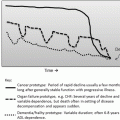
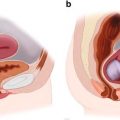
Fig. 10.1
(Left) The age-associated activation of inflammatory cells and decline in androgen hormones upset the balance between catabolic and anabolic stimuli, respectively, leading to a decline in muscle mass and composition known as sarcopenia . This detrimental response is aggravated in patients with insulin resistance and metabolic syndrome. Addition of bed rest and malnutrition initiates a vicious cycle of further decline in muscle mass, limiting the necessary mobilization of amino acids in times of stress. (Right) The accumulation of subclinical impairments in multiple organ systems resulting from cardiovascular disease, lifelong “wear and tear,” and/or genetic predisposition lead to decreased homeostatic reserve and resiliency to stressors. Other pathophysiological pathways have been proposed. Biological pathways may manifest clinically as slow walking speed, weakness, weight loss, physical inactivity, and exhaustion—termed the phenotype of frailty. CRP C-reactive protein, IL Interleukin, TNF tumor necrosis factor. Reproduced with permission from Afilalo, J, et al. Frailty assessment in the cardiovascular care of older adults. JACC 2014:63;747–62
10.1 Assessment of Frailty
There are several methods for assessing a patient to discover if frailty is present preoperatively. It is no longer acceptable to simply look at the patient and make this judgment, as was a method in the past. Rather, a protocol driven assessment is mandatory to identify the frail patient. If frailty is present, the patient is at a much increased risk for a poor outcome after a major perturbation such as surgery. At the University of Colorado Multidisciplinary Heart Valve Clinic consisting of surgeons, cardiologists, and others, three tools for the preoperative assessment to identify frailty seem effective: the 5-m walk test, grip strength as assessed by a dynamometer, and the Fried scale. The 5-m walk test is simple to conduct. One only needs a well-lighted hallway with 1-m lengths marked off to conduct this test. This test is perhaps the easiest to utilize and understand. Afilalo [7] and colleagues established that slow gait speed , defined as >6 s to walk 5 m, was an incremental risk factor for increased mortality and morbidity following cardiac surgery . These authors combined the robust risk-adjusted models of predicted mortality from the Society of Thoracic Surgeons (STS) Adult Cardiac Surgery Database and the 5-m walk test in 131 patients. Importantly, the combination of a high predicted STS risk with slow gait speed predicts a nearly 50 % chance of mortality or major morbidity (e.g., stroke, renal failure, prolonged ventilation, deep sternal wound infection, or need for re-operation) (Fig. 10.2). Finally, this study showed that slow gait speed will increase the STS predicted risk 2–3 fold. This finding is of great value in directing contemporary therapy for certain, patients at increased risk for of a poor outcome from open surgery. For example, frail elderly females (assessed by gait speed) with prior coronary artery bypass surgery and reduced left ventricular ejection fraction with severe aortic stenosis will be very high-risk patients for open, surgical AVR and therefore should be considered for Transcatheter Aortic Valve Replacement (TAVR) . Gait sped is now collected in the latest version of the STS Database and in the Transcatheter Valve Therapy (TVT) registry.
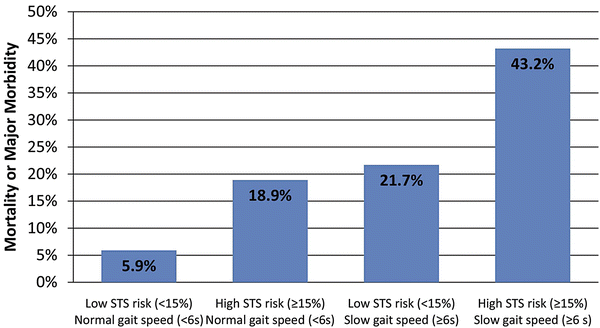

Fig. 10.2
The dual risk factors of slow gait speed (>6 s to walk 5 m) and high Society of Thoracic Surgeons (STS) score (>15 % predicted mortality or major morbidity) identified patients at the highest risk. Among those with the dual risk factors, 43.2 % experienced a major morbidity or mortality compared with only 5.9 % of those without either risk factor. Reproduced with permission from Afilalo J, et al. Gait speed as an incremental predictor of mortality and morbidity in elderly patients undergoing cardiac surgery. JACC 2010; 56: 1668–76
Frailty has a direct and strong association with excess mortality, morbidity, functional decline, and other adverse events following cardiac surgery. In a review of studies that objectively measured frailty in over 4700 patients collectively frailty was strongly associated with excess mortality, morbidity, and functional decline [8]. Not surprisingly, frailty was more pronounced in the older patients undergoing TAVR compared to younger patients undergoing coronary artery bypass or open AVR. Many studies point out the importance of identifying frailty preoperatively in patients proposed for open cardiac surgery for aortic value replacement or TAVR. Its presence predicts inferior outcomes in these interventions.
10.2 Coronary Artery Disease/Coronary Artery Bypass Grafting
The combination of the explosion of the population aged >70 and the strong association of the development of atherosclerotic coronary artery disease with advanced age has fueled a demographic shift in the surgical management of coronary artery disease. Indeed, while the total volume of coronary artery bypass procedures has decreased from 2001 to 2010, the number of elderly patients referred for bypass surgery has increased. In fact the percentage of octogenarians who receive coronary artery bypass grafting (CABG) has increased from 7 to 11 % [9]. Remarkably, the mortality risk for elderly patients undergoing CABG has decreased while the predicted risk for surgery has been gradually increasing. The reasons for this achievement are unknown; however, postulated explanations include increasing use of the left internal mammary in elderly patients, more use of off-pump CABG, and greater collective experience with CABG.
Percutaneous coronary intervention (PCI) and CABG have emerged as complementary rather than competing interventions for the management of multi-vessel coronary artery disease. The vast majority of randomized controlled trials, which have compared PCI to CABG included very few patients >75 years of age. Small, non-randomized trials before the advent of drug eluting stents (DES) favored CABG over medical therapy [10] and CABG over PCI [11]. The quality of this body of evidence, however, is insufficient to support a firm recommendation that CABG can be demonstrated to be superior to PCI or medical therapy in elderly patients. However, age alone should not preclude the consideration of CABG in the elderly cohort. A large Canadian registry, the APPROACH database, analyzed outcomes from over 21,000 patients who underwent coronary angiography for ischemic heart disease. Nearly 1000 of this patient cohort were >80 years of age. Four-year risk-adjusted survival was highest for CABG at 77.4 %, followed by 71.6 % for PCI and 60.3 % for medical therapy [12]. While a selection bias for patients who received intervention is unavoidable in this retrospective analysis, it suggests that the benefits of surgical revascularization extend to elderly patients.
Equally compelling as an outcome is functional status or quality of life (QOL) for elders who elect to undergo invasive procedures. The literature that addresses QOL following CABG suggests benefit for elderly patients undergoing CABG. A retrospective analysis reported favorable 1- and 2-year outcomes in octogenarians who underwent CABG [13]. Over 80 % of survivors were living in their own home, 74 % rated their health as good or excellent, and 82 % would undergo operation again. While frailty predicts poor outcomes, future research in this area should be directed towards answering important questions: are there long-term consequences from an episode of delirium following CABG; is longer-term quality of life—5–10 years—maintained in these patients?
What remains a central tenet in the evaluation of the elderly patient with ischemic heart disease being considered for an intervention is the evaluation and management by a dedicated team. This team should at a minimum consist of a cardiologist, surgeon, nurses, and potentially other allied specialties. With the patient as a focus, such a team is more likely to suggest wiser, thoughtful patient specific recommendations. Increasingly interdisciplinary teams consisting of a highly cohesive group of clinicians of different training backgrounds are especially effective in evaluating and caring for vulnerable seniors being treated with an invasive cardiac procedure.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree