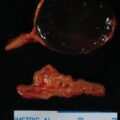
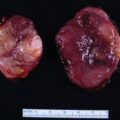
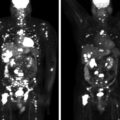
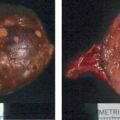
Fortunately, bilateral adrenal hemorrhage is a rare event. In situations of physiologic stress (e.g., postoperative state or sepsis), blood flow to the adrenal glands and cortisol production are markedly increased—the adrenal glands become edematous and susceptible to hemorrhage, hypotension, and venous infarction. Thus the typical clinical settings for bilateral adrenal hemorrhage include the postoperative period, trauma, neoplastic infiltration of the adrenal glands, anticoagulation therapy, and coagulopathies such as antiphospholipid-antibody syndrome. Typically, primary adrenal insufficiency, if present, is a permanent deficit. The case presented herein highlights the evolution of adrenal hemorrhage on computed tomography (CT) and the potential to recover adrenocortical function.
Case Report
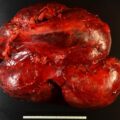
This 68-year-old woman presented to the emergency department with severe left flank pain. Eleven days previously she had undergone left total knee arthroplasty. Following the orthopedic procedure she was placed on a 7-day course of low-molecular-weight heparin for deep venous thrombosis (DVT) prophylaxis. She had no history of DVT or blood clotting disorder. An abdominal CT scan was obtained in the emergency department and showed bilateral adrenal masses with imaging characteristics consistent with bilateral adrenal hemorrhage ( Fig. 68.1 ).

INVESTIGATIONS
Laboratory testing showed hyponatremia, high-normal serum potassium concentration, and low serum cortisol concentration ( Table 68.1 ). The next study obtained in the hospital was a 250-mcg cosyntropin stimulation test that showed serum cortisol concentrations of 5.3, 6.1, and 6.4 mcg/dL obtained at baseline and 30 and 60 minutes post-cosyntropin, respectively. Serum corticotropin, although indicated in this setting, was not measured.
| Biochemical Test | Result | Reference Range |
| Sodium, mEq/L Potassium, mEq/L Creatinine, mg/dL eGFR, mL/min per BSA 7:50 am serum cortisol, mcg/dL Aldosterone, ng/dL Plasma metanephrine, nmol/L Plasma normetanephrine, nmol/L | 121 4.9 0.9 >60 3.1 <1 0.31 1.09 | 135–145 3.6–5.2 0.6–1.1 >60 7–25 ≤21 ng/dL <0.5 <0.9 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree