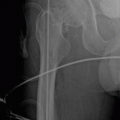
Physical modality
Tissue absorption
Action
Infrared radiations
Superficial
Muscle, joint, ulcer
Continuous shortwave
Deep
Muscle, joint
Pulsed shortwave
Wet, ionic
Muscle, nerve, edema, hematoma
Laser
Superficial vascular
Muscle, nerve, tendon, joint, open wounds
Ultrasound
Dense collagen, deep
Ligament, tendon, fascia, joint capsule, fibrotic muscle
10.2.2 Cold
Local application of cold (cryotherapy) decreases blood flow by activating a vasoconstrictive reflex and reduces inflammation and the metabolic request of hypoxic tissues. Moreover, it has a topical anesthetic effect by reducing the activation threshold of tissue nociceptors, the conduction velocity of nerves, and muscle spindle fiber activity.
Cold therapy improves pain symptoms and reduces local edema and inflammation; it is also effective in reducing muscle spasms and contractures and in the treatment of sprains, strains, contusions, tendonitis, etc. For all these reasons, cryotherapy is commonly used after acute injuries and articular diseases.
10.3 Laser Therapy
“Laser” is the acronym for “light amplification by stimulated emission of radiation.” Laser therapy transfers energy within the tissues, thus modulating the biological processes (photobiomodulation) according to “the Arndt-Schultz law”: low dosage photonic energy stimulates the biological processes (photobiostimulative effect), whereas, on the contrary, high dosage energy has an inhibitory effect (photobioinhibitive effect).
Lasers can be classified, according to the wavelength/max output power and the ability to damage exposed persons, into four classes of risk: from the lowest (class I: no hazard) to the highest (class IV: severe risk for the eyes and skin). Most therapeutic lasers are class III (low-level, cold, or low-power lasers) and deliver limited amount of energy and power (≤500 mW). However, they are not as effective as high power lasers (class IV therapeutic lasers).
The laser therapy effects are analgesic, anti-inflammatory (it stimulates the release of beta-endorphins), and reparative (regenerative action on deep structures by inducing the protein synthesis and increasing blood flow). The physiological effects are:
biostimulation (increase of cell metabolism)
blood circulation improvement and vasodilatation
increased ATP production
wound healing stimulation
increased collagen production
enhanced macrophage activity
modification of nerve conduction (velocity)
Lasers are commonly applied through a connector maniple, if small areas are to be treated (Fig. 10.1), or through scanning technique, when dealing with wider areas (Fig. 10.2).
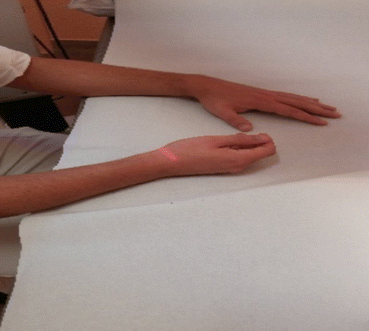
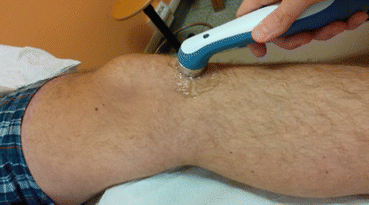

Fig. 10.1
Laser application using scanning technique

Fig. 10.2
US therapy applied directly on the knee
Common indications of laser therapy are musculoskeletal pain symptoms, inflammatory diseases of tendons and soft tissue, enthesopathies, edema, and pressure sores (Table 10.1).
10.3.1 Low-Level Laser Therapy (LLLT)
LLLT (wavelength from 600 to 1000 nm) uses red beam or NIR lasers. It consists of different procedures and is performed by different methods.
10.3.2 High Dose: High Power Laser Therapy
High power lasers are used to stimulate tissue healing, but they can also improve pain from osteoarthritis, carpal tunnel syndrome, epicondylitis, sprains or strains, and muscle disorders.
10.4 Therapeutic Ultrasound
Ultrasound (US) is a mechanical wave that, passing through the body, transfers its energy to the tissues, causing molecular vibration. US determines thermal and nonthermal effects; nonthermal effects are attributed to a combination of cavitation and shear stress (see also the paragraph on Thermotherapy). Cavitation leads to the formation of reactive oxygen species and stimulates cell repair during the inflammatory phase. Shear stress include the radiation pressure, radiation force, and acoustic streaming; the latter phenomenon changes cell diffusion rate, permeability, and membrane potentials. Thermal effects improve nerve transmission speed, increase blood flow rate, and reduce edema. From all the above, it is clear that therapeutic US is mainly used to promote tissue healing and improve the quality of tissue repair.
The frequencies used in US therapy are typically between 1.0 and 3.0 MHz. Depth of penetration is dependent on the frequency of the US machine. Therapeutic US can be applied as pulsed or continuous therapy, either directly, using a transducer and a conductive gel (Fig. 10.2), or indirectly transferred, through immersion of the transducer in water (Fig. 10.3). The penetration of US is better in tissues rich in collagen content (i.e., ligaments, tendons, fascias, joints, and fibrotic muscles) (Table 10.1) [13–16].


Fig. 10.3
US therapy through immersion technique is used for irregular surfaces
US treatment lasts approximately from 5 to 15 min and is repeated from one to three times a week; patient should never feel pain during therapy. Many clinicians use of pulsed US to treat, once or even twice daily, acute conditions. In this case, therapy lasts from 6 to 8 days until symptoms subside. In subacute or chronic conditions, patients can be treated every other day.
Indications for therapeutic US are osteoarthritis, rheumatic diseases, joint or tendon inflammation, soft tissue injuries, sprains or strains, myositis ossificans, nerve entrapments (brachialgia, sciatalgia), and muscle spasms.
Contraindications for US treatment are cardiac diseases, deep vein thrombosis, pregnancy, malignancy, and metal implants [17].
10.5 Extracorporeal Shockwave Therapy (ESWT)
Shockwaves are high-energy acoustic waves that travel faster than conventional sound wave. The more energy is applied, the more the shockwave will penetrate the tissue, determining a rapid expansion of the gases solved in blood and lymphatic fluids. Expanding gas molecules causes an increased pressure on the dysfunctional tissues, determining a phenomenon called “cavitation” in which voids quickly collapse on themselves generating an implosion (shockwave) in the tissue. Healthy tissues are not affected by the shockwaves because they can easily absorb their energy.
Shockwaves action on musculoskeletal system can determine:
Cell permeability modifications
Osteoblasts stimulation
Osteogenic action
Growth factors production
Increase in type I and III collagen synthesis
Vasoactive effects
Shockwaves can be focused or radial; they have different physical characteristic, are generated with different techniques (radial shockwaves are produced by a pneumatic system; focused shockwaves can be produced by electrohydraulic, electromagnetic, and piezoelectric shockwave generators), and use different parameters used for therapeutic penetration in the tissues (Table 10.2).
Table 10.2
Physical characteristics of ESWT
ESWT type | Pressure (bar) | Pulse duration | Pressure field | Penetration depth |
|---|---|---|---|---|
Radial | 1–10 | 0.2–0.5 ms | Radial, divergent | Small, superficial |
Focused | 100–1000 | 0.2 μs | Focused | Large |
ESWT has been proven as effective and safe for treatment of musculoskeletal diseases [18, 19]. Radial shockwaves can be used in case of myofascial pain syndromes or spasticity.
Focused shockwaves seem to have a more favorable outcome in relieving deep pain or chronic tendinitis [20, 21]; they can also be used in the occurrence of:
Tendinopathies (plantar fasciitis, ulnar and radial epicondylopathy, rotator cuff tendinitis with or without calcifications, adductor syndrome, etc.)
Impaired bone healing function (delayed healing, stress fractures, early stage of avascular bone necrosis, etc.)
Muscular pathologies (myofascial syndrome, excluded fibromyalgia excluded)
Impaired wound healing
Spasticity
10.6 Whole Body Vibration (WBV)
WBV has gained popularity in geriatric rehabilitation in the past decade. It is considered a passive exercise modality in which patients lay, sit, or stand on a platform that delivers vibration stimuli to the rest of the body. The vibration signals activate the sensory receptors by changing the length of the muscle-tendon complex and causing reflexive activation of motor units. However, the biological and mechanical effects of WBV are not completely understood.
WBV may induce positive effects on leg muscle strength, improving postural control and functional mobility among elderly adults, particularly frailer ones. Vibration therapy can also be used in multiple sclerosis, neuropathies, osteoporosis, and in case of pain (e.g., in women with fibromyalgia syndrome). WBV has also shown some positive effects on gait and balance in Parkinson disease [22–24].
Contraindications of WBV therapy are acute inflammations, infections, acute arthritis, severe cardiovascular diseases, heart failure, pacemaker, deep vein thrombosis, leg ulcers, pregnancy, spasticity, vertigo, severe headache, acute tendonitis, acute back pain, gliding spondylolisthesis, fractures, metal implants, severe osteoporosis, musculoskeletal metastatic tumors, serious ocular diseases, and fresh wounds.
10.7 Magnetotherapy
Magnetotherapy consists in applying artificial magnetic fields that are generated by electrical currents to the human body. Artificial magnetic fields used in PM have similar intensity to the earth’s, but with higher frequencies and longer time of application.
Magnetotherapy acts on cell membranes by the modification of cell permeability and the increase of intracellular metabolic exchanges; it has a biostimulating effect (increasing nucleic acid synthesis, cell metabolism, and the oxygen consumption) and an analgesic effect (suppressing the peripheral nociceptive stimuli, enhancing the production and the release of pain-inhibiting substances, and increasing peripheral blood circulation). Magnetotherapy also acts on autonomic system increasing the catecholamine or acetylcholine level and promotes bone trophysm by stimulating the bony callous formation. Therefore, the effects of magnetotherapy can be analgesic, anti-inflammatory, anti-edematous, and reparative.
Artificial magnets can be electromagnets that work when connected to electricity, pulsed electromagnets generated by a brief pulse of electric current and connected to a coil (Fig. 10.4), or permanent magnets. Magnetic fields are used with low or high intensity, in the ambulatory care or home setting for several hours per day. Instrument settings should be adjusted according to patient’s reactions; however, an increase in pain symptoms could signify a positive response to treatment.
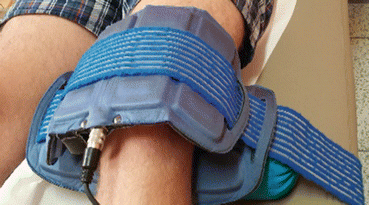

Fig. 10.4
Portable magnetotherapy with pulsed magnetic fields
Common indications for magnetotherapy are osteopenia, delayed fracture healing, posttraumatic algodystrophy, inflammatory or degenerative arthropathy, trophic ulcers, etc.
Contraindications are pacemaker, hemorrhage, pregnancy, acute infection, and malignancy.
10.8 Electrotherapy
All electrical modalities used in Physical and Rehabilitation Medicine (PRM) take the electrical current flowing from a wall outlet and modify that current to produce a specific, desired physiologic effect in human biologic tissue [25]. Electrotherapeutic devices regardless of whether they deliver alternating (AC), direct (DC), or pulsatile (PC) through electrodes attached to the skin are transcutaneous electrical stimulators. When they introduced into biologic tissue, they are capable of producing specific physiologic changes [26]. The term waveform indicates a graphic representation of the shape, direction, amplitude, duration, and pulse frequency of the electrical current being produced by the electrotherapeutic device, as displayed by an oscilloscope [27].
Waveform shapes (Fig. 10.5) can be:
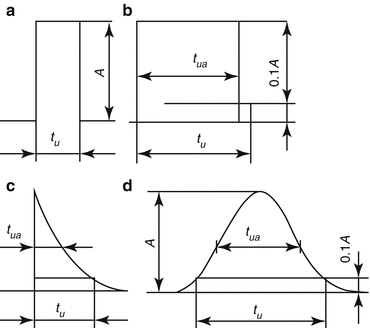
Rectangular
Square
Spike
Sinusoidal (sine)

Fig. 10.5
Waveform shapes of pulsatile currents
Knowledge of the electric properties of cells, intercellular and intracellular communication, bioelectric potentials, tissue currents, strain-generated electric potentials, and biologic effects of other nonionizing energy will be essential for the PRM specialists in order to use present and future electrical modalities for maximum clinical benefit [26].
Today PRM specialists are using electrical currents in an effort to provide a quick and effective pain management, tissue healing, and neuromuscular stimulation. The treatment protocol must be tailored toward influencing the problems identified in the evaluation. Although electrotherapeutical procedures can provide dramatic results at times, this is the exception rather than the rule. Electrotherapy should not be used in a “shotgun” approach if we are to maximize the effectiveness of this modality. Usual electrotherapy treatment lasts 30 min for each session; it can be repeated two or three times a week for a total of 10/12 sessions [28–30].
10.8.1 Iontophoresis
Iontophoresis is a therapeutic procedure that involves the introduction of various ionized drugs into the skin by means of a direct electrical current for the purpose of transporting chemicals across the membrane [31]. Iontophoresis has several advantages is a painless, sterile, and noninvasive procedure that provides a high degree of compliance, acceptability, and has a positive effect on the healing process. On the same time, it provides a high degree of patient compliance and acceptability, and it has been demonstrated to have a positive effect on the healing process. A primary advantage of iontophoresis is the ability to provide both a spiked and sustained release of a drug, thus reducing the possibility of developing a tolerance to the drug [32]. Transdermal iontophoresis delivers medication at a constant rate so that the effective plasma concentration remains within a therapeutic window for an extended period of time. Clinically, iontophoresis is used in the treatment of inflammatory musculoskeletal conditions, for analgesic effects, scar modification, wound healing and in treating edema, calcium deposits, and hyperhidrosis. The effectiveness of iontophoresis is directly related to the medication administered or the solution used for ion transfer. Each medication has its own effect, regardless of the method of application [33].
Contraindications of iontophoresis are pacemakers, epilepsy, malignancy, metal implants, gastritis or active stomach ulcer (hydrocortisone), skin sensitivity reactions, skin wounds, asthma (mecholyl), and sensitivity to metals (zinc, copper, magnesium) and seafood (iodine). The most common complication associated with iontophoresis is a chemical burn, which usually occurs as a result of the direct current itself and not as a result of the ion being used in treatment. Heat burns may occur as a result of high resistance to current flow created by poor contact of the electrodes with the skin. During the treatment, the PRM specialist should closely supervise the patient, looking for either abnormal localized reactions of the skin or systemic reactions [34].
10.8.2 Neuromuscular Electrostimulation (NMES)
NMES also known as electrical muscle stimulation (EMS), or electromyostimulation, is a noninvasive method that, using the excitability of muscle cells, allows to induce muscle contraction by an electric current; this method can be applied either to a normally innervated muscle or to a denervated muscle [35].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree