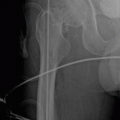
Fig. 16.1
Upper limb rigid (right) and semirigid static orthoses
16.3 Shoes and Shoe Modifications
Falls in older people are often related to footwear. Foot proprioception and plantar sensitivity worsen during age and in diabetes, peripheral neuropathies, and other medical conditions. Therapeutic shoes or shoe modifications might improve balance and reduce risk for falling; they could influence both tactile and proprioceptive mechanisms; moreover, the choice of appropriate and comfortable shoes could reduce the necessity of an orthosis [4].
Shoes should fit the shape of the foot and be one index fingerbreadth longer than the longest toe, allowing movement during standing and walking [5]. Loose or tight shoes can determine calluses, ulcers, or corns. Leather is one of the best materials to avoid this inconvenience, because it is durable and breathable, adapts itself to the patient’s foot shape, and can be easily reshaped. In patients with diabetes and peripheral neuropathy, shoes should aim to decrease pressure on prominent areas through a high wide toe box. Modified or custom-made shoes are also indicated in case of ankle stiffness, edema, or joint deformity.
Foot inversion or eversion can be treated using a heel flare on either the medial or lateral heel. Distributing forces to the lateral knee compartment through lateral heel wedges may prevent valgus medial knee compartment overload in osteoarthritis.
Metatarsalgia is treated by distributing the forces to the metatarsal shafts using either a metatarsal bar or a rocker (convex) bar, positioned on the external sole in order to promote foot rollover. A metatarsal pad inside the shoe can be placed behind metatarsal heads in less severe cases. Adding an extended shank with mild rocker sole in order to decrease shoe’s flexibility could treat toe pain, which occurs in arthritis and gout.
Talalgia, often caused by plantar fasciitis, calcaneal spurs, and Achilles tendon retraction, can be managed using an external calcaneal bar behind the painful site. If plantar fasciitis is associated with overpronation, a Thomas heel can help in pushing the foot toward the opposite side. Heel lifts or heel cushion relief pads can relieve Achilles tendon pain.
Leg length differences major than 10–15 mm should be treated using internal heel lifts [6].
16.4 Lower Limb Orthoses (LLO)
LLO and shoes are used to treat weakness, spasticity, pain, and joint deformities, in case of brain injury, neuropathies, arthritis, fractures, or amputation. Moreover, they improve abnormal posture or tone and can be used to correct irregular gait patterns. They should be periodically evaluated to monitor for patient’s comfort, skin breakdown, and their effects on ambulation; a multidisciplinary approach is advised during patient’s assessment.
According to the International Standard Organization (ISO), the classification of LLO is based on the anatomical joint, which they contain foot orthoses (FO), ankle-foot orthoses (AFO), knee orthoses (KO), knee-ankle-foot orthoses (KAFO), hip-knee-ankle-foot orthosis (HKAFO, which are used for infants in cerebral palsy), and hip orthoses (see Table 16.1).
Table 16.1
Lower limb orthoses classification
Classifications based on design | Types | |
|---|---|---|
Lower limb Orthoses | Static Dynamic | Foot orthoses (FO) Ankle-foot orthoses (AFO) Knee-ankle-foot orthoses (KAFO) Knee orthoses (KO) Hip-knee-ankle-foot orthoses (HKAFO) Hip orthoses |
- 1.
Foot Orthoses (FO)
FO are useful in reducing ground reactive forces acting on lower limb joints; moreover, these devices can control pronation and supination. Three types of FO are available: soft, semirigid, and rigid. Soft foot orthoses can provide shock absorption, whereas rigid and semirigid, which are custom-made from casts of patients’ feet, also support plantar arch (e.g., in case of severe foot deformities). It is fundamental, especially when using semirigid and rigid orthoses, to monitor skin looking for the presence of wounds or clinical signs of infection.
Flat and high-arched feet are managed using semirigid foot orthoses, which extend the foot and provide medial arch support. FO can also correct hyperpronation of the midfoot by acting on the longitudinal axis of the foot. The plantar buildup should be progressively increased to avoid an overcorrection of the deformities [6].
Soft soles can determine positive effect on foot pain sensation, but they may also determine plantar pressure changes with negative effects on balance; on the contrary, firm inlays may have an opposite action on the plantar surface [4].
- 2.
Ankle-Foot Orthoses (AFO)
AFOs are the most commonly used LLO; they provide control of ankle dorsiflexion and plantar flexion and varus-valgus deviation, both static and dynamic. They also have a secondary effect on knee during ambulation: ankle plantiflexion facilitates knee extension whereas dorsiflexion helps knee flexion [2].
Static AFOs are devices made of rigid materials which keep joints in firm position; conversely, dynamic AFOs are defined using different terms with a similar meaning, such as hinged, articulating, and static progressive. AFOs are made of leather, plastic, metal, carbon composites, or a combination of these materials. Examples of static AFOs include solid ankle AFOs, ground reaction ankle-foot orthosis (GRAFO), and the patellar tendon bearing. Dynamic AFOs are posterior leaf spring, hinged (articulated) AFO, etc. [7].
The most prescribed AFOs are solid AFO, hinged AFO, and posterior leaf spring AFO. Solid AFOs restrict ankle motion and provide mediolateral stability of the foot; however, due to their rigidity and lack of plantar flexion, they could destabilize the knee during stance. Solid AFOs are used in the presence of ankle pain, plantar flexion spasticity, and foot drop associated with weakness of plantar flexors. Hinged MAFOs can be used to control ranges of motion of plantar flexion and dorsiflexion and to limit prono-supination. Posterior leaf spring MAFOs are flexible, they have the narrowest trimline, and the calf shell encircles less than half the circumference of calf; therefore they are not indicated in case of mediolaterally unstable ankle. They help weak ankle dorsiflexors during initial contact and swing phases of gait, preventing foot drop.
“Molded AFOs” (MAFOs) are thermoplastic and have many advantages; in fact they are lightweight, compact, easily wearable, not pliable at room temperature, and relatively inexpensive. MAFOs can be custom-made or manufactured in different sizes. Foot, ankle, and knee control depends on the anterior borders or edges at the malleolar region of the MAFOs (trimline). MAFOs consist of calf shell, calf strap, shoe insert, and, depending on the MAFO, a hinge at the malleolar level.
Metal AFOs include medial and lateral metal uprights, which are proximally attached to the limb with a calf band and distally fixed to a shoe sole by a stirrup. They are used in case of insensate skin because they have few points of contact [6].
Stroke often determines a motor impairment that mainly involves trunk, pelvis, knee, and ankle coordination both in standing position and during ambulation. Hemiparetic patients have specific gait patterns in the affected side, which is characterized by shorter step length, longer stance phase, and a shorter swing phase. They may also present an equinovarus foot, in which the weight support of the heel shifts to the lateral plantar surface, leading to imbalance, insecure gait, and, consequently, increased risk of falls. AFOs decrease the incidence of ankle contractures in patients with hemiparesis, but they should always maintain the ankle joint stiff, at the same time, in order to hold the foot in the correct position while standing and keep its clearance during swing phase [8]. However, an excessively stiff AFO will obstruct both the loading response during early phase of ground contact and the dorsiflexion during stance, causing this way instability, reduced walking speed, and a delay in recovery of ambulation [9].
AFOs have several potential disadvantages such as poor ankle hyperextension during stance and ineffective triplanar foot motion control; they also require good muscle strength and flexibility for knee control during swing. Moreover, AFOs increase bulk in the shoes and are difficult to use in case of severe spasticity [10] (Figs. 16.2 and 16.3).

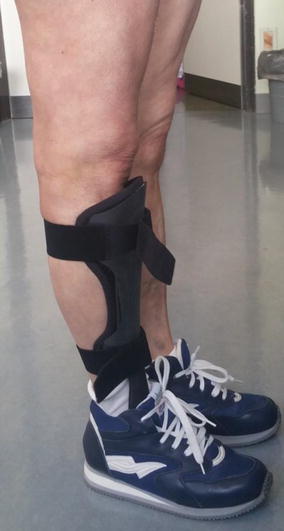

Fig. 16.2
AFOs. From left to right: AFO and posterior leaf spring AFO (in plastic material); MAFO and toe-off (in carbon composite)

Fig. 16.3
Toe-off AFO
- 3.
Knee-Ankle-Foot Orthoses (KAFO)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree