Tobacco
Richard J. O’Connor
INTRODUCTION
Regrettably, tobacco use remains one of the leading causes of death worldwide. It is projected to leave over 1 billion dead in the 21st century, after killing nearly 100 million during the course of the 20th century.1 Data from the Global Adult Tobacco Survey (GATS), which conducted representative household surveys in 14 low- and middle-income countries (Bangladesh, Brazil, China, Egypt, India, Mexico, Philippines, Poland, Russia, Thailand, Turkey, Ukraine, Uruguay, and Vietnam), suggest 41% of men and 5% of women across these countries currently smoke.2 Compare this to approximately 24% of men and 16% of women in the United States.3 A preponderance of the death and disease associated with tobacco use is associated with its combusted forms, particularly the cigarette. However, all forms of tobacco use have negative health consequences, the severity of which can vary among products. From the introduction of the mass-manufactured, mass-marketed cigarette (e.g., Camel in 1913), smoking rates grew, first among men then among women, and peaked in Western countries in the 1960s to 1970s, before beginning a steady decline.4 The smoking rate among US adults has dropped from its peak in 1965 of 42% to 19% in 2011.3 Per capita consumption has been dropping almost continuously since the 1960s, although the rate of decline has slowed since the early 2000s.5 Among youth, smoking rates have been in decline since the 1990s,6,7 although there is some evidence of growth in use of other forms of tobacco (e.g., cigars, water pipes, electronic cigarettes) in 2011 to 2012 that may be displacing cigarette use.8
Tobacco control policy interventions can impact both smoking prevalence and lung cancer incidence.9 For example, a recent analysis suggests that implementation of graphic health warnings in Canada in 1999 resulted in a significant reduction (up to 4.5 percentage points) in smoking prevalence over a decade.10 Increases in tobacco taxes have long been shown to reduce youth smoking initiation and to prompt more attempts to quit smoking.11 Evidence from state comparisons in the United States suggests that comprehensive tobacco control measures effectively implemented (such as in California and Massachusetts) can reduce lung cancer incidence.12 Indeed, Holford and colleagues13 have shown that since the seminal 1964 Report of the Surgeon General, an estimated 157 million years of life (approximately 20 years per person) have been saved by tobacco control activities in the United States over 50 years. That is, tobacco control activities are estimated to have averted 8 million premature deaths and extended mean life span by 19 to 20 years.13 However, the marketing of cigarettes has since shifted focus to the developing world, where smoking rates are on the increase. In an attempt to head off an epidemic of smoking and associated diseases, the World Health Organization initiated a public health treaty, the Framework Convention on Tobacco Control (FCTC), to coordinate international efforts to reduce tobacco use.14 The FCTC binds parties to enact measures to control the labeling and marketing of tobacco products, create a framework for testing and regulating product contents and emissions, combat smuggling and counterfeiting, and protect nonsmokers from secondhand smoke.15 To date, the FCTC has been ratified by more than 150 countries. The FCTC provides governments the opportunity to regulate the marketing, labeling, and contents/emissions of tobacco products, as well as control the global trade in tobacco products. In the United States, which is currently not a party to FCTC, the U.S. Food and Drug Administration (FDA) has, since 2009, had authority to regulate tobacco products and their marketing along similar lines.16
EPIDEMIOLOGY OF TOBACCO AND CANCER
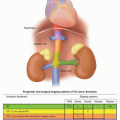
Linkages between tobacco use and cancers at various sites had been noted for several decades. In the late 1800s, it was believed that excessive cigar use created irritation that led to oral cancers.17 In the 1930s, German scientists began to establish links between cigarette smoking and lung cancers.18 However, it was not until the Doll and Hill19 and Wynder and Graham20 studies were published that the association was demonstrated in large samples and well-designed studies. Table 4.1 lists the cancers currently recognized by the U.S. Surgeon General as caused by smoking, along with their corresponding estimated mortality statistics.21,22,23 Of these, the most well-publicized link is between smoking and lung cancer. In a recent examination of National Health and Nutrition Examination Survey (NHANES) data, Jha24 showed a hazard ratio for lung cancer in smokers versus nonsmokers of 17.8 in women and 14.6 in men. However, smoking contributes substantially to overall cancer burden across multiple sites, including the oropharynx, cervix, and pancreas. Hazard ratios of 1.7 for women and 2.2 for men are seen for cancers other than in the lung in smokers versus nonsmokers.24 Emerging evidence also links smoking with breast cancer, although the data are as yet insufficient to make causal conclusions.23,25 Cancer risks associated with smoking, as well as outcomes and survival, depend on a number of factors. A common index of cancer risk is pack-years, or the number of packs of cigarettes smoked per day multiplied by the number of years smoked in the lifetime. In general, the higher the number of pack-years, the greater the cancer risk. Risks for lung cancer decline with smoking cessation, and the longer a former smoker remains off of cigarettes, the more the risk declines.26 However, excepting those smokers who quit with relatively few pack years accumulated (typically before age 40), cancer risk rarely approaches that of a never smoker.24,27
A recent study using several large cohort studies examined death rates and the relative risks associated with smoking and smoking cessation for 3 epochs (1959 to 1965, 1982 to 1988, and 2000 to 2010).27 Of most interest here is death from lung cancer. For men, the age-adjusted death rate from lung cancer increased from 1959 through 1965 to 1982 through1988, but then fell for 2000
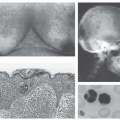
through 2010; for women, the age-adjusted death rate continued to rise over time, with the biggest increase between 1982 through 1988 to 2000 through 2010.27 In relative risk terms, the likelihood of dying from lung cancer given current smoking has increased from 2.73 to 12.65 to 25.66 among women, and 12.22 to 23.81 to 24.97 for men. Equivalent risks for former smokers increased from 1.3 to 3.85 to 6.7 among women, versus 3.48 to 7.41 to 6.75 for men. These and other analyses suggest that the cancer risks from smoking may have increased with time.27,28 The histologic subtypes of lung cancer seen in the US population have also shifted with time. Into the early 1980s, squamous cell carcinomas (SCC) were the most common manifestations of lung cancer. However, a rapid rise in adenocarcinomas has been noted, and by the 1990s, had overtaken SCC as the leading type of lung cancer.23
through 2010; for women, the age-adjusted death rate continued to rise over time, with the biggest increase between 1982 through 1988 to 2000 through 2010.27 In relative risk terms, the likelihood of dying from lung cancer given current smoking has increased from 2.73 to 12.65 to 25.66 among women, and 12.22 to 23.81 to 24.97 for men. Equivalent risks for former smokers increased from 1.3 to 3.85 to 6.7 among women, versus 3.48 to 7.41 to 6.75 for men. These and other analyses suggest that the cancer risks from smoking may have increased with time.27,28 The histologic subtypes of lung cancer seen in the US population have also shifted with time. Into the early 1980s, squamous cell carcinomas (SCC) were the most common manifestations of lung cancer. However, a rapid rise in adenocarcinomas has been noted, and by the 1990s, had overtaken SCC as the leading type of lung cancer.23
TABLE 4.1 Level of Evidence for Smoking-Attributable Cancers According to the United States Office of the Surgeon General by Cancer Site and Yearly Smoking-Attributable Mortality at Sites with Available Estimates, United States, 2004 | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||
Tobacco Use Behaviors
The level of tobacco exposure is ultimately driven by use behaviors, including the number of cigarettes smoked, the patterns of smoking on individual cigarettes, and the number of years smoked. The primary driver of smoking behavior is nicotine—the major addictive substance and primary reinforcer of continued smoking.29,30,31 Over time, smokers learn an acceptable level of nicotine intake that attains the beneficial effects they seek while avoiding negative withdrawal symptoms. Smokers can affect the amount of nicotine (and accompanying toxicants) they draw from a cigarette by altering the number of puffs taken, puff size, frequency, duration, and velocity (collectively referred to as smoking topography).32 Smokers tend to consume a relatively stable number of cigarettes per day and to smoke those cigarettes in a relatively consistent manner in order to maintain an acceptable level of nicotine in their system across the day.33 The number of cigarettes smoked per day and the smoking pattern of an individual may be influenced by the rate of nicotine metabolism.30 Nicotine is metabolized primarily to cotinine, which is further metabolized to trans-3′-hydroxycotinine (3HC), catalyzed by the liver cytochrome P450 2A6 enzyme.34 Functional polymorphisms in the genes coding for these enzymes allow for the identification of fast metabolizers, who have more rapid nicotine clearance and show greater cigarette intake and more intensive smoking topography profiles relative to normal or slow metabolizers.35,36,37 The ratio of 3HC to cotinine in plasma or saliva can be used as a reliable noninvasive phenotypic marker for CYP2A6 activity.38,39 CYP2A6 activity is known to vary across racial/ethnic groups, with those of African or Asian descent showing slower metabolism than those of Caucasian descent.40,41,42 Clinical trial data clearly show that the metabolite ratio can be used to predict success in quitting, and that the likelihood of quitting decreases as the ratio increases, such that slower metabolizers are more successful at achieving abstinence.37,41,43 Despite their addiction to nicotine, most smokers in Western countries report that they regret ever starting to smoke and want to quit smoking, and there is evidence for similar regret in developing countries as well.44,45,46 However, most smokers are unsuccessful in their attempts to quit smoking; the most effective evidence-based treatments increase the odds of quitting by 3 times, with 12-month cessation rates of approximately 40% relative to placebo.47
Evolution of Tobacco Products
Historically, tar was believed to be the main contributor to smoking-caused disease.48 It is important to note that tar is not a specific substance, but simply the collected particulate matter from cigarette smoke, less water and nicotine (in technical reports, it is often referred to as nicotine-free dry particulate matter). Soon after the first studies were done showing that painting mice with cigarette tar caused cancerous tumors, it was theorized that reducing tar yields of cigarettes might also reduce the disease burden of smoking.48 Concurrently, cigarette manufacturers were seeking to reassure their customers that their products were safe, that if hazardous compounds were identified they would be removed, and that product modifications could help to reduce risks.4,49,50,51 Indeed, in the United States and United Kingdom, average tar levels of cigarettes dropped dramatically from the 1960s through the 1990s, and have since leveled off.52,53 The European Union took the tar reduction mentality to heart in crafting maximum levels of tar in cigarettes that could be sold in member countries, beginning at 15 mg in 1992, then dropping to 12 mg in 1998, and 10 mg in 2005.54 Unfortunately, these reductions in tar yields have not translated into changes in disease risks among smokers.55 Despite initial optimism about these products, both laboratory-based and epidemiologic studies indicate neither an individual, nor a public health benefit from low-tar cigarettes as compared to full-flavor varieties.56,57,58 The health consequences of mistakenly accepting the purported benefits of lower tar and nicotine products have been significant. The increases in adenocarcinoma of the lung observed in the United States over recent decades may reflect changes made to the cigarette, such as filters, filter ventilation, and tobacco-specific nitrosamines (TSNA) in smoke produced by the relatively high amount of burley tobacco used in the typical US cigarette blend.23,59 Tobacco manufacturers engineered cigarettes be elastic; that is, cigarettes allow smokers to adjust their puffing patterns to regulate their intake of nicotine, regardless of how the cigarette might perform under the standard
testing conditions that drove the labeling and advertising of the products.55 Researchers have since come to determine that filter vents are the main design feature the industry relied on in creating elastic products.54,55,60,61 Vents facilitate taking larger puffs and also contribute to sensory perceptions, because they dilute the smoke with air.62 So, even with a larger puff, the same mass of toxins can seem less harsh and irritating because it is diluted by a proportionate amount of air, which may in turn underscore smokers’ beliefs that they are smoking safer cigarettes.62,63,64 Other smoke components (e.g., acetaldehyde, ammonia, minor tobacco alkaloids) and aspects of cigarette engineering (e.g., menthol, flavor additives) may further contribute to the addictiveness of cigarettes.65
testing conditions that drove the labeling and advertising of the products.55 Researchers have since come to determine that filter vents are the main design feature the industry relied on in creating elastic products.54,55,60,61 Vents facilitate taking larger puffs and also contribute to sensory perceptions, because they dilute the smoke with air.62 So, even with a larger puff, the same mass of toxins can seem less harsh and irritating because it is diluted by a proportionate amount of air, which may in turn underscore smokers’ beliefs that they are smoking safer cigarettes.62,63,64 Other smoke components (e.g., acetaldehyde, ammonia, minor tobacco alkaloids) and aspects of cigarette engineering (e.g., menthol, flavor additives) may further contribute to the addictiveness of cigarettes.65
Since the 1980s, manufacturers have introduced products that make more explicit claims about reduced health risks. Examples of modified cigarettelike products include Premier (RJ Reynolds), Eclipse (RJ Reynolds), Accord/Heatbar (Philip Morris), Omni (Vector Tobacco), and Advance (Brown and Williamson).66 In the 2000s, as evidence of reduced lung cancer incidence and coincident increases in snus use in Sweden appeared,67,68 manufacturers began to promote smokeless tobacco products as reduced harm alternatives. Most recently, electronic cigarettes, which vaporize a nicotine solution, have gained increasing popularity and generated concern among public health practitioners, particularly with regard to effects on youth.8,69,70 In the United States, the FDA has authority to authorize marketing claims about reduced risk, which an Institute of Medicine panel concluded should be based on extensive testing of abuse liability, likely health effects, and effects on the whole population.71
CARCINOGENS IN TOBACCO PRODUCTS AND PROCESSES OF CANCER DEVELOPMENT
Cigarette smoke has been identified as carcinogenic since the 1950s, and efforts have continued to identify specific carcinogens in smoke and smokeless tobacco products. The International Agency for Research on Cancer (IARC) has classified both cigarette smoke and smokeless tobacco as Group 1 carcinogens.72,73 IARC has also identified 72 measurable carcinogens in cigarette smoke where evidence is sufficient to classify them as Group 1 (carcinogenic to humans), 2A (probably carcinogenic to humans), or 2B (possibly carcinogenic to humans).72 The IARC list, in addition to data from the U.S. Environmental Protection Agency (EPA), the National Toxicology Program, and the National Institute for Occupational Safety and Health (NIOSH), informed the FDA’s development of a list of Harmful and Potentially Harmful Constituents (HPHC) in tobacco and tobacco smoke, which manufacturers will be required to report.74 Table 4.2 illustrates the carcinogens listed as HPHC alongside their carcinogenicity classifications by IARC or the EPA.
Compounds of Particular Concern
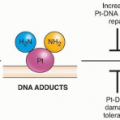
Research groups have listed components of cigarette smoke theorized to impact health risk, often relying on carcinogenic potency indices and relative concentrations in smoke.75,76 In these analyses, the N-nitrosamines, benzene, 1,3-butadiene, aromatic amines, and cadmium often rank highly. Polycyclic aromatic hydrocarbons (PAH), many of which are carcinogenic, consist of three or more fused aromatic rings resulting from incomplete combustion of organic (carbonaceous) materials, and are often found in coal tar, soot, broiled foods, and automobile engine exhaust.77 A compound of particular concern in cigarette smoke historically has been benzo(a)pyrene (BaP), which has substantial carcinogenic activity and is considered carcinogenic to humans by the IARC.77 In addition to PAH, other hydrocarbons found in significant quantities in cigarette smoke include benzene (a long-established cause of leukemia), 1,3-butadiene (a potent multiorgan carcinogen), naphthalene, and styrene. Carbonyl compounds, such as formaldehyde and acetaldehyde, are found in copious amounts in cigarette smoke, primarily coming from the combustion of sugars and cellulose.78 However, there are numerous other noncigarette exposures to these compounds, including endogenous formation during metabolism. Smoke contains a number of aromatic amines, such as known bladder carcinogens 2-aminonaphthalene and 4-aminobiphenyl, heterocyclic amines, and furans. Toxic metals, including beryllium, cadmium, lead, and polonium-210, are also present in cigarette smoke in measurable quantities,79,80 levels of which may depend in part on the region of the world where the tobacco was grown.81 Much attention has been focused on the N-nitrosamines, primarily because they are well-established carcinogens.82,83,84,85 Nitrosamines form through reactions of nitrite with amino groups. In tobacco, two compounds of concern are 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK), which is derived from nitrosation of nicotine, and N′-nitrosonornicotine (NNN), which is derived from nitrosation of nornicotine. Both of these compounds are tobacco specific. NNN and NNK primarily form during the curing process for tobacco, where the leaves are dried through contact with combustion gases from heat (flue) curing or microbial activity in air curing.78 NNK is known to be a potent lung carcinogen, but also shows tumor induction activity in the nasal cavity, the pancreas, and the liver, whereas NNN has been shown to induce tumors along the respiratory tract and esophagus in various animal models. Because they are produced in the curing process and transfer into smoke, rather than being formed by combustion, it is possible to reduce nitrosamines by changing curing and storage practices.78,86,87
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree