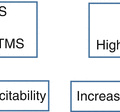
Fig. 25.1
The Scandinavian Team Arthritis Register-European Team Initiative for Care Research (STAR-ETIC) framework of arthritis rehabilitation according to Klokkerud et al. [3]
Rehabilitation Goals
Geriatric medicine aims at an improvement of functional deficits to avoid disability and delay the need for nursing for as long as possible [4]. Patient education and patient training are important to enhance the knowledge of the disease and its management possibilities. The goal of remission in the sense of “restitutio ad integrum” is illusory due to the chronic disease and frequent comorbidities of the patients as well as due to the limited future time perspective [4].
Interdisciplinary Rehabilitation Team
The attending physician (e.g. the rheumatologist, the geriatrician, the orthopaedic surgeon) should evaluate the older patient in collaboration with the entire interdisciplinary rehabilitation team of medical specialists and non-medical professionals and prescribe a comprehensive treatment programme that aims to preserve and restore function [5]. Such a programme offers the geriatric patient the best opportunity to increase physical skills and function [5].
Interventions Before Surgery
The elderly orthopaedic patient should be instructed to perform breathing exercises to prevent pulmonary complications and active lower limb exercises to maintain good circulation and joint mobility and to do functional exercises for mobilisation in and out of bed [5].
Interventions Postoperatively
The interdisciplinary rehabilitation team has to facilitate early resumption of active exercises and self-care tasks and to discourage prolonged bed rest (“bed is bad”) [4] and dependency on nursing staff and family members [5]. Physical and occupational therapy should be provided to restore mobility and self-care functions [5]. Notably, physical therapy (e.g. electrotherapy, hydrotherapy, thermotherapy, massages and lymphatic drainage) can help to reduce the amount of medication needed and thereby to avoid severe side effects [4]. Occupational therapy aims to train activities of daily living (e.g. washing, dressing and eating), including exercises to enhance fine motor skills of the fingers, strengthening exercises, sensitivity training, joint protection and the provision of aids and remedies [4]. When planning discharge, the home environment should be assessed and modifications recommended to reduce the risk of falls and to ensure independent functioning to the extent possible. As soon as the rehabilitation goals have been obtained, the patient should be discharged from the hospital, but additional therapy in terms of rehabilitation aftercare may be required, either at home or at an outpatient facility [5].
Place of Treatment
Rehabilitation interventions are not only to be carried out in the clinical context (outpatient or inpatient) but also at the patient’s home or in a nursing home. In recent studies, home-based rehabilitation provided the same or even higher gains regarding function, cognition, quality of life and patient satisfaction compared to inpatient rehabilitation.
Assessments
The comprehensive geriatric assessment encompasses the somatic, cognitive, emotional and social resources as well as functional deficits of the patient. The assessment of the baseline status of an older patient with a rheumatic disease should be conducted as detailed as needed. It may include a medical examination, laboratory assessments, radiography/imaging of the joints, an inquiry of the patient’s history, mobility tests, assessments of function in everyday life and well-being as well as the assessment of the socio-demographic and living background of the patient. Several assessments and patient questionnaires are available for the different matters of interests.
Pain, fatigue, daily activities, physical function, quality of life, coping, motivation, goal attainment, mental health and participation are the domains that are most central for evaluating the effects of rehabilitation.
Treatment Risks and Barriers
Comorbid conditions, such as cardiovascular diseases, impaired motor and cognitive functioning, geriatric problems, such as sarcopenia and frailty, and the decline of social support and income as important resources to cope with the disease may complicate disease management strategies and limit the goals of rehabilitation programmes in elderly patients. Hence, treatment interventions have to be checked for appropriateness for people at an advanced age and must be adapted to their individual cognitive or health conditions as well as to their living background.
25.3 Rehab Interventions: State of the Art in Selected Rheumatic Diseases
The rheumatic diseases which occur most often in elderly patients include osteoarthritis, rheumatoid arthritis, polymyalgia rheumatica, giant cell arteritis (arteritis temporalis), crystalline arthropathy (gout and pseudogout), fibromyalgia, the Sjögren’s syndrome [1], systemic lupus erythematosus and ankylosing spondylitis.
25.3.1 Osteoarthritis
Osteoarthritis (OA) is the most prevalent rheumatic disease with the knees being the most commonly affected joints. According to the EULAR recommendations [6], treatment of OA should be based on the localization of OA and various risk factors (age, sex, comorbidity, obesity). For the planning of interventions, the presence of inflammation, severity of structural change, level of pain and restriction of daily activities are relevant [6].
Exercise is an important non-pharmacological treatment for symptomatic OA and seems to be effective in terms of pain and function [7]. Especially aerobic and strengthening exercise as well as weight reduction improved physical function and reduced pain in patients with OA of the knee [8]. Additionally, positive effects of proprioceptive exercises and balance training have recently been shown [9]. Manual therapy combined with exercises is also recommended in the disease management of patients with OA. Pharmacological interventions encompass non-steroidal anti-inflammatory drugs (NSAIDs), COX-2 inhibitors, topical NSAIDs, topical capsaicin and chondroitin sulphate [7]. In addition to exercise and medications, adjunctive interventions include thermal therapies (e.g. heat, cold and ultrasound), transcutaneous electrical nerve stimulation (TENS), pulsed electromagnetic field therapy, laser therapy and electrical (galvanic) stimulation [7]. For acupuncture, TENS and low-level laser therapy, moderate-quality evidence with respect to pain reduction is reported [8]. In addition to enhancing the functional status, the improvement of psychological outcomes is also an essential factor in the treatment of OA. Behavioural interventions, like patient education and behavioural change techniques, lead to better psychological outcomes and a moderate pain reduction [7]. In the sense of a holistic biopsychosocial model, walking aids (e.g. a walking stick, walking frames), assistive technology and adaptations at home (e.g. handrails for stairs, walk-in shower, heightened chairs, beds and toilet seats) should be considered to increase the patients’ independency and participation [6].
25.3.2 Gout
Today, gout patients are more clinically complex than in the past, due to various combinations of advanced age, comorbidities, drug-drug interactions and refractory tophaceous disease [10]. The disease is characterised by deposition of monosodium urate crystals in and around joints and soft tissues, resulting in painful inflammation [11]. Gout is associated with significant morbidity and mortality from both intra- and extra-articular complications and has an increased incidence in the elderly. Imaging may be helpful in making a firm diagnosis since clinical presentation in the elderly may differ from that in the younger patients.
Following evidence-based recommendations [12], specific risk factors, clinical phase and general risk factors should be considered in the treatment of gout. A comprehensive treatment of gout requires non-pharmacological modalities as well as pharmacological treatments. Patient education and appropriate lifestyle counselling, regarding weight loss in the case of overweight, low animal purine diet and reduced alcohol consumption, are core aspects of the management of gout [12]. Dietary interventions refer to an inclusion of skimmed milk and/or low-fat yoghurt, soy beans and vegetable sources of protein; limited intake of high-purine foods and red meat; avoidance of liver, kidneys, shellfish and yeast extracts; and an overall restriction of protein intake [13]. Patients with gout and a history of urolithiasis should be encouraged to drink more than 2 litres of water per day to avoid dehydration [13]. This is particularly important for all older persons. Herbal remedies should not be taken without medical consultation [13]. According to physical exercise, trauma to joints and intense physical exercise should be avoided, whereas moderate physical exercise should be encouraged [13]. Xanthine oxidase inhibitor therapy with either allopurinol or febuxostat is recommended as the first-line pharmacologic urate-lowering therapy approach in (chronic) gout. Medications that are commonly used in the treatment of acute gout include oral non-steroidal anti-inflammatory drugs (NSAIDs), colchicine, oral glucocorticoids and the injection of glucocorticoids into the affected joint [11]. In addition to the pharmacological treatment of acute gout, ice packs as well as elevating and resting the affected joint have been suggested to reduce the pain [13].
25.3.3 Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a chronic inflammatory autoimmune disease characterised by joint swelling, joint tenderness and destruction of synovial joints (see Fig. 25.2), often leading to severe disability and premature mortality [14]. For people with newly diagnosed rheumatoid arthritis, treatment should follow the model of the patient-centred standards of care for RA in Europe [15]. This is especially true for people with late-onset rheumatoid arthritis (LORA) that first occurs in the age of 65 years and older (approx. 30% of all RA patients) [4].
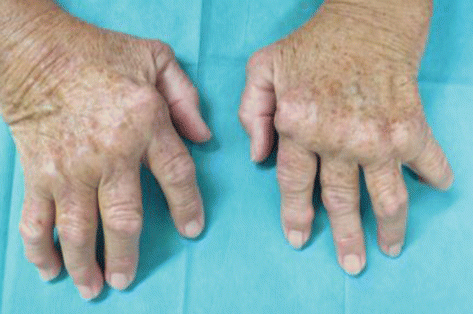

Fig. 25.2
Hands of a 70-year-old woman suffering from seropositive rheumatoid arthritis showing severe ulnar deviation in the metacarpophalangeal joints
The American College of Rheumatology (ACR) guideline for the treatment of RA [16] covers the use of traditional disease-modifying antirheumatic drugs (DMARDs), biologic agents and glucocorticoids in early (<6 months) and established (≥6 months) RA. Besides pharmacological treatment, regular exercise is one of the cornerstones of care in RA. Physical activity and exercise have numerous health benefits in patients with RA, e.g. improved joint health, physical function, mobility and psychological well-being as well as reduced rheumatoid cachexia and fatigue, without aggravating symptoms or inducing further joint damage. According to a recent review [17], long-term land-based aerobic exercise (e.g. bicycle ergometer, cycling or jogging) and muscle strengthening exercise (e.g. rubber expanders, circuit interval training) of moderate to high intensity reduced activity limitations and improved both cardiorespiratory fitness (i.e. oxygen uptake) and muscle strength, while short-term aerobic exercise increased cardiorespiratory fitness only. A review of the effects of rehabilitation recently stated that physical therapy (PT) and occupational therapy (OT) significantly reduce pain in RA patients. Furthermore, grip strength in various grip types (power grip, key pinch, precision pinch and tripod pinch) improved through hand exercise therapy (including resistance and/or active range of motion exercises) without having adverse effects on pain or disease activity [18]. With regard to the intervention content, there is some evidence in favour of a longer therapy duration and a higher therapy intensity [18]. According to a Cochrane review [19], physical activity and psychosocial interventions provided benefits in relation to self-reported fatigue in adults with RA.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree