Most patients with corticotropin (ACTH)-dependent Cushing syndrome (CS) will have an ACTH-secreting pituitary microadenoma. When the pituitary appears normal on magnetic resonance imaging (MRI), it is important to distinguish between ectopic and pituitary ACTH-dependent CS. Use of inferior petrosal sinus sampling (IPSS) can help localize the source (pituitary versus ectopic) of ACTH secretion. Pituitary-dependent CS is typically associated with mild to moderate CS, and 24-hour urinary free cortisol (UFC) excretion is typically 100–500 mcg and very rarely >1000 mcg. When patients with ACTH-dependent CS present with spontaneous hypokalemia and 24-hour UFC >1000 mcg, the clinician should suspect an ectopic ACTH-secreting tumor. A subset of patients with pituitary-dependent CS who have large pituitary adenomas demonstrate the clinical presentation that overlaps with ectopic ACTH secretion. Here we present a case of severe ACTH-dependent CS in a patient with negative MRI and IPSS suggesting a pituitary source, who was treated with bilateral adrenal cryoablation.
Case Report
The patient was a 69-year-old woman who was referred for management of ACTH-dependent CS. Evaluation was prompted by the new onset of symptoms of 3 months, duration that included progressive weakness with proximal myopathy, severe bilateral edema, uncontrolled hypertension, new-onset hypokalemia, cognitive decline, and several falls resulting in a fracture. She also noticed rounding of the face, thinning of the skin, and easy bruising. CS was suspected, and she was referred to our institution for further evaluation and management.
On physical examination, the patient was sitting in a wheelchair. Blood pressure was 150/82 mmHg, heart rate was 63 beats per minute, and weight was 108 kg. Her skin was found to be thin, with multiple bruises. She had moon facies, supraclavicular pads, and a mild dorsocervical pad. She had no striae. She had proximal myopathy on examination in both upper and lower extremities. Bilateral 3+ edema was noted.
At the time of evaluation, hypertension was treated with five drugs (spironolactone, metoprolol succinate, losartan, hydrochlorothiazide, and hydralazine), and hypokalemia was treated with 80 mEq of potassium chloride per day.
INVESTIGATIONS
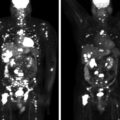
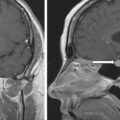
ACTH-dependent hypercortisolism was diagnosed ( Table 62.1 ). MRI of the pituitary gland was performed at that time and did not reveal a pituitary adenoma. Ectopic CS was suspected due to the rapid onset of symptoms and severity of hypercortisolism, especially in light of negative pituitary imaging. Computed tomography (CT) of the chest was obtained and demonstrated an indeterminate 9-mm lung nodule in the posterior lateral left lung base. This nodule was previously noted on a CT of the chest 3 years prior, but was smaller, measuring 6 mm. A gallium-68 (Ga-68) 1,4,7,10-tetraazacyclododecane-1,4,7,10-tetraacetic acid (DOTA)-octreotate (DOTATATE) positron emission tomography (PET)-CT scan was obtained and demonstrated no uptake in the 9-mm lung nodule. Given the negative localization workup, it was decided to proceed with IPSS that demonstrated a pituitary origin of ACTH secretion ( Box 62.1 ). Ultrasound of lower extremities was obtained and was negative for deep venous thrombosis.
| Biochemical Test | Result | Reference Range |
| 8 am serum cortisol, mcg/dL | 48 | 7–25 |
ACTH, pg/mL | 128 | 7.2–63 |
DHEA-S, mcg/dL | 86 | 9.7–159 |
24-Hour urine free cortisol, mcg | 803 | <45 |
Late night salivary cortisol, ng/dL | 2820, 1560 | <100 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree