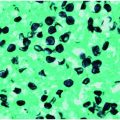
Figure 26.1 “Black dot tinea capitis” due to T. tonsurans. (Courtesy of Evelyn Koestenblatt.)
Gray patch ringworm is another form of tinea capitis, caused by the organisms Microsporum canis and M. audouinii. In this case the fungus is on the outside of the hair shaft (ectothrix invasion), causing it to have a grayish appearance. Some of these organisms produce a yellow-green fluorescence visible with a Wood’s (UV) lamp. Favus or tinea favosa is generally associated with malnutrition and poor hygiene, is rarely seen in the United States, and is most frequently due to T. schoenleinii. Clinically, favus appears as diffuse alopecia with yellow crusts or scutula, which are made up of hyphae, neutrophils, and skin debris. Microscopically, hyphae and air spaces are seen within the hair shaft.
The most common methods for diagnosing tinea capitis are KOH preparation and fungal culture. Collection of infected hair is necessary for diagnosis of tinea capitis. The hairs may be obtained for both KOH prep and culture in two ways: a scalpel blade or glass slide may be used to scrape the area or a soft toothbrush or moist gauze can be firmly rubbed over the involved scalp (Figure 26.2). The hairs are placed onto a glass slide and mixed with 10% to 20% KOH, a coverslip is applied, and the sample is then examined under a microscope. The hairs are inspected for evidence of fungal infection with spores either inside (endothrix) or outside (ectothrix) of the hair shaft. For culture, the hairs are gently placed on the surface of the fungal media for a period of several weeks. Only the specimen should be placed inside of the media tube.
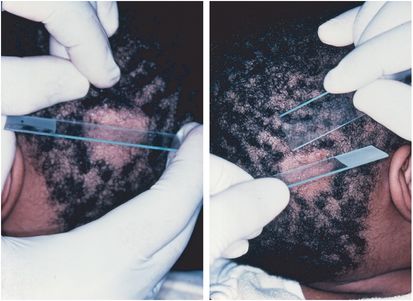
Figure 26.2 Tinea capitis techniques for collecting hair for KOH and culture. (Courtesy of Evelyn Koestenblatt.)
The gold standard of therapy for tinea capitis is oral griseofulvin. Topical therapy is most often unsuccessful because the medication cannot penetrate the hair follicle. Griseofulvin is usually given to children in conjunction with a fatty meal which stabilizes the gastric pH. The use of a warm compress to induce sweating and ultimately cutaneous excretion of the drug may also improve efficacy.
For patients who fail therapy with griseofulvin or cannot tolerate the medication, treatment with itraconazole (Sporanox), fluconazole (Diflucan), or terbinafine (Lamisil) is an option (Table 26.1). Terbinafine is an accepted alternative first-line agent for patients suffering from tinea capitas which is suspected or found to be caused by Trichophyton. Terbinafine may also be used for Microsporum infections but requies higher and longer dosing. In addition, brushes, combs, hats, hair ribbons, barrettes, and bed linen should be thoroughly washed. Children and caretakers of patients may be asymptomatic carriers of infection and ultimately sources for reinfection which necessitates further evaluation and the use of 2.5% selenium sulfide or 2% ketoconazole shampoo three times per week for at least 5 minutes by all family members to reduce the spread of infectious spores.
| Griseofulvin | Terbinafine | Itraconazole | Fluconazole |
|---|---|---|---|
| 20–25 mg/kg/d for 6–8 weeks (liquid microsize) | 62.5 mg/d ≤20 kg 125 mg/d 20–40 kg 250 mg/d >40 kg For 2–4 weeks | 5 mg/kg/d for 4–8 weeks | 6 mg/kg/d for 3–6 weeks |
Tinea corporis
Tinea corporis (Figures 26.3 and 26.4) refers to dermatophycosis of the glabrous skin. The infection may present as sharply demarcated annular lesions with a scaly border, bullous lesions, granulomatous eruptions, pustular lesions, psoriasiform plaques, and/or verrucous lesions. The disease is most prevalent in tropical areas but may be found across the world. In the United States, T. rubrum is the most common etiologic agent of tinea corporis. T. mentagrophytes and M. canis are also common. Infections caused by M. canis and some strains of T. mentagrophytes typically present with multiple lesions and are often more inflammatory and symptomatic than those caused by T. rubrum. Tinea corporis may also be seen in caretakers of children suffering from black dot tinea capitis due to T. tonsurans.
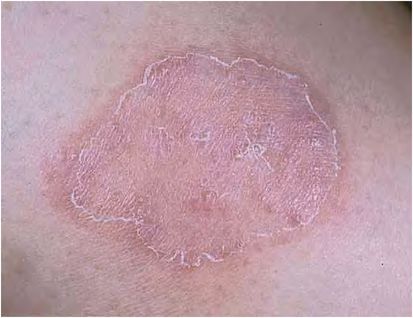
Figure 26.3 Tinea corporis. (Courtesy of Evelyn Koestenblatt.)
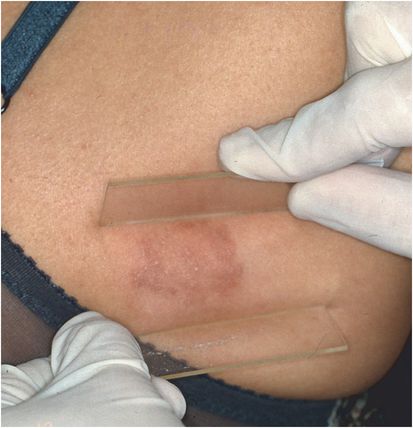
Figure 26.4 Erythematous tinea corporis with small pustules. (Courtesy of Evelyn Koestenblatt.)
Tinea cruris
Tinea cruris refers to a dermatophyte infection of the groin, including the suprapubic areas, proximal medial thighs, perineum, gluteal cleft, and buttocks. Infection is more often seen in men than women and is commonly caused by T. rubrum, T. mentagrophytes, and E. floccosum. Women more often suffer from candidiasis than tinea cruris.
Tinea pedis
Athlete’s foot or tinea pedis is the most common fungal infection (Figure 26.5). The moisture, friction, maceration, heat, darkness, and occlusion present in the feet are perfect for fungal growth. T. rubrum is the most common etiologic agent and causes a “moccasin” distribution of scale and erythema. T. rubrum is associated with a familial autosomal-dominant predisposition to this type of infection. Dermatophytosis occurring between the toes is referred to as interdigital tinea pedis. T. mentagrophytes, T. rubrum, or E. floccosum may be recovered with or without bacterial organisms and/or yeast. T. mentagrophytes may also cause a vesicular-type tinea pedis characterized by vesicles with serous exudate on the plantar surface.
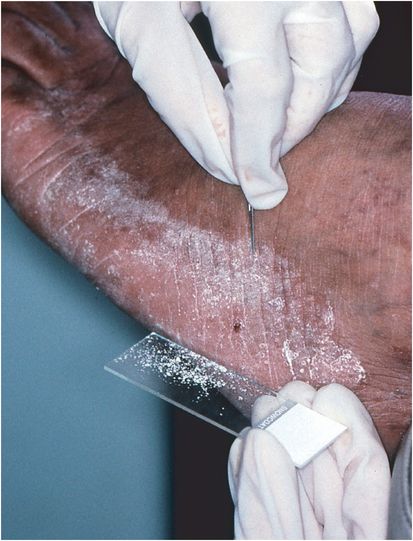
Figure 26.5 Moccasin type tinea pedis. Scrape the active border with a #15 blade for KOH preparation and culture. (Courtesy of Evelyn Koestenblatt.)
Tinea manuum
The patients commonly have dermatophycosis of both feet and one hand. Tinea manuum presents as a fine scale with some erythema covering the surface of the palm, like the feet; T. rubrum is usually recovered.
Tinea faciei and tinea barbae
Tinea faciei occurs in women and children generally on the upper lip and chin (involvement of similar area in men is termed tinea barbae) and is frequently acquired from pets (Figure 26.6). T. rubrum, T. mentagrophytes, and M. canis are typically recovered.
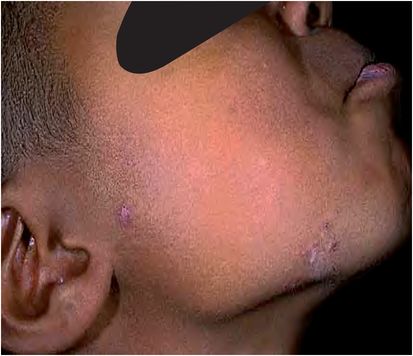
Figure 26.6 Tinea faciei. (Courtesy of Evelyn Koestenblatt.)
Tinea barbae or ringworm of the beard is seen in men and associated with exposure to animals (cattle, horses, cats, and dogs). The inflammatory type causes a deep, nodular, pyogenic reaction. T. mentagrophytes and T. verrucosum tend to cause this kerion-like response, whereas T. violaceum and T. rubrum usually cause a more superficial infection with scaling and alopecia. Extracted hairs are necessary for diagnosis by KOH preparation and culture. In some instances biopsy may be necessary to rule out other dermatoses. Given the organisms affect the hair, oral antifungal therapy is necessary as topical therapies will not adequately penetrate the hair follicle.
Dermatophytid (id) reactions
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree