Assessment
Symptom evaluation
Quality-of-life measurements
Pulmonary function tests
Comorbidities and therapy
Exercise training
Endurance training
Interval training
Resistance/strength training
Flexibility training
Upper limb training
Inspiratory muscle training
Neuromuscular electrical stimulation
Maximizing the effects of exercise training
Pharmacotherapy
Oxygen and helium–oxygen hyperoxic gas mixtures
Noninvasive positive pressure ventilation
Education
Behavior change
Collaborative self-management
Addressing motivational issues
Breathing strategies
Pursed-lip breathing
Computer-aided breathing feedback
Table 46.2
Multidisciplinary team participants in a pulmonary rehabilitation team
Pulmonologist |
Respiratory therapist |
Physical therapist |
Educational therapist |
Nurse/exercise physiologists |
Nutritionist |
Social worker |
Psychologist/behavioral specialist |
Occupational therapist |
Social worker |
46.2.1 Assessment
As mentioned above, a complete, comprehensive evaluation of the patient’s physical, psychological, and lung function status should be performed to establish the candidate’s suitability for PRP. The most frequently reported symptoms are fatigue, cough, weakness, and dyspnea at rest and/or during exertion. St. George’s Respiratory Questionnaire (SGRQ), the Chronic Respiratory Disease Questionnaire (CRQ), and the COPD Assessment Test (CAT) are the most common questionnaires that are used for symptom assessment. The presence of depression and anxiety should also be evaluated, as both conditions can adversely affect a patient’s ability to participate in a PRP. The patient’s capacity to complete activities of daily living (ADL) can be rated using performance scales, including the Manchester Respiratory Activities of Daily Living Scale, the Pulmonary Functional Status and Dyspnea Questionnaire, and the London Chest Activity of Daily Living Scale. Physicians should also evaluate if the patient is following an optimal medical regimen usually consisting in inhaled bronchodilators and corticosteroids, and if need be, long-term oxygen therapy.
Pulmonary function tests (PFT) should be routinely included in a candidate’s comprehensive pre-PR evaluation since they are essential to confirm the diagnosis of the underlying disease, to assess the level of ventilatory impairment, and to evaluate the effect of pharmacologic therapy. Static and dynamic lung volumes including total lung capacity (TLC), forced vital capacity (FVC), forced expiratory volume in first second (FEV1), and FEV1/FVC ratio can be utilized to identify an obstructive and/or restrictive ventilatory defect (Figs. 46.1 and 46.2). While a reduction in the FEV1/FVC ratio below the predicted value is consistent with an obstructive ventilatory impairment, the lack of response to inhaled bronchodilator therapy may contribute to establishing a diagnosis of COPD (Fig. 46.3). A specific evaluation of respiratory muscle strength is mandatory for patients with neuromuscular disorders (e.g., amyotrophic lateral sclerosis, myasthenia gravis, muscular dystrophies, etc.), which is based on the measurement of maximal inspiratory and expiratory pressure (MIP, MEP); a high negative MIP value (<−80 cm H2O) or a high positive MEP value (>+90 cm H2O) can, respectively, exclude clinically relevant inspiratory or expiratory muscle weakness. Functional tests should also include a maximal cardiopulmonary exercise testing (CPET) that may provide essential data to identify factors contributing to exercise limitation, assess the safety of exercise, and establish the patient’s maximal work rate.
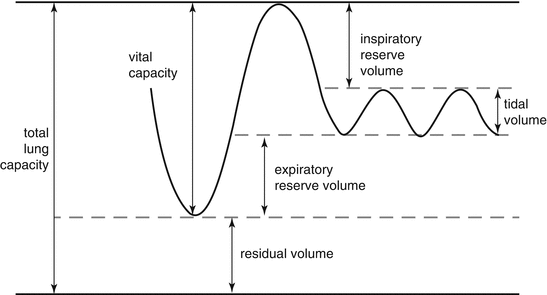
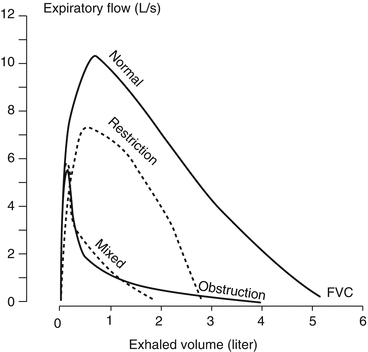
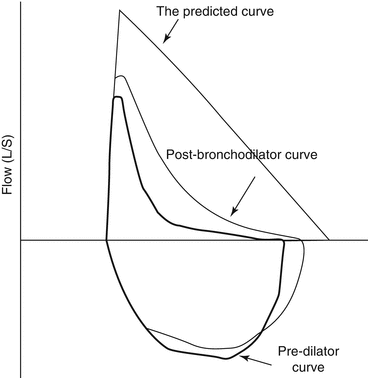

Fig. 46.1
Lung volumes and capacities according to spirometry

Fig. 46.2
Flow/volume curve recorded by a spirometric challenge test during a forced expiration, showing a normal FVC/VC ratio and obstructive, restrictive, and mixed alterations

Fig. 46.3
Flow/volume curve recorded during a forced expiratory spirometric challenge before and after bronchodilator administration
46.2.2 Exercise Training
Patients with chronic respiratory disorder commonly show shortness of breath leading to inactivity which, in turn, leads to a loss of muscle strength, mobility problems, sarcopenia, and cardiac dysfunction. Age-related pulmonary function decline and the presence of comorbidities may limit exercise even further. Considered the cornerstone of PR, exercise training is the best method to improve muscle function. An improvement in skeletal muscle function after exercise training leads to greater exercise capacity despite the absence of changes in lung function. The improved oxidative capacity and efficiency of the skeletal muscles lead, moreover, to a lower ventilatory requirement for a given submaximal work rate, which, in turn, may reduce dynamic hyperinflation and exertional dyspnea. Although the total amount of work should be individualized depending on the patient’s specific need to ameliorate aerobic capacity and muscle strength, training on a regular basis with activity loads exceeding those of everyday life is essential to improve exercise performance.
A variety of exercise regimens are available for exercise training [1–3]:
- 1.
Endurance training. Endurance training can improve aerobic capacity and reduce breathlessness and fatigue by ameliorating cardiorespiratory function. High-intensity endurance training performed by cycling or walking is usually prescribed five times per week, at an intensity of continuous exercise (>60% of maximal work rate) for 20–60 min sessions. Work intensity can be established on the basis of the results of the Borg Dyspnea Scale (target 4–6) or the Rating of Perceived Exertion (RPE) (target 12–14). The benefits expected include improvement in exercise tolerance, muscle function, and bioenergetics.
- 2.
Interval training. Interval training combines high-intensity exercise with periods of rest or low-intensity work to help the patient achieve a high training load while avoiding the onset of dyspnea and fatigue. The strategy is particularly indicated for patients with severe exercise-induced dyspnea and/or severe comorbidities.
- 3.
Resistance/strength training. As patients with chronic respiratory diseases can also show reduced muscle mass and strength that may, in turn, limit exercise tolerance, they may benefit from strength training of specific muscle groups, in particular repetitive lifting of heavy weights. Interestingly, a combination of resistive and endurance training has been found to be extremely effective in increasing exercise capacity, with the additional advantage of counteracting an abnormal loss of bone mineral density that is common among COPD patients.
- 4.
Flexibility training. Postural abnormalities such as thoracic kyphosis, increased chest anterior-posterior diameter, shoulder elevation, and protraction or trunk flexure may accelerate pulmonary function decline, increase the work of breathing, and worsen QoL in COPD patients. Upper and lower body flexibility programs, including stretching of the major muscle groups, at least 2–3 days per week, can improve thoracic posture and mobility.
- 5.
Upper limb training. Aerobic upper limb resistance training should help the patient with self-care activities including dressing, bathing, and simple household tasks.
- 6.
Inspiratory muscle training. Elderly patients with respiratory impairment may show diminished pressure-generating capacity by the inspiratory muscles that may reduce exercise tolerance and contribute to dyspnea. Inspiratory muscle training in this case could be particularly advantageous.
- 7.
Transcutaneous neuromuscular electrical stimulation (NSE). NSE, which can improve skeletal muscle strength and exercise capacity and decrease dyspnea and fatigue, can be utilized in deconditioned individuals with severe ventilatory or cardiac limitations. This technique may be beneficial to individuals with cognitive and psychological difficulties and/or severe dyspnea who are not eligible for standard PRPs.
Frequency, intensity, and specificity of exercise sessions are the most important variables determining the impact of training:
- 1.
Frequency. For pragmatic reasons, most PRPs organize sessions two or three times weekly. Although some evidence indicates that two sessions per week may be inadequate to produce effects, it is also true that most therapists instruct patients to exercise at home in between sessions.
- 2.
Intensity. Most studies indicate that there is a threshold for the training effect. An improvement in endurance seems to be a virtual certainty if a level of intensity corresponding to 60–75% of the maximum oxygen uptake can be sustained for at least 20–30 min a few days per week.
- 3.
Specificity. Training regimens are prescribed that are specific to the patient’s needs. For example, walking endurance activities increase walking endurance and thus the lower extremities but not the upper ones. Furthermore, endurance exercises improve endurance capabilities more than strength, whereas strength training (i.e., weightlifting) increases strength but not necessarily endurance or other outcomes such as exercise capacity or health status. Most programs, thus, incorporate a variety of training regimens.
46.2.2.1 Maximizing the Effects of Exercise Training
The effect of exercise training can be enhanced by a number of measures aiming to improve ventilatory capacity and blood gas exchanges, including the utilization of bronchodilators, oxygen and helium–oxygen hyperoxic gas mixtures, and noninvasive mechanical ventilation.
- 1.
Pharmacological agents. Pharmacologic therapy is one of the key components of a treatment management plan for subjects with chronic airflow limitation aiming to prevent and control symptoms, reduce exacerbations, and improve exercise tolerance and general health status. Inhaled bronchodilators can increase expiratory flow and reduce dynamic hyperinflation by acting on the airway smooth muscles. Since it increases exercise tolerance, bronchodilators are an essential component of PRP in elderly patients with COPD [4]. Although studies on anabolic hormonal supplementation, and in particular testosterone analogs, have demonstrated that they produce a positive effect on muscle mass, they do not seem to induce a significant increase in muscle strength and endurance in individuals with COPD [1].
- 2.
Supplemental oxygen therapy. Oxygen therapy is usually considered a routine supplementary measure in patients with respiratory diseases enrolled in a PRP as it tends to improve exercise tolerance and reduce breathlessness. Studies evaluating the efficacy of oxygen supplementation during exercise training have, nevertheless, produced conflicting results. In fact, while oxygen therapy with respect to compressed air results in higher training intensity in normoxic individuals with moderate to severe COPD, supplemental oxygen does not improve exercise tolerance and/or health status in individuals with severe COPD and exercise-induced hypoxemia. Given these considerations, it is not entirely clear if supplemental oxygen therapy is beneficial during exercise training. Of interest, patients administered with long-term oxygen therapy commonly require augmented oxygen flow rate during exercise to maintain adequate oxygenation [5]. With respect to room air, heliox, which is helium–oxygen mixture, may reduce gas density and lower airway resistance and air trapping in patients with obstructive disease, thereby enhancing exercise tolerance. Although heliox theoretically appears to be an effective tool to augment maximal work rate during training, evidence suggesting that it can have a beneficial impact on exercise training is still inconsistent [6].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree