Fig. 28.1
Ultrasound image of Achilles tendon degeneration
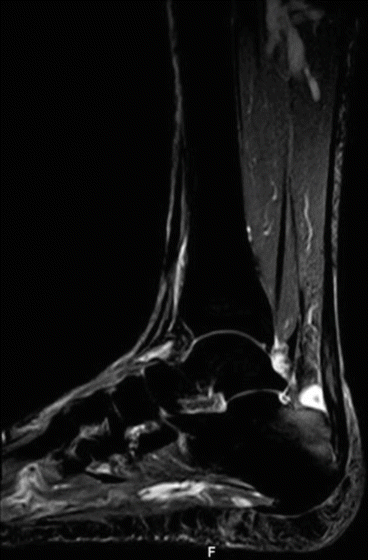
Fig. 28.2
MRI of non-insertional Achilles tendinopathy and bone marrow edema of the calcaneum
Several studies show that 16% of the general population and about 20% of elderly hospitals and community populations are affected by tendon pain. The most frequent symptoms that lead to tendinopathies are pain and loss of function.
Histopathologically, tendinopathies are related to unsuccessful healing response, represented by altered tenocyte proliferation, disruption and impaired organization of collagen fibers, increase in non-collagenous matrix, and neovascularization. In the chronic stage of tendinopathy, inflammation is absent or minimal; these findings may indicate that inflammation could play a role in the beginning, but not in the progression of the disease process [2].
During aging intrinsic and extrinsic factors influence biological environment and the capability of tendon to adapt itself to mechanical stimuli. Therefore, tendons show the typical macroscopic and microscopic aspects that are possible to observe in elderly in the major periarticular structure such as the shoulder, hip, knee, and foot [3].
Particularly, aging is often related to estrogen deficiency in postmenopausal women, obesity and diabetes, dysthyroidism, hypercholesterolemia, hyperuricemia, and other rare congenital metabolism disorders often involved in tendon degeneration. The presence of estrogen receptors in tenocytes has been demonstrated in human and animal trials, and these findings indicate that tenocytes are influenced by circulating estrogen level. In postmenopause, the reduction of blood estrogen is linked to the reduction in tensile strength; decrease in collagen synthesis, fiber diameter, and density; and increase degradation in tendon tissue. Hormone replacement therapy (HRT) with exogenous estrogens may improve tendon structure by preserving collagen fiber diameter. Furthermore, estrogen positively influences morphology and biomechanical properties of tendon in postmenopausal women. On the other hand, estrogen stimulation in younger women seems to have negative effects on tendons. In fact, in a study performed in young women, oral contraceptive user group was found to have lower collagen synthesis rate, compared to control women at the same age [4].
As mentioned above, a pathological condition often related to aging is diabetes mellitus type 2. Tendon alterations in diabetes are due to an excess of advanced glycation end products (AGEs) that are able to form covalent cross-link within fibers of collagen that alters their structure and consequently the capacity to respond to mechanical stimuli.
Obesity, particularly frequent in older and sedentary people, expose weight-bearing tendons to overuse due to the higher loads related to increasing adiposity. Moreover adipose tissue is an endocrine and signaling organ that can release hormones and peptides able to modify directly tendon structure. Particularly, adipokines modulate cytokines, prostanoids, and metalloproteinase production that cause a persistent low grade of inflammation that intensifies the detrimental effect of overuse on tendon.
Dysregulation of thyroid hormones, another disease not rarely observed in elderly, contributes to the genesis of musculoskeletal pathologies. Hypothyroidism can be related to the onset of calcific tendinopathies due to the reduction of oxygenation with consequent metaplasia that may cause calcium deposition, especially in rotator cuff tendons [5].
Extrinsic factors such as sport activities, physical loading, occupation, and environmental conditions could affect anatomo-physiological and biological characteristics of the tendon.
Correct mechanical loading is useful to tendons to stimulate their anabolic processes and also to compensate the effects of aging. On the other hand, extreme mechanical loading, immobilization, and disuse are harmful to tendons by stimulating catabolic processes such as matrix degradation and by modifying collagen synthesis, collagen organization, cellularity, vascularity, proteoglycan content, tear density, and mechanical properties.
Preclinical and clinical studies have shown that discontinuing activity negatively influences morphology and structure of the tendon, whether there are differences in training or detraining protocols, in the study design, in the types of tendons, in subjects, or in the experimental setting involved. Therefore, the authors suggested that after a period of sudden detraining (such as after an injury) physical activity should be restarted with caution and with appropriate rehabilitation programs [6].
In people affected by tendinopathies, eccentric exercise programs are widely used in the rehabilitation of Achilles tendon midportion and patellar tendon injuries with a successful outcome. Particularly in elderly, it has been shown a general preservation of eccentric strength compared to concentric strength. High-intensity resistance training, including eccentric exercises, revealed an increase muscle mass and strength in contractions comparing to traditional training protocol [7].
Therefore it’s feasible that a correct eccentric exercise protocol may be promising in the treatment and also in the prevention of tendon disorders in elderly.
28.2 Painful Shoulder in Elderly
Shoulder pain is the third most common musculoskeletal complaint in primary care physicians’ offices with high prevalence among the fourth to the sixth decade.
According to population surveys, shoulder pain affects 18–26% of adults; it is the most common regional pain syndromes. Symptoms can be persistent and disabling in terms of an individual’s ability to carry out daily activities both at home and in the workplace. There are also substantial economic costs involved, with increased demands on health care, impaired work performance, substantial sickness absence, and early retirement or job loss [8].
Common shoulder conditions in elderly patients include rotator cuff tendinopathy, rotator cuff tear, adhesive capsulitis (“frozen shoulder”), and glenohumeral arthritis.
Diagnosis is mainly clinical. Radiographs generally may be normal. Magnetic resonance and ultrasound are the most used diagnostic tools. Conservative treatments include rest, ice, topical analgesics, a short course of nonsteroidal anti-inflammatory drugs (NSAIDs), subacromial corticosteroid injections, and intra-articular hyaluronic acid (HA) injections [9]. HA is a component of the synovial fluid and is crucial for the lubrification and chondroprotection of joints. Several authors suggest that intra-articular injections of hyaluronic acid reduce inflammation and pain and improve joint function. Furthermore, HA stimulates type B synoviocytes producing endogenous HA with a chondroprotective effects on the whole joint [10, 11].
One of the most frequent causes of shoulder pain in elderly patients is shoulder osteoarthritis, which is a gradual, progressive, mechanical, and biochemical breakdown of the articular cartilage and other joint tissues, including bone and joint capsule. Several risk factors can lead to shoulder osteoarthritis, including aging, genetics, sex, weight, joint infection, history of shoulder dislocation, and previous injury. The loss of shoulder function can lead to depression, activity limitations, and job-performance problems.
Typical presenting symptom is progressive, activity related pain that is deep in the joint and often localized around the deltoid region and posteriorly. As the disease progresses, night pain becomes more common. Patients complain reduction of the shoulder range of movement, with the loss of the extra rotation and abduction in both active and passive mobilization [12, 13].
Therefore, rehabilitative goals are the restoration of strength and flexibility of the shoulder musculature on the upper thoracic, neck, and scapular muscle groups, including also the rotator cuff, arm, forearm, wrist, and hand. Isometric contraction exercises with normal range of motion in shoulder joint have a leading role in rehabilitation because these exercises will not only produce more strength in the stabilizers shoulder muscles groups but also help to minimize joint damage, reducing the inflammation and pain. The satisfactory outcome of flexibility exercises will be confirmed by the amplitude of mechanical bone blockade that is achieved by the size of glenohumeral deformity and osteophyte generation.
Osteoarthritis may lead to rotator cuff tendinopathy. However, rotator cuff tendinopathy may result from several factors like an alteration of tendon’s structure related to overloading or underloading, hormonal and/or metabolic impairment, reduction of subacromial space, and instability of the humeral head. The entirety of rotator cuff is crucial in maintaining normal humeral head position in the glenoid during elevation, flexion, and abduction movements, producing compressive forces that stabilize the humerus against the glenoid, giving a dynamic stabilization of the glenohumeral joint. In chronic rotator cuff tendinopathy, due to pain and disuse, muscles of the rotator cuff may become weak and can fatigue earlier, leading to changes in shoulder kinematics. Weakness of the rotator cuff, especially infraspinatus, reduces this compressive force, promoting instability. This instability may lead the humeral head to an abnormal range of motion out of the glenoid center, causing impingement and tendinopathy.
Generally, pain occurs in the posterolateral and deltoid region, especially when the patient performs eccentric contractions, during sleeping on the affected side or performing overhead activities with the arm abducted more than 90°. Provocative passive movements, such as the Neer and Hawkins-Kennedy tests, increase the pain. Appropriate balance of the muscles surrounding the shoulder is fundamental for flexibility and strength. Therefore, a deficit in flexibility or strength in an agonistic muscle must be compensated for by the antagonist ones, leading to dysfunction. Consequently, the restoration of the appropriate strength and flexibility in both agonistic and antagonist muscles is very important in shoulder rehabilitation [14].
In the first phase, rehabilitation should be gentle and passive with prolonged stretchability to restore flexibility of the posterior capsule, muscle balance, and scapulothoracic and glenohumeral muscular control and stability. Patients should be well educated to prevent incorrect postures and movements to avoid the occurrence of any exacerbating activities. Pendulum exercises, wall walking, or towel exercises are very effective in improving range of motion and in facilitating optimal motor pattern. Capsular stretching, pectoralis minor stretching as well as reducing upper trapezius activation are recommended to improve soft tissue tightness because it can cause anterior and superior humeral head migration, resulting in impingement. Very important in this early stage is the restoration of shoulder kinematics using wall push-ups and biofeedback exercises because an altered motion may lead to glenohumeral joint instability.
The next phase of treatment is the muscle strengthening. This phase should be performed in a pain-free range of motion. Therefore, before beginning a strengthening program, it is important to identify tight or short muscles and if flexibility was restored. Strengthening should begin with the muscles that support the shoulder. We can use shoulder shrugs, rowing, and push-ups for strengthening both agonistic and antagonist muscles, because only a proper balance in strength of these two groups helps return range of motion and the normal kinematics between the scapula and the glenohumeral joint.
Specific strengthening exercises of the serratus anterior, typically including supine protractions and wall push-up exercises, should be used in the early stages of rehabilitation, while dynamic hugs and push-up varieties are commonly utilized in later stages of rehabilitation. Strength exercises for rotator cuff tendinopathy should be initiated with low-load activities and progressing as patient comfort permits [15, 16]. An effective treatment strategy that leads to a tendon strengthening is also the eccentric training [17].
The last phase is the proprioceptive training. The most important result of this phase is the restoration of neuromuscular coordination of the muscles that provides a synergistic activation of muscles. The proprioceptive phase should begin with closed kinetic chain exercises.
Usually, shoulder pain in elderly people is associated also with an adhesive capsulitis of the shoulder, which is a common condition characterized by spontaneous onset of pain, progressive restriction of movement of the shoulder, and disability that restricts activities of daily living, work, and leisure. The disease is characterized by three stages including the painful phase, the freezing or adhesive phase, and the healing phase. This condition is more frequent in women after the age of 50 years and involves the nondominant shoulder too. The primary etiology is still unknown, but it is associated with different secondary causes, like immobilization, diabetes, hypothyroidism, autoimmune diseases, and treatment of breast cancer.
Contraction and fibrosis of the capsule lead to pain and stiffness of the joint when the capsule is stretched during typical shoulder range of motion [18].
Generally, the treatment goals are focused to decrease pain and inflammation and increase shoulder range of motion. Rehabilitation protocol is based on stretching, strengthening, pendulum, pulley, and shoulder wheel and wall-climbing exercises, overhead stretches, and crossed adduction of the affected arm. It is mandatory to start rehabilitation exercises as soon as possible because it helps to reduce pain, to improve the pain-free range of motion, and to prevent further joint capsule contraction. The next step of the treatment is a graduated exercise program that leads to rotator cuff muscles and periscapular stabilizers strengthening. To maintain an adequate range of motions and to prevent recurrence, every patient should continue the exercise program at home [19, 20].
Also an excessive thoracic kyphosis is considered a predisposing factor for shoulder pain, but, to date, the relationship between these two conditions is uncertainty. It has been demonstrated that older adults with a large thoracic kyphosis had reduced arm elevation, but further researches are needed to investigate the nature of the link between shoulder pain and thoracic spine posture and to examine the specific value of thoracic postural rehabilitation in populations with painful shoulders.
28.3 Osteoarthritis
Osteoarthritis (OA) is a chronic disease that causes pain and substantial disability. It primarily affects the hip, knee, and hands (but also the shoulder and spine). This condition limits severely the daily activities and quality of life for many individuals in industrialized countries [21]. It affects at least 20 million Americans, a number that is expected to double over the next two decades [22]. Hip and knee osteoarthritis (OA) are the main causes of the poor health of older people worldwide [23] and are considered to be the most serious musculoskeletal disorders [24, 25].
Therefore, the effective management of hip and knee OA is a priority of the World Health Organization.
Osteoarthritis is a disorder of the whole joint and affects the cartilage, synovial tissue, subchondral bone, ligaments, and muscles. The critical occurrence in OA is the damage of cartilage, caused mainly by the degradation of type II collagen [26]. This process, at the cellular level, is mediated by releasing and responding to inflammatory mediators. OA often requires decades to develop and has a range of associated risk factors that it is possible to divide in general and local ones. General risk factors enclose older age, female gender, obesity (particularly in knee and hip OA), genetics, and muscle weakness. Local risk factors include an altered distribution of loads on the articular surfaces (e.g., the varus-valgus knee, evolution of congenital hip dysplasia, impingement hip syndrome, etc.), previous joint injuries, and articular alterations produced by inflammatory or septic arthritis.
Clinically patients complain about joint pain related to activity, stiffness [27], and, in severe OA, joint deformity.
Idiopathic osteoarthritis recognizes a genetic predisposition and it is typical for elderly. However, OA can also affect young people secondary to trauma, malformations, metabolic and rheumatic diseases, repetitive works (using vibrating tools, repetitive operations under load, or no physiological positions), etc.
Diagnosis is based on clinical and instrumental evaluation. To date, the most commonly used classification of hip and knee OA is the Kellgren and Lawrence grade [28] (Figs. 28.3 and 28.4), although it has several criticisms and radiographic signs of osteoarthritis not always are closely associated with pain [29]. However, in addition to correct clinical staging, it is also important to assess the functional level and the quality of life of patients affected by osteoarthritis. The American College of Rheumatology recommends to administer several scales to better stage the pathology such as Harris Hip Score, Oxford Hip Score, WOMAC, Hip disability and Osteoarthritis Outcome Score (HOOS), and Knee injury and Osteoarthritis Outcome Score (KOOS).
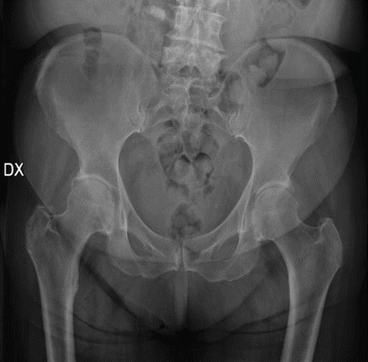
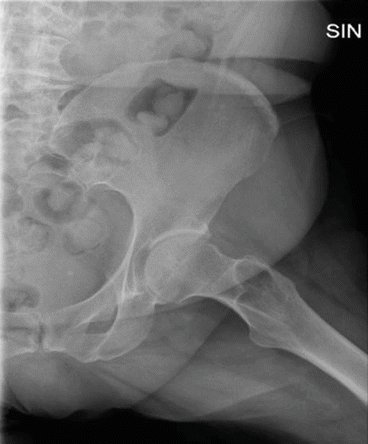

Fig. 28.3
Standard radiographic anteroposterior pelvis projection showing bilateral reduction of the hip joint space with subchondral sclerosis and initial deformities of the femoral head

Fig. 28.4
Standard radiographic lateral view of the left hip joint showing signs of osteoarthritis
The management of osteoarthritis is still heterogeneous [30].
The treatment’s options for osteoarthritis include conservative and surgical interventions. Conservative treatments aim to prevent progression and reduce symptoms such as joint pain and impairment of functions. Pharmacologic therapies and non-pharmacologic modalities are commonly used for the initial treatment of OA. Pharmacologic therapies include acetaminophen and topical and oral nonsteroidal anti-inflammatory drugs (NSAIDs). Although NSAIDs are effective in relieving pain and improving function, they should only be used in short term because of side effects [31]. Topical and systemic corticosteroids, opioids, and intra-articular drug injection may be useful. The effects of intra-articular injections of corticosteroids, as regards decreasing joint pain, are less effective over time than the hyaluronic acid injections. To date, evidences about the effectiveness of intra-articular injections of PRP are increased.
Non-pharmacologic modalities can include weight loss, aerobic exercise, muscle-strengthening exercises, neuromuscular education, dietary supplements, walking aid, bracing, and physical modalities.
In older people affected by knee or hip OA, a first approach should be weight reduction associated to perform a regular aerobic activity and joint protection brace, aimed to decrease the load on the joints of the lower limbs. The main advice should be to avoid prolonged postures and activities that overload the joint. Walking aids such as a cane or walker can decrease load on affected joints, and a simple walking stick reduces hip loading by 20–30%.
Clinical guidelines recommend that people with hip and knee osteoarthritis wear appropriate footwear, although there is no evidence supporting their use. Heel raises can be used to achieve pelvic obliquity and improve joint congruence in the setting of a functional leg-length discrepancy. In patients with knee OA and mild/moderate varus or valgus instability, a knee brace can reduce pain and improve stability and the risk of falling [32].
Exercises are a very important tool of conservative management for OA and are universally recommended by clinical guidelines [33]. Exercises should be prescribed in the early stages of OA or as preventive treatment. There is a growing evidence that the pathologic processes of OA may lead to a dysfunction of the joint surrounding muscles rather than within the cartilage. Moreover, preoperative neuromuscular exercises may constitute a viable adjunct therapy to hip or knee arthroplasty. In fact, several studies have shown that a preoperative neuromuscular exercise program leads to an earlier onset of postoperative recovery in self-reported ADL. In literature exercise programs have proven more effective in the knee OA than hip OA. There is no evidence that certain types of exercises have a better outcome than others. Generally, muscle strengthening, aerobic reconditioning, joint mobility, muscular stretching, and coordination and proprioception exercises are prescribed. Recommendations for dosage and progression of exercise in older people and people with chronic disease are aerobic moderate-intensity training for at least 30 min/day or up to 60 min and progressive strength training involving the major muscle groups for at least 2 days/week at a level of moderate to vigorous intensity. But people with chronic disease who do not reach the recommended level should perform exercises as their abilities and condition allow.
Unfortunately, physicians do not recommend physiotherapy or a program of exercises to every patient. Moreover, patients, especially elderly, often may be uncompliant to the physical work, and it is related to the increased risk of inactivity and morbidity.
Aquatic exercises have been recommended as an option for people with hip osteoarthritis because in water the percentage of body weight supported by the lower limbs is lower. Although there is strong evidence on their effectiveness compared to exercises performed on the ground, aquatic exercises are very useful for patients with obesity or neuro-musculoskeletal disorders.
The use of physical modalities such as ultrasound, electromagnetic fields, and low-level laser therapy in clinical practice is controversial and varies between countries. However, the American College of Rheumatology Clinical Guidelines recommends to instruct patients in the use of thermal agents.
Surgery should be considered only in the case of unsatisfactory results obtained with conservative treatments.
We cannot close off this section without discussing hand OA because of it high prevalence in the population, more than knee/hip OA. Because of the important functional significance of the thumb, trapeziometacarpal (TM) OA is more significant in fact of disability than osteoarthritis of other fingers.
Generally, TM OA is more frequent in women than men, but the prevalence strongly increases with aging in both genders.
Patients with TM OA reported persistent pain at the thumb base which limits their hand functions, reducing both thumb mobility and hand strength, affecting their daily activities (holding objects, preparing meals, writing), and causing a considerable reduction in quality of life, particularly in older people. While the results of surgical procedures have been well studied, gaps remain in research about the effectiveness of conservative treatments. Management of TM OA includes joint protection, education, assistive devices, hand exercises, pharmacological therapy, corticosteroid/hyaluronic acid injections, orthoses, and physical modalities.
To date, several studies have shown that hyaluronic acid injections induce a decrease of pain and an improvement in function that are also preserved in the medium to long term. Therefore, hyaluronic acid may be a safety and valid therapeutic option, which should be considered when other conservative therapies (like NSAIDs) were ineffective or contraindicated, before surgery [10].
28.4 Total Joint Replacement
According to national and international guidelines and the 2014 Osteoarthritis Research Society International (OARSI) recommendations, rehabilitation is considered the core treatment of OA and is widely indicated in primary care settings. Joint replacement is recommended if conservative treatment failed in reducing pain and improving quality of life or in patients with end-stage OA. About 119 per 100 thousand persons per year undergo total hip arthroplasty (THA) and a slightly lower number in total knee arthroplasty (TKA) worldwide.
28.4.1 Rehabilitation After Total Knee Arthroplasty (TKA)
TKA is considered as one of the useful medical interventions in terms of pain relief, improvement in function, and consequently in quality of life for patients suffering from end-stage OA. These patients show a modified gait pattern due to pain, with reduced gait speed and step length and increased time in double limb stand.
Outcomes following TKA depend on surgical technique and implant longevity; preoperative levels of knee pain, strength, flexibility, and functional ability; and, of course, on the adequacy of rehabilitation following surgery [34].
In the last decade, several authors began to argue on preoperative physiotherapy and exercise programs (called “pre-rehabilitation”) for its capability to potentially improve early postoperative pain and function and consequently reduce recovery time and hospitalization in patients undergoing joint replacement. Pre-rehabilitation programs typically include warm-up, lower limb stretching and strengthening, aerobic training, and, in some protocol, step training. Proprioceptive and balance training or home exercises have also been proposed in some studies [35]. Villadsen et al. in their review underline the importance of a neuromuscular rehabilitation protocol as a viable treatment, combined to other preoperative exercise, to optimize and accelerate postoperative recovery until 3 months after TKA [36].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





