15.1 Introduction
Since the 1950s, there has been concern that poor nutrition may affect children’s development. There is now a considerable amount of research on the association between nutritional deficiencies and children’s development and cognition and mood in adults. The main nutritional conditions studied include intrauterine growth retardation (IUGR), the benefits of breastfeeding, early childhood undernutrition (moderate and severe stunting, underweight and wasting), short-term hunger and school feeding, and micronutrient deficiencies, including iron, iodine, zinc and vitamin A. Although these conditions are usually more prevalent and severe in developing countries, in developed countries most of them still occur and iron deficiency in particular remains common.
Poor nutrition can affect development prenatally from early gestation and throughout childhood. Nutrition may also affect adult functioning, at least transiently. However, it is likely that certain periods are more vulnerable than others and these periods may differ according to the type of deficiency. For example, the first two trimesters of pregnancy are the most sensitive to iodine deficiency, whereas the first two postnatal years are probably the most sensitive to undernutrition.
Child development is multidimensional and comprises several interrelated domains including motor, cognitive, social and emotional development. Investigators studying the effect of nutrition have traditionally focused on children’s motor and cognitive development and less often on school achievement. There is relatively little information on social and emotional development and mental health.
Children with nutritional deficiencies usually come from disadvantaged environments and are likely to be exposed to multiple biological risks. These disadvantages may have independent effects on children’s development and may modify the effects of nutritional deficiencies. Thus, demonstrating an association between a nutritional deficiency and poor development is insufficient to infer a causal relationship and randomized controlled trials (RCTs) of nutritional supplementation are required, but may not always be feasible.
Development in children under 3 years has usually been assessed with infant development scales such as the Bayley Scales for Infant Development, which were standardized in the USA, or the Griffiths Scales, which were standardized in England. The Bayley gives a global mental score of general cognitive and language development and a motor score. The Griffiths has more subscales. In the first year of life infant development scales have very limited predictive value, although the predictive ability increases with age. There are now more efforts to use tests of recognition memory, problem solving and attention, which may have better predictive ability, at least in the first year. Intelligence tests such as the Weschler Intelligence Scales for Children (WISC) have been used in older children and adults to assess intelligence. Batteries of cognitive tests have been used to assess specific cognitive functions, mainly in older children and adults, and school achievement tests used to assess school subjects such as reading and arithmetic. Parental and teacher reports have usually been used to assess behavior, which may suffer from some bias in that parents of malnourished children are generally less educated and have lower intelligence quotients (IQs) than those of adequately nourished children. Behavior observations are probably a more valid way of assessing behavior, but they are time consuming and require considerable training. A problem with many tests, especially infant assessment scales and IQ tests, is that they are not standardized for most developing countries and may not be culturally appropriate. Therefore, the best approach depends on having a local control group and only making within-population comparisons. It is important to have some measure of the validity of the test within the population that is being studied.
This chapter briefly discusses the effect of the environment on child development and possible mechanisms linking nutritional deficiencies to poor child development, then describes for each of the conditions mentioned above the evidence for an effect on child development.
15.2 Child development and the role of the environment
It is important to understand how children develop and the context of undernutrition in order to evaluate the effects of undernutrition. Children’s development is multifactorial, being influenced by a multitude of factors including genetics, child characteristics (e.g. temperament), the biological state of the child (e.g. health and nutritional status), the proximal environment (e.g. level of stimulation in the home, quality of maternal–child interaction) and the distal environment (e.g. parental education, culture, urban or rural residence, type of neighborhood). Some factors are protective, whereas others make the child more vulnerable. For example, high levels of maternal education and intelligence and good stimulation in the home may act as protective factors, which reduce the detrimental effect of low birth weight or early childhood undernutrition on child development. Conversely, the same nutritional conditions are likely to have worse effects on child development when mothers are illiterate, and the family lives in a poor home with inadequate levels of stimulation. Risk and protective factors continue to affect development throughout childhood and the long-term effects of nutritional deficiencies in early childhood depend to some extent on previous, current and future experiences.
15.3 Possible mechanisms linking undernutrition to poor development
There are two main hypotheses explaining how nutritional deficiencies could affect mental development. One theory is the functional isolation hypothesis. In this theory, the behavioral characteristics of undernourished children lead to reduced interaction with the environment and this in turn leads to poor developmental outcomes. Young children who are underweight, stunted, iron deficient, small for gestational age (SGA) or, to a lesser extent, zinc deficient have been found to show altered behavior, which concurs with this hypothesis. They have reduced activity, increased fussiness and unhappiness, and less exploration than adequately nourished children. These behaviors are believed to impede development. Caregivers may also be affected by the child’s altered behavior. For example, caregivers of children with nutritional deficiencies have been described as having poorer quality vocalizations, to hold and carry their child more, to be less responsive, and to give their child less praise and affection. Poor maternal–child interactions further exacerbate the child’s poor developmental progress. It is not clear whether the mothers are less stimulating before the onset of undernutrition or become less stimulating as a response to the children’s altered behavior following the onset of malnutrition. It is likely that both occur.
Another hypothesis is that undernutrition results in structural and functional alterations in the brain. Animal studies have shown that prenatal and early postnatal malnutrition in rats leads to many changes in brain structure, although some of these changes are reversible on refeeding. However, several alterations are thought to be irreversible, including a reduction in myelin and the number of cortical dentrites in neural spines and an increase in neuronal mitochondria. Evidence of changes to brain structure and function in children is limited, although severely malnourished children have small heads and abnormal auditory-evoked potentials, which remain abnormal after recovery from the acute stage. In addition, stunted children have small heads, and head circumference in early childhood has been shown to predict IQ in later childhood. Changes in brain structure have been described in animals with protein–energy malnutrition (PEM), iron deficiency and zinc deficiency. Marked changes also occur when the fetus is exposed to severe iodine deficiency, which results in cretinism.
There is less evidence for a third possible mechanism, which is that an altered stress response could contribute to undernourished children’s behavioral differences and poorer development. In one study in Jamaica, stunted children aged 8–10 years were more inhibited in a stressful situation and had increased salivary cortisol levels and urinary adrenaline (epinephrine) and higher heart rates than nonstunted children. The finding of an altered stress response in stunted children needs replicating and further exploring in other populations to determine whether it plays a role in the etiology of poor development.
15.4 Prevalence of nutritional deficiencies
Low birth weight
In developing countries low birth weight (LBW) babies are more likely than those in developed countries to have had intrauterine growth retardation (IUGR) secondary to poor maternal nutrition and increased infections. Sixteen per cent of infants worldwide are born with LBW (<2500g) and 95% of these are in developing countries. The prevalence ranges from around 50% in Bangladesh to 6% in developed countries.
Stunting and wasting
Stunting and wasting are diagnosed by anthropometry. The child’s weight and height are expressed in standard scores of the median of internationally accepted references for their age and gender. Moderate underweight indicates weight for age below −2 standard deviations (SD) below the median of the National Center for Health Statistics (NCHS) international references, moderate stunting indicates height for age below −2 SD, and moderate wasting indicates weight for height below −2 SD. Below − 3 SD indicates a severe condition. Another form of severe undernutrition is kwashiorkor, in which edema occurs in association with underweight. Undernutrition was previously referred to as PEM. However, when children are undernourished as a result of low dietary intakes of energy and protein their diets are usually also deficient in many micronutrients. Although there has been some decline in the prevalence of childhood undernutrition it remains extremely high. In developing countries, 29% of children under 5 years are moderately underweight, 33% are moderately stunted and 10% are moderately wasted. In least developed countries, 40% of children under 5 are underweight and 45% are stunted. The prevalence of moderately and severely underweight children is estimated to have declined globally from 38% in 1980 to 30% in 1997 and 29% in 2001. However, several countries in sub-Saharan Africa are showing an increase in the prevalence of childhood undernutrition. Undernutrition thus remains a very important public health issue in the twenty-first century.
Iron deficiency anemia
The prevalence of anemia is used as a proxy indicator for iron deficiency in the public health setting. The prevalence of anemia is determined by the level of hemoglobin in the blood. The cut-off points for blood hemoglobin to define anemia differ by age and are 110 g/l for children aged 6–59 months, 115 g/l for children aged 5–11 years and 120 g/l for children aged 12–14 years. There are no recent comprehensive data on the prevalence of anemia in children, but in 1985 the estimated prevalence of anemia (hemoglobin <110 g/l) in children under 5 years of age was 46–51% in developing countries and 7–12% in developed countries. Iron-deficiency anemia (IDA) is often found in poor neighborhoods and immigrant populations in England. It is the most common cause of anemia and is most prevalent in children from 6 to 24 months of age.
Zinc deficiency
The prevalence of zinc deficiency is not known, but it is common in populations that consume little meat and high levels of phytate and fiber, which reduce zinc bioavailability. This diet is highly prevalent in many developing countries. Zinc is also lost from the body during episodes of diarrheal disease. Requirements for zinc increase during periods of rapid growth, for example, infancy and pregnancy. Therefore, in many developing countries, where young children have poor diets and frequent diarrhea, it is likely that zinc deficiency is present.
Iodine deficiency
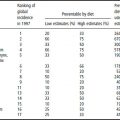
The indicators for assessing iodine-deficiency disorder (IDD) are the median urinary iodine and the prevalence of goiter. The normal median value for urinary iodine is 100–200 μg/l. Values of 50–99 μg/l indicate a mild deficiency, 20–49 μg/l indicate a moderate deficiency and below 20 μg/l indicate a severe deficiency. The presence of goiter is examined by inspection and palpation and the goiter is graded according to size. The criterion for elimination of IDD as a public health problem is a goiter prevalence of less than 5% of the population. School-aged children are usually the target group for surveillance. According to the World Health Organization (WHO), 13% of the world’s population (740 million people) are affected by IDD and a further 30% are at risk. Nearly 50 million people are believed to suffer from some form of neurological or cognitive deficits related to IDD. Iodine deficiency is prevalent in areas in which the soil is low in iodine content owing to leaching caused by high rainfall, flooding, melting snow and glaciation, and thus mountainous areas are particularly at risk.
Vitamin A deficiency
Vitamin A deficiency is diagnosed by the concentrations of serum retinol. Serum retinol below 20 μg/dl (0.70mol/l) is classified as moderate vitamin A deficiency and levels below 10 μg/dl (0.35 mol/l) are classified as severe. The WHO states that vitamin A deficiency is a public health problem in 118 countries worldwide and is especially prevalent in Africa and south-east Asia. Some 100–140 million children are vitamin A deficient and between one-quarter and half a million of these children become blind every year, with half of them dying within 12 months of losing their sight.
15.5 Intrauterine growth retardation
In developing countries, the majority of LBW infants are born at term and have suffered from IUGR as a result of maternal stunting and inadequate nutrition before and during pregnancy, and/or frequent infections such as malaria.
In contrast, in developed countries, biomedical causes such as multiple pregnancy and prematurity are responsible for a higher proportion of LBW infants. Cigarette smoking also contributes to LBW. Although at present cigarette smoking by women is not common in developing countries it is on the increase in some countries.
The effects of SGA on child development have been investigated in many studies. However, there are many problems in interpreting the results. First, different definitions of SGA have been used. The WHO recommends using the 10th centile of birth weights for gestational age from a standard population as the cut-off point. However, this cut-off may be too high to represent a risk for development.
In addition, there is a greater incidence of perinatal and neonatal complications in LBW babies that may also detrimentally affect development. Some studies have omitted children with complications, while others have included them.
Particularly in low-income countries, LBW is associated with poor environments, which may independently affect child development. Many studies have failed to control adequately for the effects of these environments.
Further problems include the fact that LBW babies are also less likely to be breast-fed and that many studies have had high dropout rates of between 30 and 50%, which are likely to be biased. For example, in a Brazilian study, LBW infants who were lost to follow-up at 12 months of age had significantly lower developmental levels at 6 months than those who were located.
The effect of being small for gestational age on child development
The majority of studies on the effects of being low birth weight born at term (LBW-T) or SGA on child development have been conducted in developed countries. Most studies have found no significant differences between SGA term babies and normal birth weight babies in the first year of life, although a few have found differences. Traditional infant developmental tests were generally used in the first year of life and may not be sensitive to some cognitive functions. However, in a study in Brazil, normal birth weight infants scored significantly higher than SGA infants on tests of both motor and mental development at 6 and 12 months. By the second year of life, most studies found significant developmental deficits for SGA children, although the differences were largely found in particularly vulnerable subgroups. These groups included male children, black children, children with congenital abnormalities and children with birth weight below 2300 g.
Studies in early childhood (2–7 years of age) have generally shown differences in development between SGA and normal birth weight infants, favoring the latter. SGA children have been found to have lower IQ, poorer language skills, lower reading readiness scores and poorer school achievement, and to be more likely to be retained at grade level or to be in a special class. These differences have been detected even when there was no difference detected in the same study sample in the first year of life.
Studies investigating the effects of SGA into adolescence have consistently found developmental deficits including lower IQ, higher placement in special education classes and poorer school achievement. These differences usually remained after controlling for socioeconomic variables, but in some studies they were no longer significant.
A few studies have examined the effects of SGA into late adolescence and adulthood and most, but not all, have found that small deficits in attained educational levels or cognitive abilities persist. Several studies have found that the relationship between cognition and birth weight is also present across the normal birth weight range.
Nearly all of the above studies were from developed countries. Two studies on the medium- or long-term development of children born SGA were identified from developing countries. In India, early childhood malnutrition had a greater effect than SGA on child development, and in Guatemala, there was no evidence of a cognitive deficit in SGA children. It may be that the poor health, poor nutrition and low levels of stimulation often experienced by children living in poverty in developing countries overwhelm the effect of SGA on child development.
Children born SGA have also been found to have different behavior than normal birth weight children. They have been described as less active, less vocal, less responsive, less happy and less cooperative in the first 2 years of life, and more fidgety, more anxious, less happy and having a poorer attention span at school age.
SGA interacts with other risk factors for development. For example, in Brazil, the development of SGA children was shown to be detrimentally affected by low levels of stimulation in the home, maternal illiteracy and frequent diarrhea, whereas the development of normal birth weight children was not. This heightened vulnerability of SGA children has implications for developing countries in that most SGA children come from disadvantaged homes which will put these children at further risk for poor development.
Recommendations for public health interventions
Children born LBW are at risk not only for poor development, but also for poor health and nutrition, and often come from poorer homes. An integrated program approach combing health, nutrition and child development activities is most appropriate. Programs involving early stimulation for LBW children in developed countries (primarily in North America) have shown benefits to children’s mental development and behavior, and similar programs are likely to be beneficial in developing countries.
15.6 Breast-feeding and its influence on child development
How breast-feeding benefits development
There are several mechanisms by which breast-feeding may benefit child development. First, breastmilk is a rich source of long-chain polyunsaturated fatty acids (LCPUFA), which are not only a source of energy, but are also the predominant molecules found in myelin, and are particularly concentrated in the retina. LCPUFA are therefore important in brain development. Humans cannot make certain LCPUFA (n-6 and n-3), and acquire them from the mother mainly in the last trimester of pregnancy and postnatally from their diet. In formula milk the concentration of LCPUFA is thought to be insufficient to meet infant requirements, particularly for preterm infants. However, it is controversial whether this insufficiency has long-term developmental consequences. Many studies have investigated the effects of LCPUFA supplementation on visual acuity. Most studies with formula-fed preterm infants have shown that supplementation improves their visual acuity in the first few months. However, some studies have shown that the nonsupplemented infants catch up on weaning. Fewer studies have looked at visual acuity in term infants and they have had inconsistent findings.
Fewer studies have examined the effects of supplementation on general development and results have again been inconsistent. In preterm infants effects were found on motor but not mental scores of the Bayley test in one study, and on Bayley mental but not motor scores in another study. In a third study no effect on Bayley scores was found. Results for term infants show less effect than for preterm infants.
Speed of processing (habituation) or problem solving has also been improved with supplementation in a few studies. There is a need for longer term studies as there is little information after the second year and most tests of infant cognition have only low predictive ability for future intelligence. In addition, the results may depend on the relative amounts of the different LCPUFA and the duration and timing of supplementation. Excessive amounts or imbalances among the PUFA may cause problems.
Secondly, breast-feeding may increase infant immunity to disease, as shown by studies in which breastfeeding is associated with a decrease in levels of diarrhea, chronic constipation, gastrointestinal illness, and respiratory tract and ear infections. Through promoting improved health of the infant, it is likely that breast-feeding will indirectly benefit psychomotor development, as a sick child is less able to explore and learn from the environment. There is some evidence that even small amounts of breast milk can increase an infant’s immunity, with a dose–response relationship between breast-feeding and reduced infection.
Finally, breast-feeding may benefit the maternal–child interaction and facilitate the development of a secure attachment, which is thus likely to benefit the child’s development and behavior.
Short-term effects of breast-feeding
There are many studies on the concurrent effects of breast-feeding on child development, involving children from birth to 2 years. Most studies were conducted in developed countries (with only two studies identified from developing countries) and used the Bayley Scale of Infant Development as the outcome measure. Studies investigated differences between breast-fed and nonbreast-fed infants at 6, 12, 18 and 24 months, and at all points in time breast-feeding was generally associated with higher scores on developmental tests, although the differences were not always significant. However, more significant differences were found in the second year of life and it may be that the Bayley test is not sensitive enough to detect small differences in the first year of life. There is some evidence that the longer the infant is breast-fed, the greater the gains in psychomotor development. Breast-feeding appears to benefit all children, regardless of social class. The benefits are usually reduced after controlling for the effects of socioeconomic variables, although they generally remain significant.
In two recent randomized trials in Honduras, infants who were exclusively breast-fed for 6 months crawled sooner in both studies and were more likely to be walking by 12 months in one of the studies than infants who were exclusively breast-fed for 4 months.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree