Fig. 4.1
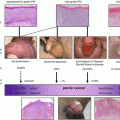
Lymphatic drainage in penile cancer. Anterior planar lymphoscintigraphy (a) shows drainage from the central injection site to both groins. On SPECT/CT (volume rendered, b and transversal slices c, d), inguinal sentinel nodes (lower dotted line) are clearly differentiated from second echelon iliac lymph nodes (upper dotted line)
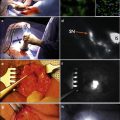
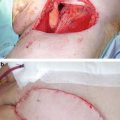
Surgery can be performed on the same or the next day. The markings on the skin are used to guide the incision, and a gamma probe is used to guide the surgeon to the sentinel node(s). The radio-guided procedure may be combined with the intraoperative use of blue dye, which is injected around the tumor for visual assistance a few minutes before the skin incision in the groin. Recently, as an alternative to blue dye, the use of a hybrid fluorescent and radioactive tracer (indocyanine green-99mTc-nanocolloid) has been studied, which combines acoustic gamma probe detection with live optical sentinel node visualization using a near-infrared camera [25].
If the sentinel node is tumor-positive after definitive histopathological examination, completion ipsilateral radical lymphadenectomy is done. Groins without tumor-positive sentinel nodes are managed with close surveillance, avoiding the lymphadenectomy-associated morbidity.
It is important to emphasize that a sentinel node procedure always needs to be preceded by a groin ultrasonography with fine needle aspiration cytology (FNAC) of suspicious nodes. Ultrasonography with FNAC can identify macroscopically tumor-positive nodes, which may be bypassed by the radioactive tracer due to obstruction of lymph flow by macroscopic metastases. In such cases, another lymph node which might be tumor-negative will falsely be identified as the sentinel node, potentially leading to a false negative procedure. Furthermore, when preoperative ultrasonography with FNAC identifies tumor-positive nodes, this obviates the need for DSNB on the affected side, and a radical inguinal lymph node dissection can be done directly [26, 27].
The accuracy of sentinel node biopsies depends on the experience of the team of surgeons and nuclear medicine physicians. In a pooled meta-analysis of 18 studies, the pooled sensitivity of sentinel node biopsy procedures was 88 % (false negative rate 12 %), but in experienced groups, sensitivities of 90–95 % are reported (false negative rate 5–10 %) [28]. It is important to realize that a modified inguinal lymph node dissection is also associated with false negatives, with a false-negative rate that is comparable to DSNB [29]. Complications of sentinel node biopsy occur in less than 5 % of explored groins, and almost all are transient and can be managed conservatively [21].
FDG-PET/CT
Over the past decades, positron emission tomography (PET) with 18F-fluorodeoxyglucose (FDG) has proven to be useful for the staging and follow-up of many types of cancer. FDG-PET is a functional imaging modality that can detect tumors and metastases based on increased uptake of glucose and FDG, resulting from their increased glycolytic activity. Modern PET scanners are combined with a CT (or MRI) scanner in one machine (PET/CT). The combination of functional PET data and anatomical information from CT has led to a higher accuracy and diagnostic confidence than separate PET and CT.
Penile cancers generally exhibit a high uptake of FDG, which makes FDG-PET/CT a potentially useful tool for staging of penile tumors (Fig. 4.2). Unlike palpation and anatomical imaging with CT, MRI, or ultrasound, FDG-PET/CT does not use lymph node size as the main criterion for malignancy. However, because of its limited spatial resolution, the sensitivity of PET drops progressively for metastases smaller than 8–10 mm, and lesions smaller than 4–5 mm are rarely detectable. False positive results can occur due to high uptake of FDG in inflammation, including reactive lymph nodes.
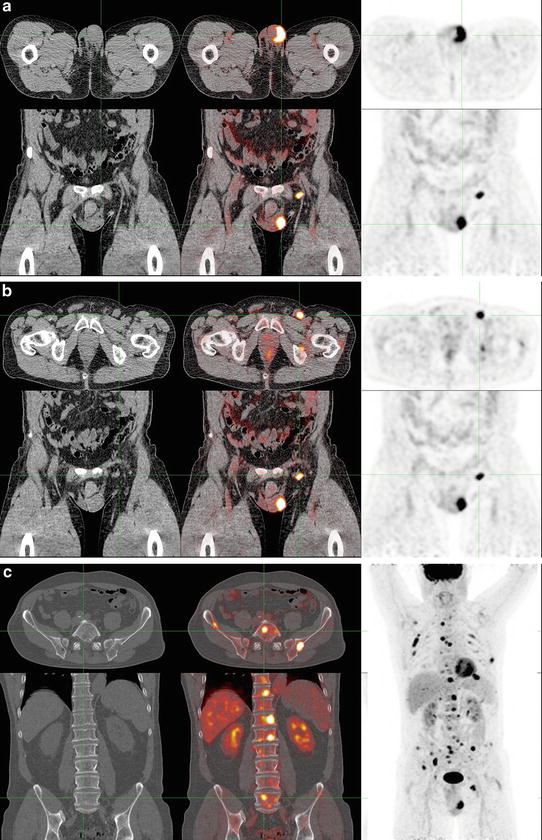

Fig. 4.2
FDG-PET/CT scan of a patient with penile cancer. The penile tumor exhibits high uptake of FDG (a). In the left groin, a prominent lymph node with high uptake of FDG is visualized (b), which is highly suspicious for metastasis. In addition, multiple bone metastases can be seen in the rest of the body (c)
The main characteristics of available studies about the accuracy of PET/CT for nodal staging of penile cancer are summarized in Table 4.1. The first study of FDG-PET/CT in 13 penile cancer patients reported a promising sensitivity of 80 % and specificity of 100 % for inguinal and obturator node metastases on a per-patient basis [30]. These results were confirmed in a larger study by Schlenker et al. (n = 35), who found a sensitivity of 88 % and specificity of 98 % for inguinal nodal metastases [31]. Souillac et al. studied 22 cN0 patients with PET/CT. They found a sensitivity of 75 % and specificity of 88 % [32]. However, in a study of 24 patients (42 cN0 groins) by our group, PET/CT detected only one out of five inguinal node metastases (sensitivity 20 %). Three false-positive results were found (specificity 92 %) [33]. The difference between these studies may be explained by differences in reference standard and initial risk stratification; some studies also included clinically node-positive patients.
Table 4.1
Characteristics of studies on accuracy of FDG-PET/CT for inguinal and pelvic staging of penile cancer
First author | Year | Initial risk stratification | n | cN-stage | n | Reference standard | Sensitivity | Specificity |
|---|---|---|---|---|---|---|---|---|
Inguinal staging | ||||||||
Scher [30] | 2005 | Susp. penile cancer | 10 | N/A | ILND/6 mo FU/Nonea | 80 % | 100 % | |
Susp. local recurrence | 2 | N/A | ||||||
Susp. ing. recurrence | 1 | N+ | ||||||
Leijte [33] | 2009 | T1-T2 | N0 | 19 | US-FNAC and DSNB | 20 % | 92 % | |
N+ unilat. | 5 | |||||||
Schlenker [31] | 2012 | Low-intermed. | 13 | N0 | 22 | ILND/24 mo FU | 88 % | 98 % |
High | 22 | N+ | 13 | |||||
Souillac [32] | 2012 | pT1b | 12 | N0 | 22 | mILND/rILND | 75 % | 88 % |
pT2 | 13 | N+ | 8 | 100 % | 100 % | |||
pT3 | 5 | |||||||
Pelvic staging | ||||||||
Graafland [34] | 2009 | N/A | N+ | 18 | PLND/12 mo FU | 91 % | 100 % | |