Fig. 18.1
Transfemoral amputation
Frequently, the general health condition of these amputated patients is compromised by:
Cardiovascular failure (80% of cases)
Respiratory diseases
Diabetic retinopathy and/or peripheral neuropathy [2]
It follows that these patients have limited energetic resources [3] and feature low-to-average functional activity levels (K1, K2); K-levels are defined by Medicare, based on an individual’s ability or potential to ambulate and navigate his/her environment; K0 patients are not eligible for prosthesis, while K4 patients have the ability or potential for prosthetic ambulation that exceeds basic ambulation skills, typical of the prosthetic demands of the child, active adult, or athlete. The high probability of successful prosthetic fitting reported among referral practices cannot be generalized to elderly individuals, but selected individuals can successfully be fitted with a prosthesis [4]. Rehabilitation efforts should best be targeted depending on needs. Rehabilitation professionals should make an educated estimate of outcomes at the beginning of rehabilitation based on the characteristics of the patients and the personal functional level on admission [5]. Considering the prosthetic application and the functional recovery that will follow, it is important to preserve as much limb as possible, with the most distal level of amputation permissible. For this reason, it is important to seriously consider:
Foot amputations (transmetatarsal, tarsal, Syme, and Pirogoff). Transmetatarsal amputation is often used in patients with infection of the forefoot, necrosis, gangrene, and diabetic neuropathy with the aim to obtain a good functionality of the limb by preserving the midfoot. When the metatarsal bones are completely removed, the amputation level is named “Lisfranc amputation”. The Chopart amputation is a disarticulation of the midfoot from the hindfoot: it is always combined with an ankle talar arthrodesis to obtain a foot with a proper support. Pirogoff level is obtained with the section of the bones of the leg over the ankle joint and with the arthrodesis of the heel’s tubercle, placed in maximum talism, with the surface of section. The limb will be shortest than contralateral, suitable to sustain the weight of the body even without prosthesis. A Syme amputation is an amputation done through the ankle joint indicated for foot trauma, infection, or tumors, which allows to obtain a limb functional and painless.
The preservation of the knee joint, if the stump achievable is longer than 4 cm, measured from the joint line [6].
Knee disarticulation, if a full load-bearing is achievable, instead of a transfemoral amputation due to its numerous advantages from a prosthetic viewpoint.
In addition, in case of transfemoral amputation, it is always best to preserve the longest lever possible (distal stump), but with an 8–10 cm difference with respect to the contralateral knee joint line. This enables to reach two important goals:
Reduction of the energy consumption (long lever)
The possibility to apply the widest range of prosthetic knees and some additional components, e.g., a static rotator, avoiding an anatomical asymmetry when compared to the contralateral knee in seated position
The absence of vascular impairment of the residual limb and timely admission to the rehabilitation hospital correlated positively with effectiveness of mobility [7], but the amputation of the contralateral limb takes place within 3–4 years, in 30% of cases of amputation, based on a study of the Queen Mary’s Hospital in Roehampton (UK).
Based on our experience, a bilateral transtibial amputee has a high probability to return to walk with two prostheses even in aged persons. On the contrary, for a bilateral transfemoral amputation, the probability is substantially lower and becomes null if stumps are proximal.
Elderly patients have a high probability of using a prosthesis when having an independent ambulation after transtibial amputation, without phantom pain, and they should be considered for prosthetic training [8].
All of the above stress the importance of careful clinical assessment of the patient by a multidisciplinary team: firstly, to evaluate the real potential for a prosthetic treatment and, secondly, to define a specific and customized prosthetic rehabilitation, possibly in collaboration with specialists in internal medicine, psychology [9], and cardiology.
The probability of success increases and the duration of the prosthetic-rehabilitative intervention decreases if a pre-prosthetic physio-kinesiotherapic intervention is applied. This aims to:
Preserve the mobility of the residual joints.
Prevent wrong postures (flexed or abducted stump) which follow after a long bed resting period or extended wheelchair use (hypokinetic syndrome) and are frequent in geriatric amputees.
Reduce postoperative edema, thanks to an elastic-compressive monodirectional elastic bandage, or similar liners (Fig. 18.2).
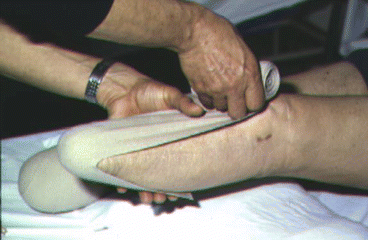
Fig. 18.2
Elastic-compressive bandage
Prevent risk factors for patient falls [10].
The application of the first prosthesis should take place shortly after amputation, in the eighth–tenth week, in the absence of complications, with the aim of accelerating gait recovery and avoiding hypokinetic syndrome’s effects. This goal can be obtained by means of the application of temporary endoskeletal prostheses. However, this category of prosthesis has little in common with the definitive prosthetic device, both considering the suspension system (thigh bands, harnesses, etc.) and the socket, which are little or non-customizable. These pitfalls frequently lead to prosthetic control issues and, consequently, to gait problems, not to mention pain, wounds, sores, and rapid muscle fatigue, which may ultimately result in depression, reject, and abandonment of the prosthesis for the majority of patients.
The application of a definitive (customized) prosthesis should also be carefully considered and followed by the renewal of the socket, after the stump stabilization.
The prostheses for geriatric patients must be designed considering technical and technological solutions that impact on three essential elements (Fig. 18.3):
Lightweight, or weight containment
Safety, to avoid falls
Comfort

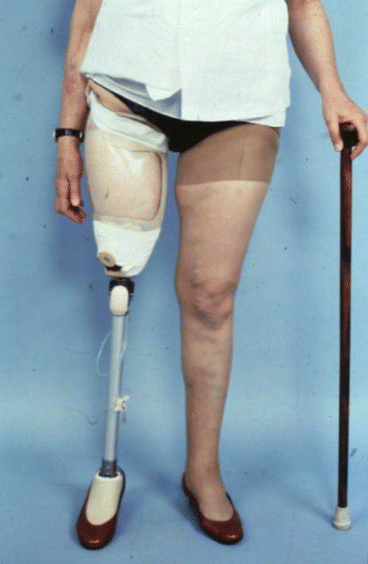
Fig. 18.3
Geriatric transfemoral prosthesis with flexible ischial containment socket and unlocking knee
Maintaining a lightweight structure aims to limit the metabolic energy expenditure (exhaustion) during gait. This essential target is always useful after proximal amputations, due to the limited resources of high-level amputees. The weight of the prostheses can be limited, mostly through a careful choice of socket materials, connecting tubes and joints. The application of carbon fiber in the socket, instead of standard materials, enables to reduce the wall thickness and, accordingly, the weight. Connecting tubes and joints (knee and ankle), made of light alloys, titanium, or carbon fiber, reduce the weight by 25% compared to standard steel, with no effect on functionality and maximum load of the prosthesis. The choice of the solid ankle cushion heel (SACH) foot, specifically designed for geriatric amputees, can further support prosthesis weight reduction, thanks to its low weight (350 g) compared to the commonly applied prosthetic feet (about 550 g) [11]. Moreover, a geriatric foot designed with a low effective foot length improves the satisfaction and reduces proximal anterior socket pressures for poor-performing persons with transtibial amputation [12]. However, all these efforts can be vanished by the use of heavy footwear.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree