascular and neural retraction from the site. The reduction in vascular flow and integrity leads to more incidents of infection because the white cells are less able to reach the affected site. This is also why antibiotic therapies may take longer to work. This is particularly true in sites with poor circulation such as hands and feet, where neuropathies are most commonly observed in primary care.
In diabetic retinopathy and other vision symptoms, the excess glucose binds directly to the retinal cells and changes their structure. This causes a change in opacity and function, leading to blurred vision and in some cases eventual loss of sight.
In diabetic renal impairment, the excess glucose binds directly to the glomerulus and nephrons, suppressing performance. This often reduces eGFR and increases the already dysfunctional Na levels caused by polyuria and polydipsia.
Diabetic ketoacidosis occurs when fatty acids are utilised for energy, given the poor control of glucose. This produces ketones, which are acidic and affect the blood pH. Investigations should include high blood glucose, presence of ketone bodies, high blood pH, U&E due to renal dysfunction due to continued dehydration, amylase to rule out pancreatitis, and full blood count (FBC) and C-reactive protein (CRP) to rule out infection.
Measuring glucose, and diagnosing and treating diabetes
Glucose levels can be measured in numerous ways, shown A to D in Figure 10.2 (below).
Random blood glucose (A) assesses the patient’s ability at a random point to have glucose under control. This is usually used in patients already diagnosed with diabetes, who are managing insulin loads or diet interventions. The random blood glucose can produce false positive values (B), particularly following a meal, especially if the meal is high in sugar. This false positive would return to normal values under the action of insulin over a few hours. Fasted blood glucose (B1) may therefore be requested to remove the chance of a high result being due to a meal.
The oral glucose tolerance test (C) measures the insulin response following a glucose load. The patient attends having fasted and a blood sample is taken (time = 0 min). The patient is then given a glucose load, usually as a drink, which should induce an insulin response. They then wait in a low exercise capacity, for two hours, for the action of biphasic insulin to be effective. Then a second blood test is taken (time = 120 min). Glucose is measured and compared in both samples; they should be within the reference range in normal patients. In glucose intolerant or diabetic patients, the 120-minute sample will have glucose outside the reference range (C1), highlighting a lack of insulin efficacy.
HbA1c is a type of haemoglobin (HbA) with glucose attached to it (D). Haemoglobin is the oxygen-carrying protein in red blood cells and it becomes irreversibly glycosylated when glucose is in excess. It is therefore a useful long-term marker of diabetes, because the red blood cell has a lifespan of 12 weeks. There are two ways to express HbA1c – either as a percentage or as a concentration. The DCCT percentage values refer to what percentage of total Hb is HbA1c. A value higher than 7% usually indicates glucose intolerance. The IFCC mmol/mol value refers to measuring the amount of HbA1c directly as a concentration. A value higher than 53 mmol/mol usually reflects glucose intolerance.
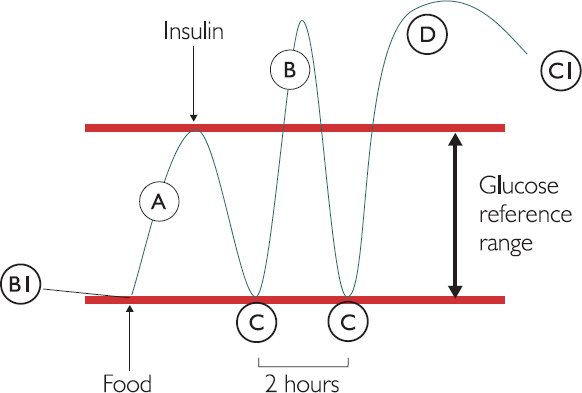
Figure 10.2: Measuring glucose levels
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree